Functional electrical stimulation
Functional electrical stimulation (FES) is a technique that uses low-energy electrical pulses to artificially generate body movements in individuals who have been paralyzed due to injury to the central nervous system. More specifically, FES can be used to generate muscle contraction in otherwise paralyzed limbs to produce functions such as grasping, walking, bladder voiding and standing. This technology was originally used to develop neuroprostheses that were implemented to permanently substitute impaired functions in individuals with spinal cord injury (SCI), head injury, stroke and other neurological disorders. In other words, a person would use the device each time he or she wanted to generate a desired function.[1] FES is sometimes also referred to as neuromuscular electrical stimulation (NMES).[2]
FES technology has been used to deliver therapies to retrain voluntary motor functions such as grasping, reaching and walking. In this embodiment, FES is used as a short-term therapy, the objective of which is restoration of voluntary function and not lifelong dependence on the FES device, hence the name functional electrical stimulation therapy, FES therapy (FET or FEST). In other words, the FEST is used as a short-term intervention to help the central nervous system of the person to re-learn how to execute impaired functions, instead of making the person dependent on neuroprostheses for the rest of her or his life.[3] Initial Phase II clinical trials conducted with FEST for reaching and grasping, and walking were carried out at KITE, the research arm of the Toronto Rehabilitation Institute.[4][5][6][7]
Principles
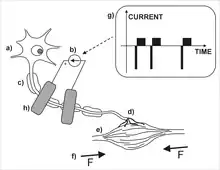
Neurons are electrically active cells.[8] In neurons, information is coded and transmitted as a series of electrical impulses called action potentials, which represent a brief change in cell electric potential of approximately 80–90 mV. Nerve signals are frequency modulated; i.e. the number of action potentials that occur in a unit of time is proportional to the intensity of the transmitted signal. Typical action potential frequency is between 4 and 12 Hz. An electrical stimulation can artificially elicit this action potential by changing the electric potential across a nerve cell membrane (this also includes the nerve axon) by inducing electrical charge in the immediate vicinity of the outer membrane of the cell.[9]
FES devices take advantage of this property to electrically activate nerve cells, which then may go on to activate muscles or other nerves.[10] However, special care must be taken in designing safe FES devices, as electric current through tissue can lead to adverse effects such as decrease in excitability or cell death. This may be due to thermal damage, electroporation of the cell membrane, toxic products from electrochemical reactions at the electrode surface, or over-excitation of the targeted neurons or muscles. Typically FES is concerned with stimulation of neurons and nerves. In some applications, FES can be used to directly stimulate muscles, if their peripheral nerves have been severed or damaged (i.e., denervated muscles).[11] However, the majority of the FES systems used today stimulate the nerves or the points where the junction occurs between the nerve and the muscle. The stimulated nerve bundle includes motor nerves (efferent nerves—descending nerves from the central nervous system to muscles) and sensory nerves (afferent nerves—ascending nerves from sensory organs to the central nervous system).
The electrical charge can stimulate both motor and sensory nerves. In some applications, the nerves are stimulated to generate localized muscle activity, i.e., the stimulation is aimed at generating direct muscle contraction. In other applications, stimulation is used to activate simple or complex reflexes. In other words, the afferent nerves are stimulated to evoke a reflex, which is typically expressed as a coordinated contraction of one or more muscles in response to the sensory nerve stimulation.
When a nerve is stimulated, i.e., when sufficient electrical charge is provided to a nerve cell, a localized depolarization of the cell wall occurs resulting in an action potential that propagates toward both ends of the axon. Typically, one "wave" of action potentials will propagate along the axon towards the muscle (orthodromic propagation) and concurrently, the other "wave" of action potentials will propagate towards the cell body in the central nervous system (antidromic propagation). While the direction of propagation in case of the antidromic stimulation and the sensory nerve stimulation is the same, i.e., towards the central nervous system, their end effects are very different. The antidromic stimulus has been considered an irrelevant side effect of FES. However, in recent years a hypothesis has been presented suggesting the potential role of the antidromic stimulation in neurorehabilitation.[12] Typically, FES is concerned with orthodromic stimulation and uses it to generate coordinated muscle contractions.
In the case where sensory nerves are stimulated, the reflex arcs are triggered by the stimulation on sensory nerve axons at specific peripheral sites. One example of such a reflex is the flexor withdrawal reflex. The flexor withdrawal reflex occurs naturally when a sudden, painful sensation is applied to the sole of the foot. It results in flexion of the hip, knee and ankle of the affected leg, and extension of the contralateral leg in order to get the foot away from the painful stimulus as quickly as possible. The sensory nerve stimulation can be used to generate desired motor tasks, such as evoking flexor withdrawal reflex to facilitate walking in individuals following stroke, or they can be used to alter reflexes or the function of the central nervous system. In the later case, the electrical stimulation is commonly described by the term neuromodulation.
