Presumed ocular histoplasmosis syndrome
Presumed ocular histoplasmosis syndrome (POHS) is a syndrome affecting the eye, which is characterized by peripheral atrophic chorioretinal scars, atrophy or scarring adjacent to the optic disc and maculopathy.
| Presumed ocular histoplasmosis syndrome | |
|---|---|
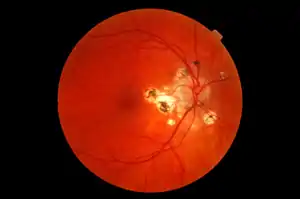 | |
| Retinal photograph of ocular histoplasmosis | |
| Specialty | Ophthalmology |
The loss of vision in POHS is caused by choroidal neovascularization.
Presentation
The diagnosis of POHS is based on the clinical triad of multiple white, atrophic choroidal scars, peripapillary pigment changes (dark spots around optic disc of the eye), and a maculopathy caused by choroidal neovascularization.
Completely distinct from POHS, acute ocular histoplasmosis may rarely occur in immunodeficiency.[1][2]
Causes
Despite its name, the "presumed" relationship of POHS to Histoplasma capsulatum is controversial and has been questioned by a number of medical professionals.[3][4][5] The fungus has rarely been isolated from cases with POHS,[6] the condition has also been found in locations where histoplasmosis is rare,[7] and there appears to be a relationship with tobacco smoking.
Diagnosis
Fluorescein angiography is usually performed for diagnosis and follow-up of patients with POHS.
Treatment
Treatment requires careful consideration of angiographic findings when a choroidal neovascular membrane is suspected which is a condition that responds to treatment. A vitreo-retinal specialist (an ophthalmologist specialized in treatment of retinal diseases) should be consulted for proper management of the case.
Presumed ocular histoplasmosis syndrome and age-related macular degeneration (AMD) have been successfully treated with laser, anti-vascular endothelial growth factors and photodynamic therapy. Ophthalmologists are using anti-vascular endothelial growth factors to treat AMD and similar conditions since research indicates that vascular endothelial growth factor (VEGF) is one of the causes for the growth of the abnormal vessels that cause these conditions.
See also
References
- Macher A, Rodrigues MM, Kaplan W, Pistole MC, McKittrick A, Lawrinson WE, Reichert CM (1985). "Disseminated bilateral chorioretinitis due to Histoplasma capsulatum in a patient with the acquired immunodeficiency syndrome". Ophthalmology. 92 (8): 1159–64. doi:10.1016/s0161-6420(85)33921-0. PMID 2413418.
- Gonzales, C. A.; Scott, I. U.; Chaudhry, N. A.; Luu, K. M.; Miller, D; Murray, T. G.; Davis, J. L. (2000). "Endogenous endophthalmitis caused by Histoplasma capsulatum var. Capsulatum: A case report and literature review". Ophthalmology. 107 (4): 725–9. doi:10.1016/s0161-6420(99)00179-7. PMID 10768335.
- Thuruthumaly C; Yee D. C.; Rao P. K. (2014). "Presumed ocular histoplasmosis". Current Opinion in Ophthalmology. 25 (6): 508–12. doi:10.1097/ICU.0000000000000100. PMID 25237930. S2CID 43761401.
- Nielsen J. S.; Fick T. A.; Saggau D. D.; Barnes C. H. (2012). "Intravitreal anti-vascular endothelial growth factor therapy for choroidal neovascularization secondary to ocular histoplasmosis syndrome". Retina. 32 (3): 468–72. doi:10.1097/IAE.0b013e318229b220. PMID 21817958. S2CID 25507234.
- Woods AC; Wahlen HE (1959). "The probable role of benign histoplasmosis in the etiology of granulomatous uveitis". Transactions of the American Ophthalmological Society. 57: 318–347. PMC 1316339. PMID 16693576.
- Presumed Ocular Histoplasmosis Syndrome
- Stefan Dithmar; Frank Gerhard Holz (28 April 2008). Fluorescence Angiography in Ophthalmology. Springer. pp. 168–. ISBN 978-3-540-78359-6. Retrieved 29 June 2010.
- Ehrlich R, Ciulla TA, Maturi R, et al. (2009). "Intravitreal bevacizumab for choroidal neovascularization secondary to presumed ocular histoplasmosis syndrome". Retina (Philadelphia, Pa.). 29 (10): 1418–23. doi:10.1097/IAE.0b013e3181babdf1. PMID 19898179. S2CID 44374405.