Amphetamine dependence
Amphetamine dependence refers to a state of psychological dependence on a drug in the amphetamine class.[1][2] Stimulants such as amphetamines and cocaine do not cause physical dependence.[3]
| Amphetamine dependence | |
|---|---|
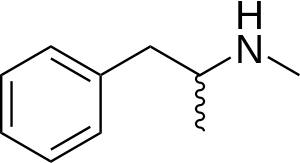 | |
| The structural formula of methamphetamine | |
| Specialty | Toxicology, psychiatry |
Signs of amphetamine intoxication manifest themselves in euphoria, hypersexuality, tachycardia, diaphoresis, and intensifications of the train of thought, speech, and movement. Over time, neurodegenerative changes become apparent in the form of altered behavior, reduced cognitive functions, and signs of neurological damage, such as a decrease in the levels of dopamine transporters (DAT) and serotonin transporters (SERT) in the brain.[4] Amphetamine use within teenagers can have lasting effects on their brain, in particular the prefrontal cortex. Amphetamine use is rising among students due to the ability to easily access prescribed stimulants like Adderall.[5] Also, in case of chronic use, vegetative disorders soon occur such as bouts of sweating, trouble sleeping, tremor, ataxia and diarrhea; the degradation of the personality takes place relatively slowly.[6][7] Tolerance is expected to develop with regular substituted amphetamine use.[7] When substituted amphetamines are used, drug tolerance develops rapidly.[8] Amphetamine dependence has shown to have the highest remission rate compared to cannabis, cocaine, and opioids.[9] Severe withdrawal associated with dependence from recreational substituted amphetamine use can be difficult for a user to cope with.[10][11][12] Long-term use of certain substituted amphetamines, particularly methamphetamine, can reduce dopamine activity in the brain.[13][4]
For amphetamine dependent individuals, psychotherapy is currently the best treatment option as no pharmacological treatment has been approved.[8] Another treatment option for amphetamine dependence is aversion therapy based on classical conditioning module; this will combine the amphetamine with a negative thing or opposite stimulus.[14] Treatment for amphetamines is growing at extremely high rates around the world.[15] Psychostimulants that increase dopamine and mimic the effects of substituted amphetamines, but with lower abuse liability, could theoretically be used as replacement therapy in amphetamine dependence.[8] However, the few studies that used amphetamine, bupropion, methylphenidate, and modafinil as a replacement therapy did not result in less methamphetamine use or craving.[8]
References
- "Amphetamine Use Disorder". The Lecturio Medical Concept Library. Retrieved 2021-06-23.
- "AWhat is methamphetamine?". National Institute on Drug Abuse. 16 May 2019. Retrieved 2021-06-23.
- Malenka RC, Nestler EJ, Hyman SE, Holtzman DM (2015). "Chapter 16: Reinforcement and Addictive Disorders". Molecular Neuropharmacology: A Foundation for Clinical Neuroscience (3rd ed.). New York: McGraw-Hill Medical. ISBN 9780071827706.
Pharmacologic treatment for psychostimulant addiction is generally unsatisfactory. As previously discussed, cessation of cocaine use and the use of other psychostimulants in dependent individuals does not produce a physical withdrawal syndrome but may produce dysphoria, anhedonia, and an intense desire to reinitiate drug use.
- Krasnova IN, Cadet JL (May 2009). "Methamphetamine toxicity and messengers of death". Brain Res Rev. 60 (2): 379–407. doi:10.1016/j.brainresrev.2009.03.002. PMC 2731235. PMID 19328213.
Neuroimaging studies have revealed that METH can indeed cause neurodegenerative changes in the brains of human addicts (Aron and Paulus, 2007; Chang et al., 2007). These abnormalities include persistent decreases in the levels of dopamine transporters (DAT) in the orbitofrontal cortex, dorsolateral prefrontal cortex, and the caudate-putamen (McCann et al., 1998, 2008; Sekine et al., 2003; Volkow et al., 2001a, 2001c). The density of serotonin transporters (5-HTT) is also decreased in the midbrain, caudate, putamen, hypothalamus, thalamus, the orbitofrontal, temporal, and cingulate cortices of METH-dependent individuals (Sekine et al., 2006).
- Varga, Matthew D. (2012-06-06). "Adderall Abuse on College Campuses: A Comprehensive Literature Review". Journal of Evidence-Based Social Work. 9 (3): 293–313. doi:10.1080/15433714.2010.525402. ISSN 1543-3714. PMID 22694135. S2CID 23405226.
- J. Saarma "Kliiniline psühhiaatria". Tallinn, 1980, p. 139
- O'Connor, Patrick. "Amphetamines: Drug Use and Abuse". Merck Manual Home Health Handbook. Merck. Retrieved 26 September 2013.
- Pérez-Mañá, C; Castells X; Torrens M; Capellà D; Farre M. (September 2013). "Efficacy of psychostimulant drugs for amphetamine abuse or dependence". Cochrane Database of Systematic Reviews. 9 (9): CD009695. doi:10.1002/14651858.CD009695.pub2. PMID 23996457. Retrieved 8 September 2013.
- Calabria, Bianca; Degenhardt, Louisa; Briegleb, Christina; Vos, Theo; Hall, Wayne; Lynskey, Michael; Callaghan, Bridget; Rana, Umer; McLaren, Jennifer (2010-08-01). "Systematic review of prospective studies investigating "remission" from amphetamine, cannabis, cocaine or opioid dependence". Addictive Behaviors. 35 (8): 741–749. doi:10.1016/j.addbeh.2010.03.019. ISSN 0306-4603. PMID 20444552.
- Chronic Amphetamine Use and Abuse Archived April 3, 2010, at the Wayback Machine
- Sax KW, Strakowski SM (2001). "Behavioral sensitization in humans". J Addict Dis. 20 (3): 55–65. doi:10.1300/J069v20n03_06. PMID 11681593. S2CID 1606101.
- I. Boileau; A. Dagher; M. Leyton; R. N. Gunn; G. B. Baker; M. Diksic; C. Benkelfat (2006). "Modeling Sensitization to Stimulants in Humans: An [11C]Raclopride/Positron Emission Tomography Study in Healthy Men". Arch Gen Psychiatry. 63 (12): 1386–1395. doi:10.1001/archpsyc.63.12.1386. PMID 17146013.
- Malenka RC, Nestler EJ, Hyman SE (2009). "15". In Sydor A, Brown RY (eds.). Molecular Neuropharmacology: A Foundation for Clinical Neuroscience (2nd ed.). New York: McGraw-Hill Medical. p. 370. ISBN 9780071481274.
Unlike cocaine and amphetamine, methamphetamine is directly toxic to midbrain dopamine neurons.
- "Title Page – Abnormal Psychology". opentext.wsu.edu. Retrieved 2021-05-28.
- Lee, Nicole K.; Jenner, Linda; Harney, Angela; Cameron, Jacqui (2018-11-01). "Corrigendum to "Pharmacotherapy for amphetamine dependence: A systematic review" [Drug Alcohol Depend. 191 (2018) 309–337]". Drug and Alcohol Dependence. 192: 238. doi:10.1016/j.drugalcdep.2018.09.002. ISSN 0376-8716. PMID 30278418.
External links
+![]() Media related to Amphetamine dependence at Wikimedia Commons
Media related to Amphetamine dependence at Wikimedia Commons