Menopause
Menopause, also known as the climacteric, is the time in women's lives when menstrual periods stop permanently, and they are no longer able to bear children.[1][6] Menopause usually occurs between the age of 47 and 54.[7] Medical professionals often define menopause as having occurred when a woman has not had any menstrual bleeding for a year.[2] It may also be defined by a decrease in hormone production by the ovaries.[8] In those who have had surgery to remove their uterus but still have functioning ovaries, menopause is not considered to have yet occurred.[9] Following the removal of the uterus, symptoms typically occur earlier.[10]
| Menopause | |
|---|---|
| Other names | Climacteric |
 | |
| Specialty | Gynecology |
| Symptoms | No menstrual periods for a year[1] |
| Duration | ~3 years |
| Causes | Usually a natural change. Can also be caused by surgery that removes both ovaries and some types of chemotherapy.[2][3] |
| Treatment | None, lifestyle changes[4] |
| Medication | Menopausal hormone therapy, clonidine, gabapentin, selective serotonin reuptake inhibitors[4][5] |
In the years before menopause, a woman's periods typically become irregular,[11][12] which means that periods may be longer or shorter in duration or be lighter or heavier in the amount of flow.[11] During this time, women often experience hot flashes; these typically last from 30 seconds to ten minutes and may be associated with shivering, sweating, and reddening of the skin.[11] Hot flashes[11] can last from four to five years.[6] Other symptoms may include vaginal dryness, trouble sleeping, and mood changes.[11] The severity of symptoms varies between women.[6] Menopause before the age of 45 years is considered to be "early menopause" and when ovarian failure/surgical removal of the ovaries occurs before the age of 40 years this is termed "premature ovarian insufficiency".[9]
In addition to symptoms (hot flushes/flashes, night sweats, mood changes, arthralgia and vaginal dryness), the physical consequences of menopause include bone loss, increased central abdominal fat, and adverse changes in a woman's cholesterol profile and vascular function.[9] These changes predispose postmenopausal women to increased risks of osteoporosis and bone fracture, and of cardio-metabolic disease (diabetes and cardiovascular disease).[9]
Menopause is usually a natural change.[3] It can occur earlier in those who smoke tobacco.[2][13] Other causes include surgery that removes both ovaries or some types of chemotherapy[14].[2] At the physiological level, menopause happens because of a decrease in the ovaries' production of the hormones estrogen and progesterone.[1] While typically not needed, a diagnosis of menopause can be confirmed by measuring hormone levels in the blood or urine.[15] Menopause is the opposite of menarche, the time when a girl's periods start.[16]
The primary indications for treatment of menopause are symptoms and prevention of bone loss.[17] Mild symptoms may be improved with treatment.[4] With respect to hot flashes, avoiding smoking, caffeine, and alcohol is often recommended;[4] sleeping naked in a cool room and using a fan may help.[4] The most effective treatment for menopausal symptoms is menopausal hormone therapy (MHT).[17] Non hormonal therapies for hot flashes include clonidine, gabapentin, or selective serotonin reuptake inhibitors.[4][5] These will not improve symptoms such as joint pain or vaginal dryness which affect over 55% of women.[17] Exercise may help with sleeping problems.[4] Many of the concerns about the use of MHT raised by older studies are no longer considered barriers to MHT in healthy women.[17] High-quality evidence for the effectiveness of alternative medicine has not been found.[6] There is tentative evidence for the use of phytoestrogens for symptomatic treatment.[18]
Signs and symptoms
.svg.png.webp)
During early menopause transition, the menstrual cycles remain regular but the interval between cycles begins to lengthen. Hormone levels begin to fluctuate. Ovulation may not occur with each cycle.[19]
The term menopause refers to a point in time that follows one year after the last menstruation.[19] During the menopausal transition and after menopause, women can experience a wide range of symptoms.[11] However, for women who enter the menopause transition without having regular menstrual cycles (due to prior surgery, other medical conditions or ongoing hormonal contraception) the menopause cannot be identified by bleeding patterns and is defined as the permanent loss of ovarian function.[17]
Vagina and uterus
During the transition to menopause, menstrual patterns can show shorter cycling (by 2–7 days);[19] longer cycles remain possible.[19] There may be irregular bleeding[11] (lighter, heavier, spotting).[19] Dysfunctional uterine bleeding is often experienced by women approaching menopause due to the hormonal changes that accompany the menopause transition. Spotting or bleeding may simply be related to vaginal atrophy, a benign sore (polyp or lesion), or may be a functional endometrial response. The European Menopause and Andropause Society has released guidelines for assessment of the endometrium, which is usually the main source of spotting or bleeding.[20]
In post-menopausal women, however, any unscheduled vaginal bleeding is of concern and requires an appropriate investigation to rule out the possibility of malignant diseases.
Urogenital symptoms that may appear during menopause and continue through postmenopause include:
Other physical effects
.jpg.webp)
Other physical symptoms of menopause include lack of energy, joint soreness, stiffness, back pain, breast enlargement, breast pain, heart palpitations, headache, dizziness, dry, itchy skin, thinning, tingling skin,[19] rosacea,[21] weight gain,[19] urinary incontinence,[19][22] urinary urgency,[19] interrupted sleeping patterns,[19][23][24][25] heavy night sweats,[19] and hot flashes.[19]
Mood and memory effects
Psychological symptoms include anxiety, poor memory, inability to concentrate, depressive mood, irritability, mood swings,[11] and less interest in sexual activity.[19][26]
Menopause-related cognitive impairment can be confused with the mild cognitive impairment that precedes dementia.[27] Tentative evidence has found that forgetfulness affects about half of menopausal women[28] and is probably caused by the effects of declining estrogen levels on the brain,[28] or perhaps by reduced blood flow to the brain during hot flashes.[29]
Cardiovascular health
Exposure to endogenous estrogen during reproductive years provides women with protection against cardiovascular disease, which is lost around 10 years after the onset of menopause. The menopausal transition is associated with an increase in fat mass (predominantly in visceral fat), an increase in insulin resistance, dyslipidaemia, and endothelial dysfunction.[30] Women with vasomotor symptoms during menopause seem to have an especially unfavorable cardiometabolic profile,[31] as well as women with premature onset of menopause (before 45 years of age).[32] These risks can be reduced by managing risk factors, such as tobacco smoking, hypertension, increased blood lipids and body weight.[33][34]
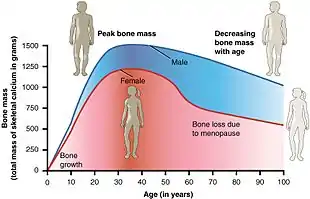
Bone health
The annual rates of bone mineral density loss are highest starting one year before the final menstrual period and continuing through the two years after it.[35] Thus, post menopausal women are at increased risk of osteopenia, osteoporosis and fractures.
Causes
Menopause can be induced or occur naturally. Induced menopause[36] occurs as a result of medical treatment such as chemotherapy, radiotherapy, oophorectomy, or complications of tubal ligation, hysterectomy, unilateral or bilateral salpingo-oophorectomy or leuprorelin usage.[37]
Age
Menopause typically occurs between 47 and 54 years of age.[7] According to various data, more than 85% of women have their last period between the ages of 47–54 (median 49–50). 2% of women under the age of 40, 5% between the ages of 40–45 and the same number between the ages of 55–58 have their last bleeding.[38] The average age of the last period in the United States is 51 years, in Russia is 50 years, in Greece is 49 years, in Turkey is 47 years, in Egypt is 47 years and in India is 46 years.[39] The menopausal transition or perimenopause leading up to menopause usually lasts 3–4 years (sometimes as long as 5–14 years).[1][12]
In rare cases, a woman's ovaries stop working at a very early age, ranging anywhere from the age of puberty to age 40. This is known as premature ovarian failure and affects 1 to 2% of women by age 40.[40]
Undiagnosed and untreated coeliac disease is a risk factor for early menopause. Coeliac disease can present with several non-gastrointestinal symptoms, in the absence of gastrointestinal symptoms, and most cases escape timely recognition and go undiagnosed, leading to a risk of long-term complications. A strict gluten-free diet reduces the risk. Women with early diagnosis and treatment of coeliac disease present a normal duration of fertile life span.[41][42]
Women who have undergone hysterectomy with ovary conservation go through menopause on average 1.5 years earlier than the expected age.[43] Another factor that can promote an earlier onset of menopause (usually 1 to 3 years early) is smoking cigarettes.[44]
Premature ovarian insufficiency
Premature ovarian insufficiency (POI) is when the ovaries stop functioning before the age of 40 years.[45][46] It is diagnosed or confirmed by high blood levels of follicle stimulating hormone (FSH) and luteinizing hormone (LH) on at least three occasions at least four weeks apart.[47]
Premature ovarian insufficiency may be auto immune and therefore co occur with other autoimmune disorders such as thyroid disease, [adrenal insufficiency], and diabetes mellitus. Other causes include chemotherapy, being a carrier of the fragile X syndrome gene, and radiotherapy.[46] However, in about 50–80% of cases of premature ovarian insufficiency, the cause is unknown, i.e., it is generally idiopathic.[45][47]
An early menopause can be related to cigarette smoking, higher body mass index, racial and ethnic factors, illnesses, and the removal of the uterus.[48]
Rates of premature menopause have been found to be significantly higher in fraternal and identical twins; approximately 5% of twins reach menopause before the age of 40. The reasons for this are not completely understood. Transplants of ovarian tissue between identical twins have been successful in restoring fertility.
