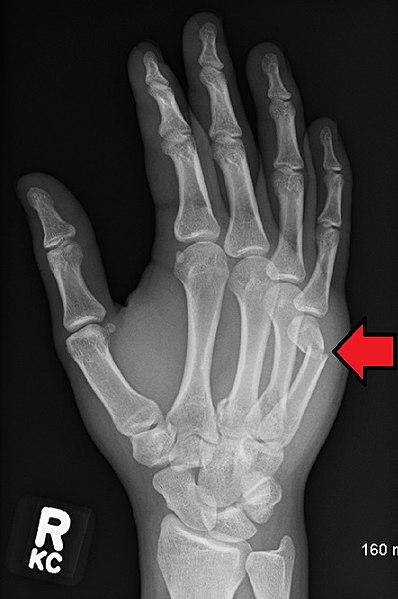
Metacarpal Hand Fracture
- Article Author:
- Alicja Moore
- Article Editor:
- Matthew Varacallo
- Updated:
- 7/10/2020 10:40:17 AM
- For CME on this topic:
- Metacarpal Hand Fracture CME
- PubMed Link:
- Metacarpal Hand Fracture
Introduction
Hand fractures are common in the general population with relative propensity seen in contact-sport athletes (e.g., boxers, football players) and manual laborers.[1]
Etiology
Metacarpal fractures typically occur secondary to a direct blow or fall directly onto the hand. These fractures commonly occur during athletic activities, particularly in contact sports. Almost one-fourth of cases occur during athletic events.[1][2][3] While a sporting injury is frequently the cause among younger patients, work-related injuries are often the cause in middle-aged patients, and falls are typically the cause in the elderly. Fifth metacarpal fractures often occur secondary to punching a wall or other solid object (hence the eponym, "boxer's fracture").[4]
Epidemiology
Hand fractures make up about 40% of all acute hand injuries, and they constitute about 20% of all fractures occurring below the elbow.[5][2] Metacarpal fractures typically occur in patients aged 10-40 years, and men are more likely to be affected than women. Young men sustain metacarpal fractures secondary to a punching mechanism or a direct blow to the hand while geriatric females sustain these injuries secondary to a low energy fall. The incidence rate of fracture seen in association with each digit's metacarpal bone increases from the radial to the ulnar side. The incidence rate of 2nd metacarpal fractures is lower than the incidence rate of 5th metacarpal fractures.[1][4]
History and Physical
Mechanism of injury is critical in delineating clinical pathology.[4][6][7] Metacarpal fractures should be under suspicion in any injury with a history of a high-energy impact to the hand, particularly if there is significant hand swelling and/or deformity present. Different mechanisms of injury tend to have different fracture patterns.[2] For example, an axial load combined with a rotational force often results in a short oblique or spiral fracture pattern. Other critical elements in the history include: [8][9][10]
- hand dominance
- occupation and current working status
- athletic participation (including sport-specific position)
- history of prior fracture or injury
- Patients may present with many potential preexisting deformities, which may warrant further questioning regarding previous interventions or surgeries. The provider should also document baseline functional status (e.g., chronic stiffness, deformity, or other limitations)
A thorough examination of the entire hand and digits is imperative.[2] Attention is given to skin integrity and any evidence of bruising, swelling, or deformity. Any compromise to the skin integrity (including abrasions, lacerations, "poke holes," and potential traumatic arthrotomies) should be noted and thoroughly documented for treatment and management. In the setting of fingertip injuries and nailbed lacerations, the examiner should control bleeding that may compromise the inspection to evaluate the degree of injury to the nail bed itself.[11]
Rotational assessment is assessable by having the patient place both hands on a flat surface with the volar side facing upward. The patient should actively make a fist while the provider observes the following:
- presence of symmetry or asymmetry between the normal and afflicted sides
- inability to make a full fist secondary to stiffness and/or pain
- rotational alignment when making a fist
- the provider can assess rotation by passively guiding the finger as the patient can tolerate
- the tips of all digits should point toward the scaphoid tubercle in cascading fashion
Assessment of neurovascular status is crucial before administering a local anesthetic.[11]
Evaluation
The evaluation includes standard radiographs of the hand (anteroposterior, lateral, and oblique). In the vast majority of cases, this will be enough to confirm the diagnosis and form a management plan. If there is any doubt, confirmation of more subtle injuries can be obtained using special views such as Brewerton (metacarpal heads), Roberts, and Betts (thumb) views.
