Infectious causes of cancer
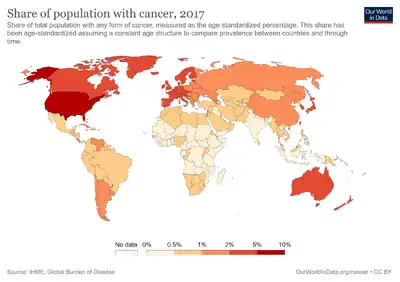
Estimates place the worldwide risk of cancers from infectious causes at 16.1%.[1] Viral infections are risk factors for cervical cancer, 80% of liver cancers, and 15–20% of the other cancers.[2] This proportion varies in different regions of the world from a high of 32.7% in Sub-Saharan Africa to 3.3% in Australia and New Zealand.[1]
A virus that can cause cancer is called an oncovirus or tumor virus. These include the human papillomavirus, which is associated with cervical carcinoma and nasopharyngeal carcinoma; Epstein-Barr virus, which is associated with a variety of Epstein-Barr virus-associated lymphoproliferative lymphomas; Kaposi's sarcoma herpesvirus, which is associated with Kaposi's sarcoma and primary effusion lymphoma; hepatitis B and hepatitis C viruses which are associated with hepatocellular carcinoma; human T-cell leukemia virus-1, which is associated with adult T-cell leukemia/lymphoma; and bovine leukemia virus, which is associated with breast cancer.[3] Bacterial infection may also increase the risk of cancer, as seen in Helicobacter pylori-induced stomach cancer.[4] Parasitic infections strongly associated with cancer include Schistosoma haematobium (squamous cell carcinoma of the bladder) and the liver flukes, Opisthorchis viverrini and Clonorchis sinensis (cholangiocarcinoma).[5]
Infection, cancer and mortality in the developed world
Infection is the fourth most important risk factor for cancer mortality in the developed world, causing about 10% of cancer mortality (see cancer prevention), coming after tobacco (~30% of cancers), diet (~30%) and obesity (~15%). Cancer causes 22.5% of deaths in the United States,[6] so that about 2% of mortality in the United States appears to be due to cancers caused by infections. This is comparable to mortality caused by influenza and pneumonia, which cause 2.1% of deaths in the United States.[6]
Importance of infectious causes of cancer mortality worldwide
Worldwide in 2015, the most common causes of cancer death were lung cancer (1.6 million deaths), liver cancer (745,000 deaths), and stomach cancer (723,000 deaths).[7] Lung cancer is largely due to non-infectious causes, such as tobacco smoke. However, liver and stomach cancer are primarily due to infectious causes. Liver cancer is largely caused by infectious hepatitis B virus (HBV) plus hepatitis C virus (HBC) and stomach cancer is largely caused by Helicobacter pylori bacteria. World-wide, the estimated number of people chronically infected with HBV and/or HCV is ~325 million.[8] Over half of the world's population is colonized with H. pylori and it is estimated that H. pylori-positive patients have a 1-2% risk of developing distal gastric cancer.[9]
Genome instability due to oncogenic infections
Genomic instability through various means such as DNA damage and epigenetic modifications[10] appear to be the basic causes of sporadic (non-familial) cancer. While infections have many effects, infectious organisms that increase the risk of cancer are frequently a source of DNA damage or genomic instability, as discussed below for oncogenic viruses and an oncogenic bacterium.
Viruses
Viruses are one of the most important risk factors for cancer development in humans.[2]
Infection by some hepatitis viruses, especially hepatitis B and hepatitis C, can induce a long-term viral infection that leads to liver cancer in about 1 in 200 of people infected with hepatitis B each year (more in Asia, fewer in North America), and in about 1 in 45 of people infected with hepatitis C each year.[11] People with chronic hepatitis B infection are more than 200 times more likely to develop liver cancer than uninfected people.[11] Liver cirrhosis, whether from chronic viral hepatitis infection or excessive alcohol use or some other cause, is independently associated with the development of liver cancer, and the combination of cirrhosis and viral hepatitis presents the highest risk of liver cancer development. Because chronic viral hepatitis is so common, and liver cancer so deadly, liver cancer is one of the most common causes of cancer-related deaths in the world, and is especially common in East Asia and parts of sub-Saharan Africa.