Surgical menopause
Menopause can be surgically induced by bilateral oophorectomy (removal of ovaries),[36] which is often, but not always, done in conjunction with removal of the Fallopian tubes (salpingo-oophorectomy) and uterus (hysterectomy).[49] Cessation of menses as a result of removal of the ovaries is called "surgical menopause". Surgical treatments, such as the removal of ovaries, might cause periods to stop altogether.[50] The sudden and complete drop in hormone levels may produce extreme withdrawal symptoms such as hot flashes, etc. The symptoms of early menopause may be more severe.[50]
Removal of the uterus without removal of the ovaries does not directly cause menopause, although pelvic surgery of this type can often precipitate a somewhat earlier menopause, perhaps because of a compromised blood supply to the ovaries. The time between surgery and possible early menopause is due to the fact that ovaries are still producing hormones.[50]
Mechanism
The menopausal transition, and postmenopause itself, is a natural change, not usually a disease state or a disorder. The main cause of this transition is the natural depletion and aging of the finite amount of oocytes (ovarian reserve). This process is sometimes accelerated by other conditions and is known to occur earlier after a wide range of gynecologic procedures such as hysterectomy (with and without ovariectomy), endometrial ablation and uterine artery embolisation. The depletion of the ovarian reserve causes an increase in circulating follicle-stimulating hormone (FSH) and luteinizing hormone (LH) levels because there are fewer oocytes and follicles responding to these hormones and producing estrogen.
The transition has a variable degree of effects.[51]
The stages of the menopause transition have been classified according to a woman's reported bleeding pattern, supported by changes in the pituitary follicle-stimulating hormone (FSH) levels.[52]
In younger women, during a normal menstrual cycle the ovaries produce estradiol, testosterone and progesterone in a cyclical pattern under the control of FSH and luteinizing hormone (LH), which are both produced by the pituitary gland. During perimenopause (approaching menopause), estradiol levels and patterns of production remain relatively unchanged or may increase compared to young women, but the cycles become frequently shorter or irregular.[53] The often observed increase in estrogen is presumed to be in response to elevated FSH levels that, in turn, is hypothesized to be caused by decreased feedback by inhibin.[54] Similarly, decreased inhibin feedback after hysterectomy is hypothesized to contribute to increased ovarian stimulation and earlier menopause.[55][56]
The menopausal transition is characterized by marked, and often dramatic, variations in FSH and estradiol levels. Because of this, measurements of these hormones are not considered to be reliable guides to a woman's exact menopausal status.[54]
Menopause occurs because of the sharp decrease of estradiol and progesterone production by the ovaries. After menopause, estrogen continues to be produced mostly by aromatase in fat tissues and is produced in small amounts in many other tissues such as ovaries, bone, blood vessels, and the brain where it acts locally.[57] The substantial fall in circulating estradiol levels at menopause impacts many tissues, from brain to skin.
In contrast to the sudden fall in estradiol during menopause, the levels of total and free testosterone, as well as dehydroepiandrosterone sulfate (DHEAS) and androstenedione appear to decline more or less steadily with age. An effect of natural menopause on circulating androgen levels has not been observed.[58] Thus specific tissue effects of natural menopause cannot be attributed to loss of androgenic hormone production.[59]
Hot flashes and other vasomotor and body symptoms accompanying the menopausal transition are associated with estrogen insufficiency and changes that occur in the brain, primarily the hypothalamus and involve complex interplay between the neurotransmitters kisspeptin, neurokinin B, and dynorphin, which are found in ‘KNDy’ neurons in the infundibular nucleus.[60]
Long-term effects of menopause may include osteoporosis, vaginal atrophy as well as changed metabolic profile resulting in increased cardiac and metabolic disease (diabetes) risks.
Ovarian aging
Decreased inhibin feedback after hysterectomy is hypothesized to contribute to increased ovarian stimulation and earlier menopause. Hastened ovarian aging has been observed after endometrial ablation. While it is difficult to prove that these surgeries are causative, it has been hypothesized that the endometrium may be producing endocrine factors contributing to the endocrine feedback and regulation of the ovarian stimulation. Elimination of these factors contributes to faster depletion of the ovarian reserve. Reduced blood supply to the ovaries that may occur as a consequence of hysterectomy and uterine artery embolisation has been hypothesized to contribute to this effect.[55][56]
Impaired DNA repair mechanisms may contribute to earlier depletion of the ovarian reserve during aging.[61] As women age, double-strand breaks accumulate in the DNA of their primordial follicles. Primordial follicles are immature primary oocytes surrounded by a single layer of granulosa cells. An enzyme system is present in oocytes that ordinarily accurately repairs DNA double-strand breaks. This repair system is called "homologous recombinational repair", and it is especially effective during meiosis. Meiosis is the general process by which germ cells are formed in all sexual eukaryotes; it appears to be an adaptation for efficiently removing damages in germ line DNA.[62]
Human primary oocytes are present at an intermediate stage of meiosis, termed prophase I (see Oogenesis). Expression of four key DNA repair genes that are necessary for homologous recombinational repair during meiosis (BRCA1, MRE11, Rad51, and ATM) decline with age in oocytes.[61] This age-related decline in ability to repair DNA double-strand damages can account for the accumulation of these damages, that then likely contributes to the depletion of the ovarian reserve.
Diagnosis
Ways of assessing the impact on women of some of these menopause effects, include the Greene climacteric scale questionnaire,[63] the Cervantes scale[64] and the Menopause rating scale.[23]
Premenopause
Premenopause is a term used to mean the years leading up to the last period, when the levels of reproductive hormones are becoming more variable and lower, and the effects of hormone withdrawal are present.[49] Premenopause starts some time before the monthly cycles become noticeably irregular in timing.[65]
Perimenopause
The term "perimenopause", which literally means "around the menopause", refers to the menopause transition years before the date of the final episode of flow.[1][12][66][67] According to the North American Menopause Society, this transition can last for four to eight years.[68] The Centre for Menstrual Cycle and Ovulation Research describes it as a six- to ten-year phase ending 12 months after the last menstrual period.[69]
During perimenopause, estrogen levels average about 20–30% higher than during premenopause, often with wide fluctuations.[69] These fluctuations cause many of the physical changes during perimenopause as well as menopause, especially during the last 1–2 years of perimenopause (before menopause).[66][70] Some of these changes are hot flashes, night sweats, difficulty sleeping, mood swings, vaginal dryness or atrophy, incontinence, osteoporosis, and heart disease.[69] Perimenopause is also associated with a higher likelihood of depression (affecting from 45 percent to 68 percent of perimenopausal women), which is twice as likely to affect those with a history of depression.[71]
During this period, fertility diminishes but is not considered to reach zero until the official date of menopause. The official date is determined retroactively, once 12 months have passed after the last appearance of menstrual blood.
The menopause transition typically begins between 40 and 50 years of age (average 47.5).[72][73] The duration of perimenopause may be for up to eight years.[73] Women will often, but not always, start these transitions (perimenopause and menopause) about the same time as their mother did.[74]
In some women, menopause may bring about a sense of loss related to the end of fertility. In addition, this change often occurs when other stressors may be present in a woman's life:
- Caring for, and/or the death of, elderly parents
- Empty nest syndrome when children leave home
- The birth of grandchildren, which places people of "middle age" into a new category of "older people" (especially in cultures where being older is a state that is looked down on)
Some research appears to show that melatonin supplementation in perimenopausal women can improve thyroid function and gonadotropin levels, as well as restoring fertility and menstruation and preventing depression associated with menopause.[75]
Postmenopause
The term "postmenopausal" describes women who have not experienced any menstrual flow for a minimum of 12 months, assuming that they have a uterus and are not pregnant or lactating.[49] In women without a uterus, menopause or postmenopause can be identified by a blood test showing a very high FSH level. Thus postmenopause is the time in a woman's life that takes place after her last period or, more accurately, after the point when her ovaries become inactive.
The reason for this delay in declaring postmenopause is that periods are usually erratic at this time of life. Therefore, a reasonably long stretch of time is necessary to be sure that the cycling has ceased. At this point a woman is considered infertile; however, the possibility of becoming pregnant has usually been very low (but not quite zero) for a number of years before this point is reached.
A woman's reproductive hormone levels continue to drop and fluctuate for some time into post-menopause, so hormone withdrawal effects such as hot flashes may take several years to disappear.
A period-like flow during postmenopause, even spotting, may be a sign of endometrial cancer.
Management
Perimenopause is a natural stage of life. It is not a disease or a disorder. Therefore, it does not automatically require any kind of medical treatment. However, in those cases where the physical, mental, and emotional effects of perimenopause are strong enough that they significantly disrupt the life of the woman experiencing them, palliative medical therapy may sometimes be appropriate.