Nerves can be stimulated using either surface (transcutaneous) or subcutaneous (percutaneous or implanted) electrodes. The surface electrodes are placed on the skin surface above the nerve or muscle that needs to be "activated". They are noninvasive, easy to apply, and generally inexpensive. Until recently the common belief in the FES field has been that due to the electrode-skin contact impedance, skin and tissue impedance, and current dispersion during stimulation, much higher-intensity pulses are required to stimulate nerves using surface stimulation electrodes as compared to the subcutaneous electrodes.
(This statement is correct for all commercially available stimulators except MyndMove stimulator (developed my Milos R. Popovic), which has implemented a new stimulation pulse that allows the stimulator to generate muscle contractions without causing discomfort during stimulation, which is a common problem with commercially available transcutaneous electrical stimulation systems, based on US Patents 8,880,178 (2014), 9,440,077 (2016), and 9,592,380 (2016) and related foreign patents.)[13][14][15]
A major limitation of the transcutaneous electrical stimulation is that some nerves, for example those innervating the hip flexors, are too profound to be stimulated using surface electrodes. This limitation can be partly addressed by using arrays of electrodes, which can use several electrical contacts to increase selectivity.[16][17][18]
Subcutaneous electrodes can be divided into percutaneous and implanted electrodes. The percutaneous electrodes consist of thin wires inserted through the skin and into muscular tissue close to the targeted nerve. These electrodes typically remain in place for a short period of time and are only considered for short-term FES interventions. However, it is worth mentioning that some groups, such as Cleveland FES Center, have been able to safely use percutaneous electrodes with individual patients for months and years at a time. One of the drawbacks of using the percutaneous electrodes is that they are prone to infection and special care has to be taken to prevent such events.
The other class of subcutaneous electrodes is implanted electrodes. These are permanently implanted in the consumer's body and remain in the body for the remainder of the consumer's life. Compared to surface stimulation electrodes, implanted and percutaneous electrodes potentially have higher stimulation selectivity, which is a desired characteristics of FES systems. To achieve higher selectivity while applying lower stimulation amplitudes, it is recommended that both cathode and anode are in the vicinity of the nerve that is stimulated. The drawbacks of the implanted electrodes are they require an invasive surgical procedure to install, and, as is the case with every surgical intervention, there exists a possibility of infection following implantation.
Typical stimulation protocols used in clinical FES involves trains of electric pulses. Biphasic, charged balanced pulses are employed as they improve the safety of electrical stimulation and minimize some of the adverse effects. Pulse duration, pulse amplitude and pulse frequency are the key parameters that are regulated by the FES devices. The FES devices can be current or voltage regulated. Current regulated FES systems always deliver the same charge to the tissue regardless of the skin/tissue resistance. Because of that, the current regulated FES systems do not require frequent adjustments of the stimulation intensity. The voltage regulated devices may require more frequent adjustments of the stimulation intensity as the charge that they deliver changes as the skin/tissue resistance changes. The properties of the stimulation pulse trains and how many channels are used during stimulation define how complex and sophisticated FES-induced function is. The system can be as simple such as FES systems for muscle strengthening or they can be complex such as FES systems used to deliver simultaneous reaching and grasping,[19] or bipedal locomotion.[20][21][22]
Note: This paragraph was developed in part using material from the following reference.[1] For more information on FES please consult that and other references provided in the paragraph.
History
Electrical stimulation had been utilized as far back as ancient Egypt, when it was believed that placing torpedo fish in a pool of water with a human was therapeutic. FES - which involves stimulating the target organ during a functional movement (e.g., walking, reaching for an item) - was initially referred to as functional electrotherapy by Liberson.[23] It was not until 1967 that the term functional electrical stimulation was coined by Moe and Post,[24] and used in a patent entitled, "Electrical stimulation of muscle deprived of nervous control with a view of providing muscular contraction and producing a functionally useful moment".[25] Offner's patent described a system used to treat foot drop.
The first commercially available FES devices treated foot drop by stimulating the peroneal nerve during gait. In this case, a switch, located in the heel end of a user's shoe, would activate a stimulator worn by the user.
Common applications
Spinal cord injury
Injuries to the spinal cord interfere with electrical signals between the brain and the muscles, resulting in paralysis below the level of injury. Restoration of limb function as well as regulation of organ function are the main application of FES, although FES is also used for treatment of pain, pressure, sore prevention, etc. Some examples of FES applications involve the use of neuroprostheses that allow the people with paraplegia to walk, stand, restore hand grasp function in people with quadriplegia, or restore bowel and bladder function.[26] High intensity FES of the quadriceps muscles allows patients with complete lower motor neuron lesion to increase their muscle mass, muscle fiber diameter, improve ultrastructural organization of contractile material, increase of force output during electrical stimulation and perform FES assisted stand-up exercises.[27]
Walking in spinal cord injury
Kralj and his colleagues described a technique for paraplegic gait using surface stimulation, which remains the most popular method in use today.[28] Electrodes are placed over the quadriceps muscles and peroneal nerves bilaterally. The user controls the neuroprosthesis with two pushbuttons attached to the left and right handles of a walking frame, or on canes or crutches. When the neuroprosthesis is turned on, both quadriceps muscles are stimulated to provide a standing posture. Electrodes are placed over the quadriceps muscles and peroneal nerves bilaterally. The user controls the neuroprosthesis with two pushbuttons attached to the left and right handles of a walking frame, or on canes or crutches. When the neuroprosthesis is turned on, both quadriceps muscles are stimulated to provide a standing posture.[29]
Kralj's approach was extended by Graupe et al.[29] into a digital FES system that employs the power of digital signal processing to result in the Parastep FES system, based on US Patents 5,014,705 (1991), 5,016,636 (1991), 5,070,873 (1991), 5,081,989 (1992), 5,092,329 (1992) and related foreign patents. The Parastep system became the first FES system for standing and walking to receive the US FDA approval (FDA, PMA P900038, 1994) and become commercially available.
