
Diabetic Foot Care
- Article Author:
- Kayla Song
- Article Editor:
- Aaron Chambers
- Updated:
- 7/31/2020 2:31:33 PM
- For CME on this topic:
- Diabetic Foot Care CME
- PubMed Link:
- Diabetic Foot Care
Introduction
Diabetes mellitus is a metabolic disease resulting in increased glucose in the bloodstream. Estimates are that there are 451 million individuals with diabetes worldwide and approximately 5 million diabetes-related deaths in 2017 globally.[1]
Patients with diabetes mellitus are at increased risk for pedal ulceration due to microvascular, neuropathic, and biomechanical changes to the foot. Neuropathic changes to the body result in decreased pedal sensation and make the diabetic foot prone to wounds from pressure, mechanical, or pressure injuries. Microvascular changes can result in reduced blood flow to the lower extremity, and delaying healing of wounds.
Hemoglobin A1c is a marker that reflects average blood glucose levels over a 2 to 3 month period. The American Diabetes Association and International Expert Committee agree that a hemoglobin A1c greater than or equal to 6.5% is the recommended level for the diagnosis of diabetes.[2] An increase in HgA1c of 1% has demonstrated to increase peripheral vascular disease risk by 25 to 28%[3].
Patients with diabetes are at high risk for lower extremity amputations, higher healthcare costs, and lower quality of life. In a systematic regarding non-traumatic amputations of patients with diabetes mellitus and peripheral vascular disease, the 5-year mortality rate of patients after a below-the-knee amputation was 40 to 82%, and mortality after an above-the-knee amputation was 40 to 90%.[4][3] Many of these complications are preventable by a thorough annual foot exam and routine foot care performed by the patient.
The purpose of this article is to discuss anatomy, indications, equipment, personnel, preparation, technique, complications, and clinical significance of the diabetic foot.
Anatomy and Physiology
The diabetic foot differs from a normal foot in several ways. Changes to the diabetic foot include musculoskeletal, dermatologic, vascular, and neurological etiologies.
In the musculoskeletal system, a decrease in intrinsic musculature, limited joint mobility, changes in foot type, and ankle equinus, and others all occur in the diabetic foot.
Limited joint mobility of the first metatarsophalangeal joint (hallux limitus) is often present in patients with diabetes, which can be caused by a thickening of the Achilles tendon and plantar fascia. This thickening of the plantar fascia and Achilles tendon leads to a more rigid foot type, increased pes planus, and possible unsteadiness of gait.[5]
The pedal musculature becomes disorganized and infiltrated with adipose tissue as a result of long-standing diabetes. Intrinsic pedal muscles become weaker than extrinsic muscles resulting in foot deformities such as hammertoes or claw toe deformities.[5]
Hammertoes and claw toes along with hallux limitus correlated with increased risk for ulcer occurrence. Bus et al. studied elevated plantar pressures in patients with diabetes with hammer and claw toes and found that plantar metatarsal head pressures significantly increased with increasing toe deformity. They noted that there is a transfer of load from distal to proximal in such toe deformities, with possible distal fat pad displacement as a mechanism.[6]
Searle et al. found that patients with diabetes have a high rate of ankle equinus, defined as less than 5 degrees of ankle dorsiflexion. This condition has correlations with increased forefoot pressure and tissue breakdown, both barefoot and with shoegear. [7]
Dermatologic integrity is one of the most important functions of human skin, but as a result of chronic diabetes, many changes put this critical organ at risk. Autonomic dysfunction as a result of diabetes decreases perspiration in the foot, which leads to increased fissuring and xerosis.[8]
Repetitive stress and pressure to one area, in conjunction with neuropathy, causes inflammation and ulceration. Plantar skin tissue thickness decrease in patients with type 2 diabetes mellitus with neuropathy compared to non-neuropathic patients with diabetes, adding to the increased risk for ulceration.[9] Even once healed, the tissue surrounding former ulceration is at increased risk for rapid breakdown and re-ulceration.[10]
Blood flow to the lower extremity is also an area where diabetes can affect the foot and ankle.