Menopausal Hormone therapy
In the context of the menopause, menopausal hormone therapy (MHT) is the use of estrogen in women without a uterus and estrogen plus progestogen in women who have an intact uterus.[76]
MHT may be reasonable for the treatment of menopausal symptoms, such as hot flashes.[77] It is the most effective treatment option, especially when delivered as a skin patch.[78][79] Its use, however, appears to increase the risk of strokes and blood clots.[80] When used for menopausal symptoms the global recommendation is MHT should be prescribed for a long as there are defined treatment effects and goals for the individual woman.[17]
MHT is also effective for preventing bone loss and osteoporotic fracture,[81] but it is generally recommended only for women at significant risk for whom other therapies are unsuitable.[82]
MHT may be unsuitable for some women, including those at increased risk of cardiovascular disease, increased risk of thromboembolic disease (such as those with obesity or a history of venous thrombosis) or increased risk of some types of cancer.[82] There is some concern that this treatment increases the risk of breast cancer.[83] Women at increased risk of cardiometabolic disease and VTE may be able to use transdermal estradiol which does not appear to increase risks in low to moderate doses.[17]
Adding testosterone to hormone therapy has a positive effect on sexual function in postmenopausal women, although it may be accompanied by hair growth, acne if used in excess. Transdermal testosterone therapy in appropriate dosing is generally safe[84]
Selective estrogen receptor modulators
SERMs are a category of drugs, either synthetically produced or derived from a botanical source, that act selectively as agonists or antagonists on the estrogen receptors throughout the body. The most commonly prescribed SERMs are raloxifene and tamoxifen. Raloxifene exhibits oestrogen agonist activity on bone and lipids, and antagonist activity on breast and the endometrium.[85] Tamoxifen is in widespread use for treatment of hormone sensitive breast cancer. Raloxifene prevents vertebral fractures in postmenopausal, osteoporotic women and reduces the risk of invasive breast cancer.[86]
Other medications
Some of the SSRIs and SNRIs appear to provide some relief from vasomotor symptoms.[5] Low dose paroxetine is the only non-hormonal medication that was FDA-approved to treat moderate-to-severe vasomotor symptoms associated with menopause as of 2016.[87][88] They may, however, be associated with appetite and sleeping problems, constipation and nausea.[5][89]
Gabapentin or clonidine may help but do not work as well as hormone therapy.[5] Gabapentin can decrease the amount of hot flashes. Side effects associated with its use include drowsiness and headaches. Clonidine is used to improve vasomotor symptoms and may be associated with constipation, dizziness, nausea and sleeping problems.[5][89]
Therapy
One review found mindfulness and cognitive behavioural therapy decreases the amount women are affected by hot flashes.[90] Another review found not enough evidence to make a conclusion.[91] A 2018 study found that 85% of study participants reported reduced hot flashes and night sweats when using a climate control system in their beds.[92]
Exercise
Exercise has been thought to reduce postmenopausal symptoms through the increase of endorphin levels, which decrease as estrogen production decreases.[93] Additionally, high BMI is a risk factor for vasomotor symptoms in particular. However, there is insufficient evidence to support the benefits of weight loss for symptom management.[94] There are mixed perspectives on the benefits of physical exercise. While one review found that there was a lack of quality evidence supporting a benefit of exercise,[93] another review recommended regular healthy exercise to reduce comorbidities, improve mood and anxiety symptoms, enhance cognition, and decrease the risk of fractures.[95] Yoga may help with postmenopausal symptoms similar to other exercise.[96] There is insufficient evidence to suggest that relaxation techniques reduce menopausal symptoms.[97]
Alternative medicine
There is no evidence of consistent benefit of alternative therapies for menopausal symptoms despite their popularity.[98]
The effect of soy isoflavones on menopausal symptoms is promising for reduction of hot flashes and vaginal dryness.[18][99] Evidence does not support a benefit from phytoestrogens such as coumestrol,[100] femarelle,[101] or the non-phytoestrogen black cohosh.[18][102] As of 2011 there is no support for herbal or dietary supplements in the prevention or treatment of the mental changes that occur around menopause.[103]
Hypnosis may reduce the severity of hot flashes. In addition, relaxation training with at-home relaxation audiotapes such as deep breathing, paced respiration, and guided imagery may have positive effects on relaxing muscles and reducing stress.[104]
There is no evidence to support the efficacy of acupuncture as a management for menopausal symptoms.[105][98] A 2016 Cochrane review found not enough evidence to show a difference between Chinese herbal medicine and placebo for the vasomotor symptoms.[106]
Other efforts
- Lack of lubrication is a common problem during and after perimenopause. Vaginal moisturizers can help women with overall dryness, and lubricants can help with lubrication difficulties that may be present during intercourse. It is worth pointing out that moisturizers and lubricants are different products for different issues: some women complain that their genitalia are uncomfortably dry all the time, and they may do better with moisturizers. Those who need only lubricants do well using them only during intercourse.
- Low-dose prescription vaginal estrogen products such as estrogen creams are generally a safe way to use estrogen topically, to help vaginal thinning and dryness problems (see vaginal atrophy) while only minimally increasing the levels of estrogen in the bloodstream.
- In terms of managing hot flashes, lifestyle measures such as drinking cold liquids, staying in cool rooms, using fans, removing excess clothing, and avoiding hot flash triggers such as hot drinks, spicy foods, etc., may partially supplement (or even obviate) the use of medications for some women.
- Individual counseling or support groups can sometimes be helpful to handle sad, depressed, anxious or confused feelings women may be having as they pass through what can be for some a very challenging transition time.
- Osteoporosis can be minimized by smoking cessation, adequate vitamin D intake and regular weight-bearing exercise. The bisphosphonate drug alendronate may decrease the risk of a fracture, in women that have both bone loss and a previous fracture and less so for those with just osteoporosis.[107]
- A surgical procedure where a part of one of the ovaries is removed earlier in life and frozen and then over time thawed and returned to the body has been tried. While at least 11 women have undergone the procedure and paid over £6,000, there is no evidence it is safe or effective.[108]
Society and culture
The cultural context within which a woman lives can have a significant impact on the way she experiences the menopausal transition. Menopause has been described as a subjective experience, with social and cultural factors playing a prominent role in the way menopause is experienced and perceived.
The word menopause was invented by French doctors at the beginning of the nineteenth century. Some of them noted that peasant women had no complaints about the end of menses, while urban middle-class women had many troubling symptoms. Doctors at this time considered the symptoms to be the result of urban lifestyles of sedentary behaviour, alcohol consumption, too much time indoors, and over-eating, with a lack of fresh fruit and vegetables.[109] Within the United States, social location affects the way women perceive menopause and its related biological effects. Research indicates that whether a woman views menopause as a medical issue or an expected life change is correlated with her socio-economic status.[110] The paradigm within which a woman considers menopause influences the way she views it: Women who understand menopause as a medical condition rate it significantly more negatively than those who view it as a life transition or a symbol of aging.[111]
Ethnicity and geography play roles in the experience of menopause. American women of different ethnicities report significantly different types of menopausal effects. One major study found Caucasian women most likely to report what are sometimes described as psychosomatic symptoms, while African-American women were more likely to report vasomotor symptoms.[112]
It seems that Japanese women experience menopause effects, or konenki, in a different way from American women.[113] Japanese women report lower rates of hot flashes and night sweats; this can be attributed to a variety of factors, both biological and social. Historically, konenki was associated with wealthy middle-class housewives in Japan, i.e., it was a "luxury disease" that women from traditional, inter-generational rural households did not report. Menopause in Japan was viewed as a symptom of the inevitable process of aging, rather than a "revolutionary transition", or a "deficiency disease" in need of management.[113]
In Japanese culture, reporting of vasomotor symptoms has been on the increase, with research conducted in 2005 finding that of 140 Japanese participants, hot flashes were prevalent in 22.1%.[114] This was almost double that of 20 years prior.[115] Whilst the exact cause for this is unknown, possible contributing factors include significant dietary changes, increased medicalisation of middle-aged women and increased media attention on the subject.[115] However, reporting of vasomotor symptoms is still significantly lower than North America.[116]
Additionally, while most women in the United States apparently have a negative view of menopause as a time of deterioration or decline, some studies seem to indicate that women from some Asian cultures have an understanding of menopause that focuses on a sense of liberation and celebrates the freedom from the risk of pregnancy.[117] Diverging from these conclusions, one study appeared to show that many American women "experience this time as one of liberation and self-actualization".[118]
Etymology
Menopause literally means the "end of monthly cycles" (the end of monthly periods or menstruation), from the Greek word pausis ("pause") and mēn ("month"). This is a medical coinage; the Greek word for menses is actually different. In Ancient Greek, the menses were described in the plural, ta emmēnia, ("the monthlies"), and its modern descendant has been clipped to ta emmēna. The Modern Greek medical term is emmenopausis in Katharevousa or emmenopausi in Demotic Greek.
The word "menopause" was coined specifically for human females, where the end of fertility is traditionally indicated by the permanent stopping of monthly menstruations. However, menopause exists in some other animals, many of which do not have monthly menstruation;[119] in this case, the term means a natural end to fertility that occurs before the end of the natural lifespan.
Menopause in popular culture
In recent years celebrities have spoken out about their experiences of the menopause which has led to it becoming less of a taboo as it has boosted awareness of the debilitating symptoms.
This has led to TV shows running features on the menopause to help women experiencing symptoms. In the UK Lorraine Kelly has been an advocate for getting women to speak about their experiences including sharing her own. This has led to an increase in women seeking treatment such as HRT[120]
Evolutionary rationale
Few animals have a menopause: humans are joined by just four other species in which females live substantially longer than their ability to reproduce. The others are all cetaceans: beluga whales, narwhals, orcas and short-finned pilot whales.[121] Various theories have been suggested that attempt to suggest evolutionary benefits to the human species stemming from the cessation of women's reproductive capability before the end of their natural lifespan. Explanations can be categorized as adaptive and non-adaptive:
Non-adaptive hypotheses
The high cost of female investment in offspring may lead to physiological deteriorations that amplify susceptibility to becoming infertile. This hypothesis suggests the reproductive lifespan in humans has been optimized, but it has proven more difficult in females and thus their reproductive span is shorter. If this hypothesis were true, however, age at menopause should be negatively correlated with the amount of energy expended to maintain the reproductive organs,[122] and the available data does not support this.[123]
A recent increase in female longevity due to improvements in the standard of living and social care has also been suggested.[124] It is difficult for selection, however, to favor aid to offspring from parents and grandparents.[125] Irrespective of living standards, adaptive responses are limited by physiological mechanisms. In other words, senescence is programmed and regulated by specific genes.[126]
Early human selection shadow
While it is fairly common for extant hunter-gatherers to live past age 50 provided that they survive childhood, fossil evidence shows that mortality in adults has decreased over the last 30,000 to 50,000 years and that it was extremely unusual for early Homo sapiens to live to age 50. This discovery has led some biologists to argue that there was no selection for or against menopause at the time at which the ancestor of all modern humans lived in Africa, suggesting that menopause is instead a random evolutionary effect of a selection shadow regarding aging in early Homo sapiens. It is also argued that since the population fraction of post-menopausal women in early Homo sapiens was so low, menopause had no evolutionary effect on mate selection or social behaviors related to mate selection.[127][128]
"Survival of the fittest" hypothesis
This hypothesis suggests that younger mothers and offspring under their care will fare better in a difficult and predatory environment because a younger mother will be stronger and more agile in providing protection and sustenance for herself and a nursing baby. The various biological factors associated with menopause had the effect of male members of the species investing their effort with the most viable of potential female mates.[129]
A problem with this hypothesis is that, if true, we would expect to see menopause exhibited among many species in the animal kingdom,[119] and another problem is that in the case of extended child development, even a female who was relatively young, still agile, and attractive when producing a child would lose future support from her male partner due to him seeking out fertile mates when she reaches menopause, while the child is still not independent. This would be counterproductive to the supposed adaptation of getting male support, as it would significantly decrease the survival for children produced over much of the female's fertile and agile life, unless children were raised in ways that did not rely on support from a male partner, which would eliminate the supposed evolutionary benefit anyway.[130][131]
Young female preference hypothesis
The young female preference hypothesis proposes that changes in male preferences for younger mates allowed late-age acting fertility mutations to accumulate in females without any evolutionary penalty, giving rise to menopause. A computer model was constructed to test this hypothesis, and showed that it was feasible.[132] However, in order for deleterious mutations that affect fertility past roughly age fifty to accumulate, human maximum lifespan had to first be extended to about its present value. As of 2016 it was unclear if there has been sufficient time since that happened for such an evolutionary process to occur.[133]
Male-biased philopatry hypothesis
The male-biased philopatry theory proposes that if human social groups were originally based around men leaving their birth communities more frequently than women, then this leads to increased relatedness to the group in relation to female age, making inclusive fitness benefits older females receive from helping the group greater than what they would receive from continued reproduction, which in turn eventually led to the evolution of menopause.[134] In a pattern of male-biased dispersal and local mating, the relatedness of the individuals in the group decreases with female age, leading to a decrease in kin selection with female age.[134] This occurs because a female will stay with her father in her birth community throughout life, initially being closely related to the males and females. Females are born and stay in the group, so relatedness to the females stays about the same. However, throughout time, the older male relatives will die and any sons she gives birth to will disperse, so that local relatedness to males, and therefore the whole group, declines. The situation is reversed in species where males are philopatric and either females disperse, or mating is non-local.[134] Under these conditions, a female's reproductive life begins away from her father and paternal relatives because she was either born into a new group from non-local mating or because she dispersed. In the case of female-biased dispersal, the female is initially equally unrelated with every individual in the group, and with non-local mating, the female is closely related to the females of the group, but not the males since her paternal relatives are in another group. As she gives birth, her sons will stay with her, increasing her relatedness to males in the group over time and thus her relatedness with the overall group. The common feature that connects these two otherwise different behaviors is male-biased philopatry, which leads to an increase in kin selection with female age.
