Tinea imbricata
| Tinea imbricata | |
|---|---|
| Other names: Tokelau[1] | |
 | |
| Tinea imbricata | |
| Specialty | Infectious diseases |
| Symptoms | Many red-brown, scaly, itchy small bumps, which spread to make overlapping rings resembling tiles on a roof[1][2] |
| Usual onset | Chidlhood[1] |
| Causes | Trichophyton concentricum[1] |
| Risk factors | Genetic predisposition[3] poor hygiene,[2] living in southwest Polynesia, Melanesia, Southeast Asia, India, and Central America.[1] |
| Treatment | Antifungals[1] |
| Medication | Terbinafine[1] |
Tinea imbricata is a superficial fungal infection of the skin.[1] It typically appears as several itchy red-brown and scaly small bumps, that spread to make overlapping rings and plaques.[1][2] Eventually it resembles tiles on a roof, lace or scales of fish.[1][2] The itch and discomfort may be worse in HIV.[4]
It is caused by Trichophyton concentricum.[1] There is possibly a genetic predisposition.[3] It occurs in areas of poor hygiene.[5]
The pattern of the rash gives away the diagnosis.[2] Microscopy of skin scrapings may be required.[2] Treatment is preferably with terbinafine.[1] Griseofulvin is another option.[1] Whitfield's cream might help remove scale.[5]
The condition is limited to southwest Polynesia, Melanesia, Southeast Asia, India, and Central America.[1] The name is derived from the Latin for "tiled" (imbricata) since the lesions are often lamellar.[6] It is rare in developed countries.[2]
The condition was first reported in 1686 by William Dampier, the English explorer in the Philippines.[5] It is known in Malay as Kaskado.[7]
Signs and symptoms
Tinea imbricata appears as several red-brown, scaly, itchy small bumps, which spread to make overlapping rings and plaques eventually resembling tiles on a roof, lace or scales of fish.[1][2]
_in_ver_gevorderde_staat_TMnr_10006761.jpg.webp) Tinea imbricata
Tinea imbricata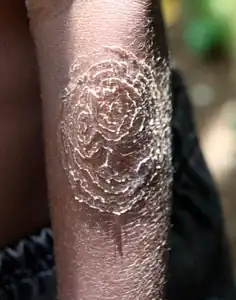
Cause and mechanism
The risk of developing tinea imbricata is probably inherited as an autosomal recessive trait.[8][9]
Tinea pseudoimbricata
The term "tinea pseudoimbricata" synonymuos with "tinea indecisiva", was coined to describe a form of tinea mimicking the concentric rings of tinea imbricata, but is caused by local or systemic immunosuppression.[10] Since then, 3 cases of Trichophyton tonsurans have been associated with it,[11] as well as Trichophyton rubrum which can trigger mycosis fungoides.[12][13] Mixed infections with scabies have been described to produce tinea pseudoimbricata.[14][15]
As of 2015 in India, corticosteroid–antifungal–antibacterial combinations sold as over-the-counter drug have led to an increase in chronic, recurrent, difficult to treat fungal infections of the skin, including tinea pseudoimbricata.[16]
See also
References
- 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 James, William D.; Elston, Dirk; Treat, James R.; Rosenbach, Misha A.; Neuhaus, Isaac (2020). "15. Diseases resulting from fungi and yeasts". Andrews' Diseases of the Skin: Clinical Dermatology (13th ed.). Elsevier. p. 296. ISBN 978-0-323-54753-6. Archived from the original on 2023-04-19. Retrieved 2023-04-19.
- 1 2 3 4 5 6 7 8 Leung, Alexander K. C.; Leong, Kin F.; Lam, Joseph M. (2019). "Tinea Imbricata: An Overview". Current Pediatric Reviews. 15 (3): 170–174. doi:10.2174/1573396315666190207151941. ISSN 1875-6336. PMID 30734680. Archived from the original on 2021-08-29. Retrieved 2021-10-06.
