Rett syndrome
Rett syndrome (RTT) is a genetic disorder that typically becomes apparent after 6–18 months of age and almost exclusively in females.[3] Symptoms include impairments in language and coordination, and repetitive movements.[3] Those affected often have slower growth, difficulty walking, and a smaller head size.[3][4] Complications of Rett syndrome can include seizures, scoliosis, and sleeping problems.[3] The severity of the condition is variable.[4]
| Rett syndrome | |
|---|---|
| Other names | Cerebroatrophic hyperammonemia (obsolete),[1] dementia, ataxia, and loss of purposeful hand use syndrome[2] |
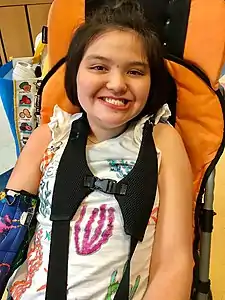 | |
| A girl with Rett Syndrome smiling at the camera | |
| Specialty | Psychiatry, pediatrics, neurology |
| Symptoms | Impairments in language and coordination, and repetitive movements, slower growth, smaller head[3] |
| Complications | Seizures, scoliosis, sleeping problems[3] |
| Usual onset | After 6–18 months of age[3] |
| Duration | Lifelong[4] |
| Causes | Mutation in the MECP2 gene[3] |
| Diagnostic method | Based on symptoms, genetic testing[4] |
| Differential diagnosis | Angelman syndrome, autism, cerebral palsy, Childhood disintegrative disorder, various neurodegenerative disorders[5] |
| Treatment | Special education, physiotherapy, braces[4] |
| Medication | Anticonvulsants[4] |
| Prognosis | Life expectancy for many is middle age.[4] |
| Frequency | 1 in 8,500 females[3] Lethal in males, with rare exceptions. |
Rett syndrome is due to a genetic mutation in the MECP2 gene,[3] on the X chromosome.[4] It almost always occurs as a new mutation, with less than one percent of cases being inherited.[3][4] It occurs almost exclusively in girls;[3] boys who have a similar mutation typically die shortly after birth.[4] Diagnosis is based on the symptoms and can be confirmed with genetic testing.[4]
There is no known cure for Rett syndrome.[4] Treatment is directed at improving symptoms.[4] Anticonvulsants may be used to help with seizures.[4] Special education, physiotherapy, and leg braces may also be useful depending on the needs of the child.[4] Many of those with the condition live into middle age.[4]
The condition affects about 1 in 8,500 females.[3] In 1999, Lebanese-American physician Huda Zoghbi discovered the mutation that causes the condition.[6][7]
Signs and symptoms
Stage I
Stage I, called early-onset, typically begins between 6 and 18 months of age.[4] This stage is often overlooked because symptoms of the disorder may be somewhat vague, and parents and doctors may not notice the subtle slowing of development at first.[4] The infant may begin to show less eye contact and have reduced interest in toys. There may be delays in gross motor skills such as sitting or crawling.[4] Hand-wringing and decreasing head growth may occur, but not enough to draw attention. This stage usually lasts for a few months but can continue for more than a year.[4]
Stage II
Stage II, or the rapid destructive stage, usually begins between ages 1 and 4 and may last for weeks or months.[4] Its onset may be rapid or gradual as the child loses purposeful hand skills and spoken language.[4] Characteristic hand movements such as wringing, washing, clapping, or tapping, as well as repeatedly moving the hands to the mouth often begin during this stage which is called mouthing.[4] The child may hold the hands clasped behind the back or held at the sides, with random touching, grasping, and releasing.[4] The movements continue while the child is awake but disappear during sleep.[4] Breathing irregularities such as episodes of apnea and hyperventilation may occur, although breathing usually improves during sleep.[4] Some girls also display autistic-like symptoms such as loss of social interaction and communication.[4] Walking may be unsteady and initiating motor movements can be difficult. Slowed head growth is usually noticed during this stage.[4]
Stage III
Stage III, or the plateau or pseudo-stationary stage, usually begins between ages 2 and 10 and can last for years.[4] Apraxia, motor problems, and seizures are prominent during this stage.[4] However, there may be improvement in behavior, with less irritability, crying, and autistic-like features.[4] In stage III there may be more interest in the surroundings and alertness, attention span, and communication skills may improve.[4] Many girls remain in this stage for most of their lives.[4]
Stage IV
Stage IV, or the late motor deterioration stage, can last for years or decades.[4] Prominent features include reduced mobility, curvature of the spine, and muscle weakness, rigidity, spasticity, and increased muscle tone with abnormal posturing of an arm or leg.[4] Girls who were previously able to walk may stop walking.[4] Cognition, communication, or hand skills generally do not decline in stage IV.[4] Repetitive hand movements may decrease and eye gaze usually improves.[4]
Variants
The signs and symptoms of the typical form of the Rett syndrome are well described. In addition to the classical form of Rett syndrome, several atypical forms have been described over the years;[8] the main groups are:
- Congenital variant (Rolando variant): in this severe subtype of Rett syndrome, the development of the patients and their head circumference are abnormal from birth.[9] The typical gaze of Rett syndrome patients is usually absent;
- Zappella variant of Rett Syndrome or preserved speech variant: in this subtype of Rett syndrome the patients acquire some manual skills and language is partially recovered around the age of 5 years (that is after the regression phase). Height, weight and head circumference are often in the normal range, and a good gross motor function can be observed.[10][11][12][13][14][15] The Zappella variant is a milder form of Rett syndrome;
- Hanefeld variant or early epilepsy variant. In this form of Rett syndrome, the patients have epilepsy before 5 months of age.[16]
The definition itself of the Rett syndrome has been refined over the years: as the atypical forms subsist near to the classical form (Hagberg & Gillberg, 1993), the "Rett Complex" terminology has been introduced.[17][18]
Cause
Genetically, Rett syndrome (RTT) is caused by mutations in the gene MECP2 located on the X chromosome (which is involved in transcriptional silencing and epigenetic regulation of methylated DNA), and can arise sporadically or from germline mutations. In less than 10% of RTT cases, mutations in the genes CDKL5 or FOXG1 have also been found to resemble it. Rett syndrome is initially diagnosed by clinical observation, but the diagnosis is definitive when there is a genetic defect in the MECP2 gene.
