Mammoplasia
| Mammoplasia | |
|---|---|
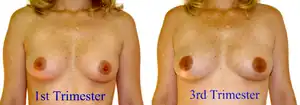 | |
| It is normal for the breasts to spontaneously enlarge during pregnancy. |
Mammoplasia is the normal or spontaneous enlargement of human breasts.[1] Mammoplasia occurs normally during puberty and pregnancy in women, as well as during certain periods of the menstrual cycle.[2][3][4] When it occurs in males, it is called gynecomastia and is considered to be pathological.[4] When it occurs in females and is extremely excessive, it is called macromastia (also known as gigantomastia or breast hypertrophy) and is similarly considered to be pathological.[5][6][7] Mammoplasia may be due to breast engorgement, which is temporary enlargement of the breasts caused by the production and storage of breast milk in association with lactation and/or galactorrhea (excessive or inappropriate production of milk).[8] Mastodynia (breast tenderness/pain) frequently co-occurs with mammoplasia.[9][10]
During the luteal phase (latter half) of the menstrual cycle, due to increased mammary blood flow and/or premenstrual fluid retention caused by high circulating concentrations of estrogen and/or progesterone, the breasts temporarily increase in size, and this is experienced by women as fullness, heaviness, swollenness, and a tingling sensation.[11][12]
Mammoplasia can be an effect or side effect of various drugs, including estrogens,[2][13] antiandrogens such as spironolactone,[14] cyproterone acetate,[15] bicalutamide,[16][17] and finasteride,[18][19] growth hormone,[20][21] and drugs that elevate prolactin levels such as D2 receptor antagonists like antipsychotics (e.g., risperidone), metoclopramide, and domperidone[22][23] and certain antidepressants like selective serotonin reuptake inhibitors (SSRIs) and tricyclic antidepressants (TCAs).[23][24][25] The risk appears to be less with serotonin-norepinephrine reuptake inhibitors (SNRIs) like venlafaxine.[26] The "atypical" antidepressants mirtazapine and bupropion do not increase prolactin levels (bupropion may actually decrease prolactin levels), and hence there may be no risk with these agents.[22] Other drugs that have been associated with mammoplasia include D-penicillamine, bucillamine, neothetazone, ciclosporin, indinavir, marijuana, and cimetidine.[6][27]
A 1997 study found an association between the SSRIs and mammoplasia in 23 (39%) of its 59 female participants.[26] Studies have also found associations between SSRIs and galactorrhea.[24][28][29][30] These side effects seem to be due to hyperprolactinemia (elevated prolactin levels) induced by these drugs, an effect that appears to be caused by serotonin-mediated inhibition of tuberoinfundibular dopaminergic neurons that inhibit prolactin secretion.[26][28][29] The mammoplasia these drugs can cause has been found to be highly correlated with concomitant weight gain (in the 1997 study, 83% of those who experienced weight gain also experienced mammoplasia, while only 30% of those who did not experience weight gain experienced mammoplasia).[26] The mammoplasia associated with SSRIs is reported to be reversible with drug discontinuation.[30] SSRIs have notably been associated with a modestly increased risk of breast cancer.[31] This is in accordance with higher prolactin levels being associated with increased breast cancer risk.[32][33]
In puberty induction in hypogonadal girls and in feminizing hormone therapy in transgender women, as well as hormonal breast enhancement in women with breast hypoplasia or small breasts, mammoplasia is a desired effect.[34][35][36][37]
See also
References
- ↑ Nathanson, Ira T. (1946). "Present Concepts of Benign Breast Disease". New England Journal of Medicine. 235 (15): 548–553. doi:10.1056/NEJM194610102351505. ISSN 0028-4793.
- 1 2 Ismail Jatoi; Manfred Kaufmann (11 February 2010). Management of Breast Diseases. Springer Science & Business Media. pp. 21–. ISBN 978-3-540-69743-5.
- ↑ Nagrath Arun; Malhotra Narendra; Seth Shikha (15 December 2012). Progress in Obstetrics and Gynecology--3. Jaypee Brothers Medical Publishers Pvt. Ltd. pp. 393–394. ISBN 978-93-5090-575-3.
- 1 2 Ora Hirsch Pescovitz; Erica A. Eugster (2004). Pediatric Endocrinology: Mechanisms, Manifestations, and Management. Lippincott Williams & Wilkins. pp. 349–. ISBN 978-0-7817-4059-3.
- ↑ Arnold G. Coran; Anthony Caldamone; N. Scott Adzick; Thomas M. Krummel; Jean-Martin Laberge; Robert Shamberger (25 January 2012). Pediatric Surgery. Elsevier Health Sciences. pp. 773–. ISBN 978-0-323-09161-9.