While not conclusive, evidence does exist to support the idea that female-biased dispersal existed in pre-modern humans. The closest living relatives to humans, chimpanzees, bonobos, and both mountain gorillas and western lowland gorillas, are female-biased dispersers.[135] Analysis of sex specific genetic material, the non-recombining portions of the Y chromosome and mitochondrial DNA, show evidence of a prevalence of female-biased dispersal as well; however, these results could also be affected by the effective breeding numbers of males and females in local populations.[136] Evidence of female-biased dispersion in hunter-gatherers is not definitive, with some studies supporting the idea,[135] and others suggesting there is no strong bias towards either sex.[137] In orcas, both sexes mate non-locally with members of a different pod but return to the pod after copulation.[138] Demographic data shows that a female's mean relatedness to the group does increase over time due to increasing relatedness to males.[139] While less well-studied, there is evidence that short-finned pilot whales, another menopausal species, also display this behavior.[140] However, mating behavior that increases local relatedness with female age is prevalent in non-menopausal species,[135] making it unlikely that it is the only factor that determines if menopause will evolve in a species.
Mother hypothesis
The mother hypothesis suggests that menopause was selected for humans because of the extended development period of human offspring and high costs of reproduction so that mothers gain an advantage in reproductive fitness by redirecting their effort from new offspring with a low survival chance to existing children with a higher survival chance.[141]
Grandmother hypothesis
The Grandmother hypothesis suggests that menopause was selected for humans because it promotes the survival of grandchildren. According to this hypothesis, post-reproductive women feed and care for children, adult nursing daughters, and grandchildren whose mothers have weaned them. Human babies require large and steady supplies of glucose to feed the growing brain. In infants in the first year of life, the brain consumes 60% of all calories, so both babies and their mothers require a dependable food supply. Some evidence suggests that hunters contribute less than half the total food budget of most hunter-gatherer societies, and often much less than half, so that foraging grandmothers can contribute substantially to the survival of grandchildren at times when mothers and fathers are unable to gather enough food for all of their children. In general, selection operates most powerfully during times of famine or other privation. So although grandmothers might not be necessary during good times, many grandchildren cannot survive without them during times of famine.
Post-reproductive female orcas tend to lead their pods, especially during years of food scarcity.[142] Furthermore, the increased mortality risk of an orca due to losing a grandmother is stronger in years of food scarcity[143]
Analysis of historical data found that the length of a female's post-reproductive lifespan was reflected in the reproductive success of her offspring and the survival of her grandchildren.[144] Another study found comparative effects but only in the maternal grandmother—paternal grandmothers had a detrimental effect on infant mortality (probably due to paternity uncertainty).[145] Differing assistance strategies for maternal and paternal grandmothers have also been demonstrated. Maternal grandmothers concentrate on offspring survival, whereas paternal grandmothers increase birth rates.[146]
Some believe variations on the mother, or grandmother effect fail to explain longevity with continued spermatogenesis in males (oldest verified paternity is 94 years, 35 years beyond the oldest documented birth attributed to females).[147] Notably, the survival time past menopause is roughly the same as the maturation time for a human child. That a mother's presence could aid in the survival of a developing child, while an unidentified father's absence might not have affected survival, could explain the paternal fertility near the end of the father's lifespan.[148] A man with no certainty of which children are his may merely attempt to father additional children, with support of existing children present but small. Note the existence of partible paternity supporting this.[149] Some argue that the mother and grandmother hypotheses fail to explain the detrimental effects of losing ovarian follicular activity, such as osteoporosis, osteoarthritis, Alzheimer's disease and coronary artery disease.[150]
The theories discussed above assume that evolution directly selected for menopause. Another theory states that menopause is the byproduct of the evolutionary selection for follicular atresia, a factor that causes menopause. Menopause results from having too few ovarian follicles to produce enough estrogen to maintain the ovarian-pituitary-hypothalamic loop, which results in the cessation of menses and the beginning of menopause. Human females are born with approximately a million oocytes, and approximately 400 oocytes are lost to ovulation throughout life.[151][152]
Reproductive conflict hypothesis
In social vertebrates, the sharing of resources among the group places limits on how many offspring can be produced and supported by members of the group. This creates a situation in which each female must compete with others of the group to ensure they are the one that reproduces.[153] The reproductive conflict hypothesis proposes that this female reproductive conflict favors the cessation of female reproductive potential in older age to avoid reproductive conflict, increasing the older female's fitness through inclusive benefits. Female-biased dispersal or non-local mating leads to an increase in relatedness to the social group with female age.[134] In the human case of female-biased dispersal, when a young female enters a new group, she is not related to any individual and she reproduces to produce an offspring with a relatedness of 0.5. An older female could also choose to reproduce, producing an offspring with a relatedness of 0.5, or she could refrain from reproducing and allow another pair to reproduce. Because her relatedness to males in the group is high, there is a fair probability that the offspring will be her grandchild with a relatedness of 0.25. The younger female experiences no cost to her inclusive fitness from using the resources necessary to successfully rear offspring since she is not related to members of the group, but there is a cost for the older female. As a result, the younger female has the advantage in reproductive competition. Although a female orca born into a social group is related to some members of the group, the whale case of non-local mating leads to similar outcomes because the younger female relatedness to the group as a whole is less than the relatedness of the older female. This behavior makes more likely the cessation of reproduction late in life to avoid reproductive conflict with younger females.
Research using both human and orca demographic data has been published that supports the role of reproductive conflict in the evolution of menopause. Analysis of demographic data from pre-industrial Finnish populations found significant reductions in offspring survivorship when mothers-in-laws and daughters-in-laws had overlapping births,[154] supporting the idea that avoiding reproductive conflict is beneficial to offspring survivorship. Humans, more so than other primates, rely on food sharing for survival,[155] so the large survivorship reduction values could be caused by a straining of community resources. Avoiding such straining is a possible explanation for why the reproductive overlap seen in humans is much lower than other primates.[156] Food sharing is also prevalent among another menopausal species, orcas.[157] Reproductive conflict has also been observed in orcas, with increased calf mortality seen when reproductive overlap between a younger and older generational female occurred.[139]
Other animals
Menopause in the animal kingdom appears to be uncommon, but the presence of this phenomenon in different species has not been thoroughly researched. Life histories show a varying degree of senescence; rapid senescing organisms (e.g., Pacific salmon and annual plants) do not have a post-reproductive life-stage. Gradual senescence is exhibited by all placental mammalian life histories.
Menopause has been observed in several species of nonhuman primates,[119] including rhesus monkeys[158] and chimpanzees.[159] Some research suggests that wild chimpanzees do not experience menopause, as their fertility declines are associated with declines in overall health.[160] Menopause also has been reported in a variety of other vertebrate species including elephants,[161] short-finned pilot whales,[162] orcas,[163] narwhals,[164] beluga whales,[164] and the guppy.[165] However, with the exception of the short-finned pilot whale, killer whale, narwhals, and beluga whales,[164] such examples tend to be from captive individuals, and thus they are not necessarily representative of what happens in natural populations in the wild.
Dogs do not experience menopause; the canine estrus cycle simply becomes irregular and infrequent. Although older female dogs are not considered good candidates for breeding, offspring have been produced by older animals.[166] Similar observations have been made in cats.[167]
See also
- European Menopause and Andropause Society
- Menopause in the workplace
- Menopause in incarceration
- Pregnancy over age 50
References
- "Menopause". Office on Women's Health. 22 February 2021. Retrieved 20 October 2022.
{{cite web}}: CS1 maint: url-status (link) - "Menopause Basics". Office on Women's Health. 22 February 2021. Retrieved 20 October 2022.
{{cite web}}: CS1 maint: url-status (link) - "Menopause Baics". Office on Women's Health. 22 February 2021. Retrieved 20 October 2022.
{{cite web}}: CS1 maint: url-status (link) - "What are the treatments for other symptoms of menopause?". Eunice Kennedy Shriver National Institute of Child Health and Human Development. 28 June 2013. Archived from the original on 20 March 2015. Retrieved 8 March 2015.
- Krause MS, Nakajima ST (March 2015). "Hormonal and nonhormonal treatment of vasomotor symptoms". Obstetrics and Gynecology Clinics of North America. 42 (1): 163–179. doi:10.1016/j.ogc.2014.09.008. PMID 25681847.