It has been argued that Rett syndrome is in fact a neurodevelopmental condition as opposed to a neurodegenerative condition. One piece of evidence for this is that mice with induced Rett Syndrome show no neuronal death, and some studies have suggested that their phenotypes can be partially rescued by adding functional MECP2 gene back when they are adults. This information has also helped lead to further studies aiming to treat the disorder.[19]
Sporadic mutations
In at least 95% of Rett syndrome cases, the cause is a de novo mutation in the child. That is, it is not inherited from either parent. Parents are generally genotypically normal, without a MECP2 mutation.
In cases of the sporadic form of RTT, the mutated MECP2 is thought to derive almost exclusively from a de novo mutation on the male copy of the X chromosome.[20] It is not yet known what causes the sperm to mutate, and such mutations are rare.
Germline mutations
It can also be inherited from phenotypically normal mothers who have a germline mutation in the gene encoding methyl-CpG-binding protein-2, MeCP2.[21] In these cases, inheritance follows an X-linked dominant pattern and is seen almost exclusively in females, as most males die in utero or shortly after birth.[22] MECP2 is found near the end of the long arm of the X chromosome at Xq28. An atypical form of RTT, characterized by infantile spasms or early onset epilepsy, can also be caused by a mutation to the gene encoding cyclin-dependent kinase-like 5 (CDKL5). As stated by Aine Merwick, Margaret O'Brien, and Norman Delanty in an article on gene disorders titled Complex single gene disorders and epilepsy, "Rett syndrome affects one in every 12,500 female live births by age 12 years."[23]
Mechanism

Pontine noradrenergic deficits
Brain levels of norepinephrine are lower in people with Rett syndrome[24] (reviewed in[25]). The genetic loss of MECP2 changes the properties of cells in the locus coeruleus, the exclusive source of noradrenergic innervation to the cerebral cortex and hippocampus.[26][27] These changes include hyperexcitability and decreased functioning of its noradrenergic innervation.[28] Moreover, a reduction of the tyrosine hydroxylase (Th) mRNA level, the rate-limiting enzyme in catecholamine synthesis, was detected in the whole pons of MECP2-null male as well as in adult heterozygous (MECP2+/-) female mice.[29] Using immunoquantitative techniques, a decrease of Th protein staining level, number of locus coeruleus Th-expressing neurons and density of dendritic arborization surrounding the structure was shown in symptomatic MeCP2-deficient mice.[29] However, locus coeruleus cells are not dying, but are more likely losing their fully mature phenotype, since no apoptotic neurons in the pons were detected.[29]
Researchers have concluded that "Because these neurons are a pivotal source of norepinephrine throughout the brainstem and forebrain and are involved in the regulation of diverse functions disrupted in Rett syndrome, such as respiration and cognition, we hypothesize that the locus coeruleus is a critical site at which loss of MECP2 results in CNS dysfunction." The restoration of normal locus coeruleus function may therefore be of potential therapeutic value in the treatment of Rett syndrome.[28][29]
Midbrain dopaminergic disturbances
The majority of dopamine in the mammalian brain is synthesized by nuclei located in the mesencephalon. The substantia nigra pars compacta (SNpc), the ventral tegmental area (VTA) and the retrorubral field (RRF) contain dopaminergic neurons expressing tyrosine hydroxylase (Th, i.e. the rate-limiting enzyme in catecholamine synthesis).[30][31][32]
The nigro-striatal pathway originates from the SNpc; its principal rostral target is the caudate-putamen (CPu), which it irradiates through the median forebrain bundle (MFB). This connection is involved in the tight modulation of motor strategies computed by a cortico-basal ganglia-thalamo-cortical loop.[33]
Indeed, based on the canonical anatomofunctional model of basal ganglia, nigrostriatal dopamine is able to modulate the motor loop by acting on dopaminergic receptors located on striatal GABAergic medium spiny neurons.[34]
Dysregulation of the nigrostriatal pathway is causative from Parkinson disease (PD) in humans.[35] Toxic and/or genetic ablation of SNpc neurons produces experimental parkinsonism in mice and primates.[36] The common features of PD and PD animal models are motor impairments[37] (hypotonia, bradykinesia, hypokinesia).