CT is sometimes necessary for the base of metacarpal fractures to check for any intra-articular displacement and determine if there is a need for surgery.[2]
Treatment / Management
The goal of treatment is a restoration of anatomy and function.[1] Antibiotics and tetanus prophylaxis are options for open fractures as per standardized guidelines.[4] The modality of treatment will vary depending on skin integrity (open versus closed fracture), the number of digits/metacarpals fractured, the stability of the specific, degree of comminution, displacement, and/or rotational malalignment.[5]
In general, increasing degrees of displacement, comminution, and rotational malalignment are critical factors in assessing the fracture patterns potential for stability and reduction maintenance with nonoperative management.
Over the last few decades have seen advances and improvements regarding low-profile plates/screws options. Kirschner wires (K-wires) might be a better option for patients who require maximum cosmesis.[1][2]
Special considerations
Thumb metacarpal fractures
The thumb metacarpal deserves special consideration given the relative lack of interossei and deep intermetacarpal ligament support.[2] Fractures deform dictated by the three muscles providing the deforming forces at the base of the thumb [12]
- Abductor pollicis longus (APL) - pulls the shaft in a proximal, dorsal, and radial deformity
- Extensor pollicis longus (EPL) - same as APL
- Adductor pollicis - pulls the shaft into supination and adduction
The distal fragment assumes an apex dorsal, adducted, and flexed position.[4]
Despite the thumb tolerating more angulation than other metacarpals due to its higher mobility, an apex dorsal angulation of over 30 degrees often fares poorly with nonoperative management. Indications for closed reduction and thumb spica casting include:
- Extra-articular fracture
- Less than 30 degrees of angulation following closed reduction
- Non-displaced (or less than 1 mm displacement) of an intra-articular fracture (i.e., Bennet fracture)
Note that intra-articular fractures (Bennett – 2 part, and Rolando – 3 part fracture patterns) most commonly require surgical fixation, as the joint surface needs to be reduced to avoid long term post-traumatic deformity and articular cartilage degeneration.[2]
Operative indications for thumb metacarpal fractures include:
- Extra-articular fracture patterns with greater than 30 degrees of angulation following attempted closed reduction
- Loss of reduction following thumb spica casting/splinting
- Intra-articular fracture patterns:
- Bennett fractures with less than 1 mm displacement or
- Rolando fracture (any type, even non-displaced/minimally displaced)
Operative techniques include:
- Closed reduction and percutaneous k-wire fixation
- Open reduction internal fixation
- often preferred over CRPP techniques in fracture patterns with greater than 1 mm displacement, or in fracture patterns with large articular pieces amenable to screw fixation
- Distraction and external fixation
- preferred in the setting of severely comminuted fracture patterns with associated major soft tissue injuries
Metacarpal head fractures
Metacarpal head fractures are the least common, and management is best performed operatively if there is an intra-articular step off. Stable fixation allows for earlier mobilization, which can reduce stiffness. Severely comminuted fractures may require:
- External fixation
- Metacarpophalangeal joint arthroplasty (MCP arthroplasty)
- MCP fusion
- indicated in the setting of severe arthritic changes, end-stage
In the setting of "fight bite" injuries, management must include early IV antibiotics, irrigation, and surgical debridement of the MCP joint.[2]
Metacarpal neck fractures
Metacarpal neck fractures are the most common as anatomically the metacarpal neck is the weakest point in the bone.[2] A metacarpal neck fracture is also known as a boxer's fracture, although not frequently present amongst professional boxers. They often result in an apex dorsal angulation deformity due to the forces of the intrinsic musculature. The more ulnar the metacarpal, the more of this deformity it can tolerate functionally.[1] Angulation of 10, 20, 30, and 40 degrees (or even up to 70) is acceptable from 2nd to 5th metacarpal.[2] If there is a significant deformity present, it will require reduction with Jahss maneuver (flex metacarpophalangeal joint, proximal interphalangeal joint, and distal interphalangeal joint, and use the curled up finger to push the metacarpal head back into position).