Human papillomaviruses (HPV) also cause many cancers. HPV is well known for causing genital warts and essentially all cases of cervical cancer, but it can also infect and cause cancer in several other parts of the body, including the esophagus larynx, lining of the mouth, nose, and throat, anus, vulva, vagina, and penis. The Papanicolaou smear ("Pap" smear) is a widely used cancer screening test for cervical cancer. DNA-based tests to identify the virus are also available.[12]
Herpesviruses are a third group of common cancer-causing viruses. Two types of herpesviruses have been associated with cancer: the Epstein–Barr virus (EBV) and human herpesvirus 8 (HHV-8).[13] EBV appears to cause all nonkeratinizing nasopharyngeal carcinomas, Epstein–Barr virus-positive diffuse large B-cell lymphomas, not otherwise specified,[14] diffuse large B-cell lymphomas associated with chronic inflammation,[14] Epstein–Barr virus-positive mucocutaneous ulcers,[15] Lymphomatoid granulomatoses[16] and, in many cases, fibrin-associated diffuse large B-cell lymphoma[17] and intravascular NK/T cell lymphomas.[18] It also appears to cause some cases of lymphoma, including Burkitt's lymphoma (this causal association is especially strong in Africa) and Hodgkin's disease,[13] EBV has been found in a variety of other types of cancer cells, although its role in causing these other cancers is not well established. KSHV/HHV-8[19] causes all cases of Kaposi's sarcoma, and has been found in some cases of a cancer-related condition called Castleman's disease.[13] Studies involving other kinds of cancer, particularly prostate cancer, have been inconsistent.[13] Both of these herpesviruses are commonly found in cancerous cells of primary effusion lymphoma.[13] Herpesviruses also cause cancer in animals, especially leukemias and lymphomas.[13]
Human T cell lymphotropic virus (HTLV-1) was the first human retrovirus discovered by Robert Gallo and colleagues at NIH.[20] The virus causes Adult T-cell leukemia, a disease first described by Takatsuki and colleagues in Japan[21] and other neurological diseases. Closely related to human T-cell leukemia virus, is another deltaretrovirus, bovine leukemia virus (BLV), which recently has met the expected criteria to accept a possible infectious agent causation of breast cancer, using sensitive PCR methods to detect BLV, and having samples from women with breast cancer compared to a control sample of women with no history of breast cancer.[22][23]
Merkel cell polyomavirus is the most recently discovered human cancer virus, isolated from Merkel cell carcinoma tissues in 2008,[24] by the same group that discovered KSHV/HHV-8 in 1994, using a new technology called digital transcriptome subtraction. About 80% of Merkel cell carcinomas are caused by Merkel cell polyomavirus; the remaining tumors have an unknown etiology and possibly a separate histogenesis. This is the only member of this group of viruses known to cause human cancer but other polyomaviruses are suspects for being additional cancer viruses.
HIV does not directly cause cancer, but it is associated with a number of malignancies, especially Kaposi's sarcoma, non-Hodgkin's lymphoma, anal cancer and cervical cancer. Kaposi's sarcoma is caused by human herpesvirus 8. AIDS-related cases of anal cancer and cervical cancer are commonly caused by human papillomavirus. After HIV destroys the immune system, the body is no longer able to control these viruses, and the infections manifest as cancer.[25] Certain other immune deficiency states (e.g. common variable immunodeficiency and IgA deficiency) are also associated with increased risk of malignancy.[26]
Common oncogenic viruses
In Western developed countries, human papillomavirus (HPV), hepatitis B virus (HBV) and hepatitis C virus (HCV) are the most frequently encountered oncogenic DNA viruses.[27]
Human papillomavirus
Worldwide, HPV causes the second largest fraction of infection-associated cancers or 5.2% of the global cancer burden.[28]
In the United States, HPV causes most cervical cancers, as well as some cancers of the vagina, vulva, penis, anus, rectum, and oropharynx (cancers of the back of the throat, including the base of the tongue and tonsils).[29] Each year in the United States, about 39,800 new cases of cancer are found in parts of the body where HPV is often found. HPV causes about 31,500 of these cancers.[29]
As reviewed by Münger et al.[30] there are about 200 HPVs. They can be classified into mucosal and cutaneous HPVs. Within each of these HPV groups, individual viruses are designated high risk or low risk according to the propensity for malignant progression of the lesions that they cause. Among the HPV high-risk viruses, the HPV E6 and E7 oncoproteins functionally inactivate the p53 and retinoblastoma tumor suppressors respectively. In addition, the high-risk HPV E6 and E7 oncoproteins can each independently induce genomic instability in normal human cells. They generate mitotic defects and aneuploidy through the induction of centrosome abnormalities.
