Causes of mental disorders
A mental disorder is an impairment of the mind disrupting normal thinking, feeling, mood, behavior, or social interactions, and accompanied by significant distress or dysfunction.[1][2][3][4] The causes of mental disorders are very complex and vary depending on the particular disorder and the individual. Although the causes of most mental disorders are not fully understood, researchers have identified a variety of biological, psychological, and environmental factors that can contribute to the development or progression of mental disorders.[5] Most mental disorders result in a combination of several different factors rather than just a single factor.[6]
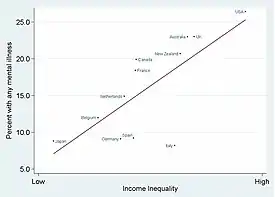
Research results
Risk factors for mental illness include psychological trauma, adverse childhood experiences, genetic predisposition, and personality traits. Correlations of mental disorders with drug use include almost all psychoactive substances, e.g., cannabis, alcohol, and caffeine.
Mental illnesses have risk factors, for instance including unequal parental treatment, adverse life events and drug use in depression, migration and discrimination, childhood trauma, loss or separation in families, and cannabis use in schizophrenia and psychosis, and parenting factors, child abuse, family history (e.g. of anxiety), and temperament and attitudes (e.g. pessimism) in anxiety. Many psychiatric disorders include problems with impulse and other emotional control.
In February 2013, a study found genetic links between five major psychiatric disorders: autism, ADHD, bipolar disorder, major depressive disorder, and schizophrenia. Abnormal functioning of neurotransmitter systems is also responsible for some mental disorders, including serotonin, norepinephrine, dopamine, and glutamate system's abnormal functioning. Differences have also been found in the size or activity of specific brain regions in some cases. Psychological mechanisms have also been implicated, such as cognitive (e.g. reasoning) biases, emotional influences, personality dynamics, temperament, and coping style. Studies have indicated[7] that variation in genes can play an important role in the evolution of mental disorders, although the reliable identification of connections between specific genes and specific disorders has proven more difficult. Environmental events surrounding pregnancy (such as maternal hypertension,[8] preeclampsia, or infection) and birth have also been implicated.[9] Traumatic brain injury may increase the risk of developing certain mental disorders. Throughout the years, there have been inconsistent links found to certain viral infections, substance misuse, and general physical health that have been false.
Adverse experiences affect a person's mental health, including abuse, neglect, bullying, social stress, traumatic events, and other overwhelming life experiences. The specific risks and pathways to particular disorders are less clear, however. Aspects of the wider community have also been implicated, including employment problems, socioeconomic inequality, lack of social cohesion, problems linked to migration, and features of particular societies and cultures. Mental stress is a common cause of mental illnesses, so finding a coping solution to cope with mental stress would be beneficial. Many solutions that have helped reduce stress are yoga, exercise, and some medications that may help.
Theories
General theories
Several theories or models seek to explain the causes (etiology) of mental disorders. These theories may differ in regards to how they explain the cause of the disorder, how to treat the disorder, and how they classify mental disorders. Theories also differ about the philosophy of mind they accept; that is, whether the mind and brain are identical or not.
During most of the 20th century, mental illness was ascribable to problematic relationships between children and their parents. This view was held well into the late 1990s, in which people still believed this child-parent relationship was a large determinant of severe mental illness, such as depression and schizophrenia. In the 21st century, additional factors have been identified such as genetic contributions, though experience also plays a role. So, the perceived causes of mental illness have changed over time and will most likely continue to alter while more research develops throughout the years.
Outside the West, community approaches remain a focus.
A practical mixture of models will explain particular issues and disorders, although there may be difficulty defining boundaries for indistinct psychiatric syndromes.
Medical or biomedical model
An overall distinction is also commonly made between a "medical model" (also known as a biomedical or disease model) and a "social model" (also known as an empowerment or recovery model) of mental disorder and disability, with the former focusing on hypothesized disease processes and symptoms, along with latter focusing on hypothesized social constructionism and social contexts.
