Oral hygiene
Oral hygiene is the practice of keeping one's oral cavity clean and free of disease and other problems (e.g. bad breath) by regular brushing of the teeth (dental hygiene) and adopting good hygiene habits. It is important that oral hygiene be carried out on a regular basis to enable prevention of dental disease and bad breath. The most common types of dental disease are tooth decay (cavities, dental caries) and gum diseases, including gingivitis, and periodontitis.[1]

General guidelines for adults suggest brushing at least twice a day with a fluoridated toothpaste: brushing before going to sleep at night and at after breakfast in the morning.[2] Cleaning between the teeth is called interdental cleaning and is as important as tooth brushing.[3] This is because a toothbrush cannot reach between the teeth and therefore only removes about 50% of plaque from the surface of the teeth.[4] There are many tools available for interdental cleaning which include floss, tape and interdental brushes; it is up to each individual to choose which tool they prefer to use.
Sometimes white or straight teeth are associated with oral hygiene. However, a hygienic mouth can have stained teeth or crooked teeth. To improve the appearance of their teeth, people may use tooth whitening treatments and orthodontics.
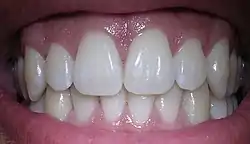
The importance of the role of the oral microbiome in dental health has been increasingly recognized.[5][6][7] Data from human oral microbiology research shows that a commensal microflora can switch to an opportunistic pathogenic flora through complex changes in their environment.[8] These changes are driven by the host rather than the bacteria.[9] Archeological evidence of calcified dental plaque shows marked shifts in the oral microbiome towards a disease-associated microbiome with cariogenic bacteria becoming dominant during the Industrial Revolution.[10][11] Streptococcus mutans is the most important bacteria in causing caries.Modern oral microbiota are significantly less diverse than historic populations.[10] Caries (cavities), for example, have become a major endemic disease, affecting 60-90% of schoolchildren in industrialized countries.[12] In contrast, dental caries and periodontal diseases were rare in pre-Neolithic and early hominins.[11][13]
Tooth cleaning and decay
.jpg.webp)
Tooth decay is the most common global disease.[14] Over 80% of cavities occur inside fissures in teeth where brushing cannot reach food left trapped after eating and saliva and fluoride have no access to neutralize acid and remineralize demineralized teeth, unlike easy-to-clean parts of the tooth, where fewer cavities occur.
Teeth cleaning is the removal of dental plaque and tartar from teeth to prevent cavities, gingivitis, gum disease, and tooth decay. Severe gum disease causes at least one-third of adult tooth loss.
Since before recorded history, a variety of oral hygiene measures have been used for teeth cleaning. This has been verified by various excavations done throughout the world, in which chew sticks, tree twigs, bird feathers, animal bones and porcupine quills have been found. In historic times, different forms of tooth cleaning tools have been used. Indian medicine (Ayurveda) has used the neem tree, or daatun, and its products to create teeth cleaning twigs and similar products; a person chews one end of the neem twig until it somewhat resembles the bristles of a toothbrush, and then uses it to brush the teeth. In the Muslim world, the miswak, or siwak, made from a twig or root, has antiseptic properties and has been widely used since the Islamic Golden Age. Rubbing baking soda or chalk against the teeth was also common; however, this can have negative side effects over time.[15]
The Australian Healthcare and Hospital Association's (AHHA) most recent evidence brief [16]) suggests that dental check-ups should be conducted once every three years for adults, and one every two years for children. It has been documented that dental professionals frequently advise for more frequent visits, but this advice is contraindicated by evidence suggesting that check up frequency should be based on individual risk factors, or the AHHA's check-up schedule. Professional cleaning includes tooth scaling, tooth polishing, and, if tartar has accumulated, debridement; this is usually followed by a fluoride treatment. However, the American Dental Hygienists' Association (ADHA) stated in 1998 that there is no evidence that scaling and polishing only above the gums provides therapeutic value, and cleaning should be done under the gums as well.[17] The Cochrane Oral Health Group found only three studies meeting the criteria for inclusion in their study and found little evidence in them to support claims of benefits from supragingival (above the gum) tooth scaling or tooth polishing.[18]
Dental sealants, which are applied by dentists, cover and protect fissures and grooves in the chewing surfaces of back teeth, preventing food from becoming trapped and thereby halt the decay process. An elastomer strip has been shown to force sealant deeper inside opposing chewing surfaces and can also force fluoride toothpaste inside chewing surfaces to aid in remineralising demineralised teeth.[19]
Between cleanings by a dental hygienist, good oral hygiene is essential for preventing tartar build-up which causes the problems mentioned above. This is done through careful, frequent brushing with a toothbrush, combined with the use of dental floss or interdental brushes to prevent accumulation of plaque on the teeth.[20] Powered toothbrushes reduce dental plaque and gingivitis more than manual toothbrushing in both short and long term.[21] Further evidence is needed to determine the clinical importance of these findings.[21]
Patients need to be aware of the importance of brushing and flossing their teeth daily. New parents need to be educated to promote healthy habits in their children.