Hepatitis B and hepatitis C viruses
Hepatitis virus-associated hepatocarcinogenesis is a serious health concern.[31] Liver cancer in the United States is primarily due to three main factors: hepatitis C virus (HCV) (22%), hepatitis B virus (HBV) (12%) and alcohol use (47%).[32] In 2017 there will be about 40,710 new cases of liver cancer in the United States.[33] World-wide, liver cancer mortality is more often due to hepatitis B virus (HBV) (33%), less often due to hepatitis C virus (HCV) (21%), and still frequently due to alcohol use (30%).[34] World-wide, liver cancer is the 4th most frequent cause of cancer mortality, causing 9% of all cancer mortality (total liver cancer deaths in 2015 being 810,500), and coming, in frequency, after lung, colorectal and stomach cancers.[34]
As reviewed by Takeda et al.,[31] HCV and HBV cause carcinogenic DNA damage and genomic instability by a number of mechanisms. HBV, and especially HCV, cause chronic inflammation in the liver, increasing reactive oxygen species (ROS) formation. ROS interact directly with DNA, causing multiple types of DNA damages (26 ROS-induced DNA damages are described by Yu et al.[35]) It also appears that chronic inflammation caused by HCV infection triggers the aberrant up-regulation of activation-induced cytidine deaminase (AID) in hepatocytes. AID creates mutations in DNA by deamination (a DNA damage) of the cytosine base, which converts cytosine into uracil. Thus, it changes a C:G base pair into a mutagenic U:G mismatch. In a still further cause of DNA damage, HCV core protein binds to the NBS1 protein and inhibits the formation of the Mre11/NBS1/Rad50 complex, thereby inhibiting DNA binding of repair enzymes.[36] As a result of reduced DNA repair mutagenic DNA damages can accumulate.
Bacteria
H. pylori, a common oncogenic bacterium
In addition to viruses, certain kinds of bacteria can cause some cancers. The most prominent example is the link between chronic infection of the wall of the stomach with Helicobacter pylori and gastric cancer.[37][38][39]
Although the data varies between different countries, overall about 1% to 3% of people infected with Helicobacter pylori develop gastric cancer in their lifetime compared to 0.13% of individuals who have no H. pylori infection.[40][9] Due to the prevalence of infection by H. pylori in middle-aged adults (74% in developing countries and 58% in developed countries in 2002[41]), and 1% to 3% likelihood of infected individuals developing gastric cancer,[42] H. pylori-induced gastric cancer is the third highest cause of worldwide cancer mortality as of 2018.[43]
The mechanism by which H. pylori causes cancer may involve chronic inflammation, or the direct action of some of its virulence factors, for example, CagA has been implicated in carcinogenesis.[44]
As reviewed by Chang and Parsonnet,[45] chronic H. pylori infection in the human stomach is characterized by chronic inflammation.[45] This is accompanied by epithelial cell release of reactive oxygen species (ROS) and reactive nitrogen species (RNOS), followed by the assembly of activated macrophages at the stomach site of infection. The macrophages also release ROS and RNOS. Levels of 8-oxo-2'-deoxyguanosine (8-OHdG), one of the predominant forms of free radical-induced oxidative DNA damages,[46] are increased more than 8-fold in DNA after infection by H. pylori, especially if the H. pylori are cagA positive.[47] The increase in 8-OHdG likely increases mutation.[48] In addition, oxidative stress, with high levels of 8-OHdG in DNA, also affects genome stability by altering chromatin status. Such alterations can lead to abnormal methylation of promoters of tumor suppressor genes.[49]
In addition to mutations caused by the direct damage to DNA by H. pylori-induced ROS, H. pylori-induced carcinogenic mutations and protein expression alterations are very often a result of H. pylori-induced epigenetic alterations.[50][51] These epigenetic alterations include H. pylori-induced methylation of CpG sites in promoters of genes[50] and H. pylori-induced altered expression of multiple microRNAs.[51]
As reviewed by Santos and Ribeiro[52] H. pylori infection is associated with epigenetically reduced efficiency of the DNA repair machinery, which favors the accumulation of mutations and genomic instability as well as gastric carcinogenesis. In particular, as reviewed by Raza et al.,[53] human gastric infection with H. pylori causes epigenetically reduced protein expression of DNA repair proteins MLH1, MGMT and MRE11. In addition, Raza et al.[53] showed that two further DNA repair proteins, ERCC1 and PMS2 had epigenetically severely reduced protein expression once H. pylori infection had progressed to cause dyspepsia (which occurs in 20% of infected individuals[54]).