Biological psychiatry has tended to follow a biomedical model focused on organic or "hardware" pathology of the brain,[10] where many mental disorders are conceptualized as disorders of brain circuits shaped by a complex interplay of genetics and experience.[11]
The social and medical models of mental disorders each work to identify and study distinct aspects, solutions, and potential therapies of disorders. The intersection and cross reference between the two models can further be used to develop more holistic models of mental disorders. Many criticisms historically of each model is the exclusivity of the other perspective. Therefore, intersectional research improved the impact and importance of future findings.[12]
Biopsychosocial model
The primary model of contemporary mainstream Western psychiatry is the biopsychosocial model (BPS), which integrates biological, psychological, and social factors.[10]
A related view, the diathesis-stress model, posits that mental disorders result from genetic dispositions and environmental stressors, combining to cause patterns of distress or dysfunction.[13]
Psychoanalytic theories
Psychoanalytic theories focus on unresolved internal and relational conflicts. These theories have been predicated as explanations of mental disorders. Many psychoanalytic groups are said to adhere to the biopsychosocial model and to accept an eclectic mix of subtypes of psychoanalysis. Sigmund Freud developed the psychoanalytic theory. This theory focuses on the impact of unconscious forces on human behavior. According to Freud, a personality has three parts: the id, ego, and superego. The id operates under the pleasure principle, the ego operates under the reality principle, and the superego is the "conscience" and incorporates what is and is not socially acceptable into a person's value system.[14] According to the psychoanalytic theory, there are five stages of psychosexual development that everyone goes through the oral stage, anal stage, phallic stage, latency stage, and genital stage. Mental disorders can be caused by an individual receiving too little or too much gratification in one of the psychosexual developmental stages. When this happens, the individual is said to be in that developmental stage.[15]
Attachment theory
Attachment theory is a kind of evolutionary-psychological approach sometimes applied in the context of mental disorders, which focuses on the role of early caregiver-child relationships, responses to danger, and the search for a satisfying reproductive relationship in adulthood. According to this theory, a child's attachment is to a nurturing adult, the more likely that child will maintain healthy relationships with others in their life.[16] As found by the Strange Situation experiment run by Mary Ainsworth based on the formulations of John Bowlby, there are four patterns of attachment: secure attachment, avoidant attachment, disorganized attachment, and ambivalent attachment.[17] Later research found the fourth pattern of attachment is known as disorganized disoriented attachment.[18] Secure attachments reflect trust in the child-caretaker relationship while insecure attachment reflects mistrust. The security of attachment in a child affects the child's emotional, cognitive, and social competence later in life.[17]
Evolutionary psychology
Evolutionary psychology and evolutionary psychiatry posit that mental disorders involve the dysfunctional operation of mental modules adapted to ancestral physical or social environments but not necessarily to modern ones. Behavioral abnormalities that resemble human mental illness have been found in related species (great apes).
Other theories suggest that mental illness could have evolutionary advantages for the species, including enhancing creativity and stress to enhance survival by activating the flight-or-fight response in anticipation of danger.
Schizophrenia could have been beneficial in prehistoric times by improving creativity during stressful times, or by helping to disseminate delusional tales that would have aided in-group cohesion and finding gullible mates. The paranoia associated with Schizophrenia could have prevented danger from other humans and other animals.
Mania and depression could have benefited from seasonal changes by helping to increase energy levels during times of plenty and rejuvenating energy during times of scarcity. In this way, mania was set in motion during the spring and summer to facilitate energy for hunting; depression worked best during the winter, similar to how bears hibernate to recover their energy levels. This may explain the connection between circadian genes and Bipolar Disorder and explain the relationship between light and seasonal affective disorder.
Biological factors
Biological factors consist of anything physical that can cause adverse effects on a person's mental health. Biological factors include genetics, prenatal damage, infections, exposure to toxins, brain defects or injuries, and substance abuse. Many professionals believe that the cause of mental disorders is the biology of the brain and the nervous system.
Mind mentions genetic factors, long-term physical health conditions, and head injuries or epilepsy (affecting behavior and mood) as factors that may trigger an episode of mental illness.
Genetics
Some rare mental disorders are caused only by genetics such as Huntington's disease.