RTT pathology, in some aspects, overlaps the motor phenotype observed in PD patients.[38][39][40] Several neuropathological studies on postmortem brain samples argued for an SNpc alteration, evidenced by neuromelanin hypopigmentation, reduction in the structure area, and even, controversially, signs of apoptosis. In parallel, a hypometabolism was underlined by a reduction of several catecholamines (dopamine, noradrenaline, adrenaline) and their principal metabolic by-products.[25] Mouse models of RTT are available; the most studied are constitutively deleted Mecp2 mice developed by Adrian Bird or Katelyn McCormick laboratories.[41][42][43][44]
In accordance with the motor spectrum of the RTT phenotype, Mecp2-null mice show motor abnormalities from postnatal day 30 that worsen until death. These models offer a crucial substrate to elucidate the molecular and neuroanatomical correlates of MeCP2-deficiency.[45] Recently (2008), it was shown that the conditional deletion of Mecp2 in catecholaminergic neurons (by crossing of Th-Cre mice with loxP-flanked Mecp2 ones) recapitulates a motor symptomatology; it was further documented that brain levels of Th in mice lacking MeCP2 in catecholaminergic neurons only are reduced, participating to the motor phenotype.[46]
However, the most studied model for the evaluation of therapeutics is the Mecp2-null mouse (totally devoid of MeCP2). In this context, a reduction in the number and soma size of Th-expressing neurons is present from 5 weeks of age and is accompanied by a decrease of Th immunoreactivity in the caudate-putamen, the principal target of dopaminergic neurons arising from the SNpc.[47] Moreover, a neurochemical analysis of dopaminergic contents in microdissected midbrain and striatal areas revealed a reduction of dopamine at five and nine weeks of age. It is noteworthy that later on (at nine weeks), the morphological parameters remain altered but not worsened, whereas the phenotype progresses and behavioral deficits are more severe. The amount of fully activated Th (Serine40-phosphorylated isoform) in neurons that remain in the SNpc is mildly affected at 5 weeks but severely impaired by 9 weeks.[47] Finally, using a chronic and oral L-Dopa treatment on MeCP2-deficient mice, authors reported an amelioration of some of the motor deficits previously identified.[47] Altogether, these results argue for an alteration of the nigrostriatal dopaminergic pathway in MeCP2-deficient animals as a contributor of the neuromotor deficits.[47]
There is an association of Rett syndrome with brain-derived neurotrophic factor (BDNF).[48]
Molecular functions of MECP2 in Rett syndrome pathology
As reviewed by Sharifi and Yasui,[49] MECP2 protein, encoded by the MECP2 gene binds to DNA with a high affinity for CpG methylated DNA sites and affects transcription. MECP2 can bind to 5mc (5-methylcytosine) and 5hmc (5-hydroxymethylcytosine) with similar affinity, and these dinucleotides account for the majority of MECP2 binding sites in the mammalian genome. MECP2 is involved in higher order chromatin organization and appears necessary for compacting chromosomes. MECP2 binding to DNA influences mRNA splicing events. MECP2 also appears to function in DNA repair processes. MECP2-/+ deficient female mice have elevated rates of cell death when exposed to DNA damaging agents and are prone to early senescence.[49]
Interactive pathway map
An interactive pathway map of Rett syndrome has been published.[50]
Diagnosis

Prior to the discovery of a genetic cause, Rett syndrome had been designated as a pervasive developmental disorder by the Diagnostic and Statistical Manual of Mental Disorders (DSM), together with the autism spectrum disorders. Some argued against this conclusive assignment because RTT resembles non-autistic disorders such as fragile X syndrome, tuberous sclerosis, or Down syndrome that also exhibit autistic features.[51] After research proved the molecular mechanism, in 2013 the DSM-5 removed the syndrome altogether from classification as a mental disorder.[52]
Rett syndrome diagnosis involves close observation of the child's growth and development to observe any abnormalities in regards to developmental milestones.[53] A diagnosis is considered when decreased head growth is observed. Conditions with similar symptoms must first be ruled out.[53]
There are certain criteria that must be met for the diagnosis. A blood test can rule in or rule out the presence of the MECP2 mutation, however, this mutation is present in other conditions as well.[54]
For a classic diagnosis, all four criteria for ruling in a diagnosis must be met, as well as the two criteria for ruling out a diagnosis. Supportive criteria may also be present, but are not required for diagnosis. For an atypical or variant diagnosis, at least two of the four criteria for ruling in the diagnosis must be met, as well as five of the eleven supportive criteria. A period of symptom regression followed by recovery or symptom stabilization must also occur.[54] Children are often misdiagnosed as having autism, cerebral palsy, or another form of developmental delay. A positive test for the MECP2 mutation is not enough to make a diagnosis.[54]
Ruling in[54]
- Decreased or loss of use of fine motor skills
- Decreased or loss of verbal speech
- Abnormalities during gait
- Repetitive hand movements such as wringing/squeezing or clapping/tapping
Ruling out[54]
- Traumatic or anoxic/hypoxic brain injury, neurometabolic disease, or severe infection that may better explain symptoms
- Abnormal psychomotor development during the first six months of life
Supportive criteria[54]
- Breathing disturbances when awake
- Bruxism while awake
- Impaired sleep pattern
- Abnormal muscle tone
- Peripheral vasomotor disturbances
- Scoliosis/kyphosis
- Growth retardation
- Small cold hands and feet
- Inappropriate laughing/screaming spells
- Diminished response to pain
- Intense eye communication (eye pointing)
Differential diagnosis
Signs of Rett syndrome that are similar to autism:
- screaming fits
- inconsolable crying
- avoidance of eye contact
- lack of social/emotional reciprocity
- markedly impaired use of nonverbal behaviors to regulate social interaction
- loss of speech
- sensory problems
- sleep regression
Signs of Rett syndrome that are also present in cerebral palsy (regression of the type seen in Rett syndrome would be unusual in cerebral palsy; this confusion could rarely be made):
- possible short stature, sometimes with unusual body proportions because of difficulty walking or malnutrition caused by difficulty swallowing
- hypotonia
- delayed or absent ability to walk
- gait/movement difficulties
- ataxia
- microcephaly in some - abnormally small head, poor head growth
- gastrointestinal problems
- some forms of spasticity
- chorea - spasmodic movements of hand or facial muscles
- dystonia
- bruxism – grinding of teeth
Treatment