Sources of problems
Plaque
Dental plaque, also known as dental biofilm, is a sticky, yellow film consisting of a wide range of bacteria that attaches to the tooth surfaces and can be visible around the gum line. It starts to reappear after the tooth surface has been cleaned, which is why regular brushing is encouraged.[1] A high-sugar diet encourages the formation of plaque. Sugar (fermentable carbohydrates), is converted into acid by the plaque. The acid then causes the breakdown of the adjacent tooth, eventually leading to tooth decay.[22]
If plaque is left on a subgingival (under the gum) surface undisturbed, not only is there an increased risk of tooth decay, but it will also go on to irritate the gums and make them appear red and swollen.[1] Some bleeding may be noticed during tooth brushing or flossing. These are the signs of inflammation that indicate poor gum health (gingivitis).[23][1]
Calculus
Dental calculus is composed of calcium phosphate minerals with live microorganisms that is covered by a unmineralized layer.[24]The longer that plaque stays on the tooth surface, the harder and more attached to the tooth it becomes. That is when it is referred to as calculus and needs to be removed by a dental professional.[1] If this is not treated, the inflammation will lead to the bone loss and will eventually lead to the affected teeth becoming loose.[25]
Preventive care
Tooth brushing
Routine tooth brushing is the principal method of preventing many oral diseases, and perhaps the most important activity an individual can practice to reduce plaque buildup.[26] Controlling plaque reduces the risk of the individual with plaque-associated diseases such as gingivitis, periodontitis, and caries – the three most common oral diseases.[27] The average brushing time for individuals is between 30 seconds and just over 60 seconds.[28][29][30][31][32][33] Many oral health care professionals agree that tooth brushing should be done for a minimum of two minutes, and be practiced at least twice a day.[34] Brushing for at least two minutes per session is optimal for preventing the most common oral diseases, and removes considerably more plaque than brushing for only 45 seconds.[26][34]
Toothbrushing can only clean to a depth of about 1.5 mm inside the gingival pockets, but a sustained regime of plaque removal above the gum line can affect the ecology of the microbes below the gums and may reduce the number of pathogens in pockets up to 5 mm in depth.[35]
Toothpaste (dentifrice) with fluoride, or alternatives such as nano-hydroxyapatite, is an important tool to readily use when tooth brushing. The fluoride (or alternative) in the dentifrice is an important protective factor against caries, and an important supplement needed to remineralize already affected enamel.[36] Currently, there is insufficient evidence to evaluate the caries inhibiting characteristics of slow release fluoride glass beads.[37] However, in terms of preventing gum disease, the use of toothpaste does not increase the effectiveness of the activity with respect to the amount of plaque removed.[26] People use toothpaste with nano-hydroxyapatite instead of fluoride as it performs the same function, and some people believe fluoride in toothpaste is a neurotoxin.
Population studies shown that regular tooth brushing is associated with reduced risk of cardiovascular diseases[38] and better blood pressure profile.[39]
Manual toothbrush
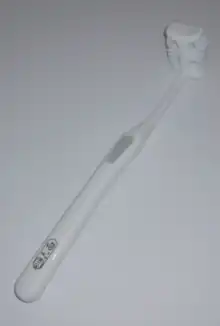
The modern manual tooth brush is a dental tool which consists of a head of nylon bristles attached to a long handle to help facilitate the manual action of tooth brushing. Furthermore, the handle aids in reaching as far back as teeth erupt in the oral cavity. The tooth brush is arguably a person's best tool for removing dental plaque from teeth, thus capable of preventing all plaque-related diseases if used routinely, correctly and effectively. Oral health professionals recommend the use of a tooth brush with a small head and soft bristles as they are most effective in removing plaque without damaging the gums.[40]
The technique is crucial to the effectiveness of tooth brushing and disease prevention.[40] Back and forth brushing is not effective in removing plaque at the gum line. Tooth brushing should employ a systematic approach, angle the bristles at a 45-degree angle towards the gums, and make small circular motions at that angle.[40] This action increases the effectiveness of the technique in removing plaque at the gum line.
Electric toothbrush
Electric toothbrushes are toothbrushes with moving or vibrating bristle heads. The two main types of electric toothbrushes are the sonic type which has a vibrating head, and the oscillating-rotating type in which the bristle head makes constant clockwise and anti-clockwise movements. Electric toothbrushes are more expensive than manual toothbrushes and more damaging to the environment.[41]
Sonic or ultrasonic toothbrushes vibrate at a high frequency with a small amplitude, and a fluid turbulent activity that aids in plaque removal.[42][43] The rotating type might reduce plaque and gingivitis compared to manual brushing, though it is currently uncertain whether this is of clinical significance.[44] The movements of the bristles and their vibrations help break up chains of bacteria up to 5mm below the gum line.[42] The oscillating-rotating electric toothbrush on the other hand uses the same mechanical action as produced by manual tooth brushing – removing plaque via mechanical disturbance of the biofilm – however at a higher frequency.
Using electric tooth brushes is less complex in regards to brushing technique, making it a viable option for children, and adults with limited dexterity. The bristle head should be guided from tooth to tooth slowly, following the contour of the gums and crowns of the tooth.[40] The motion of the toothbrush head removes the need to manually oscillate the brush or make circles.
Flossing
Tooth brushing alone will not remove plaque from all surfaces of the tooth as 40% of the surfaces are interdental.[3] One technique that can be used to access these areas is dental floss. When the proper technique is used, flossing can remove plaque and food particles from between the teeth and below the gums. The American Dental Association (ADA) reports that up to 80% of plaque may be removed by this method.[45] The ADA recommends cleaning between the teeth as part of one's daily oral hygiene regime.[45]
Types of floss include:[1]
- Unwaxed floss: Unbound nylon filaments that spread across the tooth. Plaque and debris get trapped for easy removal.[1]
- Waxed floss: less susceptible to tearing or shredding when used between tight contacts or areas with overhanging restorations.[1]
- Polytetrafluoroethylene (Teflon): Slides easily through tight contacts and does not fray.[1]
The type of floss used is a personal preference; however, without proper technique it may not be effective.[46] The correct technique to ensure maximum plaque removal is as follows:[1]
- Floss length: 15–25 cm wrapped around middle fingers.
- For upper teeth grasp the floss with thumb and index finger, for lower teeth with both index fingers. Ensure that a length of roughly an inch is left between the fingers.
- Ease the floss gently between the teeth using a back and forth motion.
- Position the floss in such a way that it becomes securely wrapped around the interdental surface of the tooth in a C shape.
- Ensure that the floss is taken below the gum margins using a back and forth up and down motion.
There are a few different options on the market that can make flossing easier if dexterity or coordination is a barrier, or as a preference over normal floss. Floss threaders are ideal for cleaning between orthodontic appliances, and flossettes are ideal for children and those with poor dexterity.[1] Special flossettes are made for those with orthodontics.