Family linkage and some twin studies have indicated that genetic factors often play a role in the heritability of mental disorders. The reliable identification of specific genetic variation can cause indication of higher risk to particular disorders, through linkage, Genome Wide Association Scores[19] or association studies, has proven difficult. This is due to the complexity of interactions between genes, environmental events, and early development or the need for new research strategies. No specific gene results in a complex trait disorder, but specific variations of alleles result in higher risk for a trait. The heritability of behavioral traits associated with a mental disorder may be in permissive than in restrictive environments, and susceptibility genes probably work through both "within-the-skin" (physiological) pathways and "outside-the-skin" (behavioral and social) pathways. Investigations increasingly focus on links between genes and endophenotypes because they are more specific traits. Some include neurophysiological, biochemical, endocrinological, neuroanatomical, cognitive, or neuropsychological, rather than disease categories. Concerning a well-known mental disorder, schizophrenia, it is said with certainty that alleles (forms of genes) were responsible for this disorder. Some research has indicated only multiple, rare mutations are thought to alter neurodevelopmental pathways that can ultimately contribute to schizophrenia; virtually every rare structural mutation was different in each individual.
Research has shown that many conditions are polygenic meaning there are multiple defective genes rather than only one that is responsible for a disorder, and these genes may also be pleiotropic meaning that they cause multiple disorders, not just one.[20] Schizophrenia and Alzheimer's are both examples of hereditary mental disorders. When exonic genes encode for proteins, these proteins do not just affect one trait. The pathways that contribute to complex traits and phenotypes interact with multiple systems, even though proteins have specific functions.[21] brain plasticity (neuroplasticity) raises questions of whether some brain differences may be caused by mental illnesses or by pre-existing and then causing them.
Prenatal damage
Any damage that occurs to a fetus while still in its mother's womb is considered prenatal damage. Mental disorders can develop if the pregnant mother uses drugs or alcohol or is exposed to illnesses or infections during pregnancy. According to research, autism results from a disruption of early fetal brain progression.
Environmental events surrounding pregnancy and birth have increased the development of mental illness in the offspring. Some events may include maternal exposure to stress or trauma, conditions of famine, obstetric birth complications, infections, and gestational exposure to alcohol or cocaine. These factors have been hypothesized to affect areas of neurodevelopment, general development, and restrict neuroplasticity.
Infection, disease and toxins
There have been some findings of links between infection by the parasite Toxoplasma gondii and schizophrenia.[22]
AIDS has been linked to some mental disorders. Research shows that infections and exposure to toxins such as HIV[23] and streptococcus cause dementia.[24] This HIV infection that makes its way to the brain is called encephalopathy which spreads itself through the brain leading to dementia.[23] The infections or toxins that trigger a change in the brain chemistry can develop into a mental disorder.
Depression and emotional liability may be also be caused by babesiosis.
There is some evidence that there may be a relationship between BoDV-1 infection and psychiatric disease.
The research on Lyme disease caused by a deer tick and toxins is expanding the link between bacterial infections and mental illness.[25]
Injury and brain defects
Any damage to the brain can cause a mental disorder. The brain is the control system for the nervous system and the rest of the body. Without it, the body cannot function properly.
Increased mood swings, insane behavior, and substance abuse disorders are traumatic brain injury (TBI) examples. Findings on the relationship between TBI severity and prevalence of subsequent psychiatric disorders have been inconsistent, and occurrence relates to prior mental health problems. Direct neurophysiological effects in a complex interaction with personality, attitude, and social influences.
Head trauma classifies as either open or closed head injury. In open head injury, the skull is punctured and the brain tissue is demolished. Closed head injury is more common, the skull is not punctured because there is an impact of the brain against the skull that creates permanent structural damage (subdural hematoma). With both types, symptoms may disappear or persist over time. Typically the longer the length of time spent unconscious and the length of post-traumatic amnesia the worse the prognosis for the individual. The cognitive residual symptoms of head trauma are associated with the type of injury (either an open head injury or closed head injury) and the amount of tissue destroyed. Closed injury head trauma symptoms include; Deficits in abstract reasoning ability, judgment, memory, and marked personality changes. Open injury head trauma symptoms tend to be the experience of classic neuropsychological syndromes like aphasia, visual-spatial disorders, and types of memory or perceptual disorders.
Brain tumors are classified as either malignant and benign, and as intrinsic (directly infiltrate the parenchyma of the brain) or extrinsic (grows on the external surface of the brain and produces symptoms as a result of pressure on the brain tissue). Progressive cognitive changes associated with brain tumors may include confusion, poor comprehension, and even dementia. Symptoms tend to depend on the location of the tumor in the brain. For example, tumors on the frontal lobe tend to be associated with the sign of impairment of judgment, apathy, and loss of the ability to regulate/modulate behavior.
