Intestinal permeability
Intestinal permeability is a term describing the control of material passing from inside the gastrointestinal tract through the cells lining the gut wall, into the rest of the body. The intestine normally exhibits some permeability, which allows nutrients to pass through the gut, while also maintaining a barrier function to keep potentially harmful substances (such as antigens) from leaving the intestine and migrating to the body more widely.[1] In a healthy human intestine, small particles (< 4 Å in radius) can migrate through tight junction claudin pore pathways,[2] and particles up to 10–15 Å (3.5 kDa) can transit through the paracellular space uptake route.[3] There is some evidence abnormally increased intestinal permeability may play a role in some chronic diseases and inflammatory conditions.[4] The most well understood condition with observed increased intestinal permeability is celiac disease.[5]
Physiology
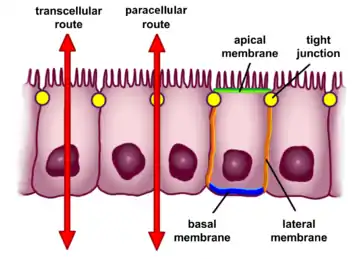
The barrier formed by the intestinal epithelium separates the external environment (the contents of the intestinal lumen) from the body[6] and is the most extensive and important mucosal surface of the body.[7] However, the intestinal mucin can also be barriers for the host antimicrobial peptides, thus plays a bidirectional barrier for host-microbial interaction.[8] The intestinal epithelium is composed of a single layer of cells and serves two crucial functions. First, it acts as a barrier, preventing the entry of harmful substances such as foreign antigens, toxins and microorganisms.[6][9] Second, it acts as a selective filter which facilitates the uptake of dietary nutrients, electrolytes, water and various other beneficial substances from the intestinal lumen.[6] Selective permeability is mediated via two major routes:[6]
- Transepithelial or transcellular permeability. This consists of specific transport of solutes across the epithelial cells. It is predominantly regulated by the activities of specialised transporters that translocate specific electrolytes, amino acids, sugars, short chain fatty acids and other molecules into or out of the cell.[6]
- Paracellular permeability. It depends on transport through the spaces that exist between epithelial cells. It is regulated by cellular junctions that are localized in the laminal membranes of the cells.[6] This is the main route of passive flow of water and solutes across the intestinal epithelium. Regulation depends on the intercellular tight junctions which have the most influence on paracellular transport.[10] Disruption of the tight junction barrier can be a trigger for the development of intestinal diseases.
Modulation
One way in which intestinal permeability is modulated is via CXCR3 receptors in cells in the intestinal epithelium, which respond to zonulin.[4]
Gliadin (a glycoprotein present in wheat) activates zonulin signaling in all people who eat gluten, irrespective of the genetic expression of autoimmunity. This leads to increased intestinal permeability to macromolecules.[4][11][5] Bacterial infections such as cholera, select enteric viruses, parasites, and stress can all modulate intestinal tight junction structure and function, and these effects may contribute to the development of chronic intestinal disorders.[4][12][11] So called absorption modifying excipients, investigated for the possibility of increasing intestinal drug absorption, can increase the gut permeability.[13]
Clinical significance
Most people do not experience adverse symptoms, but the opening of intercellular tight junctions (increased intestinal permeability) can act as a trigger for diseases that can affect any organ or tissue depending on genetic predisposition.[4][5][14]
Increased intestinal permeability is a factor in several diseases, such as Crohn's disease, celiac disease,[15] type 1 diabetes,[16] type 2 diabetes,[15] rheumatoid arthritis, spondyloarthropathies,[17] inflammatory bowel disease,[4][18] schizophrenia,[19][20] certain types of cancer,[4] obesity,[21] fatty liver,[22] atopy and allergic diseases,[16] among others. In the majority of cases, increased permeability develops prior to disease,[4] but the cause–effect relationship between increased intestinal permeability in most of these diseases is not clear.[18][23]
A well studied model is celiac disease, in which increased intestinal permeability appears secondary to the abnormal immune reaction induced by gluten and allows fragments of gliadin protein to get past the intestinal epithelium, triggering an immune response at the intestinal submucosa level that leads to diverse gastrointestinal or extra-gastrointestinal symptoms.[24][25] Other environmental triggers may contribute to alter permeability in celiac disease, including intestinal infections and iron deficiency.[24] Once established, this increase of permeability might self-sustain the inflammatory immune responses and perpetuate a vicious cycle.[24] Eliminating gluten from the diet leads to normalization of intestinal permeability and the autoimmune process shuts off.[26]
Research directions
In normal physiology, glutamine plays a key role in signalling in enterocytes that are part of the intestinal barrier, but it is not clear if supplementing the diet with glutamine is helpful in conditions where there is increased intestinal permeability.[27]
Prebiotics and certain probiotics such as E.Coli strain Nissle 1917 have been found to reduce increased intestinal permeability.[11] Lactobacillus rhamnosus,[28] Lactobacillus reuteri,[28] and Faecalibacterium prausnitzii[29] have also been shown to significantly reduce increased intestinal permeability.