Interdental brushes
Interdental brushes come in a range of color-coded sizes. They consist of a handle with a piece of wire covered in tapered bristles, designed to be placed into the interdental space for plaque removal.[1] Studies indicate that interdental brushes are equally or more effective than floss when removing plaque and reducing gum inflammation.[1] They are especially recommended to people with orthodontics, often to use as well as floss.
The steps in using an interdental brush are as follows:[1]
- Identify the size required, the largest size that will fit without force is ideal, if necessary more than one size can be used.
- Insert the bristles into the interdental space at a 90-degree angle.
- Move the brush back and forth between the teeth.
- Rinse under water to remove debris when necessary.
- Rinse with warm soapy water once complete and store in a clean dry area.
- Replace once bristles are worn.
Tongue scrapers
The tongue contains numerous bacteria which causes bad breath. Tongue cleaners are designed to remove the debris built up on the tongue. Using a toothbrush to clean the tongue is another possibility, however it might be hard to reach the back of the tongue and the bristles of the toothbrush may be too soft to remove the debris.[1] Steps of using a tongue scraper:
- Rinse the tongue scraper in order to clean it and remove any present debris
- Start at the back of the tongue and gently scrape forwards. Be sure to clean the sides of the tongue, as well as the middle portion
- After the cleaning is completed, rinse the tongue scraper and any debris that is left behind
- Rinse the mouth[47]
Oral irrigation
Some dental professionals recommend subgingival irrigation, also known as water flossing, as a way to clean teeth and gums. Oral irrigators may be used instead of or in addition to flossing.[48][49][50][51]
Single-tufted brushes
Single-tufted brushes are a tool in conjunction with tooth brushing.[52] The tooth brush is designed to reach the 'hard to reach places' within the mouth. This tool is best used behind the lower front teeth, behind the back molars, crooked teeth and between spaces where teeth have been removed.[4] The single- tufted brush design has an angled handle, a 4mm diameter and rounded bristle tips.[4]
Gum stimulators
Toothbrushes with pointed rubber tips at the ends of the handles have been available for many years, and have more recently been replaced by a standalone tool called a gum stimulator designed to massage the gum line and the bases of the areas between the teeth. Such stimulators help to increase circulation to the gum line and to clear away bacteria which might not be removed by brushing and flossing alone.[53]
Oral swabs
Oral care swabs, commonly known as Toothettes, are small sponges attached to a stick, often used for oral care in hospital or long-term care settings.[54] The sponge is used to moisten and clear the patient's mouth of debris or thickened saliva in situations where conventional toothbrushing is not an option.[54]
Food and drink
Foods that help muscles and bones also help teeth and gums. Vitamin C is necessary, for example, to prevent scurvy, which manifests as serious gum disease.
Eating a balanced diet and limiting sugar intake can help prevent tooth decay and periodontal disease.[55] The Fédération dentaire internationale (FDI World Dental Federation) has promoted foods such as raw vegetables, plain yogurt, cheese, or fruit as dentally beneficial—this has been echoed by the American Dental Association (ADA).[56]
Beneficial foods
- Community water fluoridation is the addition of fluoride to adjust the natural fluoride concentration of a community's water supply to the level recommended for optimal dental health, approximately 1.0 ppm (parts per million).[57] Fluoride is a primary protector against dental cavities. Fluoride makes the surface of teeth more resistant to acids during the process of remineralization. Drinking fluoridated water is recommended by some dental professionals while others say that using toothpaste alone is enough.
- Milk, cheese, nuts and chicken are also rich in calcium and phosphate, and may also encourage remineralization.[58]
- The body cannot absorb all the required calcium if it lacks vitamin D, so fatty fish (salmon, for instance) as a major source of vitamin D helps an individual's teeth and gums to get more benefits of calcium.
- Green and black tea which is richly endowed with polyphenols acts as a suppressor of the bacteria that cause plaque, therefore it helps in sustaining oral health and is advisable during or after a meal.[59]
- Foods high in fiber (like vegetables) may help to increase the flow of saliva, and a bolus of fibre like celery string, fresh carrot or broccoli can force saliva into trapped food inside pits and fissures on chewing surfaces where over 80% of cavities occur, to dilute carbohydrates like sugar, neutralize acid and remineralize teeth on easy-to-reach surfaces.
Harmful foods
Sugars are commonly associated with dental cavities. Other carbohydrates, especially cooked starches, e.g. crisps/potato chips, may also damage teeth, although to a lesser degree (and indirectly) since starch has to be converted to glucose by salivary amylase (an enzyme in the saliva) first. Sugars in foods that are more 'sticky', such as toffee, are likely to cause more damage to teeth than those in less 'sticky' foods, such as certain forms of chocolate or most fruits.
- Sucrose (table sugar) is most commonly associated with cavities. The amount of sugar consumed at any one time is less important than how often food and drinks that contain sugar are consumed. The more frequently sugars are consumed, the greater the time during which the tooth is exposed to low pH levels, at which point demineralisation occurs (below 5.5 for most people). It is important therefore to try to encourage infrequent consumption of food and drinks containing sugar so that teeth have a chance to be repaired by remineralisation and fluoride. Limiting sugar-containing foods and drinks to meal times is one way to reduce the incidence of cavities. Sugars from fruit and fruit juices, e.g., glucose, fructose, and maltose can also cause cavities. Sucrose is used by Streptococcus mutans bacteria to produce biofilm. The sucrose is split by glucansucrase, which allows the bacteria to use the resulting glucose for building glucan polymer film and the resulting fructose as fuel to be converted to lactic acid.
- Acids contained in fruit juice, vinegar and soft drinks lower the pH level of the oral cavity which causes the enamel to demineralize. Drinking drinks such as orange juice or cola throughout the day raises the risk of dental cavities.[Source?]
- Another factor which affects the risk of developing cavities is the stickiness of foods. Some foods or sweets may stick to the teeth and so reduce the pH in the mouth for an extended time, particularly if they are sugary. It is important that teeth be cleaned at least twice a day, preferably with a toothbrush and fluoride toothpaste, to remove any food sticking to the teeth. Regular brushing and the use of dental floss also removes the dental plaque coating the tooth surface.