The Parastep's digital design allows a considerable reduction in rate of patient-fatigue by drastically reducing of stimulation pulse-width (100–140 microseconds) and pulse-rate (12–24 per sec.), to result, in walking times of 20–60 minutes and average walking distances of 450 meters per walk, for adequately trained thoracic-level complete paraplegics patients who complete training that includes daily treadmill sessions,[29] with some patients exceeding one mile per walk.[30] Also, Parestep-based walking was reported to result in several medical and psychological benefits, including restoration of near-normal blood flow to lower extremities and holding of bone density decline.[31][32][29]
Walking performance with the Parastep system greatly depends on rigorous upper body conditioning-training and on a completing 3–5 months of a daily one–two-hour training program which includes 30 of more minutes of treadmill training.[29]
An alternative approach to the above techniques is the FES system for walking developed using the Compex Motion neuroprosthesis, by Popovic et al. .[33][34] Compex Motion neuroprosthesis for walking is an eight to sixteen channel surface FES system used to restore voluntary walking in stroke and spinal cord injury individuals.[4] This system does not apply peroneal nerve stimulation to enable locomotion. Instead, it activates all relevant lower limb muscles in a sequence similar to the one that brain uses to enable locomotion. The hybrid assistive systems (HAS)[35] and the RGO[36] walking neuroprostheses are devices that also apply active and passive braces, respectively. The braces were introduced to provide additional stability during standing and walking. A major limitation of neuroprostheses for walking that are based on surface stimulation is that the hip flexors cannot be stimulated directly. Therefore, hip flexion during walking must come from voluntary effort, which is often absent in paraplegia, or from the flexor withdrawal reflex. Implanted systems have the advantage of being able to stimulate the hip flexors, and therefore, to provide better muscle selectivity and potentially better gait patterns.[37] Hybrid systems with exoskeleton have been also proposed to solve this problem.[38] These technologies have been found to be successful and promising, but at the present time these FES systems are mostly used for exercise purposes and seldom as an alternative to wheelchair mobility.
Stroke and upper limb recovery
In the acute stage of stroke recovery, the use of cyclic electrical stimulation has been seen to increase the isometric strength of wrist extensors. In order to increase strength of wrist extensors, there must be a degree of motor function at the wrist spared following the stroke and have significant hemiplegia. Patients who will elicit benefits of cyclic electrical stimulation of the wrist extensors must be highly motivated to follow through with treatment. After 8 weeks of electrical stimulation, an increase in grip strength can be apparent. Many scales, which assess the level of disability of the upper extremities following a stroke, use grip strength as a common item. Therefore, increasing strength of wrist extensors will decrease the level of upper extremity disability.
Patients with hemiplegia following a stroke commonly experience shoulder pain and subluxation; both of which will interfere with the rehabilitation process. Functional electrical stimulation has been found to be effective for the management of pain and reduction of shoulder subluxation, as well as accelerating the degree and rate of motor recovery. Furthermore, the benefits of FES are maintained over time; research has demonstrated that the benefits are maintained for at least 24 months.[39]
Drop foot
Drop foot is a common symptom in hemiplegia, characterized by a lack of dorsiflexion during the swing phase of gait, resulting in short, shuffling strides. It has been shown that FES can be used to effectively compensate for the drop foot during the swing phase of the gait. At the moment just before the heel off phase of gait occurs, the stimulator delivers a stimulus to the common peroneal nerve, which results in contraction of the muscles responsible for dorsiflexion. There are currently a number of drop foot stimulators that use surface and implanted FES technologies.[40][41][42][43][44] Drop foot stimulators have been used successfully with various patient populations, such as stroke, spinal cord injury and multiple sclerosis.[45]
The term "orthotic effect" can be used to describe the immediate improvement in function observed when the individual switches on their FES device compared to unassisted walking. This improvement disappears as soon as the person switches off their FES device. In contrast, a "training" or "therapeutic effect" is used to describe a long term improvement or restoration of function following a period of using the device which is still present even when the device is switched off. A further complication to measuring an orthotic effect and any long term training or therapeutic effects is the presence of a so-called "temporary carry over effect". Liberson et al., 1961[23] was the first to observe that some stroke patients appeared to benefit from a temporary improvement in function and were able to dorsiflex their foot for up to an hour after the electrical stimulation had been turned off. It has been hypothesised that this temporary improvement in function may be linked to a long term training or therapeutic effect.