- 1 2 David J. Dabbs (2012). Breast Pathology. Elsevier Health Sciences. pp. 19–. ISBN 978-1-4377-0604-8.
- ↑ J.P. Lavery; J.S. Sanfilippo (6 December 2012). Pediatric and Adolescent Obstetrics and Gynecology. Springer Science & Business Media. pp. 99–. ISBN 978-1-4612-5064-7.
- ↑ G. P. TALWAR; L .M. SRIVASTAVA (1 January 2002). TEXTBOOK OF BIOCHEMISTRY AND HUMAN BIOLOGY. PHI Learning Pvt. Ltd. pp. 959–. ISBN 978-81-203-1965-3.
- ↑ Christoph Zink (1 January 1988). Dictionary of Obstetrics and Gynecology. Walter de Gruyter. pp. 152–. ISBN 978-3-11-085727-6.
- ↑ Michael Heinrich Seegenschmiedt; Hans-Bruno Makoski; Klaus-Rüdiger Trott; Luther W. Brady, eds. (15 April 2009). Radiotherapy for Non-Malignant Disorders. Springer Science & Business Media. pp. 719–. ISBN 978-3-540-68943-0.
- ↑ Ruth A. Lawrence; Robert M. Lawrence (26 October 2015). Breastfeeding: A Guide for the Medical Profession. Elsevier Health Sciences. p. 60. ISBN 978-0-323-35776-0.
The cyclic changes of the adult mammary gland can be associated with the menstrual cycle and the hormonal changes that control that cycle. Estrogens stimulate parenchymal proliferation, with formulation of epithelial sprouts. This hyperplasia continues into the secretory phase of the cycle. Anatomically, when the corpus luteum provides increased amounts of estrogen and progesterone, there is lobular edema, thickening of the epithelial basal membrane, and secretory material in the alveolar lumen. Lymphoid and plasma cells infiltrate the stroma. Clinically, mammary blood flow increases in this luteal phase. This increased flow is experienced by women as fullness, heaviness, and turgescence. The breast may become nodular because of interlobular edema and ductular-acinar growth.
- ↑ Milligan D, Drife JO, Short RV (1975). "Changes in breast volume during normal menstrual cycle and after oral contraceptives". Br Med J. 4 (5995): 494–6. doi:10.1136/bmj.4.5995.494. PMC 1675650. PMID 1192144.
[M]any women report breast changes during the normal menstrual cycle, with a feeling of fullness and a tingling sensation immediately before menstruation.1 Women taking oral contraceptives also seem to experience similar breast symptoms.2 It has been claimed that there are also pronounced changes in breast volume during the normal menstrual cycle, with maximum values occurring in the week before menstruation.3
- ↑ Robert Alan Lewis (23 March 1998). Lewis' Dictionary of Toxicology. CRC Press. pp. 470–. ISBN 978-1-56670-223-2.
- ↑ Jeffrey K. Aronson (2 March 2009). Meyler's Side Effects of Cardiovascular Drugs. Elsevier. pp. 255–. ISBN 978-0-08-093289-7.
- ↑ Elizabeth Martin (28 May 2015). Concise Medical Dictionary. Oxford University Press. pp. 189–. ISBN 978-0-19-968781-7.
- ↑ Patrick C. Walsh; Janet Farrar Worthington (31 August 2010). Dr. Patrick Walsh's Guide to Surviving Prostate Cancer, Second Edition. Grand Central Publishing. pp. 258–. ISBN 978-1-4555-0016-1.
- ↑ Harvey B. Simon (3 February 2004). The Harvard Medical School Guide to Men's Health: Lessons from the Harvard Men's Health Studies. Simon and Schuster. pp. 403–. ISBN 978-0-684-87182-0.
- ↑ Jeffrey K. Aronson (21 February 2009). Meyler's Side Effects of Endocrine and Metabolic Drugs. Elsevier. pp. 155–. ISBN 978-0-08-093292-7.
- ↑ Jacqueline Burchum; Laura Rosenthal (2 December 2014). Lehne's Pharmacology for Nursing Care. Elsevier Health Sciences. pp. 802–. ISBN 978-0-323-34026-7.
- ↑ Sat Dharam Kaur (2003). The Complete Natural Medicine Guide to Breast Cancer: A Practical Manual for Understanding, Prevention & Care. R. Rose. p. 79. ISBN 978-0-7788-0083-5.
- ↑ Souza, Flavio Moutinho; Collett-Solberg, Paulo Ferrez (2011). "Adverse effects of growth hormone replacement therapy in children". Arquivos Brasileiros de Endocrinologia & Metabologia. 55 (8): 559–565. doi:10.1590/S0004-27302011000800009. ISSN 0004-2730.