Chewing gum
Chewing gum assists oral irrigation between and around the teeth, cleaning and removing particles, but for teeth in poor condition it may damage or remove loose fillings as well. Dental chewing gums claim to improve dental health. Sugar-free chewing gum stimulates saliva production, and helps to clean the surface of the teeth.
Other
Smoking is one of the leading risk factors associated with periodontal diseases.[62][63] It is thought that smoking impairs and alters normal immune responses, eliciting destructive processes while inhibiting reparative responses promoting the incidence and development of periodontal diseases.[64]
Regular vomiting, as seen in bulimia nervosa and morning sickness also causes significant damage, due to acid erosion.
People with intellectual disability have increased risk of developing oral health problems like gum diseases or dental decay than the general population. For those people with severe disability, understanding the importance of oral hygiene and developing skills to achieve higher quality of oral care may not be their top priority. Therefore, studies have been conducted to assess different interventions to improve the knowledge and skills of the people with intellectual disabilities and their carer.[65]
Mouthwash
There are three commonly used kinds of mouthwash: saline (salty water), essential oils (Listerine, etc.), and chlorhexidine gluconate.
Saline
Saline (warm salty water) is usually recommended after procedures like dental extractions. In a study completed in 2014, warm saline mouthrinse was compared to no mouthrinse in preventing alveolar osteitis (dry socket) after extraction. In the group that was instructed to rinse with saline, the prevalence of alveolar osteitis was less than in the group that did not.[66]
Essential oils (EO) or cetyl pyridinium chloride (CPC)
Essential oils, found in Listerine mouthwash, contains eucalyptol, menthol, thymol, and methyl salicylate. CPC containing mouthwash contains cetyl pyridinium chloride, found in brands such as Colgate Plax, Crest Pro Health, Oral B Pro Health Rinse. In a meta-analyses completed in 2016, EO and CPC mouthrinses were compared and it was found that plaque and gingivitis levels were lower with EO mouthrinse when used as an adjunct to mechanical plaque removal (toothbrushing and interdental cleaning).[67]
Chlorhexidine
Chlorhexidine gluconate is an antiseptic mouthrinse that should only be used in two-week time periods due to brown staining on the teeth and tongue.[68] Compared to essential oils, it is more efficacious in controlling plaque levels, but has no better effect on gingivitis and is therefore generally used for post-surgical wound healing or the short-term control of plaque.[69]
Sodium hypochlorite
As mentioned earlier, sodium hypochlorite, a common household bleach, can be used as a 0.2% solution for 30 seconds two or three times a week as a cheap and effective means of combating harmful bacteria. The commercial product is 5% or 6%, so this requires diluting the product by a factor of about 30 (half a tablespoon in a full glass of water). The solution will lose activity with time and may be discarded after one day.[35]
Appliances care
Dentures
Dentures must be kept extremely clean. It is recommended that dentures be cleaned mechanically twice a day with a soft-bristled brush and denture cleansing paste. It is not recommended to use toothpaste, as it is too abrasive for acrylic, and will leave plaque retentive scratches in the surface.[70] Dentures should be taken out at night, as leaving them in whilst sleeping has been linked to poor oral health. Leaving a denture in during sleep reduces the protective cleansing and antibacterial properties of saliva against Candida albicans (oral thrush) and denture stomatitis; the inflammation and redness of the oral mucosa underneath the denture.[71] For the elderly, wearing a denture during sleep has been proven to greatly increase the risk of pneumonia.[71] It is now recommended that dentures should be stored in a dry container overnight, as keeping dentures dry for 8 hours significantly reduces the amount of Candida albicans on an acrylic denture.[72] Approximately once a week it is recommended to soak a denture overnight with an alkaline-peroxide denture cleansing tablet, as this has been proved to reduce bacterial mass and pathogenicity.[73][74]
Retainers
As with dentures, it is recommended to clean retainers properly at least once a day (avoiding toothpaste and using soap) and to soak them overnight with an alkaline-peroxide denture cleansing tablet once a week. Hot temperatures will warp the shape of the retainer, therefore rinsing under cold water is preferred. Keeping the retainer in a plastic case and rinsing it beforehand considered to help reduce the number of bacteria being transferred back into the mouth.[75][76]
Braces
While undertaking the braces treatment, it is recommended to use a small-sized or specialized toothbrush with a soft head to access hard-to-reach areas. Brushing after every meal is highly advisable.[77][78] Using a high fluoride toothpaste during treatment can be more effective than using a normal toothpaste.[79] Regular flossing is as important as brushing, and helps to remove any plaque build-up, as well as smaller food particles that are stuck in your braces or between your teeth. Floss threaders for braces or interdental brushes are also an option.[77][78] Furthermore, fluoride foam (high fluoride concentrations) application by a dentist every 6–8 weeks during treatment, could reduce dental decay. However, more research needs to be carried out regarding this.[79]
Education
To become a dental hygienist in the US one must attend a college or university that is approved by the Commission on Dental Accreditation and take the National Board Dental Hygiene Examination. There are several degrees one may receive. An associate degree after attending community college is the most common and only takes two years to obtain. After doing so, one may work in a dental office. There is also the option of receiving a bachelor's degree or master's degree if one plans to work in an educational institute either for teaching or research.