Stroke
Hemiparetic stroke patients, who are impacted by the denervation, muscular atrophy, and spasticity, typically experience an abnormal gait pattern due to muscular weakness and the incapacity to voluntary contract certain ankle and hip muscles at the appropriate walking phase. Liberson et al., (1961) were the first to pioneer FES in stroke patients.[23] More recently, there have been a number of studies that have been conducted in this area. A systematic review conducted in 2012 on the use of FES in chronic stroke included seven randomized controlled trials with a total of 231 participants. The review found a small treatment effect for using FES for the 6-minute walking test.[46]
Multiple sclerosis
FES has also been found to be useful for treating foot drop in people with multiple sclerosis. The first use was reported in 1977 by Carnstam et al., who found that it was possible to generate strength increases through using peroneal stimulation.[47][48] A more recent study examined the use of FES compared to an exercise group and found that although there was an orthotic effect for the FES group, no training effect in walking speed was found.[49] Further qualitative analysis including all participants from the same study found improvements in activities of daily living and a reduced number of falls for those using FES compared with exercise.[50] A further small scale (n=32) longitudinal observational study has found evidence for a significant training effect through using FES.[51] With NMES treatment there were measurable gains in ambulatory function.[52]
However, a further large observational study (n=187) was supportive of previous findings and found a significant improvement in orthotic effect for walking speed.[53]
Cerebral palsy
FES has been found to be useful for treating the symptoms of cerebral palsy. A recent randomised controlled trial (n=32) found significant orthotic and training effects for children with unilateral spastic cerebral palsy. Improvements were found in gastrocnemius spasticity, community mobility and balance skills.[54] A recent comprehensive literature review of the area of using electrical stimulation and FES to treat children with disabilities mostly included studies on children with cerebral palsy.[55] The reviewers summarised the evidence as the treatment having the potential to improve a number of different areas including muscle mass and strength, spasticity, passive range of motion, upper extremity function, walking speed, positioning of the foot and ankle kinematics. The review further concludes that adverse events were rare and the technology is safe and well tolerated by this population. The applications of FES for children with cerebral palsy are similar to those for adults. Some common applications of FES devices include stimulation of muscles whilst mobilizing to strengthen muscle activity, to reduce muscle spasticity, to facilitate initiation of muscle activity, or to provide a memory of movement.[56]
National Institute for Health and Care Excellence Guidelines (NICE) (UK)
NICE have issued full guidelines on the treatment of drop foot of central neurological origin[57] (IPG278). NICE have stated that "current evidence on the safety and efficacy (in terms of improving gait) of functional electrical stimulation (FES) for drop foot of central neurological origin appears adequate to support the use of this procedure provided that normal arrangements are in place for clinical governance, consent and audit".
In popular culture
- Mark Coggins' novel No Hard Feelings (2015) features a female protagonist with a spinal cord injury who regains mobility via advanced FES technology developed by a fictional biomedical startup.[58]
See also
- Electrical muscle stimulation
- Electrotherapy
- Cleveland FES Center
- Shannon Criteria
References
- 1 2 M.R. Popovic, K. Masani and S. Micera, "Chapter 9 – Functional Electrical Stimulation Therapy: Recovery of function following spinal cord injury and stroke," In press, Neurorehabilitation Technology – Second Edition, Z. Rymer, T. Nef and V. Dietz, Ed. Springer Science Publishers in November 2015.
- ↑ M. Claudia et al., (2000), Artificial Grasping System for the Paralyzed Hand, International Society for Artificial Organs, Vol. 24 No. 3
- ↑ M.K. Nagai, C. Marquez-Chin, and M.R. Popovic, "Why is functional electrical stimulation therapy capable of restoring motor function following severe injury to the central nervous system?" Translational Neuroscience, Mark Tuszynski, Ed. Springer Science and Business Media LLC, pp: 479-498, 2016.
- 1 2 Kapadia N., Masani K., Craven B.C., Giangregorio L.M., Hitzig S.L., Richards K., Popovic M.R. (2014). "A randomized trial of functional electrical stimulation for walking in incomplete spinal cord injury: Effects on walking competency". The Journal of Spinal Cord Medicine. 37 (5): 511–524. doi:10.1179/2045772314y.0000000263. PMC 4166186. PMID 25229735.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Thrasher, T. Adam; Zivanovic, Vera; McIlroy, William; Popovic, Milos R. (29 October 2008). "Rehabilitation of Reaching and Grasping Function in Severe Hemiplegic Patients Using Functional Electrical Stimulation Therapy". Neurorehabilitation and Neural Repair. 22 (6): 706–714. doi:10.1177/1545968308317436. PMID 18971385.
- ↑ Marquez-Chin, Cesar; Bagher, Shaghayegh; Zivanovic, Vera; Popovic, Milos R. (17 January 2017). "Functional electrical stimulation therapy for severe hemiplegia: Randomized control trial revisited: La simulation électrique fonctionnelle pour le traitement d'une hémiplégie sévère : un essai clinique aléatoire revisité". Canadian Journal of Occupational Therapy. 84 (2): 87–97. doi:10.1177/0008417416668370. PMID 28093928.