Mycobacterium
Tuberculosis is a risk factor for lung cancer.[55]
Other bacteria
One meta-analysis of serological data comparing prior Chlamydia pneumoniae infection in patients with and without lung cancer found results suggesting prior infection was associated with a slightly increased risk of developing lung cancer.[56][57][58]
Parasites
The parasites that cause schistosomiasis (bilharzia), especially S. haematobium, can cause bladder cancer and cancer at other sites.[59] Inflammation triggered by the worm's eggs appears to be the mechanism by which squamous cell carcinoma of the bladder is caused. In Asia, infection by S. japonicum is associated with colorectal cancer.[59]
Distomiasis, caused by parasitic liver flukes, is associated with cholangiocarcinoma (cancer of the bile duct) in East Asia.[59]
Malaria is associated with Burkitt's lymphoma in Africa, especially when present in combination with Epstein-Barr virus, although it is unclear whether it is causative.[59]
Parasites are also a significant cause of cancer in animals. Cysticercus fasciolaris, the larval form of the common tapeworm of the cat, Taenia taeniaformis, causes cancer in rats.[59] Spirocerca lupi is associated with esophageal cancer in dogs, at least within the southern United States.[59]
A novel type of case, reported in 2015, involved an immunocompromised man whose tapeworm underwent malignant transformation, causing metastasis of tapeworm cell neoplasia throughout his body. This was not a cancer of his own cells but of the parasite's. This isolated case has no substantive bearing on public health but is interesting for being "a novel disease mechanism that links infection and cancer."[60]
See also
- Barry Marshall
- Clonally transmissible cancer
- Harald zur Hausen
- Helicobacter pylori eradication protocols
- J. Robin Warren
- List of human diseases associated with infectious pathogens
- List of oncogenic bacteria
- List of infectious diseases
- Francis Peyton Rous
References
- 1 2 de Martel C, Ferlay J, Franceschi S, Vignat J, Bray F, Forman D, Plummer M (June 2012). "Global burden of cancers attributable to infections in 2008: a review and synthetic analysis". The Lancet. Oncology. 13 (6): 607–15. doi:10.1016/S1470-2045(12)70137-7. PMID 22575588.
- 1 2 De Paoli P, Carbone A (October 2013). "Carcinogenic viruses and solid cancers without sufficient evidence of causal association". International Journal of Cancer. 133 (7): 1517–29. doi:10.1002/ijc.27995. PMID 23280523. S2CID 38402898.
- ↑ Buehring GC, Sans HM (December 2019). "Breast Cancer Gone Viral? Review of Possible Role of Bovine Leukemia Virus in Breast Cancer, and Related Opportunities for Cancer Prevention". International Journal of Environmental Research and Public Health. 17 (1): 209. doi:10.3390/ijerph17010209. PMC 6982050. PMID 31892207.
- ↑ Pagano JS, Blaser M, Buendia MA, Damania B, Khalili K, Raab-Traub N, Roizman B (December 2004). "Infectious agents and cancer: criteria for a causal relation". Seminars in Cancer Biology. 14 (6): 453–71. doi:10.1016/j.semcancer.2004.06.009. PMID 15489139.
- ↑ Samaras V, Rafailidis PI, Mourtzoukou EG, Peppas G, Falagas ME (June 2010). "Chronic bacterial and parasitic infections and cancer: a review". Journal of Infection in Developing Countries. 4 (5): 267–81. doi:10.3855/jidc.819. PMID 20539059.
- 1 2 "The top 10 leading causes of death in the United States". 4 July 2019. Archived from the original on 24 November 2018. Retrieved 16 July 2023.
- ↑ Ferlay J, Soerjomataram I, Dikshit R, Eser S, Mathers C, Rebelo M, et al. (March 2015). "Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012". International Journal of Cancer. 136 (5): E359-86. doi:10.1002/ijc.29210. PMID 25220842. S2CID 6067341.
- ↑ "WHO | New hepatitis data highlight need for urgent global response". Archived from the original on April 21, 2017.
- 1 2 Kusters JG, van Vliet AH, Kuipers EJ (July 2006). "Pathogenesis of Helicobacter pylori infection". Clinical Microbiology Reviews. 19 (3): 449–90. doi:10.1128/CMR.00054-05. PMC 1539101. PMID 16847081.
- ↑ Ferguson LR, Chen H, Collins AR, Connell M, Damia G, Dasgupta S, et al. (December 2015). "Genomic instability in human cancer: Molecular insights and opportunities for therapeutic attack and prevention through diet and nutrition". Seminars in Cancer Biology. 35 Suppl (Suppl): S5–S24. doi:10.1016/j.semcancer.2015.03.005. PMC 4600419. PMID 25869442.