Oral hygiene and systemic diseases
Several recent clinical studies suggest oral disease and inflammation (oral bacteria & oral infections) may be a risk factor for serious systemic diseases, such as:[80][81]
- cardiovascular disease (heart attack and Stroke)
- bacterial pneumonia: Oral hygiene care for critically ill patients has been reported to reduce the risk of ventilator-associated pneumonia.[82]
- low birth weight or extreme high birth weight of one's baby
- diabetes complications
- osteoporosis
How mental illness and oral hygiene are related
Mental health disorders are a disturbance in a person's emotions that cause problems in mental functioning.[83] For example, the disorders can range from depression, anxiety, bipolar, and personality disorders. These mental health disorders can be a burden and are a daily challenge for many people. [83] Joanne Hudson reports, "It is estimated around 792 million people suffer mental health illness". The Coronavirus has caused an increase in how many people are suffering mental health illness.[84]There is found to be a strong correlation between people with mental health disorders and having dental fear.[85]People suffering from mental health disorders can have problems arising due to neglect of daily care of oral hygiene. For example, the problems that may arise are dry mouth, dental caries, jaw pain, oral cancer, and periodontitis also called gum disease. [86] In a twenty-five-year study, it was found that people suffering from mental health disorders have a 2.8 times increased chance of losing their teeth. [87]
In a study of an Australian community, there was a semi-structured interview that included males and females over the age of eighteen. The goal was to see how having mental health challenges affects a person's overall health, focusing mainly on oral health. The results showed not going to the dentist for cleanings, and not brushing their teeth at all, resulted in signs of tooth decay.[88]
Mental illness and oral hygiene in healthcare
Individuals are recommended to go to the dentist every six months for regular cleanings. The findings showed that individuals were less likely to do so because they felt that they would be treated differently, unfairly, or judged by the dentist.[89] At a National Opinion Research Center at the University of Chicago, a survey of about 150 questions was asked to a group of about 17,000 people. It was found that people struggling with bad oral health came from areas of low income, did not visit the dentist regularly, and struggled with poor mental health. [90]
In a study involving 2,784 psychiatric patients and 31,084 people from the general population, along with 131 nurses, a dental hygienist educated these patients on the importance of oral hygiene. The dental hygienist provided a twenty-minute PowerPoint presentation to show proper cleaning methods. The psychiatric patients observed that their oral hygiene was lacking and after the presentation, their oral care increased drastically. [91] It was reported by Shappell and her colleagues that individuals with psychiatric disorders stated that they do nothing for their oral health. She found that these individuals struggle with chronic oral pain and that is a stressor that decreases serotonin levels causing their mental health disorders to be a bigger challenge. [92]
See also
Reference list
- Darby M, Walsh MM (2010). Procedures Manual to Accompany Dental Hygiene: Theory and Practice. St. Louis, Mo.: Saunders/Elsevier.
- "Delivering better oral health: an evidence-based toolkit for prevention". GOV.UK. Retrieved 8 May 2021.
- Claydon NC (2008). "Current concepts in toothbrushing and interdental cleaning". Periodontology 2000. 48: 10–22. doi:10.1111/j.1600-0757.2008.00273.x. PMID 18715352.
- Lee DW, Moon IS (June 2011). "The plaque-removing efficacy of a single-tufted brush on the lingual and buccal surfaces of the molars". Journal of Periodontal & Implant Science. 41 (3): 131–134. doi:10.5051/jpis.2011.41.3.131. PMC 3139046. PMID 21811688.
- Kilian M, Chapple IL, Hannig M, Marsh PD, Meuric V, Pedersen AM, et al. (November 2016). "The oral microbiome - an update for oral healthcare professionals". British Dental Journal. 221 (10): 657–666. doi:10.1038/sj.bdj.2016.865. PMID 27857087.
- Mahasneh SA, Mahasneh AM (September 2017). "Probiotics: A Promising Role in Dental Health". Dentistry Journal. 5 (4): 26. doi:10.3390/dj5040026. PMC 5806962. PMID 29563432.
- Huttenhower C, Gevers D, Knight R, Abubucker S, Badger JH, Chinwalla AT, et al. (Human Microbiome Project Consortium) (June 2012). "Structure, function and diversity of the healthy human microbiome". Nature. 486 (7402): 207–214. Bibcode:2012Natur.486..207T. doi:10.1038/nature11234. PMC 3564958. PMID 22699609.
- Bartold PM, Van Dyke TE (June 2013). "Periodontitis: a host-mediated disruption of microbial homeostasis. Unlearning learned concepts". Periodontology 2000. 62 (1): 203–217. doi:10.1111/j.1600-0757.2012.00450.x. PMC 3692012. PMID 23574467.
- Marsh PD, Devine DA (March 2011). "How is the development of dental biofilms influenced by the host?". Journal of Clinical Periodontology. 38 (Suppl 11): 28–35. doi:10.1111/j.1600-051X.2010.01673.x. PMID 21323701.
- Adler CJ, Dobney K, Weyrich LS, Kaidonis J, Walker AW, Haak W, et al. (April 2013). "Sequencing ancient calcified dental plaque shows changes in oral microbiota with dietary shifts of the Neolithic and Industrial revolutions". Nature Genetics. 45 (4): 450–5, 455e1. doi:10.1038/ng.2536. PMC 3996550. PMID 23416520.
- Arthur C. Aufderheide (1998). The Cambridge Encyclopedia of Human Paleopathology. ISBN 9780521552035.
- Petersen PE, Bourgeois D, Ogawa H, Estupinan-Day S, Ndiaye C (September 2005). "The global burden of oral diseases and risks to oral health" (PDF). Bulletin of the World Health Organization. 83 (9): 661–669. PMC 2626328. PMID 16211157.
- Grine FE, Gwinnett AJ, Oaks JH (1990). "Early hominid dental pathology: interproximal caries in 1.5 million-year-old Paranthropus robustus from Swartkrans". Archives of Oral Biology. 35 (5): 381–386. doi:10.1016/0003-9969(90)90185-D. PMID 2196866.
- "Dental Caries (Tooth Decay)". Centers for Disease Control. 12 December 2018.
- "How to Whiten Your Teeth". WebMd.
- Gussy MG, Bracksley SA, Boxall AM (27 June 2013). "How often should you have dental visits?" (PDF). Deeble Institute.
- "American Dental Hygienists' Association Position Paper on the Oral Prophylaxis" (PDF). American Dental Hygienists' Association. 29 April 1998. Retrieved 28 June 2012.
- Lamont T, Worthington HV, Clarkson JE, Beirne PV (December 2018). "Routine scale and polish for periodontal health in adults". The Cochrane Database of Systematic Reviews. 12 (12): CD004625. doi:10.1002/14651858.CD004625.pub5. PMC 6516960. PMID 30590875.
- "Submission 9(b)—SuperTooth" (PDF). Archived from the original (PDF) on 27 February 2015. Retrieved 22 August 2014.