- ↑ Popovic, Milos R.; Kapadia, Naaz; Zivanovic, Vera; Furlan, Julio C.; Craven, B. Cathy; McGillivray, Colleen (June 2011). "Functional Electrical Stimulation Therapy of Voluntary Grasping Versus Only Conventional Rehabilitation for Patients With Subacute Incomplete Tetraplegia: A Randomized Clinical Trial". Neurorehabilitation and Neural Repair. 25 (5): 433–442. doi:10.1177/1545968310392924. ISSN 1545-9683. PMID 21304020.
- ↑ Guyton and Hall Textbook of Medical Physiology, John Hall, 13th edition, Elsevier Health Sciences, 31 May 2015
- ↑ M.R. Popovic and T.A. Thrasher, "Neuroprostheses", in Encyclopedia of Biomaterials and Biomedical Engineering, G.E. Wnek and G.L. Bowlin, Eds.: Marcel Dekker, Inc., vol. 2, pp. 1056–1065, 2004.
- ↑ Control of Movement for the Physically Disabled: Control for Rehabilitation Technology, Dejan Popovic and Thomas Sinkjaer, Springer Science & Business Media, 6 December 2012.
- ↑ Reichel M, Breyer T, Mayr W, Rattay F (2002). "Simulation of the three-dimensional electrical field in the course of functional electrical stimulation". Artificial Organs. 26 (3): 252–255. doi:10.1046/j.1525-1594.2002.06945.x. PMID 11940026.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Rushton D (2003). "Functional electrical stimulation and rehabilitation—an hypothesis". Med Eng Phys. 25 (1): 75–78. doi:10.1016/s1350-4533(02)00040-1. PMID 12485788.
- ↑ , "Functional electrical stimulation device and system, and use thereof", issued 2011-06-02
- ↑ , "Functional electrical stimulation device and system, and use thereof", issued 2014-09-29
- ↑ , "Electrical stimulation system with pulse control", issued 2014-03-13
- ↑ Kuhn A, Keller T, Micera S, Morari (2009). "a simulation study". Medical Engineering & Physics. 31 (8): 945–951. doi:10.1016/j.medengphy.2009.05.006. PMID 19540788.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Micera S, Keller T, Lawrence M, Morari M, Popović DB (2010). "Wearable neural prostheses. Restoration of sensory-motor function by transcutaneous electrical stimulation". IEEE Engineering in Medicine and Biology Magazine. 29 (3): 64–69. doi:10.1109/memb.2010.936547. PMID 20659859. S2CID 24863622.
- ↑ Popović DB, Popović MB (2009). "Automatic determination of the optimal shape of a surface electrode: selective stimulation". Journal of Neuroscience Methods. 178 (1): 174–181. doi:10.1016/j.jneumeth.2008.12.003. PMID 19109996. S2CID 447158.
- ↑ Popovic MR, Thrasher TA, Zivanovic P, Takaki M, Hajek P (2005). "Neuroprosthesis for Retraining Reaching and Grasping Functions in Severe Hemiplegic Patients". Neuromodulation. 8 (1): 58–72. doi:10.1111/j.1094-7159.2005.05221.x. PMID 22151384.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Bajd T, Kralj A, Stefancic M, Lavrac N (1999). "Use of functional electrical stimulation in the lower extremities of incomplete spinal cord injured patients". Artificial Organs. 23 (5): 403–409. doi:10.1046/j.1525-1594.1999.06360.x. PMID 10378929.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Kapadia N, Masani K, Craven BC, Giangregorio LM, Hitzig SL, Richards K, Popovic (2014). "Effects on walking competency". The Journal of Spinal Cord Medicine. 37 (5): 511–524. doi:10.1179/2045772314y.0000000263. PMC 4166186. PMID 25229735.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Bailey SN, Hardin EC, Kobetic R, Boggs LM, Pinault G, Triolo RJ (2010). "Neurotherapeutic and neuroprosthetic effects of implanted functional electrical stimulation for ambulation after incomplete spinal cord injury". Journal of Rehabilitation Research and Development. 47 (1): 7–16. doi:10.1682/JRRD.2009.03.0034. PMID 20437323.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - 1 2 3 Liberson, W. T.; Holmquest, H. J.; Scot, D.; Dow, M. (1961). "Functional electrotherapy: Stimulation of the peroneal nerve synchronized with the swing phase of the gait of hemiplegic patients". Archives of Physical Medicine and Rehabilitation. 42: 101–105. PMID 13761879.
- ↑ Moe J. H., Post H. W. (1962). "Functional electrical stimulation for ambulation in hemiplegia". The Journal-Lancet. 82: 285–288. PMID 14474974.
- ↑ Offner et al. (1965), Patent 3,344,792
- ↑ Pow–ell, Joanna; David Pandyan; Malcolm Granat; Margart Cameron; David Stott (1999). "Electrical Stimulation of Wrist Extensors in Poststroke Hemiplegia". Stroke. 30 (7): 1384–1389. doi:10.1161/01.STR.30.7.1384. PMID 10390311.