Findings have indicated abnormal functioning of brainstem structures in individuals with mental disorders such as schizophrenia, and other disorders that have to do with impairments in maintaining sustained attention. Some abnormalities in the average size or shape of some regions of the brain have been found in some disorders, reflecting genes and experiences. Studies of schizophrenia have tended to find enlarged ventricles and sometimes reduced volume of the cerebrum and hippocampus, while studies of (psychotic) bipolar disorder have sometimes found increased amygdala volume. Findings differ over whether volumetric abnormalities are risk factors or are only found alongside the course of mental health problems, possibly reflecting neurocognitive or emotional stress processes and medication use or substance use. Some studies have also found reduced hippocampal volumes in major depression, possibly worsening with time depression.

Neurotransmitter systems
Abnormal levels of dopamine activity correspond with several disorders (reduced in ADHD and OCD, and increased in schizophrenia). The dysfunction in serotonin and other monoamine neurotransmitters (norepinephrine and dopamine) correspond with certain mental disorders and their associated neural networks. Some include major depression, obsessive-compulsive disorder, phobias, post-traumatic stress disorder, and generalized anxiety disorder. Studies of depleted levels of monoamine neurotransmitters show an association with depression and other psychiatric disorders, but "... it should be questioned whether 5-HT [serotonin] represents just one of the final and not the main, factors in the neurological chain of events underlying psychopathological symptoms...."
Simplistic "chemical imbalance" explanations for mental disorders have never received empirical support; and most prominent psychiatrists, neuroscientists, and psychologists have not espoused such ill-defined, facile etiological theories. Instead, neurotransmitter systems have been understood in the context of the diathesis-stress or biopsychosocial models. The following 1967 quote from renowned psychiatric and neuroscience researchers exemplifies this more sophisticated understanding (in contrast to the woolly "chemical imbalance" notion).
Whereas specific genetic factors may be of importance in the etiology of some, and possibly all, depressions, it is equally conceivable that early experiences of the infant or child may cause enduring biochemical changes, that may predispose some individuals to depressions in adulthood. It is not likely that changes in the metabolism of the biogenic amines alone will account for the complex phenomena of normal or pathological affect.
Substance abuse
Substance abuse, especially long-term abuse, can cause or exacerbate many mental disorders. Alcoholism is linked to depression while abuse of amphetamines and LSD can leave a person feeling paranoid and anxious.
Correlations of mental disorders with drug use include cannabis, alcohol, and caffeine. At more than 300 mg, caffeine may cause anxiety or worsen anxiety disorders. Illicit drugs can stimulate particular parts of the brain that can affect development in adolescence. Cannabis has also been found to worsen depression and lessen an individual's motivation. Alcohol has the potential to damage "white matter" in the brain that affects thinking and memory. Alcohol is a problem in many countries due to many people participating in excessive drinking or binge drinking.
Life experience and environmental factors
The term "environment" is very loosely defined when it comes to mental illness. Unlike biological and psychological causes, environmental causes are stressors that individuals deal with in everyday life. These stressors range from financial issues to having low self-esteem. Environmental causes are more psychologically based, making them more closely related. Events that evoke feelings of loss or damage are most likely to cause a mental disorder to develop in an individual. Environmental factors include but are not limited to dysfunctional home life, poor relationships with others, substance abuse, not meeting social expectations, low self-esteem, and poverty.
Mind mentions childhood abuse, trauma, violence or neglect, social isolation, loneliness or discrimination, the death of someone close, stress, homelessness or housing, social disadvantage, poverty or debt, unemployment, caring for a family member or friend, significant trauma as an adult, such as military combat, and being involved in an accident or being the victim of a violent crime as possibly triggering an episode of mental illness.
Repeating generational patterns are a risk factor for mental illness.
Life events and emotional stress
Treatment in childhood and adulthood, including sexual abuse, physical abuse, emotional abuse, domestic violence, and bullying, has been linked to the development of mental disorders, through a complex interaction of societal, family, psychological and biological factors. Negative or stressful life events more generally have been implicated in the development of a range of disorders, including mood and anxiety disorders. The main risks appear to be from a cumulative combination of such experiences over time, although exposure to a single major trauma can sometimes lead to psychopathology, including PTSD. Resilience to such experiences varies, and a person may be resistant to some forms of experience but susceptible to others. Features associated with variations in resilience include genetic vulnerability, temperamental characteristics, cognitive set, coping patterns, and other experiences.