Larazotide acetate (previously known as AT-1001) is a zonulin receptor antagonist that has been probed in clinical trials. It seems to be a drug candidate for use in conjunction with a gluten-free diet in people with celiac disease, with the aim to reduce the intestinal permeability caused by gluten and its passage through the epithelium, and therefore mitigating the resulting cascade of immune reactions.[25][30]
Decreasing intestinal barrier function with aging can cause increased translocation of microbial products, such as lipopolysaccharide, into the systemic blood circulation that subsequently causes systemic inflammation (inflammaging) and significant clinical outcomes: metabolic syndrome, decreased physical function, and mortality.[31][32] It has been shown that the loss of intestinal barrier function is associated with an increased formation of nitric oxide (NO) and lower activity of arginase.[33][34] Genetic disruption of arginase-2 in mouse attenuates the onset of senescence and extends lifespan.[35][34] Arginase inhibitors have been developed to reduce the effect of NO on intestinal permeability.[34]
Leaky gut syndrome
"Leaky gut syndrome" is a hypothetical, medically unrecognized condition.[18] It has been popularized by some nutritionists and practitioners of alternative medicine who claim that restoring normal functioning of the gut wall can cure many systemic health conditions. However, reliable source evidence to support this claim has not been published. Nor has there been published any reliable evidence that the treatments promoted for so-called "leaky gut syndrome"—including nutritional supplements, probiotics,[11] herbal remedies, (or low-FODMAP diets; low-sugar, antifungal, or gluten-free diets)—have any beneficial effect for most of the conditions they are claimed to help.[18]
Exercise-induced stress
Exercise-induced stress can diminish intestinal barrier function.[36][37][38] In humans, the level of physical activity modulates the gastrointestinal microbiota, an increased intensity and volume of exercise may lead to gut dysbiosis, and supplementation may keep gut microbiota in biodiversity, especially with intense exercise.[39] In mice, exercise reduced the richness of the microbial community, but increased the distribution of bacterial communities.[40]
References
- M. Campieri; C. Fiocchi; S.B. Hanauer (31 March 2002). Inflammatory Bowel Disease: A Clinical Case Approach to Pathophysiology, Diagnosis, and Treatment. Springer. p. 7. ISBN 978-0-7923-8772-5.
- Thoma YM, Anderson JM, Turner JR (2012). Johnson LR, et al. (eds.). Tight Junctions and the Intestinal Barrier. pp. 1043–. ISBN 978-0-12-382027-3.
{{cite book}}:|work=ignored (help) - Fasano, A. (February 2012). "Leaky Gut and Autoimmune Diseases". Clinical Reviews in Allergy & Immunology (Review). 42 (1): 71–78. doi:10.1007/s12016-011-8291-x. PMID 22109896. S2CID 4088994.
- Fasano A (Jan 2011). "Zonulin and its regulation of intestinal barrier function: the biological door to inflammation, autoimmunity, and cancer". Physiological Reviews (Review). 91 (1): 151–75. CiteSeerX 10.1.1.653.3967. doi:10.1152/physrev.00003.2008. PMID 21248165.
- Leonard MM, Sapone A, Catassi C, Fasano A (2017). "Celiac Disease and Nonceliac Gluten Sensitivity: A Review". JAMA (Review). 318 (7): 647–656. doi:10.1001/jama.2017.9730. PMID 28810029. S2CID 205094729.