- 1 2 Sung MW, Thung SN, Acs G (2000). "Hepatitis Viruses". In Bast RC, Kufe DW, Pollock RE, et al. (eds.). Holland-Frei Cancer Medicine (5th ed.). Hamilton, Ontario: B.C. Decker. ISBN 1-55009-113-1. Archived from the original on 2022-01-20. Retrieved 2023-07-16.
- ↑ McLachlin CM, Crum CP (2000). "Papillomaviruses and Cervical Neoplasia". In Bast RC, Kufe DW, Pollock RE, et al. (eds.). Holland-Frei Cancer Medicine (e.5 ed.). Hamilton, Ontario: B.C. Decker. ISBN 1-55009-113-1. Archived from the original on 2021-04-22. Retrieved 2023-07-16.
- 1 2 3 4 5 6 Cohen JI (2000). "Herpesviruses". In Bast RC, Kufe DW, Pollock RE, et al. (eds.). Cancer Medicine (e.5 ed.). Hamilton, Ontario: B.C. Decker. ISBN 1-55009-113-1. Archived from the original on 2023-08-26. Retrieved 2023-07-16.
- 1 2 Grimm KE, O'Malley DP (February 2019). "Aggressive B cell lymphomas in the 2017 revised WHO classification of tumors of hematopoietic and lymphoid tissues". Annals of Diagnostic Pathology. 38: 6–10. doi:10.1016/j.anndiagpath.2018.09.014. PMID 30380402. S2CID 53196244.
- ↑ Ikeda T, Gion Y, Yoshino T, Sato Y (2019). "A review of EBV-positive mucocutaneous ulcers focusing on clinical and pathological aspects". Journal of Clinical and Experimental Hematopathology. 59 (2): 64–71. doi:10.3960/jslrt.18039. PMC 6661964. PMID 31257347.
- ↑ Sukswai N, Lyapichev K, Khoury JD, Medeiros LJ (January 2020). "Diffuse large B-cell lymphoma variants: an update". Pathology. 52 (1): 53–67. doi:10.1016/j.pathol.2019.08.013. PMID 31735345. S2CID 208142227.
- ↑ Boyer DF, McKelvie PA, de Leval L, Edlefsen KL, Ko YH, Aberman ZA, Kovach AE, Masih A, Nishino HT, Weiss LM, Meeker AK, Nardi V, Palisoc M, Shao L, Pittaluga S, Ferry JA, Harris NL, Sohani AR (March 2017). "Fibrin-associated EBV-positive Large B-Cell Lymphoma: An Indolent Neoplasm With Features Distinct From Diffuse Large B-Cell Lymphoma Associated With Chronic Inflammation". The American Journal of Surgical Pathology. 41 (3): 299–312. doi:10.1097/PAS.0000000000000775. PMID 28195879. S2CID 3521190.
- ↑ Zanelli M, Mengoli MC, Del Sordo R, Cagini A, De Marco L, Simonetti E, Martino G, Zizzo M, Ascani S (November 2018). "Intravascular NK/T-cell lymphoma, Epstein-Barr virus positive with multiorgan involvement: a clinical dilemma". BMC Cancer. 18 (1): 1115. doi:10.1186/s12885-018-5001-6. PMC 6238309. PMID 30442097.
- ↑ Chang Y, Cesarman E, Pessin MS, Lee F, Culpepper J, Knowles DM, Moore PS (December 1994). "Identification of herpesvirus-like DNA sequences in AIDS-associated Kaposi's sarcoma". Science. 266 (5192): 1865–9. Bibcode:1994Sci...266.1865C. doi:10.1126/science.7997879. PMID 7997879. S2CID 29977325. Archived from the original on 2020-09-22. Retrieved 2023-07-16.
- ↑ Poiesz BJ, Ruscetti FW, Gazdar AF, Bunn PA, Minna JD, Gallo RC (December 1980). "Detection and isolation of type C retrovirus particles from fresh and cultured lymphocytes of a patient with cutaneous T-cell lymphoma". Proceedings of the National Academy of Sciences of the United States of America. 77 (12): 7415–9. Bibcode:1980PNAS...77.7415P. doi:10.1073/pnas.77.12.7415. PMC 350514. PMID 6261256.
- ↑ Takatsuki K (March 2005). "Discovery of adult T-cell leukemia". Retrovirology. 2: 16. doi:10.1186/1742-4690-2-16. PMC 555581. PMID 15743528.