For bipolar disorder, stress (such as childhood adversity) is not a specific cause but does place genetically and biologically vulnerable individuals at risk for a more severe course of illness.
Poor parenting, abuse and neglect
Poor parenting is a risk factor for depression and anxiety. Separation or bereavement in families, and childhood trauma, be risk factors for psychosis and schizophrenia.
Severe psychological trauma, such as abuse, can wreak havoc on a person's life. Children are much more susceptible to psychological harm from traumatic events than adults. Once again, the reaction to the trauma will vary based on the person and the individual's age. Many factors impact these children. Many factors include the type of event, the length of exposure, and how the individual was affected. Study shows that human-induced trauma, such as a tumultuous childhood, affects children even more than natural disasters.
Neglect is a type of maltreatment related to the failure to provide needed, age-appropriate care, supervision, and protection. It is not to be confused with abuse, which, in this context, is defined as any action that intentionally harms or injures another person. Neglect most often happens during childhood by the parents or caretakers. Parents who are guilty of neglect were also neglected as children. The long-term effects of neglect are reduced physical, emotional, and mental health in a child and throughout adulthood.
Adverse childhood experiences
Adverse childhood experiences (ACEs) such as physical or emotional neglect or both, abuse, poverty, malnutrition, and traumatic experiences can have long-lasting negative consequences. Adverse experiences in childhood can affect the structural and functional development of the brain, giving structural and functional abnormalities in the future, and adulthood. ACEs and chronic trauma can disrupt the control of immune responses and promote chronic immune system activation giving rise to lasting inflammatory dysregulation. The Adverse Childhood Experiences Study has shown a strong dose–response relationship between ACEs and numerous health, social, and behavioral problems throughout a person's lifespan, including suicide attempts and frequency of depressive episodes. Several adverse childhood experiences can give a level of stress known as toxic stress. A child's neurological development can be disrupted when chronically exposed to stressful events such as physical, emotional, or sexual abuse, physical or emotional neglect, witnessing violence in the household, or a parent being incarcerated or having a mental illness. As a result, the child's cognitive functioning or ability to cope with negative or disruptive emotions can diminish. Over time, the child may adopt various harmful coping strategies that contribute to later disease and disability. Childhood adversity is associated with an increased risk of developing severe mental illnesses, including schizophrenia. Studies show that it could contribute to some features of the illness, including cognitive impairment. Findings from several studies have been mixed but some suggest that cognitive impairment is more related to forms of neglect than any other form of adversity. Underlying mechanisms remain unknown.
Familial and close relationships
Relationships and community have been extensively associated with mental health, success, and mental disorders. Home life and parental support impact social and mental development and health of individuals. Parental divorce, death, absence, or lack of continuity appears to increase risk, perhaps only if there is family discord or disorganization.[26] Early social privation, or lack of ongoing, harmonious, secure, committed relationships, has been implicated in the development of mental disorders.[27]
How an individual interacts with others as well as the quality of relationships can greatly increase or decrease a person's quality of living. Continuous conflict with friends, support system, and family can all lead to an increased risk of developing or worsening a mental illness or mental health state. A dysfunctional family may include disobedience, child neglect, and/or one with mental and/or abuse which occurs.[28]
Divorce is also another factor that can take a toll on both children and adults alike. Divorcees may have emotional adjustment problems due to a loss of intimacy and social connections. Newer statistics show that the negative effects of divorce have been overstated. The effects of divorce on children can be impactful on the child's mental health and development.
Social expectations and esteem
How individuals view themselves ultimately determines who they are, their abilities, and what they can be. Having both too low of self-esteem or too high can be detrimental to an individual's mental health. A person's self-esteem plays a role in their overall happiness and quality of life. Poor self-esteem can result in aggression, violence, self-deprecating behavior, anxiety, and other mental disorders.
Not fitting in with the masses can result in bullying and other types of emotional abuse. Bullying can result in depression, feelings of anger, loneliness.