Currently there is no cure for Rett syndrome.[4] Treatment is directed towards improving function and addressing symptoms.[4] A multi-disciplinary team approach is typically used to treat the person throughout life. This team may include a primary care physician, physical therapist, occupational therapist, speech-language pathologist, nutritionist, and support services in academic and occupational settings. Some children may require special equipment and aids such as braces to arrest scoliosis, splints to modify hand movements, and nutritional programs to help them maintain adequate weight.[4]
Because of the increased risk of sudden cardiac death, when long QT syndrome is found on an annual screening EKG it is treated with an anti-arrhythmic such as a beta-blocker. There is some evidence that phenytoin may be more effective than a beta-blocker.[55]
While medicinal interventions to mitigate breathing challenges in children with Rett Syndrome (RTT) are still being developed,[56] children with RTT may be prescribed rebreathing techniques (e.g., rebreathing masks), oxygen delivery, or non-invasive ventilation as preventative or rescue breathing treatments.[57] High oxidative stress levels in individuals with RTT have exacerbated effects on their cardiorespiratory health and functionality,[56] dramatically increasing the risk for sudden cardiac death—an anomaly that has an associated 300x increased occurrence risk in children with Rett Syndrome.[58] Due to this, it is vital to closely monitor atypical breathing behaviors in children with RTT, making sure to effectively use lifesaving respiratory improvement devices and strategies as prescribed.[59]
Prescribed treatment methods may vary depending on the breathing characteristic phenotype expressed by the child. Physicians have identified three major RTT breathing phenotypes; forceful breathers, feeble breathers, and apneustic breathers.[60] For forceful breathers, for example, rebreathing masks may be used while the child is awake.[60]
In Dec 2021, Australian company Neuren Pharmaceuticals reported positive results in a phase 3 trial of trofinetide for the treatment of Rett syndrome.[61] In Sep 2022, the FDA accepted a new drug application for trofinetide and granted it priority review.[62] In March 2023 the drug received FDA approval for treatment of Rett Syndrome.[63]
Prognosis

Males with pathogenic MECP2 mutations usually die within the first 2 years from severe encephalopathy, unless they have one or more extra X chromosomes, or have somatic mosaicism.
Male fetuses with the disorder rarely survive to term. Because the disease-causing gene is located on the X chromosome, a female born with an MECP2 mutation on her X chromosome has another X chromosome with an ostensibly normal copy of the same gene, while a male with the mutation on his X chromosome has no other X chromosome, only a Y chromosome; thus, he has no normal gene. Without a normal gene to provide normal proteins in addition to the abnormal proteins caused by a MECP2 mutation, the XY karyotype male fetus is unable to slow the development of the disease, hence the failure of many male fetuses with a MECP2 mutation to survive to term.
Females with a MECP2 mutation, however, have a non-mutant chromosome that provides them enough normal protein to survive longer. Research shows that males with Rett syndrome may result from Klinefelter's syndrome, in which the male has an XXY karyotype.[64] Thus, a non-mutant MECP2 gene is necessary for a Rett's-affected embryo to survive in most cases, and the embryo, male or female, must have another X chromosome.
There have, however, been several cases of 46,XY karyotype males with a MECP2 mutation (associated with classical Rett syndrome in females) carried to term, who were affected by neonatal encephalopathy and died before 2 years of age.[65] The incidence of Rett syndrome in males is unknown, partly owing to the low survival of male fetuses with the Rett syndrome-associated MECP2 mutations, and partly to differences between signs caused by MECP2 mutations and those caused by Rett's.[65]
Females can live up to 40 years or more. Laboratory studies on Rett syndrome may show abnormalities such as:
- EEG abnormalities from 2 years of age
- atypical brain glycolipids
- elevated CSF levels of beta-endorphin and glutamate
- reduction of substance P
- decreased levels of CSF nerve growth factors
A high proportion of deaths are abrupt, but most have no identifiable cause; in some instances death is the result most likely of:
- spontaneous brainstem dysfunction
- cardiac arrest, likely due to long QT syndrome, ventricular tachycardia or other arrhythmias[66]
- seizures
- gastric perforation
History
Andreas Rett, a pediatrician in Vienna Austria, first described the condition in 1966.[4][67] As his writings were in German, they did not become widely known in the English-speaking world.[6] Bengt Hagberg, a Swedish pediatrician, published an English article in 1983 and named the condition after Rett.[6] In 1999, Lebanese-American physician Huda Zoghbi discovered the mutation that causes the condition.[6][7]
There are organizations that support this syndrome's awareness campaigns and fundraise to support treatment and research. For instance, the Noemie association hosts football (soccer) competitions for young girls with Rett syndrome. Thierry Breton, an osteopath at the Parisis clinic, is the organizer of this event, which takes place in Cormeilles-en-Paris.[68] Twelve teams will compete in this event. This soccer competition is held in support of the group La vie selon Noémi. Shirts from professional footballers Zlatan Ibrahimovic, Adrien Rabiot, Gianelli Imbula, Axel Ngando, and Karl Toko-Ekambi will be among the prizes given away. Two to three children with the syndrome will receive some of the treatment they need in a specialized facility in Barcelona, Spain with the money contributed. The organization was named after Noémie, who was born at the hospital in Cormeilles, Paris. The girl's parents founded this organization to aid her and other kids with multiple disabilities and to spread awareness of this condition.[69]
Research
Gene therapy is under study in animal models to achieve regulated expression of a normal MECP2 gene.[4] In March 2022, Taysha Gene Therapies announced that they had received Clinical Trial Application (CTA) approval from Health Canada for a clinical trial of their investigational gene therapy for adult females with Rett Syndrome.[70]
In fiction
In August 2021, a novel by British author Victoria Scott, Patience, was published by Head of Zeus.[71] The novel featured a character with Rett syndrome and explored recent developments in gene therapy.
See also
References
- Davis, Andrew S. (25 October 2010). [Rett syndrome Handbook of Pediatric Neuropsychology]. Springer Publishing Company. ISBN 978-0826157362. Archived from the original on 5 November 2017.