- ↑ Buehring GC, Shen HM, Jensen HM, Jin DL, Hudes M, Block G (2 September 2015). "Exposure to Bovine Leukemia Virus Is Associated with Breast Cancer: A Case-Control Study". PLOS ONE. 10 (9): e0134304. Bibcode:2015PLoSO..1034304B. doi:10.1371/journal.pone.0134304. PMC 4557937. PMID 26332838.
- ↑ Schwingel D, Andreolla AP, Erpen LM, Frandoloso R, Kreutz LC (27 February 2019). "Bovine leukemia virus DNA associated with breast cancer in women from South Brazil". Sci Rep. 9 (1): 2949. Bibcode:2019NatSR...9.2949S. doi:10.1038/s41598-019-39834-7. PMC 6393560. PMID 30814631.
- ↑ Feng H, Shuda M, Chang Y, Moore PS (February 2008). "Clonal integration of a polyomavirus in human Merkel cell carcinoma". Science. 319 (5866): 1096–100. Bibcode:2008Sci...319.1096F. doi:10.1126/science.1152586. PMC 2740911. PMID 18202256.
- ↑ Wood C, Harrington W (2005). "AIDS and associated malignancies". Cell Research. 15 (11–12): 947–52. doi:10.1038/sj.cr.7290372. PMID 16354573. S2CID 9498126.
- ↑ Mellemkjaer L, Hammarstrom L, Andersen V, Yuen J, Heilmann C, Barington T, et al. (December 2002). "Cancer risk among patients with IgA deficiency or common variable immunodeficiency and their relatives: a combined Danish and Swedish study". Clinical and Experimental Immunology. 130 (3): 495–500. doi:10.1046/j.1365-2249.2002.02004.x. PMC 1906562. PMID 12452841.
- ↑ Anand P, Kunnumakkara AB, Kunnumakara AB, Sundaram C, Harikumar KB, Tharakan ST, et al. (September 2008). "Cancer is a preventable disease that requires major lifestyle changes". Pharmaceutical Research. 25 (9): 2097–116. doi:10.1007/s11095-008-9661-9. PMC 2515569. PMID 18626751.
- ↑ Parkin DM (June 2006). "The global health burden of infection-associated cancers in the year 2002". International Journal of Cancer. 118 (12): 3030–44. CiteSeerX 10.1.1.623.9022. doi:10.1002/ijc.21731. PMID 16404738. S2CID 10042384.
- 1 2 "Human Papillomavirus (HPV) and Cancer | CDC". 2019-08-21. Archived from the original on 2018-09-09. Retrieved 2023-07-16.
- ↑ Münger K, Baldwin A, Edwards KM, Hayakawa H, Nguyen CL, Owens M, et al. (November 2004). "Mechanisms of human papillomavirus-induced oncogenesis". Journal of Virology. 78 (21): 11451–60. doi:10.1128/JVI.78.21.11451-11460.2004. PMC 523272. PMID 15479788.
- 1 2 Takeda H, Takai A, Inuzuka T, Marusawa H (January 2017). "Genetic basis of hepatitis virus-associated hepatocellular carcinoma: linkage between infection, inflammation, and tumorigenesis". Journal of Gastroenterology. 52 (1): 26–38. doi:10.1007/s00535-016-1273-2. PMID 27714455. S2CID 20772491.
- ↑ Akinyemiju T, Abera S, Ahmed M, Alam N, Alemayohu MA, Allen C, et al. (December 2017). "The Burden of Primary Liver Cancer and Underlying Etiologies From 1990 to 2015 at the Global, Regional, and National Level: Results From the Global Burden of Disease Study 2015". JAMA Oncology. 3 (12): 1683–1691. doi:10.1001/jamaoncol.2017.3055. PMC 5824275. PMID 28983565.
- ↑ "Key Statistics About Liver Cancer". Archived from the original on 2018-09-21. Retrieved 2023-07-16.
- 1 2 Wang H, Naghavi M, Allen C, Barber RM, Bhutta ZA, Carter A, et al. (GBD 2015 Mortality and Causes of Death Collaborators) (October 2016). "Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980-2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet. 388 (10053): 1459–1544. doi:10.1016/S0140-6736(16)31012-1. PMC 5388903. PMID 27733281.
- ↑ Yu Y, Cui Y, Niedernhofer LJ, Wang Y (December 2016). "Occurrence, Biological Consequences, and Human Health Relevance of Oxidative Stress-Induced DNA Damage". Chemical Research in Toxicology. 29 (12): 2008–2039. doi:10.1021/acs.chemrestox.6b00265. PMC 5614522. PMID 27989142.