Poverty

Studies show that there is a direct correlation between poverty and mental illness. The lower the socioeconomic status of an individual the higher the risk of mental illness. Impoverished people are two to three times more likely to develop mental illness than those of a higher economic class.
Low levels of self-efficiency and self-worth are experienced by children of disadvantaged families or those from the economic underclass. Theorists of child development have argued that persistent poverty leads to high levels of psychopathology and poor self-concepts.
This increased risk for psychiatric complications remains consistent for all individuals among the impoverished population, regardless of any in-group demographic differences that they may possess. These families must deal with economic stressors like unemployment and lack of affordable housing, which leads to mental health disorders. A person's socioeconomic class outlines the psychosocial, environmental, behavioral, and biomedical risk factors that are associated with mental health.
According to findings, there is a strong association between poverty and substance abuse. Substance abuse only perpetuates a continuous cycle. It can make it extremely difficult for individuals to find and keep jobs. As stated earlier, both financial problems and substance abuse can cause mental illnesses to develop.
Communities and cultures
Problems in communities or cultures, including poverty, unemployment or underemployment, lack of social cohesion, and migration, have been associated with the development of mental disorders. Stresses and strains related to socioeconomic position (socioeconomic status (SES) or social class) have been linked to the occurrence of major mental disorders, with a lower or more insecure educational, occupational, economic, or social position generally linked to more mental disorders. There have been mixed findings on the nature of the links and on the extent to which pre-existing personal characteristics influence the links. Both personal resources and community factors have been implicated, as well as interactions between individual-level and regional-level income levels. The causal role of different socioeconomic factors may vary by country. Socioeconomic deprivation in neighborhoods can cause worse mental health, even after accounting for genetic factors. Minority ethnic groups, including first or second-generation immigrants, are at greater risk for developing mental disorders, which has been attributed to various kinds of life insecurities and disadvantages, including racism. The direction of causality is sometimes unclear, and alternative hypotheses such as the drift hypothesis sometimes need to be discounted.
Psychological and individual factors, including resilience
Some clinicians believe that psychological characteristics alone determine mental disorders. Others speculate that abnormal behavior can be explained by a mix of social and psychological factors. In many examples, environmental and psychological triggers complement one another resulting in emotional stress, which in turn activates a mental illness. Each person is unique in how they will react to psychological stressors. What may break one person may have little to no effect on another. Psychological stressors, which can trigger mental illness, are as follows: emotional, physical, or sexual abuse, loss of a significant loved one, neglect, and being unable to relate to others.
The inability to relate to others is also known as emotional detachment. Emotional detachment makes it difficult for an individual to empathize with others or to share their feelings. An emotionally detached person may try to rationalize or apply logic to a situation to which there is no logical explanation. These individuals tend to stress the importance of their independence and maybe a bit neurotic. Often, the inability to relate to others stems from a traumatic event.
Mental characteristics of individuals, as assessed by both neurological and psychological studies, have been linked to the development and maintenance of mental disorders. This includes cognitive or neurocognitive factors, such as the way a person perceives, thinks, or feels about certain things; or an individual's overall personality, temperament, or coping style or the extent of protective factors or "positive illusions" such as optimism, personal control and a sense of meaning.
References
- "Mental, behavioural or neurodevelopmental disorders". International Classification of Diseases for Mortality and Morbidity Statistics, 11th rev. (ICD-11 MMS). World Health Organization. April 2019. Retrieved 2019-10-30.
Mental, behavioural and neurodevelopmental disorders are syndromes characterized by clinically significant disturbance in an individual's cognition, emotional regulation, or behaviour that reflects a dysfunction in the psychological, biological, or developmental processes that underlie mental and behavioural functioning. These disturbances are usually associated with distress or impairment in personal, family, social, educational, occupational, or other important areas of functioning.
- Webster's Third New International Dictionary, (Springfield, MA: Merriam-Webster, 1961, rev. 2016), ("mental illness noun, variants: or mental disorder or less commonly mental disease, Definition of mental illness: any of a broad range of medical conditions (such as major depression, schizophrenia, obsessive compulsive disorder, or panic disorder) that are marked primarily by sufficient disorganization of personality, mind, or emotions to impair normal psychological functioning and cause marked distress or disability and that are typically associated with a disruption in typical thinking, feeling, mood, behavior, interpersonal interactions, or daily functioning").