- "Menopause: Overview". National Library of Medicine - Bookshelf. Institute for Quality & Efficiency in Health Care. 2 July 2020. Retrieved 20 October 2022.
{{cite web}}: CS1 maint: url-status (link) - Takahashi TA, Johnson KM (May 2015). "Menopause". The Medical Clinics of North America. 99 (3): 521–534. doi:10.1016/j.mcna.2015.01.006. PMID 25841598.
- Sievert LL (2006). Menopause: a biocultural perspective ([Online-Ausg.] ed.). New Brunswick, N.J.: Rutgers University Press. p. 81. ISBN 9780813538563. Archived from the original on 10 September 2017.
- Davis SR, Lambrinoudaki I, Lumsden M, Mishra GD, Pal L, Rees M, et al. (April 2015). "Menopause". Nature Reviews. Disease Primers. 1 (1): 15004. doi:10.1038/nrdp.2015.4. PMID 27188659.
- International position paper on women's health and menopause : a comprehensive approach. DIANE Publishing. 2002. p. 36. ISBN 9781428905214. Archived from the original on 10 September 2017.
- "Menopause Symptoms and Relief". Office on Women's Health. 22 February 2021. Retrieved 20 October 2022.
{{cite web}}: CS1 maint: url-status (link) - "What Is Menopause?". National Institute on Aging. 30 September 2021. Retrieved 20 October 2022.
{{cite web}}: CS1 maint: url-status (link) - Warren M, Soares CN, eds. (2009). The menopausal transition: interface between gynecology and psychiatry ([Online-Ausg.] ed.). Basel: Karger. p. 73. ISBN 978-3805591010.
- "Menopause & Chemotherapy - Managing Side Effects - Chemocare". chemocare.com. Retrieved 20 October 2022.
- "How do health care providers diagnose menopause?". Eunice Kennedy Shriver National Institute of Child Health and Human Development. 6 May 2013. Archived from the original on 2 April 2015. Retrieved 8 March 2015.
- Wood J. "9". Dynamics of Human Reproduction: Biology, Biometry, Demography. Transaction Publishers. p. 401. ISBN 9780202365701. Archived from the original on 10 September 2017.
- Davis SR, Baber RJ (August 2022). "Treating menopause - MHT and beyond". Nature Reviews. Endocrinology. 18 (8): 490–502. doi:10.1038/s41574-022-00685-4. PMID 35624141. S2CID 249069157.
- Franco OH, Chowdhury R, Troup J, Voortman T, Kunutsor S, Kavousi M, et al. (June 2016). "Use of Plant-Based Therapies and Menopausal Symptoms: A Systematic Review and Meta-analysis". JAMA. 315 (23): 2554–2563. doi:10.1001/jama.2016.8012. PMID 27327802.
- Hoffman B (2012). Williams Gynecology. New York: McGraw-Hill Medical. pp. 555–56. ISBN 9780071716727.
- Dreisler E, Poulsen LG, Antonsen SL, Ceausu I, Depypere H, Erel CT, Lambrinoudaki I, Pérez-López FR, Simoncini T, Tremollieres F, Rees M, Ulrich LG (June 2013). "EMAS clinical guide: assessment of the endometrium in peri and postmenopausal women". Maturitas. 75 (2): 181–90. doi:10.1016/j.maturitas.2013.03.011. PMID 23619009.
- "Red in the Face". NIH News in Health. 27 June 2017. Retrieved 31 March 2021.
- Pérez-López FR, Cuadros JL, Fernández-Alonso AM, Chedraui P, Sánchez-Borrego R, Monterrosa-Castro A (December 2012). "Urinary incontinence, related factors and menopause-related quality of life in mid-aged women assessed with the Cervantes Scale". Maturitas. 73 (4): 369–72. doi:10.1016/j.maturitas.2012.09.004. PMID 23041251.
- Chedraui P, Pérez-López FR, Mendoza M, Leimberg ML, Martínez MA, Vallarino V, Hidalgo L (January 2010). "Factors related to increased daytime sleepiness during the menopausal transition as evaluated by the Epworth sleepiness scale". Maturitas. 65 (1): 75–80. doi:10.1016/j.maturitas.2009.11.003. PMID 19945237.
- Arakane M, Castillo C, Rosero MF, Peñafiel R, Pérez-López FR, Chedraui P (June 2011). "Factors relating to insomnia during the menopausal transition as evaluated by the Insomnia Severity Index". Maturitas. 69 (2): 157–61. doi:10.1016/j.maturitas.2011.02.015. PMID 21444163.
- Monterrosa-Castro A, Marrugo-Flórez M, Romero-Pérez I, Chedraui P, Fernández-Alonso AM, Pérez-López FR (April 2013). "Prevalence of insomnia and related factors in a large mid-aged female Colombian sample". Maturitas. 74 (4): 346–51. doi:10.1016/j.maturitas.2013.01.009. PMID 23391501.
- Llaneza P, García-Portilla MP, Llaneza-Suárez D, Armott B, Pérez-López FR (February 2012). "Depressive disorders and the menopause transition". Maturitas. 71 (2): 120–30. doi:10.1016/j.maturitas.2011.11.017. PMID 22196311.
- Panay N, Briggs P, Kovacs G (20 August 2015). "Memory and Mood in the Menopause". Managing the Menopause: 21st Century Solutions. Cambridge University Press. ISBN 9781316352717.
- Birkhaeuser M, Genazzani AR (30 January 2018). Pre-Menopause, Menopause and Beyond: Volume 5: Frontiers in Gynecological Endocrinology. Springer. pp. 38–39. ISBN 9783319635408.
- Papadakis MA, McPhee SJ, Rabow MW (11 September 2017). Current Medical Diagnosis and Treatment 2018, 57th Edition. McGraw Hill Professional. p. 1212. ISBN 9781259861499.
- Nappi RE, Chedraui P, Lambrinoudaki I, Simoncini T (June 2022). "Menopause: a cardiometabolic transition". The Lancet. Diabetes & Endocrinology. 10 (6): 442–456. doi:10.1016/S2213-8587(22)00076-6. PMID 35525259. S2CID 248561432.
- Thurston RC (April 2018). "Vasomotor symptoms: natural history, physiology, and links with cardiovascular health". Climacteric. 21 (2): 96–100. doi:10.1080/13697137.2018.1430131. PMC 5902802. PMID 29390899.
- Stevenson JC, Collins P, Hamoda H, Lambrinoudaki I, Maas AH, Maclaran K, Panay N (October 2021). "Cardiometabolic health in premature ovarian insufficiency". Climacteric. 24 (5): 474–480. doi:10.1080/13697137.2021.1910232. PMID 34169795. S2CID 235634591.
- Souza HC, Tezini GC (September 2013). "Autonomic Cardiovascular Damage during Post-menopause: the Role of Physical Training". Aging and Disease. 4 (6): 320–328. doi:10.14336/AD.2013.0400320. PMC 3843649. PMID 24307965.
- ESHRE Capri Workshop Group (2011). "Perimenopausal risk factors and future health". Human Reproduction Update. 17 (5): 706–717. doi:10.1093/humupd/dmr020. PMID 21565809.
- Warming L, Hassager C, Christiansen C (1 February 2002). "Changes in bone mineral density with age in men and women: a longitudinal study". Osteoporosis International. 13 (2): 105–112. doi:10.1007/s001980200001. PMID 11905520. S2CID 618576.
- "Early or premature menopause | Office on Women's Health". www.womenshealth.gov. Retrieved 21 October 2022.
- "Gynaecologic Problems: Menopausal Problems". Health on the Net Foundation. Archived from the original on 25 February 2021. Retrieved 22 February 2012.
- Morabia A, Costanza MC (December 1998). "International variability in ages at menarche, first livebirth, and menopause. World Health Organization Collaborative Study of Neoplasia and Steroid Contraceptives". American Journal of Epidemiology. 148 (12): 1195–205. doi:10.1093/oxfordjournals.aje.a009609. PMID 9867266.
- Ringa V (2000). "Menopause and treatments". Quality of Life Research. 9 (6): 695–707. doi:10.1023/A:1008913605129. JSTOR 4036942. S2CID 22496307.
- Podfigurna-Stopa A, Czyzyk A, Grymowicz M, Smolarczyk R, Katulski K, Czajkowski K, Meczekalski B (September 2016). "Premature ovarian insufficiency: the context of long-term effects". Journal of Endocrinological Investigation. 39 (9): 983–90. doi:10.1007/s40618-016-0467-z. PMC 4987394. PMID 27091671.
- Tersigni C, Castellani R, de Waure C, Fattorossi A, De Spirito M, Gasbarrini A, Scambia G, Di Simone N (2014). "Celiac disease and reproductive disorders: meta-analysis of epidemiologic associations and potential pathogenic mechanisms". Human Reproduction Update. 20 (4): 582–93. doi:10.1093/humupd/dmu007. PMID 24619876.
- Lasa JS, Zubiaurre I, Soifer LO (2014). "Risk of infertility in patients with celiac disease: a meta-analysis of observational studies". Arquivos de Gastroenterologia. 51 (2): 144–50. doi:10.1590/S0004-28032014000200014. PMID 25003268.
- Davis SR, Baber RJ (August 2022). "Treating menopause - MHT and beyond". Nature Reviews. Endocrinology. 18 (8): 490–502. doi:10.1038/s41574-022-00685-4. PMID 35624141. S2CID 249069157.
- Healthline (2 July 2014). "What causes early menopause". Healthline. Archived from the original on 28 September 2013.
- Laissue P (August 2015). "Aetiological coding sequence variants in non-syndromic premature ovarian failure: From genetic linkage analysis to next generation sequencing". Molecular and Cellular Endocrinology (Review). 411: 243–57. doi:10.1016/j.mce.2015.05.005. PMID 25960166.
- Fenton AJ (2015). "Premature ovarian insufficiency: Pathogenesis and management". Journal of Mid-Life Health (Review). 6 (4): 147–53. doi:10.4103/0976-7800.172292. PMC 4743275. PMID 26903753.
- Kalantaridou SN, Davis SR, Nelson LM (December 1998). "Premature ovarian failure". Endocrinology and Metabolism Clinics of North America. 27 (4): 989–1006. doi:10.1016/s0889-8529(05)70051-7. PMID 9922918.