Rett initially called this syndrome cerebroaatrophic hyperammonemia, but the elevated ammonia levels in the bloodstream were later found to be only rarely associated with this condition (can Acker, Loncola, & Can Acker, 2005).
{{cite book}}: Check|url=value (help) - "MeSH Browser". meshb.nlm.nih.gov. Archived from the original on 4 December 2020. Retrieved 22 October 2019.
- "Rett syndrome". Genetics Home Reference. December 2013. Archived from the original on 14 October 2017. Retrieved 14 October 2017.
- "Rett Syndrome Fact Sheet". National Institute of Neurological Disorders and Stroke. Archived from the original on 14 October 2017. Retrieved 14 October 2017.
- "Rett Syndrome". NORD (National Organization for Rare Disorders). 2015. Archived from the original on 19 February 2017. Retrieved 14 October 2017.
- Percy, Alan (January 2014). "The American History of Rett Syndrome". Pediatric Neurology. 50 (1): 1–3. doi:10.1016/j.pediatrneurol.2013.08.018. PMC 3874243. PMID 24200039.
- Amir, Ruthie; Van den Veyver, Ignatia; Wan, Mimi; Tran, Charles; Francke, Uta; Zoghbi, Huda (1999). "Rett syndrome is caused by mutations in X-linked MECP2, encoding methyl-CpG-binding protein 2". Nature Genetics. 23 (2): 185–8. doi:10.1038/13810. PMID 10508514. S2CID 3350350.
- Neul, Jeffrey l.; Kaufmann, Walter E.; Glaze, Daniel G.; Christodoulou, John; Clarke, Angus J.; Bahi-Buisson, Nadia; Leonard, Helen; Bailey, Mark E. S.; Schanen, N. Carolyn; Zappella, Michele; Renieri, Alessandra; Huppke, Peter; Percy, Alan K.; et al. (Rettsearch Consortium) (2010). "Rett syndrome: Revised diagnostic criteria and nomenclature". Annals of Neurology. 68 (6): 944–50. doi:10.1002/ana.22124. PMC 3058521. PMID 21154482.
- Ariani, Francesca; Hayek, Giuseppe; Rondinella, Dalila; Artuso, Rosangela; Mencarelli, Maria Antonietta; Spanhol-Rosseto, Ariele; Pollazzon, Marzia; Buoni, Sabrina; Spiga, Ottavia; Ricciardi, Sara; Meloni, Ilaria; Longo, Ilaria; Mari, Francesca; Broccoli, Vania; Zappella, Michele; Renieri, Alessandra (11 July 2008). "FOXG1 is Responsible for the Congenital Variant of Rett Syndrome". The American Journal of Human Genetics. 83 (1): 89–93. doi:10.1016/j.ajhg.2008.05.015. PMC 2443837. PMID 18571142.
- Zappella, Michele (1992). "The rett girls with preserved speech". Brain and Development. 14 (2): 98–101. doi:10.1016/S0387-7604(12)80094-5. PMID 1621933. S2CID 4782923.
- Skjeldal, O. H.; Von Tetzchner, S.; Jacobsen, K.; Smith, L.; Heiberg, A. (2007). "Rett Syndrome - Distribution of Phenotypes with Special Attention to the Preserved Speech Variant". Neuropediatrics. 26 (2): 87. doi:10.1055/s-2007-979732. PMID 7566462.
- Sørensen, E.; Viken, B. (20 February 1995). "[Rett syndrome a developmental disorder. Presentation of a variant with preserved speech]". Tidsskrift for den Norske Laegeforening (in Norwegian). 115 (5): 588–590. ISSN 0029-2001. PMID 7900110.
- Zappella, M (1997). "The preserved speech variant of the Rett complex: A report of 8 cases". European Child & Adolescent Psychiatry. 6 Suppl 1: 23–5. PMID 9452915.
- Renieri, A.; Mari, F.; Mencarelli, M.A.; Scala, E.; Ariani, F.; Longo, I.; Meloni, I.; Cevenini, G.; Pini, G.; Hayek, G.; Zappella, M. (March 2009). "Diagnostic criteria for the Zappella variant of Rett syndrome (the preserved speech variant)". Brain and Development. 31 (3): 208–16. doi:10.1016/j.braindev.2008.04.007. PMID 18562141. S2CID 6223422.
- Buoni, Sabrina; Zannolli, Raffaella; De Felice, Claudio; De Nicola, Anna; Guerri, Vanessa; Guerra, Beatrice; Casali, Stefania; Pucci, Barbara; Corbini, Letizia; Mari, Francesca; Renieri, Alessandra; Zappella, Michele; Hayek, Joseph (May 2010). "EEG features and epilepsy in MECP2-mutated patients with the Zappella variant of Rett syndrome". Clinical Neurophysiology. 121 (5): 652–7. doi:10.1016/j.clinph.2010.01.003. PMID 20153689. S2CID 12976926.
- Huppke, Peter; Held, Melanie; Laccone, Franco; Hanefeld, Folker (2003). "The spectrum of phenotypes in females with Rett Syndrome". Brain and Development. 25 (5): 346–51. doi:10.1016/S0387-7604(03)00018-4. PMID 12850514. S2CID 9566219.
- Gillberg, d. (1997). "Communication in Rett syndrome complex". European Child & Adolescent Psychiatry. 6 Suppl 1: 21–2. PMID 9452914.
- Zappella, Michele; Gillberg, Christopher; Ehlers, Stephan (1998). "The preserved speech variant: A subgroup of the Rett complex: A clinical report of 30 cases". Journal of Autism and Developmental Disorders. 28 (6): 519–26. doi:10.1023/A:1026052128305. PMID 9932238. S2CID 22152062.