Previous studies have shown that gliadin can cause an immediate and transient increase in gut permeability. This permeating effect is secondary to the binding of specific undigestible gliadin fragments to the CXCR3 chemokine receptor with subsequent release of zonulin, a modulator of intercellular tight junctions. This process takes place in all individuals who ingest gluten. For the majority, these events do not lead to abnormal consequences. However, these same events can lead to an inflammatory process in genetically predisposed individuals when the immunologic surveillance system mistakenly recognizes gluten as a pathogen.
- Groschwitz KR, Hogan SP (July 2009). "Intestinal barrier function: molecular regulation and disease pathogenesis". The Journal of Allergy and Clinical Immunology. 124 (1): 3–20, quiz 21–2. doi:10.1016/j.jaci.2009.05.038. PMC 4266989. PMID 19560575.
- Rao JN, Wang JY (2010-01-01). "Intestinal Architecture and Development". Morgan & Claypool Life Sciences.
{{cite journal}}: Cite journal requires|journal=(help) - Hartmann P, Chen P, Wang HJ, Wang L, McCole DF, Brandl K, et al. (July 2013). "Deficiency of intestinal mucin-2 ameliorates experimental alcoholic liver disease in mice". Hepatology. 58 (1): 108–19. doi:10.1002/hep.26321. PMC 3695050. PMID 23408358.
- Khan N, Asif AR (2015-01-01). "Transcriptional regulators of claudins in epithelial tight junctions". Mediators of Inflammation. 2015: 219843. doi:10.1155/2015/219843. PMC 4407569. PMID 25948882.
- Näslund E, Hellström PM (September 2007). "Appetite signaling: from gut peptides and enteric nerves to brain". Physiology & Behavior. 92 (1–2): 256–62. doi:10.1016/j.physbeh.2007.05.017. PMID 17582445. S2CID 230872.
- Rapin JR, Wiernsperger N (2010). "Possible links between intestinal permeability and food processing: A potential therapeutic niche for glutamine". Clinics (Review). 65 (6): 635–43. doi:10.1590/S1807-59322010000600012. PMC 2898551. PMID 20613941.
- O'Hara JR, Buret AG (May 2008). "Mechanisms of intestinal tight junctional disruption during infection". Frontiers in Bioscience. 13 (13): 7008–21. doi:10.2741/3206. PMID 18508712.
- Dahlgren D, Roos C, Lundqvist A, Tannergren C, Langguth P, Sjöblom M, et al. (December 2017). "Preclinical Effect of Absorption Modifying Excipients on Rat Intestinal Transport of Model Compounds and the Mucosal Barrier Marker 51Cr-EDTA". Molecular Pharmaceutics. 14 (12): 4243–4251. doi:10.1021/acs.molpharmaceut.7b00353. PMID 28737406.
- Suzuki T (February 2013). "Regulation of intestinal epithelial permeability by tight junctions". Cellular and Molecular Life Sciences. 70 (4): 631–59. doi:10.1007/s00018-012-1070-x. PMID 22782113. S2CID 16512214.
- Bischoff SC, Barbara G, Buurman W, Ockhuizen T, Schulzke JD, Serino M, Tilg H, Watson A, Wells JM (Nov 18, 2014). "Intestinal permeability--a new target for disease prevention and therapy". BMC Gastroenterology (Review). 14: 189. doi:10.1186/s12876-014-0189-7. PMC 4253991. PMID 25407511.
- Viggiano D, Ianiro G, Vanella G, Bibbò S, Bruno G, Simeone G, et al. (2015). "Gut barrier in health and disease: focus on childhood" (PDF). European Review for Medical and Pharmacological Sciences. 19 (6): 1077–85. PMID 25855935.
- Yeoh N, Burton JP, Suppiah P, Reid G, Stebbings S (Mar 2013). "The role of the microbiome in rheumatic diseases". Current Rheumatology Reports (Review). 15 (3): 314. doi:10.1007/s11926-012-0314-y. PMID 23378145. S2CID 25721240.
- "Leaky gut syndrome". NHS Choices. 26 February 2015. Archived from the original on 2018-02-11. Retrieved 15 August 2016.
- Yarandi SS, Peterson DA, Treisman GJ, Moran TH, Pasricha PJ (2016). "Modulatory Effects of Gut Microbiota on the Central Nervous System: How Gut Could Play a Role in Neuropsychiatric Health and Diseases". Journal of Neurogastroenterology and Motility (Review). 22 (2): 201–12. doi:10.5056/jnm15146. PMC 4819858. PMID 27032544.