Three main arteries and their branches supply the six angiosomes of the foot and ankle. The posterior tibial artery originates from the popliteal artery and supplies the plantar foot. The peroneal artery originates from the posterior tibial artery and supplies the anterolateral ankle and rearfoot. The anterior tibial artery originates from the popliteal artery and continues into the foot as the dorsalis pedis artery. It supplies the anterior ankle and dorsal foot.[11]
Patients with diabetes have an increased risk of developing peripheral arterial disease (PAD). PAD is the atherosclerotic occlusive disease of the lower extremities. While over half of patients can be asymptomatic, some patients may experience such symptoms as intermittent claudication (aching in lower extremities with activity and relieved with rest) and rest pain, or in more severe cases tissue loss and gangrene.
Neurologically, the foot receives innervation from five main nerves and their branches: the tibial, superficial peroneal, deep peroneal, sural, and saphenous nerves. The tibial nerve originates from the sciatic nerve and divides into the medial and lateral plantar nerves, which further divide into the digital nerves. The tibial nerve provides motor innervation to the posterior lower leg muscles and sensory innervations to the plantar foot and heel. The superficial peroneal nerve (SPN) originates from the common peroneal nerve and branches into the medial and intermediate dorsal cutaneous nerves. The SPN innervates the peroneus longus and brevis muscles and also provides the sensory function to the anterior lower leg and dorsal foot and toes (except for the first webspace). The deep peroneal nerve originates from the common peroneal nerve. It has motor innervations to the anterior compartment muscles and sensory innervations to the first web space. The sural nerve forms from the tibial nerve and peroneal nerve, and it provides sensory innervation to the posterior lateral lower leg and posterior-lateral foot. The saphenous nerve originates from the femoral nerve and provides sensory innervation to the medial-distal leg, ankle, and foot.[12][13]
A neurological manifestation of diabetes is diabetic neuropathy.[14] Distal symmetrical polyneuropathy is the most common type of diabetic neuropathy. It can involve a combination of sensory or motor neuropathy due to small and/or large nerve fiber dysfunction. Large fiber (A alpha/beta fiber damage) neuropathy is painless paresthesia with reduced sensations in vibration, joint position, touch, pressure, and loss of ankle reflexes. Small fiber (myelinated A-delta and unmyelinated C fiber damage) neuropathy is painful, burning, with reduced pain and temperature sensations.
Diabetic peripheral neuropathy usually starts distally in the toes and progresses proximally. With progression, the patient may start to notice decreased sensation in their upper extremities in a stocking-glove distribution. Symptoms may worsen at night during sleep. Muscle weakness may also develop later in the disease. The exact pathogenesis of diabetic peripheral neuropathy is still the subject of research; however, a major suspect in this process may be chronic hyperglycemia with related metabolic changes leading to a combination of direct axonal injury and nerve ischemia.[15][16]
A dreaded complication of uncontrolled diabetes and peripheral neuropathy is Charcot neuroarthropathy (CN). This condition is likely the result of both neurovascular changes (i.e., arteriovenous shunting causing increased blood flow and increased bone resorption) and micro-trauma.[17] These changes result in collapsed joints and severe pedal deformities. The most common joint to collapse in CN is the tarsometatarsal joint, which leads to a rocker bottom deformity.
Patients with Charcot foot have a 17% chance annually to develop ulceration. The lower extremity amputation risk for CN patients who have ulceration is 12 times higher compared to patients who have Charcot foot without ulceration.[18] Early detection and treatment of CN improve outcomes; therefore, astute providers should suspect CN when a diabetic patient presents with a warm, erythematous, edematous foot with possible pedal structural changes.