[4] If the reduction is stable, then early mobilization is ideal, and it rarely needs splinting for longer than six weeks. Radiographs can be obtained to make sure alignment maintenance in the follow-up period[2]. However, when assessing stability, it is important to remember that in most cases, clinical stability occurs well before healing is apparent on radiographs.[4] If the reduction is unstable or the fracture has severely angulated, surgical fixation is the recommendation. Rotational deformity, pseudoclawing, and fracture in a neighboring ray are also indications to consider surgical fixation. Fixation can be either using K-wires or plating, although some papers suggest open reduction and internal fixation should be avoided to prevent stiffness.[1][2]
Metacarpal shaft fractures
The consensus on the acceptable nonoperative parameters following closed reduction of metacarpal shaft fractures include the following:
- index and long finger
- Angulation (degrees): 10-20
- Shortening (mm): 2-5
- ring finger
- Angulation (degrees): 30
- Shortening (mm): 2-5
- small finger
- Angulation (degrees): 40
- Shortening (mm): 2-5
Shaft fractures can be transverse, oblique, spiral, or comminuted.[2] They are less stable if present in the index or little finger metacarpals as these injuries lack the inherent soft tissue support and stabilization compared to the adjacent metacarpals.[1]
Transverse and short oblique fractures tend to result in a dorsal angulation deformity. Less angulation is tolerated compared to metacarpal neck fractures. Oblique fractures tend to shorten as fragments slide on each other. If the fracture line is long enough (twice the diameter of the bone) and bones fragments are large enough (three times width of the screw), a double lag screw fixation is possible. If it is not possible, a single screw will require a neutralization plate. The use of K-wires is also a possibility.[1]
The same principles apply to spiral fractures while exercising care that lag screws are placed perpendicularly to the fracture line. Screws require less dissection than plating, which can reduce adhesions and scarring, although with aggressive physiotherapy stiffness can be minimized in either instance.[1]
Metacarpal base fractures
In the presence of metacarpal base fractures, it is important to rule out carpometacarpal dislocation, as high energy is likely to be involved in the trauma. Intra-articular fractures are more common on the ulnar side of the hand than the radial due to the higher mobility of these joints.[2]
Open fractures
Open fractures should have treatment with local wound care and antibiotics. Although controversial, healthcare providers are to utilize best judgment practices regarding timely debridement with removal of any dirt/debris, and primary versus secondary wound closure in the acute setting. For example, management of fight bite injuries is best with formal surgical irrigation and debridement of the MCP joint given the high risk of infection with local wound care in the emergency department only. When in doubt, clinicians should consult the hand surgical service on call at the institution.
Extensive open fracture patterns and soft tissue injury may require subsequent/serial irrigation and debridement procedures, depending on the extent of the injury. Occasionally, second look debridement 1-3 days later may be necessary.[5] Rigid fixation of the skeleton is required to repair overlying soft-tissues injuries successfully. True rigidity is achievable with plates or external fixator.[4] Definitive fixation is only possible once the wound is clean. Intravenous antibiotic therapy needs to remain until the wound has been debrided and cleaned in the operating theater. After debridement in theater and skin closure, antibiotic therapy should terminate. Antibiotics should be broad but tailored to the mechanism of injury (particularly bites, marine, or farm contamination). The importance of this is great as deep infection can be present in up to 11% of open fractures compared to about 0.5% in closed fractures treated operatively.[5]
Differential Diagnosis
Injuries to neighboring bones (carpal bones, phalanges) and associated soft tissues (ligaments, tendons) need to be excluded.
Prognosis
Prognosis depends on the exact type of fracture, the method of fixation, and any complications arising in the recovery period.