- Bucher, et al. 1930
- Harlow SD, Gass M, Hall JE, Lobo R, Maki P, Rebar RW, Sherman S, Sluss PM, de Villiers TJ (April 2012). "Executive summary of the Stages of Reproductive Aging Workshop + 10: addressing the unfinished agenda of staging reproductive aging". Fertility and Sterility. 97 (4): 843–51. doi:10.1016/j.fertnstert.2012.01.128. PMC 3340904. PMID 22341880.
- "Early or premature menopause". Womenshealth.gov. 12 July 2017. Retrieved 7 November 2018.
- Cohen LS, Soares CN, Vitonis AF, Otto MW, Harlow BL (April 2006). "Risk for new onset of depression during the menopausal transition: the Harvard study of moods and cycles". Archives of General Psychiatry. The Harvard Study of Moods and Cycles. 63 (4): 385–90. doi:10.1001/archpsyc.63.4.385. PMID 16585467.
- Soules MR, Sherman S, Parrott E, Rebar R, Santoro N, Utian W, Woods N (December 2001). "Executive summary: Stages of Reproductive Aging Workshop (STRAW)". Climacteric. 4 (4): 267–72. doi:10.1080/cmt.4.4.267.272. PMID 11770182. S2CID 28673617.
- Prior JC (August 1998). "Perimenopause: the complex endocrinology of the menopausal transition". Endocrine Reviews. 19 (4): 397–428. doi:10.1210/edrv.19.4.0341. PMID 9715373.
- Burger HG (January 1994). "Diagnostic role of follicle-stimulating hormone (FSH) measurements during the menopausal transition—an analysis of FSH, oestradiol and inhibin". European Journal of Endocrinology. 130 (1): 38–42. doi:10.1530/eje.0.1300038. PMID 8124478.
- Nahás E, Pontes A, Traiman P, NahásNeto J, Dalben I, De Luca L (April 2003). "Inhibin B and ovarian function after total abdominal hysterectomy in women of reproductive age". Gynecological Endocrinology. 17 (2): 125–31. doi:10.1080/713603218. PMID 12737673.
- Petri Nahás EA, Pontes A, Nahas-Neto J, Borges VT, Dias R, Traiman P (February 2005). "Effect of total abdominal hysterectomy on ovarian blood supply in women of reproductive age". Journal of Ultrasound in Medicine. 24 (2): 169–74. doi:10.7863/jum.2005.24.2.169. PMID 15661947. S2CID 30259666.
- Simpson ER, Davis SR (November 2001). "Minireview: aromatase and the regulation of estrogen biosynthesis—some new perspectives". Endocrinology. 142 (11): 4589–94. doi:10.1210/endo.142.11.8547. PMID 11606422.
- Davison SL, Bell R, Donath S, Montalto JG, Davis SR (July 2005). "Androgen levels in adult females: changes with age, menopause, and oophorectomy". The Journal of Clinical Endocrinology and Metabolism. 90 (7): 3847–53. doi:10.1210/jc.2005-0212. PMID 15827095.
- Fogle RH, Stanczyk FZ, Zhang X, Paulson RJ (August 2007). "Ovarian androgen production in postmenopausal women". The Journal of Clinical Endocrinology and Metabolism. 92 (8): 3040–3. doi:10.1210/jc.2007-0581. PMID 17519304.
- Skorupskaite K, George JT, Anderson RA (2014). "The kisspeptin-GnRH pathway in human reproductive health and disease". Human Reproduction Update. 20 (4): 485–500. doi:10.1093/humupd/dmu009. PMC 4063702. PMID 24615662.
- Titus S, Li F, Stobezki R, Akula K, Unsal E, Jeong K, Dickler M, Robson M, Moy F, Goswami S, Oktay K (February 2013). "Impairment of BRCA1-related DNA double-strand break repair leads to ovarian aging in mice and humans". Science Translational Medicine. 5 (172): 172ra21. doi:10.1126/scitranslmed.3004925. PMC 5130338. PMID 23408054.
- Brandl E, Mirzaghaderi G (September 2016). "The evolution of meiotic sex and its alternatives". Proceedings of the Royal Society B: Biological Sciences. Proc Biol Sci. 283 (1838). doi:10.1098/rspb.2016.1221. PMC 5031655. PMID 27605505.
- Greene JG (May 1998). "Constructing a standard climacteric scale". Maturitas. 29 (1): 25–31. doi:10.1016/s0378-5122(98)00025-5. PMID 9643514.
- Monterrosa-Castro A, Romero-Pérez I, Marrugo-Flórez M, Fernández-Alonso AM, Chedraui P, Pérez-López FR (August 2012). "Quality of life in a large cohort of mid-aged Colombian women assessed using the Cervantes Scale". Menopause. 19 (8): 924–30. doi:10.1097/gme.0b013e318247908d. PMID 22549166. S2CID 19201297.
- Schneider HP, Naftolin F (2005). Climacteric medicine where do we go?. London: Taylor & Francis. p. 28. ISBN 9780203024966.
- "What Is Perimenopause?". WebMD. Retrieved 6 October 2018.
- "Perimenopause – Symptoms and causes". Mayo Clinic. Retrieved 6 October 2018.
- "Menopause 101". A primer for the perimenopausal. The North American Menopause Society. Archived from the original on 10 April 2013. Retrieved 11 April 2013.
- Prior J. "Perimenopause". Centre for Menstrual Cycle and Ovulation Research (CeMCOR). Archived from the original on 25 February 2013. Retrieved 10 May 2013.
- Chichester M, Ciranni P (August–September 2011). "Approaching menopause (but not there yet!): caring for women in midlife". Nursing for Women's Health. 15 (4): 320–4. doi:10.1111/j.1751-486X.2011.01652.x. PMID 21884497.
- Gilbert N (27 January 2022). "When depression sneaks up on menopause". Knowable Magazine. doi:10.1146/knowable-012722-1. Retrieved 17 May 2022.
- Hurst BS (2011). Disorders of menstruation. Chichester, West Sussex: Wiley-Blackwell. ISBN 9781444391817.
- McNamara M, Batur P, DeSapri KT (February 2015). "In the clinic. Perimenopause". Annals of Internal Medicine. 162 (3): ITC1–15. doi:10.7326/AITC201502030. PMID 25643316.
- Kessenich C. "Inevitable Menopause". Archived from the original on 2 November 2013. Retrieved 11 April 2013.
- Bellipanni G, DI Marzo F, Blasi F, Di Marzo A (December 2005). "Effects of melatonin in perimenopausal and menopausal women: our personal experience". Annals of the New York Academy of Sciences. 1057 (1): 393–402. Bibcode:2005NYASA1057..393B. doi:10.1196/annals.1356.030. PMID 16399909. S2CID 25213110.
- The Woman's Health Program Monash University, Oestrogen and Progestin as Hormone Therapy Archived 11 July 2012 at the Wayback Machine
- North American Menopause Society (March 2010). "Estrogen and progestogen use in postmenopausal women: 2010 position statement of The North American Menopause Society". Menopause. 17 (2): 242–255. doi:10.1097/gme.0b013e3181d0f6b9. PMID 20154637. S2CID 24806751.
- North American Menopause Society (March 2012). "The 2012 hormone therapy position statement of: The North American Menopause Society". Menopause. 19 (3): 257–71. doi:10.1097/GME.0000000000000921. PMC 3443956. PMID 22367731.
- Sarri G, Pedder H, Dias S, Guo Y, Lumsden MA (September 2017). "Vasomotor symptoms resulting from natural menopause: a systematic review and network meta-analysis of treatment effects from the National Institute for Health and Care Excellence guideline on menopause" (PDF). BJOG. 124 (10): 1514–1523. doi:10.1111/1471-0528.14619. PMID 28276200. S2CID 206909766.
- Boardman HM, Hartley L, Eisinga A, Main C, Roqué i Figuls M, Bonfill Cosp X, Gabriel Sanchez R, Knight B (March 2015). "Hormone therapy for preventing cardiovascular disease in post-menopausal women". The Cochrane Database of Systematic Reviews (3): CD002229. doi:10.1002/14651858.CD002229.pub4. PMID 25754617.
- de Villiers TJ, Stevenson JC (June 2012). "The WHI: the effect of hormone replacement therapy on fracture prevention". Climacteric. 15 (3): 263–6. doi:10.3109/13697137.2012.659975. PMID 22612613. S2CID 40340985.
- Marjoribanks J, Farquhar C, Roberts H, Lethaby A, Lee J (January 2017). "Long-term hormone therapy for perimenopausal and postmenopausal women". The Cochrane Database of Systematic Reviews. 1: CD004143. doi:10.1002/14651858.CD004143.pub5. PMC 6465148. PMID 28093732.
- Chlebowski RT, Anderson GL (April 2015). "Menopausal hormone therapy and breast cancer mortality: clinical implications". Therapeutic Advances in Drug Safety. 6 (2): 45–56. doi:10.1177/2042098614568300. PMC 4406918. PMID 25922653.
- Davis SR, Baber R, Panay N, Bitzer J, Cerdas Perez S, Islam RM, et al. (October 2019). "Global Consensus Position Statement on the Use of Testosterone Therapy for Women". Climacteric. 22 (5): 429–434. doi:10.1080/13697137.2019.1637079. PMID 31474158. S2CID 201713094.
- Davis SR, Dinatale I, Rivera-Woll L, Davison S (May 2005). "Postmenopausal hormone therapy: from monkey glands to transdermal patches". The Journal of Endocrinology. 185 (2): 207–22. doi:10.1677/joe.1.05847. PMID 15845914.
- Bevers TB (September 2007). "The STAR trial: evidence for raloxifene as a breast cancer risk reduction agent for postmenopausal women". Journal of the National Comprehensive Cancer Network. 5 (8): 719–24. doi:10.6004/jnccn.2007.0073. PMID 17927929.
- Orleans RJ, Li L, Kim MJ, Guo J, Sobhan M, Soule L, Joffe HV (May 2014). "FDA approval of paroxetine for menopausal hot flushes". The New England Journal of Medicine. 370 (19): 1777–9. doi:10.1056/NEJMp1402080. PMID 24806158.
