Neonatal hepatitis
| Neonatal hepatitis | |
|---|---|
| Other names: Neonatal hepatitis syndrome,[1] nonspecific neonatal hepatitis,[2] idiopathic neonatal hepatitis,[2] cryptogenic neonatal hepatitis,[2] idiopathic neonatal cholestasis[3] | |
| Video explanation | |
| Specialty | Neonatology |
| Symptoms | Yellowish skin and eyes, itchiness, dark urine[3] |
| Complications | Failure to grow normally, bleeding, liver failure[3] |
| Usual onset | First year of life[2] |
| Causes | Unknown, viral infection, metabolic disease, anatomical abnormality, tumor, toxin exposure, autoimmune disorder[1][2] |
| Diagnostic method | High conjugated bilirubin, ultrasound, liver biopsy[3] |
| Treatment | Special nutrition, vitamin supplementation, ursodeoxycholic acid, liver transplant[3] |
| Frequency | 1 in 2,500 newborns[2] |
Neonatal hepatitis refers to prolonged cholestasis in a baby (high conjugated bilirubin).[2] Some use the term when this occurs for any reason,[1] while others use the term only when the cause is unknown.[2] Symptoms may include yellowish skin and eyes, itchiness, and dark urine.[3] Complications may include failure to grow normally, bleeding, and liver failure.[3]
The cause may be unknown, viral infection, metabolic disease, anatomical abnormalities such as biliary atresia, tumor, toxin exposure, or autoimmune disorder.[1][2] The most commonly implicated metabolic condition is galactosaemia and the most common infection is cytomegalovirus.[2] Diagnosis may involve ultrasound and liver biopsy.[3]
Treatment may include special nutrition, vitamin supplementation, and ursodeoxycholic acid.[3] Occasionally if end stage liver disease occurs a liver transplant is required.[3]
Neonatal hepatitis affects about 1 in 2,500 newborns.[2] About 25% of cases have an unknown cause and this has become less common as medicine has advanced.[2] Biliary atresia represents about 25% of cases, while infections represent about 10%, and parenteral nutrition, alpha-1-antitrypsin deficiency, and perinatal asphyxia each cause about 5%.[2]
Signs and symptoms
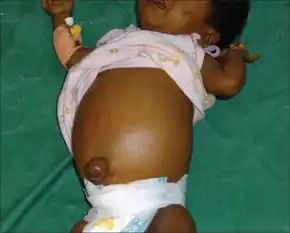
The infant with neonatal hepatitis usually has jaundice that appears at one to two months of age, is not gaining weight and growing normally, and has an enlarged liver and spleen. Infants with this condition are usually jaundiced. Jaundice that is caused by neonatal hepatitis is not the same as physiologic neonatal jaundice. In contrast with physiologic neonatal jaundice, infants with neonatal hepatitis present with dark urine. Infants may also present with delayed growth.[4]
Causes
The causes of neonatal hepatitis are many. Viruses that have been identified include cytomegalovirus, rubella virus, hepatitis A and B viruses, herpes simplex viruses, coxsackievirus, echovirus, and paramyxovirus.[5]
Metabolic and immune disorders can also cause neonatal hepatitis.[5] Giant cell transformation throughout the parenchyma is common.[5]
Diagnosis
Differential diagnosis
Conditions that can present similarly include galactosaemia, hereditary fructose intolerance, cystic fibrosis, and biliary atresia.[5]
Treatment
In terms of the management of this condition is symptom specific, additionally there is also[3]:
- Special supplement/formulas (may be used)
- Ursodeoxycholic acid (itching/pruritus)
- Liver transplantation
See also
References
- 1 2 3 4 Roberts, EA (October 2003). "Neonatal hepatitis syndrome". Seminars in neonatology : SN. 8 (5): 357–74. doi:10.1016/S1084-2756(03)00093-9. PMID 15001124.
- 1 2 3 4 5 6 7 8 9 10 11 12 13 Hadžić, N; Verkade, HJ (September 2016). "The Changing Spectrum of Neonatal Hepatitis". Journal of pediatric gastroenterology and nutrition. 63 (3): 316–9. doi:10.1097/MPG.0000000000001203. PMID 27007400.
- 1 2 3 4 5 6 7 8 9 10 11 "Neonatal Cholestasis". NORD (National Organization for Rare Disorders). Archived from the original on 23 October 2020. Retrieved 20 February 2021.
- ↑ Pediatric Gastrointestinal and Liver Disease (5 ed.). Elsevier. 2016. pp. 823–837.
- 1 2 3 4 Burt, Alastair (2018). MacSween's Pathology of the Liver (7 ed.). Elsevier. pp. 119–130.
External links
| Classification |
|---|