- 1 2 "Tinea corporis". dermnetnz.org. Archived from the original on 27 September 2021. Retrieved 6 October 2021.
- ↑ "Tinea Corporis Clinical Presentation: History, Physical Examination". emedicine.medscape.com. Archived from the original on 20 September 2017. Retrieved 6 October 2021.
- 1 2 3 Abdulazeem, Al-Bassam Rana; Salem, Al Afari Basmah; Saad, Alsharif Sadeem; Mohamed, Salem Manal Hassan (2019). "A systematic review of diagnosis and treatment options options or tinea imbricata". International Journal of pharma and Bio Sciences. doi:10.22376/ijpbs/lpr.2019.9.4.l28-33. Archived from the original on 2021-10-09. Retrieved 2021-10-06.
- ↑ Bonifaz A, Archer-Dubon C, Saúl A (July 2004). "Tinea imbricata or Tokelau". International Journal of Dermatology. 43 (7): 506–10. doi:10.1111/j.1365-4632.2004.02171.x. PMID 15230889. S2CID 45272404.
- ↑ Henley, David (2005). Fertility, Food and Fever: Population, Economy and Environment in North and Central Sulawesi, 1600-1930. Leiden: KITLV Press. p. 259. ISBN 90-6718-209-5. Archived from the original on 2021-10-09. Retrieved 2021-10-06.
- ↑ Serjeantson S, Lawrence G (January 1977). "Autosomal recessive inheritance of susceptibility to tinea imbricata". Lancet. 1 (8001): 13–5. doi:10.1016/s0140-6736(77)91653-1. PMID 63655. S2CID 27447510.
- ↑ Ravine D, Turner KJ, Alpers MP (October 1980). "Genetic inheritance of susceptibility to tinea imbricata". Journal of Medical Genetics. 17 (5): 342–8. doi:10.1136/jmg.17.5.342. PMC 1048596. PMID 7218274.
- ↑ Lim S. P. R., Smith A. G. (2003). "Tinea corporis in a renal transplant recipient mimicking the concentric rings of tinea imbricata". Clinical and Experimental Dermatology. 28 (3): 332–3. doi:10.1046/j.1365-2230.2003.01281.x. PMID 12780732. S2CID 30983522.
- ↑ Ouchi T1, Nagao K, Hata Y, Otuka T, Inazumi T. Trichophyton tonsurans infection manifesting as multiple concentric annular erythemas. J Dermatol. 2005 Jul;32(7):565-8.
- ↑ Poonawalla T, Chen W, Duvic M (2006). "Mycosis fungoides with tinea pseudoimbricata owing to Trichophyton rubrum infection". J Cutan Med Surg. 10 (1): 52–6. doi:10.1007/7140.2006.00007. PMID 17241575. S2CID 208341303.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Verma S, Hay RJ (2015). "Topical steroid-induced tinea pseudoimbricata: a striking form of tinea incognito". Int J Dermatol. 54 (5): e192–3. doi:10.1111/ijd.12734. PMID 25601089. S2CID 31276542.
- ↑ Poziomczyk CS, Köche B, Becker FL, Dornelles SI, Bonamigo RR. Tinea pseudoimbricata caused by M. gypseum associated to crusted scabies.An Bras Dermatol. 2010 Jul-Aug;85(4):558-9.[English, Portuguese]
- ↑ Verma S (2017). "Tinea pseudoimbricata". Indian Journal of Dermatology, Venereology and Leprology. 83 (3): 344–345. doi:10.4103/0378-6323.187686. PMID 27506504.
- ↑ Bishnoi Anuradha; et al. (2018). "Emergence of recalcitrant dermatophytosis in India". The Lancet Infectious Diseases. 18 (3): 250–251. doi:10.1016/S1473-3099(18)30079-3. PMID 29485088.
External links
| Classification |
|---|