- Hill DA, Crider M, Hill SR (December 2016). "Hormone Therapy and Other Treatments for Symptoms of Menopause". American Family Physician. 94 (11): 884–889. PMID 27929271.
- Potter B, Schrager S, Dalby J, Torell E, Hampton A (December 2018). "Menopause". Primary Care. Women's Health. 45 (4): 625–641. doi:10.1016/j.pop.2018.08.001. PMID 30401346. S2CID 239485855.
- van Driel CM, Stuursma A, Schroevers MJ, Mourits MJ, de Bock GH (February 2019). "Mindfulness, cognitive behavioural and behaviour-based therapy for natural and treatment-induced menopausal symptoms: a systematic review and meta-analysis". BJOG. 126 (3): 330–339. doi:10.1111/1471-0528.15153. PMC 6585818. PMID 29542222.
- Goldstein KM, Shepherd-Banigan M, Coeytaux RR, McDuffie JR, Adam S, Befus D, et al. (April 2017). "Use of mindfulness, meditation and relaxation to treat vasomotor symptoms". Climacteric. 20 (2): 178–182. doi:10.1080/13697137.2017.1283685. PMID 28286985. S2CID 10446084.
- "BedJet is Clinically Proven Treatment for Menopausal Sleep Disturbances". 9 October 2018. Retrieved 24 November 2019.
- Hickey M, Szabo RA, Hunter MS (November 2017). "Non-hormonal treatments for menopausal symptoms". BMJ. 359: j5101. doi:10.1136/bmj.j5101. PMID 29170264. S2CID 46856968.
- Moore TR, Franks RB, Fox C (May 2017). "Review of Efficacy of Complementary and Alternative Medicine Treatments for Menopausal Symptoms". Journal of Midwifery & Women's Health. 62 (3): 286–297. doi:10.1111/jmwh.12628. PMID 28561959. S2CID 4756342.
- Grindler NM, Santoro NF (December 2015). "Menopause and exercise". Menopause. 22 (12): 1351–8. doi:10.1097/GME.0000000000000536. PMID 26382311. S2CID 27802470.
- Cramer H, Peng W, Lauche R (March 2018). "Yoga for menopausal symptoms-A systematic review and meta-analysis". Maturitas. 109: 13–25. doi:10.1016/j.maturitas.2017.12.005. PMID 29452777.
- Saensak S, Vutyavanich T, Somboonporn W, Srisurapanont M (20 July 2014). "Relaxation for perimenopausal and postmenopausal symptoms". Cochrane Database Syst Rev (7): CD008582. doi:10.1002/14651858.CD008582.pub2. PMID 25039019.
- Nedrow A, Miller J, Walker M, Nygren P, Huffman LH, Nelson HD (July 2006). "Complementary and alternative therapies for the management of menopause-related symptoms: a systematic evidence review". Archives of Internal Medicine. 166 (14): 1453–65. doi:10.1001/archinte.166.14.1453. PMID 16864755.
- Bolaños R, Del Castillo A, Francia J (2010). "Soy isoflavones versus placebo in the treatment of climacteric vasomotor symptoms: systematic review and meta-analysis". Menopause. 17 (3): 660–6. doi:10.1097/gme.0b013e3181cb4fb5. PMID 20464785. S2CID 25552285.
- Lethaby A, Marjoribanks J, Kronenberg F, Roberts H, Eden J, Brown J (December 2013). "Phytoestrogens for menopausal vasomotor symptoms". The Cochrane Database of Systematic Reviews. 12 (12): CD001395. doi:10.1002/14651858.CD001395.pub4. PMID 24323914.
- EFSA Femarelle® and bone mineral density Archived 30 January 2012 at the Wayback Machine Scientific substantiation of a health claim related to "Femarelle®" and "induces bone formation and increases bone mineral density reducing the risk for osteoporosis and other bone disorders" pursuant to Article 14 of the Regulation (EC) No 1924/20061 Scientific Opinion of the Panel on Dietetic Products, Nutrition and Allergies. The EFSA Journal (2008) 785, pp. 1–10]
- Leach MJ, Moore V (September 2012). "Black cohosh (Cimicifuga spp.) for menopausal symptoms". The Cochrane Database of Systematic Reviews. 9 (9): CD007244. doi:10.1002/14651858.CD007244.pub2. PMC 6599854. PMID 22972105.
- Clement YN, Onakpoya I, Hung SK, Ernst E (March 2011). "Effects of herbal and dietary supplements on cognition in menopause: a systematic review". Maturitas. 68 (3): 256–63. doi:10.1016/j.maturitas.2010.12.005. PMID 21237589.
- Johnson A, Roberts L, Elkins G (2019). "Complementary and Alternative Medicine for Menopause". Journal of Evidence-Based Integrative Medicine. 24: 2515690X19829380. doi:10.1177/2515690X19829380. PMC 6419242. PMID 30868921.
- Dodin S, Blanchet C, Marc I, Ernst E, Wu T, Vaillancourt C, Paquette J, Maunsell E (July 2013). "Acupuncture for menopausal hot flushes". The Cochrane Database of Systematic Reviews. 7 (7): CD007410. doi:10.1002/14651858.CD007410.pub2. PMC 6544807. PMID 23897589.
- Zhu X, Liew Y, Liu ZL (March 2016). "Chinese herbal medicine for menopausal symptoms". The Cochrane Database of Systematic Reviews. 3: CD009023. doi:10.1002/14651858.CD009023.pub2. PMC 4951187. PMID 26976671.
- Wells GA, Cranney A, Peterson J, Boucher M, Shea B, Robinson V, Coyle D, Tugwell P (January 2008). "Alendronate for the primary and secondary prevention of osteoporotic fractures in postmenopausal women". The Cochrane Database of Systematic Reviews (1): CD001155. doi:10.1002/14651858.CD001155.pub2. PMID 18253985.
- "Concerns over new 'menopause delay' procedure". BBC News. 28 January 2020.
- Moore AM (2018). "Conceptual Layers in the Invention of Menopause in Nineteenth-Century France". French History. 32 (2): 226–248. doi:10.1093/fh/cry006.
- Winterich, J. (August 2008). "Gender, medicine, and the menopausal body: How biology and culture influence women's experiences with menopause". Paper presented at the annual meeting of the American Sociological Association, New York. Retrieved 11 November 2008 from Allacademic.com Archived 9 July 2012 at the Wayback Machine
- Gannon L, Ekstrom B (1993). "Attitudes toward menopause: The influence of sociocultural paradigms". Psychology of Women Quarterly. 17 (3): 275–88. doi:10.1111/j.1471-6402.1993.tb00487.x. hdl:2286/R.I.44298. S2CID 144546258.
- Avis N, Stellato RC, Bromberger J, Gan P, Cain V, Kagawa-Singer M (2001). "Is there a menopausal syndrome? Menopausal status and symptoms across racial/ethnic group". Social Science & Medicine. 52 (3): 345–56. doi:10.1016/S0277-9536(00)00147-7. PMID 11330770.
- Lock M (1998). "Menopause: lessons from anthropology". Psychosomatic Medicine. 60 (4): 410–9. doi:10.1097/00006842-199807000-00005. PMID 9710286. S2CID 38878080.
- Melby MK (2005). "Factor analysis of climacteric symptoms in Japan". Maturitas. 52 (3–4): 205–22. doi:10.1016/j.maturitas.2005.02.002. PMID 16154301.
- Lock M, Nguyen V (2010). "Chapter 4: Local Biologies and Human Difference". An Anthropology of Biomedicine. West Sussex: Wiley-Blackwell. pp. 84–89.
- Gold EB, Block G, Crawford S, Lachance L, FitzGerald G, Miracle H, Sherman S (June 2004). "Lifestyle and demographic factors in relation to vasomotor symptoms: baseline results from the Study of Women's Health Across the Nation". American Journal of Epidemiology. 159 (12): 1189–99. doi:10.1093/aje/kwh168. PMID 15191936.
- Maoz B, Dowty N, Antonovsky A, Wisjenbeck H (1970). "Female attitudes to menopause". Social Psychiatry. 5: 35–40. doi:10.1007/BF01539794. S2CID 30147685.
- Stotland NL (August 2002). "Menopause: social expectations, women's realities". Archives of Women's Mental Health. 5 (1): 5–8. doi:10.1007/s007370200016. PMID 12503068. S2CID 9248759.
- Walker ML, Herndon JG (September 2008). "Menopause in nonhuman primates?". Biology of Reproduction. 79 (3): 398–406. doi:10.1095/biolreprod.108.068536. PMC 2553520. PMID 18495681.
- "'Breakthrough moment': how Lorraine Kelly helped shift the menopause debate". The Guardian. 29 April 2022. Retrieved 2 August 2022.
- Guarino B (27 August 2018). "Beluga Whales and Narwhals Go Through the Menopause Too". Retrieved 24 November 2019.
- Gaulin SJ (1980). "Sexual Dimorphism in the Human Post-reproductive Life-span: Possible Causes". Journal of Human Evolution. 9 (3): 227–32. doi:10.1016/0047-2484(80)90024-X.
- Holmberg I (1970). Fecundity, Fertility and Family Planning. Demography Institute University of Gothenburg Reports (Report). Vol. 10. pp. 1–109.
- Washburn SL (981). "Longevity in Primates". In McGaugh JL, Kiesler SB (eds.). Aging: Biology and Behavior. Academic Press. pp. 11–29.
- Hawkes K (March 2004). "Human longevity: the grandmother effect". Nature. 428 (6979): 128–9. Bibcode:2004Natur.428..128H. doi:10.1038/428128a. PMID 15014476. S2CID 4342536.
- Ricklefs RE, Wikelski M (2002). "The Physiology/Life-history Nexus". Trends in Ecology & Evolution. 17 (10): 462–68. doi:10.1016/S0169-5347(02)02578-8.
- Barash DP, Barash D, Lipton JE (2009). How Women Got Their Curves and Other Just-So Stories: Evolutionary Enigmas. Columbia University Press. ISBN 978-0-231-14664-7.