- 1 2 Torre DL, Falorni A (2007). "Pharmacological causes of hyperprolactinemia". Ther Clin Risk Manag. 3 (5): 929–51. PMC 2376090. PMID 18473017.
- 1 2 Madhusoodanan, Subramoniam; Parida, Suprit; Jimenez, Carolina (2010). "Hyperprolactinemia associated with psychotropics-a review". Human Psychopharmacology: Clinical and Experimental. 25 (4): 281–297. doi:10.1002/hup.1116. ISSN 0885-6222. PMID 20521318.
- 1 2 Jeffrey A. Lieberman; Allan Tasman (16 May 2006). Handbook of Psychiatric Drugs. John Wiley & Sons. pp. 75–. ISBN 978-0-470-02821-6.
- ↑ Kaufman, K. R.; Podolsky, D.; Greenman, D.; Madraswala, R. (2013). "Antidepressant-Selective Gynecomastia". Annals of Pharmacotherapy. 47 (1): e6. doi:10.1345/aph.1R491. ISSN 1060-0280. PMID 23324513.
- 1 2 3 4 Amsterdam JD, Garcia-España F, Goodman D, Hooper M, Hornig-Rohan M (1997). "Breast enlargement during chronic antidepressant therapy". J Affect Disord. 46 (2): 151–6. doi:10.1016/s0165-0327(97)00086-4. PMID 9479619.
- ↑ Dancey, Anne; Khan, M.; Dawson, J.; Peart, F. (2008). "Gigantomastia – a classification and review of the literature". Journal of Plastic, Reconstructive & Aesthetic Surgery. 61 (5): 493–502. doi:10.1016/j.bjps.2007.10.041. ISSN 1748-6815. PMID 18054304.
- 1 2 Coker F, Taylor D (2010). "Antidepressant-induced hyperprolactinaemia: incidence, mechanisms and management". CNS Drugs. 24 (7): 563–74. doi:10.2165/11533140-000000000-00000. PMID 20527996.
- 1 2 Mondal, S.; Saha, I.; Das, S.; Ganguly, A.; Das, D.; Tripathi, S. K. (2013). "A new logical insight and putative mechanism behind fluoxetine-induced amenorrhea, hyperprolactinemia and galactorrhea in a case series". Therapeutic Advances in Psychopharmacology. 3 (6): 322–334. doi:10.1177/2045125313490305. ISSN 2045-1253. PMC 3840809. PMID 24294485.
- 1 2 Benjamin Sadock (26 November 2013). Kaplan & Sadock's Pocket Handbook of Psychiatric Drug Treatment. Lippincott Williams & Wilkins. pp. 312–. ISBN 978-1-4698-5538-7.
- ↑ Boursi B, Lurie I, Mamtani R, Haynes K, Yang YX (2015). "Anti-depressant therapy and cancer risk: A nested case-control study". Eur Neuropsychopharmacol. 25 (8): 1147–57. doi:10.1016/j.euroneuro.2015.04.010. PMID 25934397.
- ↑ Hankinson, S. E.; Willett, W. C.; Michaud, D. S.; Manson, J. E.; Colditz, G. A.; Longcope, C.; Rosner, B.; Speizer, F. E. (1999). "Plasma Prolactin Levels and Subsequent Risk of Breast Cancer in Postmenopausal Women". JNCI Journal of the National Cancer Institute. 91 (7): 629–634. doi:10.1093/jnci/91.7.629. ISSN 0027-8874. PMID 10203283.
- ↑ Tworoger, S. S. (2004). "Plasma Prolactin Concentrations and Risk of Postmenopausal Breast Cancer". Cancer Research. 64 (18): 6814–6819. doi:10.1158/0008-5472.CAN-04-1870. ISSN 0008-5472. PMID 15375001.
- ↑ de Muinck Keizer-Schrama SM (2007). "Introduction and management of puberty in girls". Horm. Res. 68 Suppl 5 (5): 80–3. doi:10.1159/000110584. PMID 18174716.
- ↑ Gunther Göretzlehner; Christian Lauritzen; Thomas Römer; Winfried Rossmanith (1 January 2012). Praktische Hormontherapie in der Gynäkologie. Walter de Gruyter. pp. 385–. ISBN 978-3-11-024568-4.
- ↑ R.E. Mansel; Oystein Fodstad; Wen G. Jiang (14 June 2007). Metastasis of Breast Cancer. Springer Science & Business Media. pp. 217–. ISBN 978-1-4020-5866-0.
- ↑ Hartmann BW, Laml T, Kirchengast S, Albrecht AE, Huber JC (1998). "Hormonal breast augmentation: prognostic relevance of insulin-like growth factor-I". Gynecol. Endocrinol. 12 (2): 123–7. doi:10.3109/09513599809024960. PMID 9610425.