In patients with schizophrenia, there are increased intestinal permeability and change in intestinal function
- Severance EG, Yolken RH, Eaton WW (2016). "Autoimmune diseases, gastrointestinal disorders and the microbiome in schizophrenia: more than a gut feeling". Schizophrenia Research (Review). 176 (1): 23–35. doi:10.1016/j.schres.2014.06.027. PMC 4294997. PMID 25034760.
- Teixeira TF, Collado MC, Ferreira CL, Bressan J, Peluzio Mdo C (September 2012). "Potential mechanisms for the emerging link between obesity and increased intestinal permeability". Nutrition Research (Review). 32 (9): 637–47. doi:10.1016/j.nutres.2012.07.003. PMID 23084636.
- Festi D, Schiumerini R, Eusebi LH, Marasco G, Taddia M, Colecchia A (November 2014). "Gut microbiota and metabolic syndrome". World Journal of Gastroenterology (Review). 20 (43): 16079–16094. doi:10.3748/wjg.v20.i43.16079. PMC 4239493. PMID 25473159.
- Kiefer D, Ali-Akbarian L (2004). "A brief evidence-based review of two gastrointestinal illnesses: irritable bowel and leaky gut syndromes". Alternative Therapies in Health and Medicine. 10 (3): 22–30, quiz 31, 92. PMID 15154150.
- Heyman M, Abed J, Lebreton C, Cerf-Bensussan N (September 2012). "Intestinal permeability in coeliac disease: insight into mechanisms and relevance to pathogenesis". Gut (Review). 61 (9): 1355–64. doi:10.1136/gutjnl-2011-300327. PMID 21890812. S2CID 42581980.
Changes in intestinal paracellular and transcellular permeability appear secondary to the abnormal immune reaction induced by gluten. Gliadin was suggested to increase junction permeability to small molecules through the release of prehaptoglobin-2. Environmental triggers of CD other than gliadin may also promote changes in permeability. Intestinal infection and iron deficiency can stimulate the expression of the transferrin receptor (TfR) CD71 in enterocytes. ... Once established, the alterations in intestinal permeability, notably the retro-transport of IgA-gliadin peptides, might self-sustain the inflammatory immune responses and perpetuate a vicious circle.
- Khaleghi S, Ju JM, Lamba A, Murray JA (January 2016). "The potential utility of tight junction regulation in celiac disease: focus on larazotide acetate". Therapeutic Advances in Gastroenterology (Review. Research Support, N.I.H., Extramural). 9 (1): 37–49. doi:10.1177/1756283X15616576. PMC 4699279. PMID 26770266.
- Fasano A (October 2012). "Intestinal permeability and its regulation by zonulin: diagnostic and therapeutic implications". Clinical Gastroenterology and Hepatology (Review). 10 (10): 1096–100. doi:10.1016/j.cgh.2012.08.012. PMC 3458511. PMID 22902773.
- Akobeng AK, Elawad M, Gordon M (February 2016). "Glutamine for induction of remission in Crohn's disease" (PDF). The Cochrane Database of Systematic Reviews. 2016 (2): CD007348. doi:10.1002/14651858.CD007348.pub2. PMC 10405219. PMID 26853855.
- Lopetuso LR, Scaldaferri F, Bruno G, Petito V, Franceschi F, Gasbarrini A (2015). "The therapeutic management of gut barrier leaking: the emerging role for mucosal barrier protectors". European Review for Medical and Pharmacological Sciences. 19 (6): 1068–1076. PMID 25855934.
- Ganesan K, Chung SK, Vanamala J, Xu B (2018). "Causal Relationship between Diet-Induced Gut Microbiota Changes and Diabetes: A Novel Strategy to Transplant Faecalibacterium prausnitzii in Preventing Diabetes". International Journal of Molecular Sciences. 19 (12): E3720. doi:10.3390/ijms19123720. PMC 6320976. PMID 30467295.
- Crespo Pérez L, et al. (Jan 2012). "Non-dietary therapeutic clinical trials in coeliac disease". European Journal of Internal Medicine (Review). 23 (1): 9–14. doi:10.1016/j.ejim.2011.08.030. PMID 22153524.