- ↑ Kern H, Carraro U, Adami N, Biral D, Hofer C, Forstner C, Mödlin M, Vogelauer M, Pond A, Boncompagni S, Paolini C, Mayr W, Protasi F, Zampieri S (2010). "Home-based functional electrical stimulation rescues permanently denervated muscles in paraplegic patients with complete lower motor neuron lesion". Neurorehabil Neural Repair. 24 (8): 709–721. doi:10.1177/1545968310366129. PMID 20460493. S2CID 5963094.
- ↑ Kralj A, Bajd T, and Turk R. "Enhancement of gait restoration in spinal injured patients by functional electrical stimulation. Clin Orthop Relat Res 1988; 34–43
- 1 2 3 4 5 Graupe D, Davis R, Kordylewski H, Kohn K (1998). "Ambulation by traumatic T4-12 paraplegics using functional neuromuscular stimulation". Crit Rev Neurosurg. 8 (4): 221–231. doi:10.1007/s003290050081. PMID 9683682.
- ↑ Daniel Graupe (27 January 2012). "PARASTEP 30 min walk by compete paraplegic UNBRACED PARAPLEG-70.divx". Archived from the original on 21 December 2021. Retrieved 15 April 2019 – via YouTube.
- ↑ Nash N S, Jacobs P L, Montalvo B M, Klose K J, Guest B, Needham-Shroshire M (1997). "Evaluation of a training program for persons with SCI paraplegia using the Parastep®1 ambulation system: Part 5. Lower extremity blood flow and hyperemic responses to occlusion are augmented by ambulation training". Archives of Physical Medicine and Rehabilitation. 78 (8): 808–814. doi:10.1016/S0003-9993(97)90192-1. PMID 9344298.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Gater D R, Dolbow D, Tsui B, Gorgey A S (2011). "Functional electrical stimulation therapies after spinal cord injury". NeuroRehabilitation. 28 (3): 231–248. doi:10.3233/nre-2011-0652. PMID 21558629.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Popovic MR, Keller T (2005). "Modular transcutaneous functional electrical stimulation system". Medical Engineering & Physics. 27 (1): 81–92. doi:10.1016/j.medengphy.2004.08.016. PMID 15604009.
- ↑ Thrasher TA, Flett HM, Popovic MR (2006). "Gait training regimen for incomplete spinal cord injury using functional electrical stimulation". Spinal Cord. 44 (6): 357–361. doi:10.1038/sj.sc.3101864. PMID 16249784.
- ↑ Popovic D, Tomović R, Schwirtlich L (1989). "Hybrid assistive system--the motor neuroprosthesis". IEEE Transactions on Bio-Medical Engineering. 36 (7): 729–737. CiteSeerX 10.1.1.126.9159. doi:10.1109/10.32105. PMID 2787281. S2CID 14663596.
- ↑ Solomonow M, Baratta R, Hirokawa S, Rightor N, Walker W, Beaudette P, Shoji H, D'Ambrosia R (1989). "The RGO Generation II: muscle stimulation powered orthosis as a practical walking system for thoracic paraplegics". Orthopedics. 12 (10): 1309–1315. doi:10.3928/0147-7447-19891001-06. PMID 2798239.
- ↑ Triolo RJ, Bieri C, Uhlir J, Kobetic R, Scheiner A, Marsolais EB (1996). "Implanted Functional Neuromuscular Stimulation systems for individuals with cervical spinal cord injuries: clinical case reports". Archives of Physical Medicine and Rehabilitation. 77 (11): 1119–1128. doi:10.1016/s0003-9993(96)90133-1. PMID 8931521.
- ↑ Kobetic R, To CS, Schnellenberger JR, Audu ML, Bulea TC, Gaudio R, Pinault G, Tashman S, Triolo RJ (2009). "Development of hybrid orthosis for standing, walking, and stair climbing after spinal cord injury". Journal of Rehabilitation Research and Development. 46 (3): 447–462. doi:10.1682/JRRD.2008.07.0087. PMID 19675995. S2CID 12626060.
- ↑ Chantraine, Alex; Baribeault, Alain; Uebelhart, Daniel; Gremion, Gerald (1999). "Shoulder Pain and Dysfunction in Hemiplegia: Effects of Functional Electrical Stimulation". Archives of Physical Medicine and Rehabilitation. 80 (3): 328–331. doi:10.1016/s0003-9993(99)90146-6. PMID 10084443.
- ↑ Taylor PN, Burridge JH, Dunkerley AL, Wood DE, Norton JA, Singleton C, Swain ID (1999). "Clinical use of the Odstock dropped foot stimulator: its effect on the speed and effort of walking". Archives of Physical Medicine and Rehabilitation. 80 (12): 1577–1583. doi:10.1016/s0003-9993(99)90333-7. PMID 10597809.