- ↑ Machida K, McNamara G, Cheng KT, Huang J, Wang CH, Comai L, et al. (December 2010). "Hepatitis C virus inhibits DNA damage repair through reactive oxygen and nitrogen species and by interfering with the ATM-NBS1/Mre11/Rad50 DNA repair pathway in monocytes and hepatocytes". Journal of Immunology. 185 (11): 6985–98. doi:10.4049/jimmunol.1000618. PMC 3101474. PMID 20974981.
- ↑ Peter S, Beglinger C (2007). "Helicobacter pylori and gastric cancer: the causal relationship". Digestion. 75 (1): 25–35. doi:10.1159/000101564. PMID 17429205. S2CID 21288653.
- ↑ Wang C, Yuan Y, Hunt RH (August 2007). "The association between Helicobacter pylori infection and early gastric cancer: a meta-analysis". The American Journal of Gastroenterology. 102 (8): 1789–98. doi:10.1111/j.1572-0241.2007.01335.x. PMID 17521398. S2CID 22361105.
- ↑ Traulsen, Jan; Zagami, Claudia; Daddi, Alice Anna; Boccellato, Francesco (2021-03-01). "Molecular modelling of the gastric barrier response, from infection to carcinogenesis". Best Practice & Research Clinical Gastroenterology. 50–51: 101737. doi:10.1016/j.bpg.2021.101737. ISSN 1521-6918. PMID 33975688. S2CID 233900318. Archived from the original on 2022-06-18. Retrieved 2023-07-16.
- ↑ Kuipers EJ. Review article: exploring the link between Helicobacter pylori and gastric cancer. Alimentary Pharmacology & Therapeutics. Mar 1999 Supplement, Vol. 13, p3-11. 9p. DOI: 10.1046/j.1365-2036.1999.00002.x. (open access).
- ↑ Parkin DM (June 2006). "The global health burden of infection-associated cancers in the year 2002". International Journal of Cancer. 118 (12): 3030–44. doi:10.1002/ijc.21731. PMID 16404738. S2CID 10042384.
- ↑ Wroblewski LE, Peek RM, Wilson KT (October 2010). "Helicobacter pylori and gastric cancer: factors that modulate disease risk". Clinical Microbiology Reviews. 23 (4): 713–39. doi:10.1128/CMR.00011-10. PMC 2952980. PMID 20930071.
- ↑ Ferlay J, Colombet M, Soerjomataram I, Mathers C, Parkin DM, Piñeros M, et al. (April 2019). "Estimating the global cancer incidence and mortality in 2018: GLOBOCAN sources and methods". International Journal of Cancer. 144 (8): 1941–1953. doi:10.1002/ijc.31937. PMID 30350310. S2CID 53034092.
- ↑ Hatakeyama M, Higashi H (December 2005). "Helicobacter pylori CagA: a new paradigm for bacterial carcinogenesis". Cancer Science. 96 (12): 835–43. doi:10.1111/j.1349-7006.2005.00130.x. PMID 16367902. S2CID 5721063.
- 1 2 Chang AH, Parsonnet J (October 2010). "Role of bacteria in oncogenesis". Clinical Microbiology Reviews. 23 (4): 837–57. doi:10.1128/CMR.00012-10. PMC 2952975. PMID 20930075.
- ↑ Valavanidis A, Vlachogianni T, Fiotakis C (April 2009). "8-hydroxy-2' -deoxyguanosine (8-OHdG): A critical biomarker of oxidative stress and carcinogenesis". Journal of Environmental Science and Health. Part C, Environmental Carcinogenesis & Ecotoxicology Reviews. 27 (2): 120–39. doi:10.1080/10590500902885684. PMID 19412858. S2CID 8109353. Archived from the original on 2022-08-13. Retrieved 2023-07-16.
- ↑ Raza Y, Khan A, Farooqui A, Mubarak M, Facista A, Akhtar SS, et al. (October 2014). "Oxidative DNA damage as a potential early biomarker of Helicobacter pylori associated carcinogenesis". Pathology & Oncology Research. 20 (4): 839–46. doi:10.1007/s12253-014-9762-1. PMID 24664859. S2CID 18727504.
- ↑ Yasui M, Kanemaru Y, Kamoshita N, Suzuki T, Arakawa T, Honma M (March 2014). "Tracing the fates of site-specifically introduced DNA adducts in the human genome". DNA Repair. 15: 11–20. doi:10.1016/j.dnarep.2014.01.003. PMID 24559511.