Complications
Unfortunately, irrespective of chosen treatment modality, metacarpal fractures have complications associated with them, and treating those is essential to achieve good outcomes. Scope for complications is greater with open injuries and those with a soft tissue damage component. The greater the damage to surrounding soft tissues, the poorer the outcome tends to be, and the incidence of complications increases.[5] Conversely, in young and healthy patients, complications are less common.[2]
Metacarpal fracture complications include:
- Compartment syndrome. Severe trauma and/or soft tissue injury may result in compartment syndrome of the hand whether or not the injury presents in a closed (as opposed to open) fashion.[4] Although relatively rare compared to the lower extremities, acute compartment syndrome of the hand should be ruled out in all clinical presentations associated with significant hand soft tissue swelling/deformity.[13][14]
- Stiffness. Stiffness is common and often coexists with tendon adhesions. Longer immobilization periods, as well as periosteal stripping and neurovascular injuries, increase the risk of it. Prevention includes using low profile plates, splinting in functional positions, pain control, and early mobilization. In severe cases, tenolysis might be needed to improve the outcome.[5]
- Malunion. Malunion is the most common complication and results in a deformity, which can be problematic both functionally and cosmetically. Extensors are more likely to be affected than flexors in metacarpal fractures because of bone shortening. Surgery is required to treat malunion if indicated in a particular patient.[5]
- Non-union. Non-union is a lack of bone healing four months after the injury. It is rare and commonly associated with nerve injury, infection, bone loss, and devascularizing methods of fixation. Diagnosis is made clinically with the help of radiological evidence. It can result from inadequate immobilization, failed fixation, bone loss, and poor tissue approximation. The treatment is a stable fixation with or without bone grafting. Occasionally tenolysis is also required to improve function.[5]
- Tendon rupture. Plate fixation runs a risk of tendon irritation and in worst cases, rupture. If plates are used, periosteal closure should be done whenever possible to reduce this risk.[2] Healthcare providers should evaluate extensor tendon function following operative and nonoperative management of these injuries.[15]
- Infection (including osteomyelitis). Although metacarpal osteomyelitis is rare, it requires removal of all metalwork, taking cultures from tissues, and thorough debridement. Over 50% of such infections ends in amputation.[5]
- Cold intolerance. Cold intolerance is a known complication of hand trauma and may affect over a third of patients.[4]
- Chronic pain. Intra-articular fractures have a slightly worse prognosis, with 40% of patients with metacarpal base fractures reporting chronic pain irrespective of management method. Arthrodesis can be performed to manage this if severe.[2]
- Instability. Long-term instability is a risk, particularly in thumb base fractures.[2]
Postoperative and Rehabilitation Care
Full strength and range of motion is the goal of rehabilitation. Hand exercises with light resistance such as rubber bands or squeeze ball can help if there is scarring or extensor lag develops[2]. Soft tissue recovery may be more of a problem than the bony one. Rest and elevation are important, and so is the quality of splinting - poor splinting can cause stiffness, pressure sores, or even compartment syndrome.[4]
Pearls and Other Issues
Main points on metacarpal fractures:
- Common hand injury
- Require thorough assessment consisting of the history, examination, and radiological investigations
- They mostly divide into open or closed, based on the digit they affect, intra-articular or extra-articular status, and based on the location on the bone itself (head, neck, shaft, base)
- May have conservative or operative treatment
- Can have long-term sequelae requiring further management
Enhancing Healthcare Team Outcomes
Metacarpal fractures make up about a third of all hand fractures.[11] It is crucial that healthcare staff know how to assess and manage them and when to refer them to hand surgeons for specialist treatment as prompt management of these fractures whether conservative or operative is essential for swift functional recovery. Orthopedic nurses are involved in postoperative care, educate patients and their families, and report back to the team. [Level 5] Once the immediate injury undergoes initial treatment, working closely with hand therapists can prevent some long-term complications such as stiffness.[5]
These examples of interprofessional activity will drive better outcomes. [Level 5]