- Curtis J (13 November 2007). "Effective Tooth Brushing and Flossing". WebMD. Retrieved 24 December 2007.
- Yaacob M, Worthington HV, Deacon SA, Deery C, Walmsley AD, Robinson PG, Glenny AM (June 2014). "Powered versus manual toothbrushing for oral health". The Cochrane Database of Systematic Reviews. 2014 (6): CD002281. doi:10.1002/14651858.CD002281.pub3. PMC 7133541. PMID 24934383.
- Fejerskov O, Kidd E (2015). Dental Caries (2nd ed.). Chichester, West Sussex: Wiley Blackwell. p. 4.
- Porth C, Porth C (2011). Essentials of Pathophysiology (1st ed.). Philadelphia: Wolters Kluwer/Lippincott Williams & Wilkins.
- Forshaw R (9 December 2022). "Dental calculus - oral health, forensic studies and archaeology: a review". British Dental Journal. 233 (11): 961–967. doi:10.1038/s41415-022-5266-7. ISSN 0007-0610. PMC 9734501. PMID 36494546.
- Julihn A, Barr Agholme M, Modeer T (June 2008). "Risk factors and risk indicators in relation to incipient alveolar bone loss in Swedish 19-year-olds". Acta Odontologica Scandinavica. 66 (3): 139–147. doi:10.1080/00016350802087024. PMID 18568472. S2CID 3281135.
- Creeth JE, Gallagher A, Sowinski J, Bowman J, Barrett K, Lowe S, et al. (2009). "The effect of brushing time and dentifrice on dental plaque removal in vivo". Journal of Dental Hygiene. 83 (3): 111–116. PMID 19723429.
- "Oral health". World Health Organization. 2012. Archived from the original on 25 December 2007. Retrieved 7 May 2017.
- Dahl LO, Muhler JC (1955). "Oral Hygiene habits of young adults". J Periodontol. 26: 43–47. doi:10.1902/jop.1955.26.1.43.
- Van der Weijden GA, Timmerman MF, Nijboer A, Lie MA, Van der Velden U (August 1993). "A comparative study of electric toothbrushes for the effectiveness of plaque removal in relation to toothbrushing duration. Timerstudy". Journal of Clinical Periodontology. 20 (7): 476–481. doi:10.1111/j.1600-051X.1993.tb00394.x. PMID 8354721.
- Van der Weijden FA, Timmerman MF, Snoek IM, Reijerse E, Van der Velden U (July 1996). "Toothbrushing duration and plaque removing efficacy of electric toothbrushes". American Journal of Dentistry. 9 Spec No: S31–S36. PMID 9002786.
- Saxer UP, Barbakow J, Yankell SL. "New studies on estimated and actual toothbrushing times and dentifrice use." J Clin Dent 1998;9(2):49–51
- Robinson HB (September 1946). "Toothbrushing habits of 405 persons". Journal of the American Dental Association. 33 (17): 1112–1117. doi:10.14219/jada.archive.1946.0156. PMID 21000167.
- Beals D, Ngo T, Feng Y, Cook D, Grau DG, Weber DA. "Development and laboratory evaluation of a new toothbrush with a novel brush head design." Am J Dent. 2000;13:5A–13A
- McCracken GI, Janssen J, Swan M, Steen N, de Jager M, Heasman PA (May 2003). "Effect of brushing force and time on plaque removal using a powered toothbrush". Journal of Clinical Periodontology. 30 (5): 409–413. doi:10.1034/j.1600-051x.2003.20008.x. PMID 12716332.
- Slots J (October 2012). "Low-cost periodontal therapy". Periodontology 2000. 60 (1): 110–137. doi:10.1111/j.1600-0757.2011.00429.x. PMID 22909110.
- Marinho VC, Worthington HV, Walsh T, Clarkson JE (July 2013). "Fluoride varnishes for preventing dental caries in children and adolescents". The Cochrane Database of Systematic Reviews (7): CD002279. doi:10.1002/14651858.CD002279.pub2. PMID 23846772.
- Chong LY, Clarkson JE, Dobbyn-Ross L, Bhakta S (March 2018). "Slow-release fluoride devices for the control of dental decay". The Cochrane Database of Systematic Reviews. 3 (3): CD005101. doi:10.1002/14651858.CD005101.pub4. PMC 6494221. PMID 29495063.
- Park SY, Kim SH, Kang SH, Yoon CH, Lee HJ, Yun PY, et al. (April 2019). "Improved oral hygiene care attenuates the cardiovascular risk of oral health disease: a population-based study from Korea". European Heart Journal. 40 (14): 1138–1145. doi:10.1093/eurheartj/ehy836. PMID 30561631.
- Del Pinto R, Pietropaoli D, Grassi G, Muiesan ML, Monaco A, Cossolo M, et al. (December 2022). "Home oral hygiene is associated with blood pressure profiles: Results of a nationwide survey in Italian pharmacies". Journal of Clinical Periodontology. 49 (12): 1234–1243. doi:10.1111/jcpe.13720. PMC 9826426. PMID 36089901.
- "Brushing – Your Dental Health". Australian Dental Association. Retrieved 16 May 2017.
- "New research finds electric toothbrushes 'fairly horrifying' for the environment - but bamboo brushes aren't the answer". independent. 15 September 2020. Retrieved 8 May 2021.
- Hashizume LN, Dariva A (December 2015). "Effect of sonic vibration of an ultrasonic toothbrush on the removal of Streptococcus mutans biofilm from enamel surface". American Journal of Dentistry. 28 (6): 347–350. PMID 26846041.
- Re D, Augusti G, Battaglia D, Giannì AB, Augusti D (March 2015). "Is a new sonic toothbrush more effective in plaque removal than a manual toothbrush?". European Journal of Paediatric Dentistry. 16 (1): 13–18. PMID 25793947.
- Deacon SA, Glenny AM, Deery C, Robinson PG, Heanue M, Walmsley AD, Shaw WC (December 2010). "Different powered toothbrushes for plaque control and gingival health". The Cochrane Database of Systematic Reviews. 2010 (12): CD004971. doi:10.1002/14651858.CD004971.pub2. PMC 8406707. PMID 21154357.