- ↑ Stein RB, Everaert DG, Thompson AK, Chong SL, Whittaker M, Robertson J, Kuether G (2010). "Long-term therapeutic and orthotic effects of a foot drop stimulator on walking performance in progressive and nonprogressive neurological disorders". Neurorehabilitation and Neural Repair. 24 (2): 152–167. doi:10.1177/1545968309347681. PMID 19846759. S2CID 5977665.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Hausdorff JM, Ring H (2008). "Effects of a new radio frequency-controlled neuroprosthesis on gait symmetry and rhythmicity in patients with chronic hemiparesis". American Journal of Physical Medicine & Rehabilitation. 87 (1): 4–13. doi:10.1097/phm.0b013e31815e6680. PMID 18158427. S2CID 10860495.
- ↑ Burridge JH, Haugland M, Larsen B, Svaneborg N, Iversen HK, Christensen PB, Pickering RM, Sinkjaer T (2008). "Patients' perceptions of the benefits and problems of using the ActiGait implanted drop-foot stimulator". J Rehabil Med. 40 (10): 873–875. doi:10.2340/16501977-0268. PMID 19242627.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Kenney L, Bultstra G, Buschman R, Taylor P, Mann G, Hermens H, Holsheimer J, Nene A, Tenniglo M, van der Aa H, Hobby J (2002). "An implantable two channel drop foot stimulator: initial clinical results". Artificial Organs. 26 (3): 267–270. doi:10.1046/j.1525-1594.2002.06949.x. PMID 11940030.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Alnajjar, Fady; Zaier, Riadh; Khalid, Sumayya; Gochoo, Munkhjargal (28 December 2020). "Trends and Technologies in Rehabilitation of Foot Drop: A Systematic Review". Expert Review of Medical Devices. 18 (1): 31–46. doi:10.1080/17434440.2021.1857729. ISSN 1743-4440.
- ↑ Pereira, Shelialah; Mehta, Swati; McIntyre, Amanda; Lobo, Liane; Teasell, Robert W. (1 December 2012). "Functional electrical stimulation for improving gait in persons with chronic stroke". Topics in Stroke Rehabilitation. 19 (6): 491–498. doi:10.1310/tsr1906-491. ISSN 1074-9357. PMID 23192714. S2CID 7908908.
- ↑ Cook AW (1976). "Electrical stimulation in multiple sclerosis". Hosp Pract. 11 (4): 51–8. doi:10.1080/21548331.1976.11706516. PMID 1088368.
- ↑ Carnstam, B.; Larsson, L. E.; Prevec, T. S. (1 January 1977). "Improvement of gait following functional electrical stimulation. I. Investigations on changes in voluntary strength and proprioceptive reflexes". Scandinavian Journal of Rehabilitation Medicine. 9 (1): 7–13. ISSN 0036-5505. PMID 302481.
- ↑ Barrett, C. L.; Mann, G. E.; Taylor, P. N.; Strike, P. (1 April 2009). "A randomized trial to investigate the effects of functional electrical stimulation and therapeutic exercise on walking performance for people with multiple sclerosis". Multiple Sclerosis (Houndmills, Basingstoke, England). 15 (4): 493–504. doi:10.1177/1352458508101320. ISSN 1352-4585. PMID 19282417. S2CID 5080471.
- ↑ Esnouf, J. E.; Taylor, P. N.; Mann, G. E.; Barrett, C. L. (1 September 2010). "Impact on activities of daily living using a functional electrical stimulation device to improve dropped foot in people with multiple sclerosis, measured by the Canadian Occupational Performance Measure". Multiple Sclerosis (Houndmills, Basingstoke, England). 16 (9): 1141–1147. doi:10.1177/1352458510366013. ISSN 1477-0970. PMID 20601398. S2CID 19846734.
- ↑ Stein, Richard B.; Everaert, Dirk G.; Thompson, Aiko K.; Chong, Su Ling; Whittaker, Maura; Robertson, Jenny; Kuether, Gerald (1 February 2010). "Long-term therapeutic and orthotic effects of a foot drop stimulator on walking performance in progressive and nonprogressive neurological disorders". Neurorehabilitation and Neural Repair. 24 (2): 152–167. doi:10.1177/1545968309347681. ISSN 1552-6844. PMID 19846759. S2CID 5977665.
- ↑ Wahls TL, Reese D, Kaplan D, Darling WG (2010). "Rehabilitation with neuromuscular electrical stimulation leads to functional gains in ambulation in patients with secondary progressive and primary progressive multiple sclerosis: a case series report". J Altern Complement Med. 16 (12): 1343–9. doi:10.1089/acm.2010.0080. PMID 21138391.
- ↑ Street, Tamsyn; Taylor, Paul; Swain, Ian (1 April 2015). "Effectiveness of functional electrical stimulation on walking speed, functional walking category, and clinically meaningful changes for people with multiple sclerosis". Archives of Physical Medicine and Rehabilitation. 96 (4): 667–672. doi:10.1016/j.apmr.2014.11.017. ISSN 1532-821X. PMID 25499688.
- ↑ Pool, Dayna; Valentine, Jane; Bear, Natasha; Donnelly, Cyril J.; Elliott, Catherine; Stannage, Katherine (1 January 2015). "The orthotic and therapeutic effects following daily community applied functional electrical stimulation in children with unilateral spastic cerebral palsy: a randomised controlled trial". BMC Pediatrics. 15: 154. doi:10.1186/s12887-015-0472-y. ISSN 1471-2431. PMC 4603297. PMID 26459358.