- Guy, J.; Gan, J.; Selfridge, J.; Cobb, S.; Bird, A. (2007). "Reversal of Neurological Defects in a Mouse Model of Rett Syndrome". Science. 315 (5815): 1143–7. Bibcode:2007Sci...315.1143G. doi:10.1126/science.1138389. PMC 7610836. PMID 17289941. S2CID 25172134.
- Trappe, R.; Laccone, F.; Cobilanschi, J.; Meins, M.; Huppke, P.; Hanefeld, F.; Engel, W. (2001). "MECP2 Mutations in Sporadic Cases of Rett Syndrome Are Almost Exclusively of Paternal Origin". The American Journal of Human Genetics. 68 (5): 1093–101. doi:10.1086/320109. PMC 1226090. PMID 11309679.
- Zoghbi, Huda Y.; Van Den Veyver, Ruthie E.; Wan, Ignatia B.; Tran, Mimi; Francke, Charles Q.; Zoghbi, Uta (1999). "Rett syndrome is caused by mutations in X-linked MECP2, encoding methyl-CpG-binding protein 2". Nature Genetics. 23 (2): 185–8. doi:10.1038/13810. PMID 10508514. S2CID 3350350.
- "Rett syndrome". Genetics Home Reference. Archived from the original on 27 July 2016. Retrieved 29 May 2016.
- Merwick, Aine; O'Brien, Margaret; Delanty, Norman (2012). "Complex single gene disorders and epilepsy". Epilepsia. 53 (s4): 81–91. doi:10.1111/j.1528-1167.2012.03617.x. ISSN 1528-1167. PMID 22946725. S2CID 37226510.
- Zoghbi, Huda Y.; Milstien, Sheldon; Butler, Ian J.; Smith, E. O'Brian; Kaufman, Seymour; Glaze, Daniel G.; Percy, Alan K. (1989). "Cerebrospinal fluid biogenic amines and biopterin in Rett syndrome". Annals of Neurology. 25 (1): 56–60. doi:10.1002/ana.410250109. PMID 2913929. S2CID 351243.
- Roux, Jean-Christophe; Villard, Laurent (2009). "Biogenic Amines in Rett Syndrome: The Usual Suspects". Behavior Genetics. 40 (1): 59–75. doi:10.1007/s10519-009-9303-y. PMID 19851857. S2CID 20352177.
- Hokfelt, T.; Martensson, R.; Bjorklund, A.; Kleinau, S.; Goldstein, M (1984). "Distribution maps of tyrosine-hydroxylase-immunoreactive neurons in the rat brain". In Bjorklund, A.; Hokfelt, T. (eds.). Handbook of Chemical Neuroanatomy. Classical Transmitters in the CNS, Part I. Vol. 2. New York: Elsevier. pp. 277–379.
- Berridge, Craig W; Waterhouse, Barry D (2003). "The locus coeruleus–noradrenergic system: Modulation of behavioral state and state-dependent cognitive processes". Brain Research Reviews. 42 (1): 33–84. doi:10.1016/S0165-0173(03)00143-7. PMID 12668290. S2CID 477754.
- Taneja, P.; Ogier, M.; Brooks-Harris, G.; Schmid, D. A.; Katz, D. M.; Nelson, S. B. (2009). "Pathophysiology of Locus Ceruleus Neurons in a Mouse Model of Rett Syndrome". Journal of Neuroscience. 29 (39): 12187–95. doi:10.1523/JNEUROSCI.3156-09.2009. PMC 2846656. PMID 19793977.
- Roux, Jean-Christophe; Panayotis, Nicolas; Dura, Emmanuelle; Villard, Laurent (2009). "Progressive noradrenergic deficits in the locus coeruleus of Mecp2 deficient mice". Journal of Neuroscience Research. 88 (7): 1500–9. doi:10.1002/jnr.22312. PMID 19998492. S2CID 3404695.
- Björklund, A.; Lindvall, O (1984). "Dopamine-containing systems in the CNS". In Björklund, A.; Hökfelt, T. (eds.). Handbook of Chemical Neuroanatomy. Classical Transmitters in the CNS, Part l. Vol. 2. New York: Elsevier. pp. 55–122.
- Hokfelt, T.; Martensson, R.; Björklund, A.; Kleinau, S.; Goldstein, M. (1984). "Distribution maps of tyrosine-hydroxylase-immunoreactive neurons in the rat brain". In Björklund, A.; Hökfelt, T. (eds.). Handbook of Chemical Neuroanatomy. Classical Transmitters in the CNS, Part I. Vol. 2. New York: Elsevier. pp. 277–379.
- Björklund, Anders; Dunnett, Stephen B. (2007). "Dopamine neuron systems in the brain: An update". Trends in Neurosciences. 30 (5): 194–202. doi:10.1016/j.tins.2007.03.006. PMID 17408759. S2CID 14239716.
- Parent, André; Hazrati, Lili-Naz (1995). "Functional anatomy of the basal ganglia. I. The cortico-basal ganglia-thalamo-cortical loop". Brain Research Reviews. 20 (1): 91–127. doi:10.1016/0165-0173(94)00007-C. PMID 7711769. S2CID 28252990.
- Gerfen, Charles R. (2000). "Molecular effects of dopamine on striatal-projection pathways". Trends in Neurosciences. 23 (10 Suppl): S64–70. doi:10.1016/S1471-1931(00)00019-7. PMID 11052222. S2CID 3965480.
- Lees, Andrew J; Hardy, John; Revesz, Tamas (2009). "Parkinson's disease". The Lancet. 373 (9680): 2055–66. doi:10.1016/S0140-6736(09)60492-X. PMID 19524782. S2CID 42608600.