- American Heritage Dictionary of the English Language, 5th ed. (Boston: Houghton Mifflin Harcourt, 2011, rev. 2018), ("mental disorder, n. - Any of various disorders, such as schizophrenia, bipolar disorder, or autism spectrum disorder, characterized by a distressing or disabling impairment of an individual's cognitive, emotional, or social functioning.")
- Oxford English Dictionary, 3rd ed. (Oxford, UK: Oxford University Press, September 2001), ("II. Senses relating to the mind in an unhealthy or abnormal state. 5. a. Designating a temporary or permanent impairment of the mind due to inherited defect, injury, illness, or environment, usually needing special care or rehabilitation. Esp. in mental breakdown, mental deficiency, mental disease, mental disorder, mental incapacity, mental retardation, etc.; see also mental illness n. at Compounds. ... mental illness n. a condition which causes serious abnormality in a person's thinking or behaviour, esp. one requiring special care or treatment; a psychiatric illness. Now somewhat dated, and sometimes avoided as being potentially offensive.").
- Arango C, Díaz-Caneja CM, McGorry PD, Rapoport J, Sommer IE, Vorstman JA, et al. (July 2018). "Preventive strategies for mental health". The Lancet. Psychiatry. 5 (7): 591–604. doi:10.1016/S2215-0366(18)30057-9. hdl:11370/92f1a79c-f53d-47ae-be92-7a4c8d4b4e25. PMID 29773478. S2CID 21703364.
- Clark LA, Cuthbert B, Lewis-Fernández R, Narrow WE, Reed GM (September 2017). "Three Approaches to Understanding and Classifying Mental Disorder: ICD-11, DSM-5, and the National Institute of Mental Health's Research Domain Criteria (RDoC)". Psychological Science in the Public Interest. 18 (2): 72–145. doi:10.1177/1529100617727266. PMID 29211974. S2CID 206743519.
... research has shown that psychopathology generally arises from multiple biological, behavioral, psychosocial, and cultural factors, all interacting in complex ways and filtered through an individual's lifetime of experience. Research also has shown that the outcomes of these factors and their interactions are not clearly definable, distinct diseases, but are instead complex and variable combinations of psychological problems.
- Gatt JM, Burton KL, Williams LM, Schofield PR (January 2015). "Specific and common genes implicated across major mental disorders: a review of meta-analysis studies". Journal of Psychiatric Research. 60: 1–13. doi:10.1016/j.jpsychires.2014.09.014. PMID 25287955.
- Lahti-Pulkkinen M, Girchenko P, Tuovinen S, Sammallahti S, Reynolds RM, Lahti J, et al. (June 2020). "Maternal Hypertensive Pregnancy Disorders and Mental Disorders in Children". Hypertension. Ovid Technologies (Wolters Kluwer Health). 75 (6): 1429–1438. doi:10.1161/hypertensionaha.119.14140. PMID 32306771. S2CID 216028720.
- Rice F, Harold GT, Boivin J, van den Bree M, Hay DF, Thapar A (February 2010). "The links between prenatal stress and offspring development and psychopathology: disentangling environmental and inherited influences". Psychological Medicine. 40 (2): 335–345. doi:10.1017/S0033291709005911. PMC 2830085. PMID 19476689. S2CID 13752317.
- Ghaemi SN (November 2006). "Paradigms of psychiatry: eclecticism and its discontents". Current Opinion in Psychiatry. 19 (6): 619–624. doi:10.1097/01.yco.0000245751.98749.52. PMID 17012942. S2CID 22068456.
- Insel TR, Wang PS (May 2010). "Rethinking mental illness". JAMA. 303 (19): 1970–1971. doi:10.1001/jama.2010.555. PMID 20483974. S2CID 8210144.
- Hogan A. J. (2019). Social and medical models of disability and mental health: evolution and renewal. CMAJ: Canadian Medical Association journal, 191(1), E16–E18. https://doi.org/10.1503/cmaj.181008
- Murthy RS, et al. (2002) [2001]. The World Health Report 2001: Mental Health, New Understanding, New Hope (Reprint ed.). Geneva: World Health Organization. ISBN 9789241562010.