- Accepted Dental Therapeutics. Vol. Section III (40th ed.). Council on Dental Therapeutics.
- Schmid MO, Balmelli OP, Saxer UP (August 1976). "Plaque-removing effect of a toothbrush, dental floss, and a toothpick". Journal of Clinical Periodontology. 3 (3): 157–165. doi:10.1111/j.1600-051X.1976.tb01863.x. PMID 1067277.
- Wiley C (2017). "Using a Tongue Cleaner for a Cleaner Mouth". Colgate. Retrieved 16 April 2017.
- Cobb CM, Rodgers RL, Killoy WJ (March 1988). "Ultrastructural examination of human periodontal pockets following the use of an oral irrigation device in vivo". Journal of Periodontology. 59 (3): 155–163. doi:10.1902/jop.1988.59.3.155. PMID 3162980.
- Greenstein G (April 1988). "The ability of subgingival irrigation to enhance periodontal health". Compendium. 9 (4): 327–9, 332–4, 336–8. PMID 3073855.
- Ciancio S (1988). "Oral Irrigation: A Current Perspective". Biological Therapies in Dentistry. 3: 33.
- Flemmig TF, Newman MG, Nachnani S, Rodrigues A, Calsina G, Lee Y, et al. (1989). "Chlorhexidine and irrigation in gingivitis: 6 months correlative clinical and microbiological findings". J Dent Res (68 (spec issue)).
- Slot DE, Dörfer CE, Van der Weijden GA (November 2008). "The efficacy of interdental brushes on plaque and parameters of periodontal inflammation: a systematic review". International Journal of Dental Hygiene. 6 (4): 253–264. doi:10.1111/j.1601-5037.2008.00330.x. PMID 19138177.
- Prevention Magazine Editors (2 March 2010). The Doctors Book of Home Remedies: Quick Fixes, Clever Techniques, and Uncommon Cures to Get You Feeling Better Fast. Potter/Ten Speed/Harmony/Rodale. p. 442. ISBN 978-1-60529-160-4.
- Dyck D, Bertone M, Knutson K, Campbell A (November 2012). "Improving oral care practice in long-term care". The Canadian Nurse. 108 (9): 20–24. PMID 23193758.
- "Academy of General Dentistry. How Does What I Eat Affect My Oral Health?". www.knowyourteeth.com. Retrieved 30 April 2020.
- Staff (2011). "Prevention". British Dental Centre. Archived from the original on 19 July 2012. Retrieved 28 June 2012.
- "Fluoride Facts" (PDF). American Dental Hygienists Association.
- "Diet and Oral Health". Web MD. Retrieved 9 October 2019.
- "7 foods for healthy teeth". Orthodontics Australia. 27 September 2017. Retrieved 10 February 2020.
- "Symptoms and causes - Mayo Clinic". Mayo Clinic. Retrieved 7 May 2017.
- "The cold, hard truth: Chewing ice and teeth". Go Ask Alice!. Retrieved 7 May 2017.
- Dietrich T, Maserejian NN, Joshipura KJ, Krall EA, Garcia RI (April 2007). "Tobacco use and incidence of tooth loss among US male health professionals". Journal of Dental Research. 86 (4): 373–377. doi:10.1177/154405910708600414. PMC 2582143. PMID 17384035.
- Palmer RM, Wilson RF, Hasan AS, Scott DA (2005). "Mechanisms of action of environmental factors--tobacco smoking". Journal of Clinical Periodontology. 32 (Suppl 6): 180–195. doi:10.1111/j.1600-051X.2005.00786.x. PMID 16128837.
- Ryder MI (2007). "The influence of smoking on host responses in periodontal infections". Periodontology 2000. 43: 267–277. doi:10.1111/j.1600-0757.2006.00163.x. PMID 17214844.
- Waldron C, Nunn J, Mac Giolla Phadraig C, Comiskey C, Guerin S, van Harten MT, et al. (May 2019). "Oral hygiene interventions for people with intellectual disabilities". The Cochrane Database of Systematic Reviews. 5 (5): CD012628. doi:10.1002/14651858.CD012628.pub2. PMC 6543590. PMID 31149734.
- Osunde OD, Adebola RA, Adeoye JB, Bassey GO (May 2014). "Comparative study of the effect of warm saline mouth rinse on complications after dental extractions". International Journal of Oral and Maxillofacial Surgery. 43 (5): 649–653. doi:10.1016/j.ijom.2013.09.016. PMID 24314857.
- Haas AN, Wagner TP, Muniz FW, Fiorini T, Cavagni J, Celeste RK (December 2016). "Essential oils-containing mouthwashes for gingivitis and plaque: Meta-analyses and meta-regression". Journal of Dentistry. 55: 7–15. doi:10.1016/j.jdent.2016.09.001. PMID 27628316.
- Strydonck DA, Slot DE, Velden U, Weijden F. "Effect of a chlorhexidine mouthrinse on plaque, gingival inflammation and staining in gingivitis patients: a systematic review." Journal of Clinical Periodontology. 2012;39(11):1042–1055.
- Van Leeuwen MP, Slot DE, Van der Weijden GA (February 2011). "Essential oils compared to chlorhexidine with respect to plaque and parameters of gingival inflammation: a systematic review". Journal of Periodontology. 82 (2): 174–194. doi:10.1902/jop.2010.100266. PMID 21043801.
- Harrison Z, Johnson A, Douglas CW (May 2004). "An in vitro study into the effect of a limited range of denture cleaners on surface roughness and removal of Candida albicans from conventional heat-cured acrylic resin denture base material". Journal of Oral Rehabilitation. 31 (5): 460–467. doi:10.1111/j.1365-2842.2004.01250.x. PMID 15140172.
- Iinuma T, Arai Y, Abe Y, Takayama M, Fukumoto M, Fukui Y, et al. (March 2015). "Denture wearing during sleep doubles the risk of pneumonia in the very elderly". Journal of Dental Research. 94 (3 Suppl): 28S–36S. doi:10.1177/0022034514552493. PMC 4541085. PMID 25294364.