- Dauer, William; Przedborski, Serge (2003). "Parkinson's Disease". Neuron. 39 (6): 889–909. doi:10.1016/S0896-6273(03)00568-3. PMID 12971891. S2CID 10400095.
- Jenner, Peter (2009). "Functional models of Parkinson's disease: A valuable tool in the development of novel therapies". Annals of Neurology. 64: S16–29. doi:10.1002/ana.21489. PMID 19127585. S2CID 26065287.
- Fitzgerald, Patricia M.; Jankovic, Joseph; Percy, Alan K. (1990). "Rett syndrome and associated movement disorders". Movement Disorders. 5 (3): 195–202. doi:10.1002/mds.870050303. PMID 2388636. S2CID 43376602.
- Neul, Jeffrey L.; Zoghbi, Huda Y. (2004). "Rett Syndrome: A Prototypical Neurodevelopmental Disorder". The Neuroscientist. 10 (2): 118–28. doi:10.1177/1073858403260995. PMID 15070486. S2CID 9617631.
- Segawa, Masaya (2005). "Early motor disturbances in Rett syndrome and its pathophysiological importance". Brain and Development. 27: S54–S58. doi:10.1016/j.braindev.2004.11.010. PMID 16182486. S2CID 30218744.
- Guy, Jacky; Hendrich, Brian; Holmes, Megan; Martin, Joanne E.; Bird, Adrian (2001). "A mouse Mecp2-null mutation causes neurological symptoms that mimic Rett syndrome". Nature Genetics. 27 (3): 322–6. doi:10.1038/85899. hdl:1842/727. PMID 11242117. S2CID 8698208.
- Chen, Richard Z.; Akbarian, Schahram; Tudor, Matthew; Jaenisch, Rudolf (2001). "Deficiency of methyl-CpG binding protein-2 in CNS neurons results in a Rett-like phenotype in mice". Nature Genetics. 27 (3): 327–31. doi:10.1038/85906. PMID 11242118. S2CID 24979562.
- Nan, X; Ng, H. H.; Johnson, C. A.; Laherty, C. D.; Turner, B. M.; Eisenman, R. N.; Bird, A (1998). "Transcriptional repression by the methyl-CpG-binding protein MeCP2 involves a histone deacetylase complex". Nature. 393 (6683): 386–9. Bibcode:1998Natur.393..386N. doi:10.1038/30764. PMID 9620804. S2CID 4427745.
- Cheval, H; Guy, J; Merusi, C; De Sousa, D; Selfridge, J; Bird, A (2012). "Postnatal inactivation reveals enhanced requirement for MeCP2 at distinct age windows". Human Molecular Genetics. 21 (17): 3806–14. doi:10.1093/hmg/dds208. PMC 3412380. PMID 22653753.

- Ricceri, Laura; De Filippis, Bianca; Laviola, Giovanni (2008). "Mouse models of Rett syndrome: From behavioural phenotyping to preclinical evaluation of new therapeutic approaches". Behavioural Pharmacology. 19 (5–6): 501–17. doi:10.1097/FBP.0b013e32830c3645. PMID 18690105. S2CID 33364486.
- Samaco, R. C.; Mandel-Brehm, C.; Chao, H.-T.; Ward, C. S.; Fyffe-Maricich, S. L.; Ren, J.; Hyland, K.; Thaller, C.; Maricich, S. M.; Humphreys, P.; Greer, J. J.; Percy, A.; Glaze, D. G.; Zoghbi, H. Y.; Neul, J. L. (2009). "Loss of MeCP2 in aminergic neurons causes cell-autonomous defects in neurotransmitter synthesis and specific behavioral abnormalities". Proceedings of the National Academy of Sciences. 106 (51): 21966–71. Bibcode:2009PNAS..10621966S. doi:10.1073/pnas.0912257106. JSTOR 40536204. PMC 2799790. PMID 20007372.
- Panayotis, Nicolas; Pratte, Michel; Borges-Correia, Ana; Ghata, Adeline; Villard, Laurent; Roux, Jean-Christophe (2011). "Morphological and functional alterations in the substantia nigra pars compacta of the Mecp2-null mouse". Neurobiology of Disease. 41 (2): 385–97. doi:10.1016/j.nbd.2010.10.006. PMID 20951208. S2CID 25414717.
- Sun, Yi E.; Wu, Hao (2006). "The Ups and Downs of BDNF in Rett Syndrome". Neuron. 49 (3): 321–3. doi:10.1016/j.neuron.2006.01.014. PMID 16446133.
- Sharifi, Osman; Yasui, Dag H. (2021). "The Molecular Functions of MeCP2 in Rett Syndrome Pathology". Frontiers in Genetics. 12: 624290. doi:10.3389/fgene.2021.624290. PMC 8102816. PMID 33968128.
- Ehrhart, Friederike; Coort, Susan L. M.; Cirillo, Elisa; Smeets, Eric; Evelo, Chris T.; Curfs, Leopold M. G. (25 November 2016). "Rett syndrome – biological pathways leading from MECP2 to disorder phenotypes". Orphanet Journal of Rare Diseases. 11 (1): 158. doi:10.1186/s13023-016-0545-5. PMC 5123333. PMID 27884167.
- Tsai, Luke Y. (1992). "Is Rett syndrome a subtype of pervasive developmental disorders?" (PDF). Journal of Autism and Developmental Disorders. 22 (4): 551–61. doi:10.1007/BF01046327. hdl:2027.42/44607. PMID 1483976. S2CID 17817425. Archived from the original on 29 August 2021. Retrieved 20 April 2018.