- ↑ Nishida N, Arizumi T, Takita M, Kitai S, Yada N, Hagiwara S, et al. (2013). "Reactive oxygen species induce epigenetic instability through the formation of 8-hydroxydeoxyguanosine in human hepatocarcinogenesis". Digestive Diseases. 31 (5–6): 459–66. doi:10.1159/000355245. PMID 24281021. S2CID 23484545.
- 1 2 Muhammad JS, Eladl MA, Khoder G (February 2019). "Helicobacter pylori-induced DNA Methylation as an Epigenetic Modulator of Gastric Cancer: Recent Outcomes and Future Direction". Pathogens. 8 (1): 23. doi:10.3390/pathogens8010023. PMC 6471032. PMID 30781778.
- 1 2 Noto JM, Peek RM (2011). "The role of microRNAs in Helicobacter pylori pathogenesis and gastric carcinogenesis". Frontiers in Cellular and Infection Microbiology. 1: 21. doi:10.3389/fcimb.2011.00021. PMC 3417373. PMID 22919587.
- ↑ Santos JC, Ribeiro ML (August 2015). "Epigenetic regulation of DNA repair machinery in Helicobacter pylori-induced gastric carcinogenesis". World Journal of Gastroenterology. 21 (30): 9021–37. doi:10.3748/wjg.v21.i30.9021. PMC 4533035. PMID 26290630.
- 1 2 Raza Y, Ahmed A, Khan A, Chishti AA, Akhter SS, Mubarak M, et al. (February 2020). "Helicobacter pylori severely reduces expression of DNA repair proteins PMS2 and ERCC1 in gastritis and gastric cancer". DNA Repair. 89: 102836. doi:10.1016/j.dnarep.2020.102836. PMID 32143126. S2CID 212622031.
- ↑ Dore MP, Pes GM, Bassotti G, Usai-Satta P (2016). "Dyspepsia: When and How to Test for Helicobacter pylori Infection". Gastroenterology Research and Practice. 2016: 8463614. doi:10.1155/2016/8463614. PMC 4864555. PMID 27239194.
- ↑ Pallis AG, Syrigos KN (December 2013). "Lung cancer in never smokers: disease characteristics and risk factors". Critical Reviews in Oncology/Hematology. 88 (3): 494–503. doi:10.1016/j.critrevonc.2013.06.011. PMID 23921082.
- ↑ Zhan P, Suo LJ, Qian Q, Shen XK, Qiu LX, Yu LK, Song Y, et al. (March 2011). "Chlamydia pneumoniae infection and lung cancer risk: a meta-analysis". European Journal of Cancer. 47 (5): 742–7. doi:10.1016/j.ejca.2010.11.003. PMID 21194924.
- ↑ Mager DL (March 2006). "Bacteria and cancer: cause, coincidence or cure? A review". Journal of Translational Medicine. 4 (1): 14. doi:10.1186/1479-5876-4-14. PMC 1479838. PMID 16566840.
- ↑ Littman AJ, Jackson LA, Vaughan TL (April 2005). "Chlamydia pneumoniae and lung cancer: epidemiologic evidence". Cancer Epidemiology, Biomarkers & Prevention. 14 (4): 773–8. doi:10.1158/1055-9965.EPI-04-0599. PMID 15824142. S2CID 6510957.
- 1 2 3 4 5 6 Mustacchi P (2000). "Parasites". In Bast RC, Kufe DW, Pollock RE, Weichselbaum RR, Holland JF, Frei E (eds.). Holland-Frei Cancer Medicine (5th ed.). Hamilton, Ontario: B.C. Decker. ISBN 1-55009-113-1. Archived from the original on 2022-07-02. Retrieved 2023-07-16.
- ↑ Muehlenbachs A, Bhatnagar J, Agudelo CA, Hidron A, Eberhard ML, Mathison BA, et al. (November 2015). "Malignant Transformation of Hymenolepis nana in a Human Host". The New England Journal of Medicine. 373 (19): 1845–52. doi:10.1056/NEJMoa1505892. PMID 26535513.
- Bibliography
- Pelini P (2016). "Tumor and metastases to the lung caused by the bacterium Pseudomonas". Journal Contribution. figshare: 57227 Bytes. doi:10.6084/m9.figshare.3382954.v1.
Further reading
- Cornwall, Claudia M. Catching cancer : the quest for its viral and bacterial causes. Lanham: Rowman & Littlefield Publishers, 2013.