Indications
All patients with diabetes should receive education on proper diabetic foot care. Prevention of diabetic foot complications includes identifying the at-risk foot, daily exam and inspection, patient/family/healthcare provider education, appropriate shoegear, and proper and early treatment of pre-ulcerative lesions. Higher risk patients should obtain a referral to podiatry for management and monitoring. The International Working Group on Diabetic Foot (IWGDF) classification recommends diabetic foot screening by a medical professional[19]:
- Once a year for individuals without peripheral neuropathy
- Every six months for individuals with peripheral neuropathy
- Every 3 to 6 months for individuals with peripheral neuropathy, peripheral arterial disease and/or foot deformity
- Every 1 to 3 months for individuals with peripheral neuropathy and history of pedal ulceration or lower extremity amputation
Contraindications
There are no contraindications to proper diabetic foot care.
Equipment
A basic diabetic foot exam requires minimal specialty instruments and is performable by most primary care, podiatric, or other physicians.
The neurological evaluation requires a Semmes-Weinstein monofilament for neuropathy and protective-sensation testing. A 128Hz-tuning fork can test vibratory sensation, and cotton wool can test tactile sensation.[3]
Vascular testing may require a Doppler ultrasound to assess blood flow.
During diabetic foot care, the caregiver may encounter ulcerations. If ulceration is present and requires debridement or offloading, scalpels, tissue nippers, and offloading padding (e.g., felt pads, foam pads, cushions) should be readily available.
For advanced wound care settings, an array of products should be available: gauze, cleaning solutions (e.g., saline, hydrogen peroxide, acetic acid), topical antimicrobials (e.g., povidone-iodine, cadexomer iodine, silver, medical-grade honey, moisture-retentive dressings (e.g., films, foams, alginates, hydrogels, hydrocolloids), vacuum-assisted closure devices, and bioengineered dressings.[20]
Personnel
An interdisciplinary approach to managing diabetic foot and its possible complications can reduce amputations up to 85%. Endocrinology, diabetology, vascular surgery, podiatry, orthotics, prosthetics, wound care nursing, and educators are crucial to caring for the diabetic foot. Other specialties that may play roles in diabetic foot care depending on medical issues and infection include infectious disease, nephrology, cardiology, dermatology, and others. Goals should be to medically optimize comorbidities, prevent pedal issues, and treat pedal complications.
Preparation
Patients with diabetes should remove both shoes and socks before the exam. Clean and dry feet thoroughly prior to foot exam or dressing change. If performing a dressing change on a diabetic foot ulcer, wash hands before and after the dressing change. Patients should prepare a clean and sanitary environment to decrease the chances of contamination and infection.
Technique
The clinical diabetic foot exam includes four major components: dermatological, vascular, neurological, musculoskeletal.
The dermatological exam includes a thorough evaluation of the entire foot and ankle, including interdigital spaces and nails. Hyperkeratosis requires debriding. Pre-ulcerative and ulcerative lesions need detailed documentation of location, size, depth, the appearance of wound base, peri-wound skin, undermining, tracking, probing to the bone, exudate quality, and signs of infection (e.g., warmth, erythema, malodor, crepitus). A temperature of greater than 3 to 4 degrees compared to the contralateral foot may indicate an infection or acute Charcot neuroarthropathy. Also, a prior history of ulcerations, treatments, and preventative modalities requires documentation. A baseline foot radiograph is in order for patients with new ulcerations, and if osteomyelitis is concerned, the clinician should obtain serial radiographs for monitoring and exclusion.[21]