- Abbeduto, Leonard; Ozonoff, Susan; Thurman, Angela John; McDuffie, Angela; Schweitzer, Julie (18 March 2014). Hales, Robert; Yudofsky, Stuart; Robert, Laura Weiss (eds.). Chapter 8. Neurodevelopmental Disorders, The American Psychiatric Publishing Textbook of Psychiatry (6 ed.). Arlington, VA: American Psychiatric Publishing. doi:10.1176/appi.books.9781585625031.rh08. ISBN 978-1-58562-444-7. S2CID 241966275.
- "Rett syndrome Tests and diagnosis". Mayo Clinic. Archived from the original on 30 October 2017.
- "About Rett syndrome - Rett Syndrome Diagnosis". rettsyndrome.org. International Rett Syndrome Foundation. Archived from the original on 29 October 2017. Retrieved 10 May 2020.
- McCauley, Mark D.; Wang, Tiannan; Mike, Elise; Herrera, Jose; Beavers, David L.; Huang, Teng-Wei; Ward, Christopher S.; Skinner, Steven; Percy, Alan K. (14 December 2011). "Pathogenesis of Lethal Cardiac Arrhythmias in Mecp2 Mutant Mice: Implication for Therapy in Rett Syndrome". Science Translational Medicine. 3 (113): 113ra125. doi:10.1126/scitranslmed.3002982. ISSN 1946-6234. PMC 3633081. PMID 22174313.
- Mackay, Jessica; Downs, Jenny; Wong, Kingsley; Heyworth, Jane; Epstein, Amy; Leonard, Helen (2017). "Autonomic breathing abnormalities in Rett syndrome: caregiver perspectives in an international database study". Journal of Neurodevelopmental Disorders. 9: 15. doi:10.1186/s11689-017-9196-7. ISSN 1866-1947. PMC 5410057. PMID 28465761.
- Harish Kumar, S. (19 January 2017). "Cardio respiratory physiotherapy management in Rett's syndrome - Literature review". International Journal of Pharma and Bio Sciences: 5 – via ResearchGate.
- Kyle, Stephanie M.; Vashi, Neeti; Justice, Monica J. (February 2018). "Rett syndrome: a neurological disorder with metabolic components". Open Biology. 8 (2): 170216. doi:10.1098/rsob.170216. ISSN 2046-2441. PMC 5830535. PMID 29445033.
- De Felice, Claudio; Maffei, Silvia; Signorini, Cinzia; Leoncini, Silvia; Lunghetti, Stefano; Valacchi, Giuseppe; D'Esposito, Maurizio; Filosa, Stefania; Della Ragione, Floriana; Butera, Gianfranco; Favilli, Roberto (April 2012). "Subclinical myocardial dysfunction in Rett syndrome". European Heart Journal: Cardiovascular Imaging. 13 (4): 339–345. doi:10.1093/ejechocard/jer256. ISSN 2047-2412. PMID 22113206. Archived from the original on 29 November 2021. Retrieved 29 November 2021.
- Smeets, Eric E. J.; Julu, Peter O. O.; Waardenburg, Dick van; Engerström, Ingegerd Witt; Hansen, Stig; Apartopoulos, Flora; Curfs, Leopold M. G.; Schrander-Stumpel, Connie T. R. M. (1 November 2006). "Management of a severe forceful breather with Rett Syndrome using carbogen". Brain and Development. 28 (10): 625–632. doi:10.1016/j.braindev.2006.04.010. ISSN 0387-7604. PMID 16765005. S2CID 15545729. Archived from the original on 1 October 2022. Retrieved 29 November 2021.
- Positive top-line results from pivotal Phase 3 trial in Rett syndrome (PDF) (Report). Australian Stock Exchange. 7 December 2021.
- Rett Syndrome New Drug Application accepted for Priority Review by FDA (PDF) (Report). Australian Stock Exchange. 13 September 2022.
- "Breakthrough drug from Dame Margaret Brimble's lab". University of Auckland. 11 March 2023. Retrieved 6 May 2023.
- Schwartzman, J. S.; Bernardino, Andrea; Nishimura, Agnes; Gomes, Raquel R.; Zatz, Mayana (2001). "Rett Syndrome in a Boy with a 47,XXY Karyotype Confirmed by a Rare Mutation in the MECP2 Gene". Neuropediatrics. 32 (3): 162–4. doi:10.1055/s-2001-16620. PMID 11521215.
- Hardwick, Simon A; Reuter, Kirsten; Williamson, Sarah L; Vasudevan, Vidya; Donald, Jennifer; Slater, Katrina; Bennetts, Bruce; Bebbington, Ami; Leonard, Helen; Williams, Simon R; Smith, Robert L; Cloosterman, Desiree; Christodoulou, John (2007). "Delineation of large deletions of the MECP2 gene in Rett syndrome patients, including a familial case with a male proband". European Journal of Human Genetics. 15 (12): 1218–29. doi:10.1038/sj.ejhg.5201911. PMID 17712354.
- Acampa, M.; Guideri, F. (May 2006). "Cardiac disease and Rett syndrome". Archives of Disease in Childhood. 91 (5): 440–443. doi:10.1136/adc.2005.090290. ISSN 1468-2044. PMC 2082747. PMID 16632674.
- Rett, A. (10 September 1966). "[On an unusual brain atrophy syndrome in hyperammonemia in childhood]". Wiener Medizinische Wochenschrift (in German). 116 (37): 723–726. ISSN 0043-5341. PMID 5300597.
- "Cormeilles : Un tournoi de foot solidaire au profit de Noémie". 26 June 2015.
- "Association Noémi".
- "Taysha Gene Therapies Announces Initiation of Clinical Development of TSHA-102 in Rett Syndrome". Taysha Gene Therapies. March 2022. Archived from the original on 30 March 2022. Retrieved 6 May 2022.
- "title". Head of Zeus. Archived from the original on 1 October 2022. Retrieved 7 May 2022.