- ↑ Bosques, Glendaliz; Martin, Rebecca; McGee, Leah; Sadowsky, Cristina (31 May 2016). "Does therapeutic electrical stimulation improve function in children with disabilities? A comprehensive literature review". Journal of Pediatric Rehabilitation Medicine. 9 (2): 83–99. doi:10.3233/PRM-160375. ISSN 1875-8894. PMID 27285801.
- ↑ Singleton, Christine; Jones, Helen; Maycock, Lizz (2019). "Functional electrical stimulation (FES) for children and young people with cerebral palsy". Paediatrics and Child Health. 29 (11): 498–502. doi:10.1016/j.paed.2019.07.015. ISSN 1751-7222.
- ↑ "Functional electrical stimulation for drop foot of central neurological origin | Guidance and guidelines | NICE". www.nice.org.uk. Retrieved 14 June 2016.
- ↑ "The Rap Sheet, "The Story Behind the Story: No Hard Feelings by Mark Coggins"". 28 August 2015. Retrieved 10 February 2016.
Further reading
- Chudler, Eric H. "Neuroscience For Kids - Cells of the Nervous System." UW Faculty Web Server. Eric H. Chudler, 1 June 2011. Web. 7 June 2011.<http://faculty.washington.edu/chudler/cells.html>.
- Cooper E.B., Scherder E.J.A., Cooper J.B (2005) "Electrical treatment of reduced consciousness: experience with coma and Alzheimer's disease," Neuropsyh Rehab (UK).Vol. 15,389-405.
- Cooper E.B, Cooper J.B. (2003). "Electrical treatment of coma via the median nerve". Acta Neurochirurg Supp. 87: 7–10. doi:10.1007/978-3-7091-6081-7_2. ISBN 978-3-7091-7223-0. PMID 14518514.
- "FEScenter.org » Cleveland FES Center." FEScenter.org » Home. Cleveland VA Medical Center, Case Western Reserve University, MetroHealth Medical Center, 3 June 2011. Web. 8 June 2011. <http://fescenter.org/index.php?option=com_content>
- Graupe D (2002). "An overview of the state of the art of noninvasive FES for independent ambulation by thoracic level paraplegics". Neurological Research. 24 (5): 431–442. doi:10.1179/016164102101200302. PMID 12117311. S2CID 29537770.
- Graupe D, Cerrel-Bazo H, Kern H, Carraro U (2008). "Walking Performance, Medical Outcomes and Patient Training in FES of Innervated Muscles for Ambulation by Thoracic-Level Complete Paraplegics". Neurol. Res. 31 (2): 123–130. doi:10.1179/174313208X281136. PMID 18397602. S2CID 34621751.
- Johnston, Laurance. "FES." Human Spinal Chord Injury: New & Emerging Therapies. Institute of Spinal Cord Injury, Iceland. Web. 7 June 2011. <http://www.sci-therapies.info/FES.htm>.
- Lichy A., Libin A., Ljunberg I., Groach L., (2007) " Preserving bone health after acute spinal cord injury: Differential responses to a neuromuscular electrical stimulation intervention", Proc. 12th Annual Conf. of the International FES Soc., Philadelphia, PA, Session 2, Paper 205.
- Liu Yi-Liang, Ling Qi-Dan, Kang En-Tang, Neoh Koon-Gee, Liaw Der-Jang, Wang Kun-Li, Liou Wun-Tai, Zhu Chun-Xiang, Siu-Hung Chan Daniel (2009). "Volatile Electrical Switching in a Functional Polyimide Containing Electron-donor and -acceptor Moieties". Journal of Applied Physics. 105 (4): 1–9. Bibcode:2009JAP...105d4501L. doi:10.1063/1.3077286.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - Nolte, John, and John Sundsten. The Human Brain: an Introduction to Its Functional Anatomy. 5th ed. St. Louis: Mosby, 2002.
- Rosenzweig, Mark R., Arnold L. Leiman, and S. Marc. Breedlove. Biological Psychology. Sunderland: Sinauer Associates, 2003.
- Wilkenfeld Ari J., Audu Musa L., Triolo Ronald J. (2006). "Feasibility of Functional Electrical Stimulation for Control of Seated Posture after Spinal Cord Injury: A Simulation Study". The Journal of Rehabilitation Research and Development. 43 (2): 139–43. doi:10.1682/jrrd.2005.06.0101. PMID 16847781.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - Yuan Wang, Ming Zhang, Rana Netra, Hai Liu, Chen-wang Jin, Shao-hui Ma (2010). "A Functional Magnetic Resonance Imaging Study of Human Brain in Pain-related Areas Induced by Electrical Stimulation with Different Intensities". Neurology India. 58 (6): 922–27. doi:10.4103/0028-3886.73748. PMID 21150060.
{{cite journal}}: CS1 maint: multiple names: authors list (link)