Clinical evaluation of vascularity and PAD starts with a thorough medical history (e.g., PAD risk factors, claudication, rest pain, history of non-healing wounds). Palpation of dorsalis pedis and posterior tibial arteries are the baseline for diabetic foot exams, but palpation of popliteal and femoral pulses can further assess the level of PAD. A decrease in pedal pulses may warrant evaluation with a Doppler ultrasound or further non-invasive testing for PAD. A Doppler ultrasound of pedal arteries can reveal triphasic flow (normal), biphasic flow (some arterial disease), monophasic flow (PAD with risk for limb ischemia), or absent (severe PAD and high risk for ischemia and limb loss). Non-invasive vascular tests include vascular labs (i.e., ankle-brachial index (ABI), segmental pressures, pulse volume recording, toe pressures, and transcutaneous partial pressure of oxygen [TcPO2]) and treadmill functional testing. The American Diabetes Association (ADA) recommends a screening ABI in patients with diabetes greater than 50 years old, and if normal, a repeat ABI should take place every five years. Screening ABI in patients with diabetes less 50 years old should be a consideration if they also have PAD risk factors (e.g., smoking, hypertension, hyperlipidemia, diabetes greater than ten years). If any indications of PAD are present during these exams, a referral to vascular surgery should follow.[22][21]
The diabetic foot neurological exam consists of Achilles reflex testing, Semmes-Weinstein monofilament testing (SWMT), 128 Hz tuning fork testing, and pinprick testing. The Achilles reflex is performed on bilateral Achilles tendon with a reflex hammer. Reflexes are graded as 0+ (absent), 1+ (decreased), 2+ (brisk, normal), 3+ (increased), 4+ (increased with clonus). The 5.07/10 g SWMT is the most commonly used monofilament and examines pressure/light touch sensation. It should test for ten sites on each foot as follows: Distal first toe, distal third toe, distal fifth toe, plantar first metatarsal head, plantar third metatarsal head, plantar fifth metatarsal head, plantar medial and lateral arch, plantar heel, and dorsal first interspace. The 128-Hz non-graduated standard tuning fork tests vibratory sensation, and an abnormal result can reveal diabetic neuropathy if the patient can no longer distinguish vibration. The pinprick can be performed with a sharp pin device and evaluates whether the patient can distinguish sharp vs. dull sensations.[23][24][25]
Musculoskeletal evaluation should determine lower extremity muscle strength and foot or ankle deformities and limitations. The flexibility and rigidity of the joint range of motion should be determined to guide treatment options. As mentioned previously, patients with diabetes are at higher risk of developing pedal deformities such as digital contractures and ankle equinus, which increases the risk for ulceration. For example, a flexible ankle equinus due to gastrocnemius tightness may result in increased plantar foot pressures and tissue breakdown in the neuropathic patient. Patients with pedal deformities should be referred to podiatry or other surgical practitioners for further management as they may benefit from surgical correction. For example, a digital flexor tenotomy may help in preventing distal toe ulcerations where tissue breakdown has developed.[26]
Patient and family education and enforcement of proper diabetic foot care should be also be provided during the visit.[27]
Patients should understand the importance of ambulating in protective shoegear, both indoors and outdoors. They should wear properly fitted shoes to prevent ulcerations. Additionally, patients with diabetes may require specialized shoegear and should undergo evaluation for such during the diabetic foot exam. The appropriate offloading and protective modality will depend on an individualized assessment of biomechanical changes, pressure points, and pathology. Shoe modifications, temporary shoegear, toe spacers, orthosis, and offloading felt pads or foam may all assist in protecting the diabetic foot.[28]
Complications
Poor diabetic foot care increases the risk of ulceration, infection, and limb loss. Armstrong D.G. and Harkless L.B. found that noncompliant patients, defined as missing greater than 50% of scheduled appointments in 1 year, are 54 times more likely to develop pedal ulcerations and 20 times more likely to have amputations compared to compliant patients.[29] One study found that patients with diabetes fear major lower extremity amputations more than death, foot infection, or end-stage renal disease.[30] Another study found that amputation had the greatest effect on the quality of life when compared to other diabetes complications (i.e., stroke, blindness, renal failure, heart failure, myocardial infarction).[31] Therefore, high-risk limbs require close monitoring and care by specialists such as podiatrists.