- Jasienska G, Sherry DS, Holmes DJ (2017). The Arc of Life: Evolution and Health Across the Life Course. New York: Springer Science+Business Media. ISBN 978-1-4939-4036-3.
- Darwin C. Origin of Species. Archived from the original on 3 October 2013. Retrieved 24 September 2013.
- Dusseldorp GL (2009). A view to a kill: Investigating Middle Palaeolithic subsistence using an optimal foraging perspective. Sidestone Press. ISBN 978-9-088-90020-4.
- Bjorklund BR, Bee HL (2003). The journey of adulthood (PDF). Florida: Pearson. ISBN 978-1-292-06488-8.
- Morton RA, Stone JR, Singh RS (13 June 2013). "Mate choice and the origin of menopause". PLOS Computational Biology. 9 (6): e1003092. Bibcode:2013PLSCB...9E3092M. doi:10.1371/journal.pcbi.1003092. PMC 3681637. PMID 23785268.
- Takahashi M, Singh RS, Stone J (6 January 2017). "A Theory for the Origin of Human Menopause". Frontiers in Genetics. 7: 222. doi:10.3389/fgene.2016.00222. PMC 5216033. PMID 28111590.
- Johnstone RA, Cant MA (December 2010). "The evolution of menopause in cetaceans and humans: the role of demography". Proceedings. Biological Sciences. 277 (1701): 3765–71. doi:10.1098/rspb.2010.0988. PMC 2992708. PMID 20591868.
- Lawson Handley LJ, Perrin N (April 2007). "Advances in our understanding of mammalian sex-biased dispersal". Molecular Ecology. 16 (8): 1559–78. doi:10.1111/j.1365-294x.2006.03152.x. PMID 17402974.
- Ségurel L, Martínez-Cruz B, Quintana-Murci L, Balaresque P, Georges M, Hegay T, Aldashev A, Nasyrova F, Jobling MA, Heyer E, Vitalis R (September 2008). "Sex-specific genetic structure and social organization in Central Asia: insights from a multi-locus study". PLOS Genetics. 4 (9): e1000200. doi:10.1371/journal.pgen.1000200. PMC 2535577. PMID 18818760.
- Sugiyama Y (July 2017). "Sex-biased dispersal of human ancestors". Evolutionary Anthropology. 26 (4): 172–180. doi:10.1002/evan.21539. PMID 28815964. S2CID 19996159.
- Bigg MA, Olesiuk PF, Ellis GM, Ford JK, Balcomb KC (1 January 1990). "Social organization and genealogy of resident killer whales (Orcinus orca) in the coastal waters of British Columbia and Washington State". Report of the International Whaling Commission. 12: 383–405.
- Croft DP, Johnstone RA, Ellis S, Nattrass S, Franks DW, Brent LJ, Mazzi S, Balcomb KC, Ford JK, Cant MA (January 2017). "Reproductive Conflict and the Evolution of Menopause in Killer Whales". Current Biology. 27 (2): 298–304. doi:10.1016/j.cub.2016.12.015. PMID 28089514.
- Heimlich-Boran JR (1993). Social organisation of the short-finned pilot whale, Globicephala macrorhynchus, with special reference to the comparative social ecology of delphinids (Doctoral thesis). University of Cambridge.
- Peccei JS (2001). "Menopause: Adaptation or Epiphenomenon?". Evolutionary Anthropology. 10 (2): 43–57. doi:10.1002/evan.1013. S2CID 1665503.
- Brent LJ, Franks DW, Foster EA, Balcomb KC, Cant MA, Croft DP (March 2015). "Ecological knowledge, leadership, and the evolution of menopause in killer whales". Current Biology. 25 (6): 746–750. doi:10.1016/j.cub.2015.01.037. PMID 25754636. S2CID 3488959.
- Nattrass S, Croft DP, Ellis S, Cant MA, Weiss MN, Wright BM, et al. (December 2019). "Postreproductive killer whale grandmothers improve the survival of their grandoffspring". Proceedings of the National Academy of Sciences of the United States of America. 116 (52): 26669–26673. Bibcode:2019PNAS..11626669N. doi:10.1073/pnas.1903844116. PMC 6936675. PMID 31818941.
- Lahdenperä M, Lummaa V, Helle S, Tremblay M, Russell AF (March 2004). "Fitness benefits of prolonged post-reproductive lifespan in women" (PDF). Nature. 428 (6979): 178–81. Bibcode:2004Natur.428..178L. doi:10.1038/nature02367. PMID 15014499. S2CID 4415832.
- Voland E, Beise J (November 2002). "Opposite effects of maternal and paternal grandmothers on infant survival in historical Krummhörn". Behavioral Ecology and Sociobiology. 52 (6): 435-443 10.1007/s00265-002-0539-2. doi:10.1007/s00265-002-0539-2. S2CID 24382325.
- Mace R, Sear R (2004). "Are Humans Communal Breeders?". In Voland E, Chasiotis A, Schiefenhoevel W (eds.). Grandmotherhood – the Evolutionary Significance of the Second Half of Female Life. Rutgers University Press.
- Finch CE (1994). Longevity, Senescence, and the Genome (Pbk. ed.). Chicago: University of Chicago Press. ISBN 978-0-226-24889-9.
- Pavard S, Sibert A, Heyer E (May 2007). "The effect of maternal care on child survival: a demographic, genetic, and evolutionary perspective". Evolution; International Journal of Organic Evolution. 61 (5): 1153–61. doi:10.1111/j.1558-5646.2007.00086.x. PMID 17492968. S2CID 13118937.
- Walker RS, Flinn MV, Hill KR (November 2010). "Evolutionary history of partible paternity in lowland South America". Proceedings of the National Academy of Sciences of the United States of America. 107 (45): 19195–200. Bibcode:2010PNAS..10719195W. doi:10.1073/pnas.1002598107. PMC 2984172. PMID 20974947.
- Massart F, Reginster JY, Brandi ML (November 2001). "Genetics of menopause-associated diseases". Maturitas. 40 (2): 103–16. doi:10.1016/S0378-5122(01)00283-3. PMID 11716989.
- Leidy L. "Menopause in evolutionary perspective". In Trevathan WR, McKenna JJ, Smith EO (eds.). Evolutionary Medicine'. Oxford University Press. pp. 407–427.
- Clinical Obstetrics and Gynaecology (3 ed.). Elsevier Health Sciences. 2014. p. 69. ISBN 9780702054105.
- Clutton-Brock TH, Hodge SJ, Spong G, Russell AF, Jordan NR, Bennett NC, Sharpe LL, Manser MB (December 2006). "Intrasexual competition and sexual selection in cooperative mammals". Nature. 444 (7122): 1065–8. Bibcode:2006Natur.444.1065C. doi:10.1038/nature05386. PMID 17183322. S2CID 4397323.
- Lahdenperä M, Gillespie DO, Lummaa V, Russell AF (November 2012). "Severe intergenerational reproductive conflict and the evolution of menopause". Ecology Letters. 15 (11): 1283–1290. doi:10.1111/j.1461-0248.2012.01851.x. PMID 22913671.
- Jaeggi AV, Gurven M (July 2013). "Natural cooperators: food sharing in humans and other primates". Evolutionary Anthropology. 22 (4): 186–95. doi:10.1002/evan.21364. PMID 23943272. S2CID 25989629.
- Cant MA, Johnstone RA (April 2008). "Reproductive conflict and the separation of reproductive generations in humans". Proceedings of the National Academy of Sciences of the United States of America. 105 (14): 5332–6. Bibcode:2008PNAS..105.5332C. doi:10.1073/pnas.0711911105. PMC 2291103. PMID 18378891.
- Wright BM, Stredulinsky EH, Ellis GM, Ford JK (May 2016). "Kin-directed food sharing promotes lifetime natal philopatry of both sexes in a population of fish-eating killer whales, Orcinus orca". Animal Behaviour. 115: 81–95. doi:10.1016/j.anbehav.2016.02.025.
- Walker ML (1995). "Menopause in female rhesus monkeys". American Journal of Primatology. 35 (1): 59–71. doi:10.1002/ajp.1350350106. PMID 31924061. S2CID 83848539.
- Bowden DM, Williams DD (1984). "Aging". Advances in Veterinary Science and Comparative Medicine. 28: 305–341. doi:10.1016/b978-0-12-039228-5.50015-2. ISBN 9780120392285. PMID 6395674.
- Emery Thompson M, Jones JH, Pusey AE, Brewer-Marsden S, Goodall J, Marsden D, et al. (December 2007). "Aging and fertility patterns in wild chimpanzees provide insights into the evolution of menopause". Current Biology. 17 (24): 2150–6. doi:10.1016/j.cub.2007.11.033. PMC 2190291. PMID 18083515.
- Sukumar R (1992). The Asian Elephant. ISBN 9780521437585. Archived from the original on 12 May 2016.
- Marsh H, Kasuya T (1986). "Evidence for reproductive senescence in female cetaceans" (PDF). Reports of the International Whaling Commission. pp. 57–74. Archived from the original (PDF) on 21 September 2020. Retrieved 9 June 2018.
- Brent LJ, Franks DW, Foster EA, Balcomb KC, Cant MA, Croft DP (March 2015). "Ecological knowledge, leadership, and the evolution of menopause in killer whales". Current Biology. 25 (6): 746–750. doi:10.1016/j.cub.2015.01.037. PMID 25754636.
- Ellis S, Franks DW, Nattrass S, Currie TE, Cant MA, Giles D, Balcomb KC, Croft DP (August 2018). "Analyses of ovarian activity reveal repeated evolution of post-reproductive lifespans in toothed whales". Scientific Reports. 8 (1): 12833. Bibcode:2018NatSR...812833E. doi:10.1038/s41598-018-31047-8. PMC 6110730. PMID 30150784.
- Reznick D, Bryant M, Holmes D (January 2006). "The evolution of senescence and post-reproductive lifespan in guppies (Poecilia reticulata)". PLOS Biology. 4 (1): e7. doi:10.1371/journal.pbio.0040007. PMC 1318473. PMID 16363919.
- Canine reproduction
- "How long is a cat in heat?". Animal Planet. 15 May 2012. Retrieved 12 June 2018.