- Stafford GD, Arendorf T, Huggett R (April 1986). "The effect of overnight drying and water immersion on candidal colonization and properties of complete dentures". Journal of Dentistry. 14 (2): 52–56. doi:10.1016/0300-5712(86)90051-5. PMID 3469239.
- Duyck J, Vandamme K, Krausch-Hofmann S, Boon L, De Keersmaecker K, Jalon E, Teughels W (2016). "Impact of Denture Cleaning Method and Overnight Storage Condition on Denture Biofilm Mass and Composition: A Cross-Over Randomized Clinical Trial". PLOS ONE. 11 (1): e0145837. Bibcode:2016PLoSO..1145837D. doi:10.1371/journal.pone.0145837. PMC 4701668. PMID 26730967.
- Duyck J, Vandamme K, Muller P, Teughels W (December 2013). "Overnight storage of removable dentures in alkaline peroxide-based tablets affects biofilm mass and composition". Journal of Dentistry. 41 (12): 1281–1289. doi:10.1016/j.jdent.2013.08.002. PMID 23948391.
- "How to care for your retainer?". Orthodontics Australia. 16 January 2020. Retrieved 10 February 2020.
- "How to Take Care of Your Retainer". priebeorthodontics.com. 23 April 2018. Retrieved 10 February 2020.
- Dr. Akshima Sahi. "Taking Care of Your Teeth with Braces". News Medical. Retrieved 10 February 2020.
- "Caring for braces". Orthodontics Australia. 27 June 2017. Retrieved 10 February 2020.
- Benson PE, Parkin N, Dyer F, Millett DT, Germain P (November 2019). "Fluorides for preventing early tooth decay (demineralised lesions) during fixed brace treatment". The Cochrane Database of Systematic Reviews. 2019 (11). doi:10.1002/14651858.cd003809.pub4. PMC 6863098. PMID 31742669.
- Li X, Kolltveit KM, Tronstad L, Olsen I (October 2000). "Systemic diseases caused by oral infection". Clinical Microbiology Reviews. 13 (4): 547–558. doi:10.1128/CMR.13.4.547-558.2000. PMC 88948. PMID 11023956.
- Lai YL (August 2004). "Osteoporosis and periodontal disease". Journal of the Chinese Medical Association. 67 (8): 387–388. PMID 15553796.
- Zhao T, Wu X, Zhang Q, Li C, Worthington HV, Hua F (December 2020). "Oral hygiene care for critically ill patients to prevent ventilator-associated pneumonia". The Cochrane Database of Systematic Reviews. 2020 (12): CD008367. doi:10.1002/14651858.CD008367.pub4. PMC 8111488. PMID 33368159.
- Joury, E.; Kisely, S.; Watt, R.G.; Ahmed, N.; Morris, A.J.; Fortune, F.; Bhui, K. (January 2023). "Mental Disorders and Oral Diseases: Future Research Directions". Journal of Dental Research. 102 (1): 5–12. doi:10.1177/00220345221120510. ISSN 0022-0345. PMID 36081351. S2CID 252160239.
- Hudson, Joanna (August 2021). "How mental health affects oral health". BDJ Student. 28 (3): 21–23. doi:10.1038/s41406-021-0225-3. ISSN 2056-4813. PMC 8407107.
- Kisely, Steve (May 2016). "No Mental Health without Oral Health". The Canadian Journal of Psychiatry. 61 (5): 277–282. doi:10.1177/0706743716632523. ISSN 0706-7437. PMC 4841282. PMID 27254802.
- "How mental illness affects your oral health".
- Kisely, Steve; Baghaie, Hooman; Lalloo, Ratilal; Siskind, Dan; Johnson, Newell W. (January 2015). "A Systematic Review and Meta-Analysis of the Association Between Poor Oral Health and Severe Mental Illness". Psychosomatic Medicine. 77 (1): 83–92. doi:10.1097/PSY.0000000000000135. ISSN 0033-3174. PMID 25526527. S2CID 23281727.
- Ho, HD; Satur, J; Meldrum, R (29 March 2017). "Perceptions of oral health by those living with mental illnesses in the Victorian Community - The consumer's perspective". International Journal of Dental Hygiene. 16 (2): e10–e16. doi:10.1111/idh.12278. hdl:11343/292713. ISSN 1601-5029. PMID 28370974. S2CID 4932351.
- Brondani, Mario A.; Alan, Rana; Donnelly, Leeann (22 May 2017). "Stigma of addiction and mental illness in healthcare: The case of patients' experiences in dental settings". PLOS ONE. 12 (5): e0177388. Bibcode:2017PLoSO..1277388B. doi:10.1371/journal.pone.0177388. ISSN 1932-6203. PMC 5439661. PMID 28531176.
- Tiwari, Tamanna; Kelly, Abigail; Randall, Cameron L.; Tranby, Eric; Franstve-Hawley, Julie (2022). "Association Between Mental Health and Oral Health Status and Care Utilization". Frontiers in Oral Health. 2. doi:10.3389/froh.2021.732882. ISSN 2673-4842. PMC 8859414. PMID 35199101.
- de Mey, Langha; Çömlekçi, Ceren; de Reuver, Fione; van Waard, Ineke; van Gool, Ronald; Scheerman, Janneke F.M.; van Meijel, Berno (July 2016). "Oral Hygiene in Patients With Severe Mental Illness: A Pilot Study on the Collaboration Between Oral Hygienists and Mental Health Nurses: Oral Hygiene in Patients With Severe Mental Illness: A Pilot Study on the Collaboration Between Oral Hygienists and Mental Health Nurses". Perspectives in Psychiatric Care. 52 (3): 194–200. doi:10.1111/ppc.12117. PMID 25902957.
- Shappell, Antoinette V.; Cartier, Pierre M. (27 June 2023). "Understanding the Mental-Dental Health Connection Said to Be Integral to Patient Care". Psychiatric News. 58 (7). doi:10.1176/appi.pn.2023.07.6.15. S2CID 259712437.