Clinical Significance
Proper diabetic foot care is a crucial aspect of diabetes treatment for limb preservation. One of the leading causes of hospitalization and amputation in patients with diabetes is foot ulcerations. The majority of diabetic foot complications result from ischemia, neuropathy, and/or infection. Patients with diabetes and neuropathy have a 7 to 10% chance of developing foot ulceration each year, and the probability increases to 25 to 30% for patients with more risk factors (e.g., peripheral arterial disease, pedal deformities, previous amputation or ulcerations). 85% of amputations on Patients with diabetes are secondary to complications from foot ulcerations. Patients with diabetes over 45 years old are eight times more likely to have an amputation, over 65 years old are 12 times more likely, and 65 to 74 years old are 23 times more likely.[3]
Enhancing Healthcare Team Outcomes
Diabetic foot care requires interprofessional care. The severity of amputation, length of stay, and mortality rates improved in patients receiving care from a team when compared to those who did not. There may also be an improvement in regards to ulcer healing and quality of life.[32] [Level 1]
Proper diabetes management is an essential part of diabetic foot care. In addition to routine management with endocrinology/diabetology, studies show that a group-based self-management education system improves body weight, fasting blood glucose, waist circumference, diabetic knowledge, and triglyceride levels. These monitoring activities can fall between the clinicians, nursing, and pharmacists; in any event, the results and observations require charing and communication with the rest of the team. Interventions done by interprofessional teams with peer supporters improved HgA1c when compared to peer-led groups.[33] [Level 1] Diabetic and foot care nurses are often responsible for foot assessment. They should also educate patients regarding proper foot care. However, all members of the interprofessional team bear responsibility for this training, from nursing to pharmacists, and of course, all clinicians - this interprofessional collaboration can improve patient self-care as well as outcomes, preventing many adverse sequelae as outlined above. [Level 5]
Nursing, Allied Health, and Interprofessional Team Interventions
Intensive patient education (e.g., lifestyle management, podiatric care, proper examinations, callus management) for diabetic foot care by nursing helps prevent diabetic foot ulcerations and decrease the amputation rate for high-risk diabetic feet. Also, intensive education helps to lower plasma glucose, blood pressure, and high-density lipoprotein cholesterol levels.[34]
Nursing, Allied Health, and Interprofessional Team Monitoring
Care for the diabetic foot is an interprofessional responsibility. Holstein et al. found a 75% decrease in major limb amputations in patients with diabetes when establishing an interdisciplinary/interprofessional foot clinic with increased revascularization rates.[35] Primary care physicians and nursing can identify the diabetic foot and provide extensive education on proper care and monitoring. A patient with increased risk factors and pedal deformities should be followed regularly by podiatry. If ulcerations develop, more frequent monitoring may be required and may need a referral to other specialists such as vascular surgery, infectious disease, plastic surgery, and prosthetics.
(Click Image to Enlarge)
(Click Image to Enlarge)
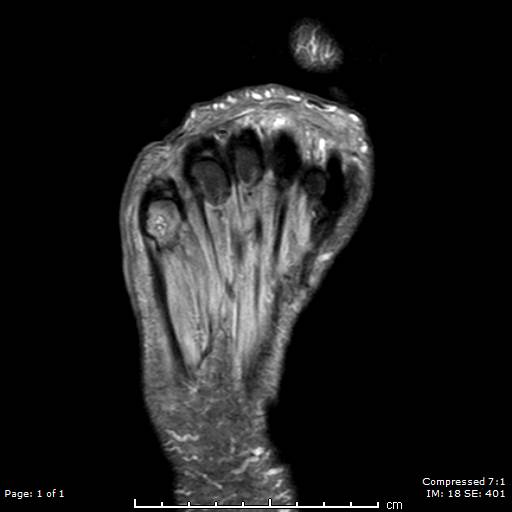
T2-weighted MRI image of a patient's right foot. Patient had history of uncontrolled diabetes, peripheral neuropathy and a long-standing ulceration under the 5th metatarsal head resulting in osteomyelitis of the 5th metatarsal head and shaft. Patient subsequently underwent a partial 5th ray resection with long term IV antibiotics for treatment and healed uneventfully.
Contributed by Aaron R. Chambers, DPM, FACFAS
(Click Image to Enlarge)

Xray of a patient's right foot after undergoing partial ray resection of the 5th metatarsal for acute osteomyelitis. Patient had history of uncontrolled diabetes, peripheral neuropathy and a long-standing ulceration under the 5th metatarsal head resulting in osteomyelitis of the 5th metatarsal head and shaft. Patient underwent a partial 5th ray resection with long term IV antibiotics for treatment and healed uneventfully.
Contributed by Aaron R. Chambers, DPM, FACFAS