- Kavanagh K, Hsu FC, Davis AT, Kritchevsky SB, Rejeski WJ, Kim S (December 2019). "Biomarkers of leaky gut are related to inflammation and reduced physical function in older adults with cardiometabolic disease and mobility limitations". Geroscience. 41 (6): 923–933. doi:10.1007/s11357-019-00112-z. PMC 6925090. PMID 31654268.
- Dambroise E, Monnier L, Ruisheng L, Aguilaniu H, Joly JS, Tricoire H, Rera M (March 2016). "Two phases of aging separated by the Smurf transition as a public path to death". Sci Rep. 6: 23523. Bibcode:2016NatSR...623523D. doi:10.1038/srep23523. PMC 4802314. PMID 27002861.
- Baumann A, Rajcic D, Brandt A, Sánchez V, Jung F, Staltner R, Nier A, Trauner M, Staufer K, Bergheim I (February 2022). "Alterations of nitric oxide homeostasis as trigger of intestinal barrier dysfunction in non-alcoholic fatty liver disease". J Cell Mol Med. 26 (4): 1206–1218. doi:10.1111/jcmm.17175. PMC 8831936. PMID 35029027.
- Brandt A, Baumann A, Hernández-Arriaga A, Jung F, Nier A, Staltner R, Rajcic D, Schmeer C, Witte OW, Wessner B, Franzke B, Wagner KH, Camarinha-Silva A, Bergheim I (December 2022). "Impairments of intestinal arginine and NO metabolisms trigger aging-associated intestinal barrier dysfunction and 'inflammaging'". Redox Biol. 58: 102528. doi:10.1016/j.redox.2022.102528. PMC 9649383. PMID 36356464.
- Xiong Y, Yepuri G, Montani JP, Ming XF, Yang Z (2017). "Arginase-II Deficiency Extends Lifespan in Mice". Front Physiol. 8: 682. doi:10.3389/fphys.2017.00682. PMC 5596098. PMID 28943853.
- Clark, Allison; Mach, Núria (5 January 2016). "Exercise-induced stress behavior, gut-microbiota-brain axis and diet: a systematic review for athletes". Journal of the International Society of Sports Nutrition. 13 (1): 346–349. doi:10.1186/s12970-016-0155-6. PMC 5121944. PMID 5121944.

- Keirns, Bryant H.; Koemel, Nicholas A.; Sciarrillo, Christina M.; Anderson, Kendall L.; Emerson, Sam R. (1 October 2020). "Exercise and intestinal permeability: another form of exercise-induced hormesis?". American Journal of Physiology. Gastrointestinal and Liver Physiology. 319 (4): G512–G518. doi:10.1152/ajpgi.00232.2020. PMID 32845171. S2CID 221328089.
- Van Wijck, Kim; Lenaerts, Kaatje; Van Bijnen, Annemarie A.; Boonen, Bas; Van Loon, Luc J. C.; Dejong, Cornelis H. C.; Buurman, Wim A. (December 2012). "Aggravation of Exercise-Induced Intestinal Injury by Ibuprofen in Athletes". Medicine & Science in Sports & Exercise. 44 (12): 2257–2262. doi:10.1249/mss.0b013e318265dd3d. PMID 22776871. S2CID 9982820.
- Dziewiecka, Hanna; Buttar, Harpal S.; Kasperska, Anna; Ostapiuk–Karolczuk, Joanna; Domagalska, Małgorzata; Cichoń, Justyna; Skarpańska-Stejnborn, Anna (7 July 2022). "Physical activity induced alterations of gut microbiota in humans: a systematic review". BMC Sports Science, Medicine and Rehabilitation. 14 (1): 122. doi:10.1186/s13102-022-00513-2. PMC 9264679. PMID 35799284.

- Yan, Qiuyu; Zhai, Wenhui; Yang, Chenghao; Li, Zihao; Mao, Longfei; Zhao, Mingyi; Wu, Xiushan (12 October 2021). "The Relationship among Physical Activity, Intestinal Flora, and Cardiovascular Disease". Cardiovascular Therapeutics. 2021: 1–10. doi:10.1155/2021/3364418. PMC 8526197. PMID 34729078.