- Nyongesa, Andrew (2018-09-23). Tintinnabulation of Literary Theory: Traversing Genres to Contemporary Experience. Mwanaka Media and Publishing. doi:10.2307/j.ctvh9vxtv.8. ISBN 978-1-77906-514-8. JSTOR j.ctvh9vxtv. S2CID 239252932.
- Beardsworth, Sara (2005). "Freud's Oedipus and Kristeva's Narcissus: Three Heterogeneities". Hypatia. 20 (1): 54–77. doi:10.1111/j.1527-2001.2005.tb00373.x. ISSN 0887-5367. S2CID 143641177.
- Keller, Heidi (2018-11-05). "Universality claim of attachment theory: Children's socioemotional development across cultures". Proceedings of the National Academy of Sciences. 115 (45): 11414–11419. doi:10.1073/pnas.1720325115. ISSN 0027-8424. PMC 6233114. PMID 30397121.
- Waters, Everett; Hamilton, Claire E.; Weinfield, Nancy S. (2000). "The Stability of Attachment Security from Infancy to Adolescence and Early Adulthood: General Introduction". Child Development. 71 (3): 678–683. doi:10.1111/1467-8624.00175. ISSN 0009-3920. JSTOR 1132385. PMID 10953933.
- Fearon, R. Pasco; Bakermans-Kranenburg, Marian J.; van IJzendoorn, Marinus H.; Lapsley, Anne-Marie; Roisman, Glenn I. (2010). "The Significance of Insecure Attachment and Disorganization in the Development of Children's Externalizing Behavior: A Meta-Analytic Study". Child Development. 81 (2): 435–456. doi:10.1111/j.1467-8624.2009.01405.x. ISSN 0009-3920. JSTOR 40598991. PMID 20438450.
- https://www.genome.gov/genetics-glossary/Genome-Wide-Association-Studies Genome-wide association studies (GWAS). Genome.gov. (n.d.). Retrieved August 8, 2022
- Lu H, Qiao J, Shao Z, Wang T, Huang S, Zeng P (December 2021). "A comprehensive gene-centric pleiotropic association analysis for 14 psychiatric disorders with GWAS summary statistics". BMC Medicine. 19 (1): 314. doi:10.1186/s12916-021-02186-z. PMC 8667366. PMID 34895209.
- Lynch M. (2005). Simple evolutionary pathways to complex proteins. Protein science: a publication of the Protein Society, 14(9), 2217–2227. https://doi.org/10.1110/ps.041171805
- Contopoulos‐Ioannidis, Despina G.; Gianniki, Maria; Ai‐Nhi Truong, Angeline; Montoya, Jose G. (2022). "Toxoplasmosis and Schizophrenia: A Systematic Review and Meta‐Analysis of Prevalence and Associations and Future Directions". Psychiatric Research and Clinical Practice. American Psychiatric Association Publishing. 4 (2): 48–60. doi:10.1176/appi.prcp.20210041. ISSN 2575-5609. S2CID 248354624.
- "HIV and Dementia". www.hopkinsmedicine.org. Baltimore MD: The Johns Hopkins University, The Johns Hopkins Hospital, and Johns Hopkins Health System. 2021-08-08. Archived from the original on 2020-08-03. Retrieved 2022-05-04.
- Ebert, S.; Goos, M.; Rollwagen, L.; Baake, D.; Zech, W. D.; Esselmann, H.; Wiltfang, J.; Mollenhauer, B.; Schliebs, R.; Gerber, J.; Nau, R. (2010). "Recurrent systemic infections with Streptococcus pneumoniae do not aggravate the course of experimental neurodegenerative diseases". Journal of Neuroscience Research. 88 (5): 1124–1136. doi:10.1002/jnr.22270. PMID 19859962. S2CID 35148634.
- "Lyme Disease and Mental Health".
- Tashjian, Sarah; Mullins, Jordan (May 16, 2018). "Parenting Styles and Child Behavior". Psychology in Action. Archived from the original on October 17, 2018.
- https://www.mhanational.org/relationships Relationships. Mental Health America. (n.d.). Retrieved August 8, 2022
- Marquis, Peter (1992). "Family Dysfunction as a Risk Factor in the Development of Antisocial Behavior". Psychological Reports. 71 (2): 468–470. doi:10.2466/pr0.1992.71.2.468. PMID 1410104. S2CID 8826585.