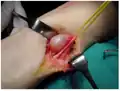
Schwannoma
| Schwannoma | |
|---|---|
| Other names: Neurilemmoma | |
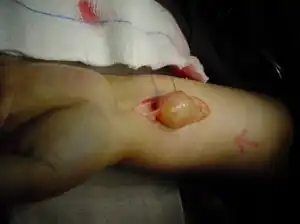 | |
| Schwannoma involving median nerve | |
| Specialty | Neurology, oncology |
| Usual onset | 30s to 50s[1] |
| Causes | Unknown[1] |
| Frequency | Rare, males=females[1] |
A schwannoma, also known as neurilemmoma, is a nerve sheath tumor, a type of soft tissue tumor composed of Schwann cells, which normally produce the insulating myelin sheath covering peripheral nerves.[1][2] Symptoms are typically of a small firm bump deep in tissue which may or may not be painful.[3] There may be one or several.[3]
The tumor cells always stay on the outside of the nerve, but the tumor itself may either push the nerve aside and/or up against a bony structure (thereby possibly causing damage). Schwannomas are relatively slow-growing. For reasons not yet understood, schwannomas are mostly benign and less than 1% become malignant, degenerating into a form of cancer known as neurofibrosarcoma. These masses are generally contained within a capsule, so surgical removal is often successful.[4]
Schwannomas can be associated with neurofibromatosis type II, which may be due to a loss-of-function mutation in the protein merlin.[5] They are universally S-100 positive, which is a marker for cells of neural crest cell origin.
Schwannomas of the head and neck are a fairly common occurrence and can be found incidentally in 3–4% of patients at autopsy.[5] Most common of these is a vestibular schwannoma, a tumor of the vestibulocochlear nerve that may lead to tinnitus and hearing loss on the affected side. Outside the cranial nerves, schwannomas may present on the flexor surfaces of the limbs. Rare occurrences of these tumors in the penis have been documented in the literature.[6]
Verocay bodies are seen histologically in schwannomas.[3]
Variants
- Pleural schwannoma is extremely rare. A unique subtype of schwannoma that typically develops in superficial (cutaneous or subcutaneous) sites and may be identified by its development pattern, which is plexiform (intraneuralnodular)[7][8].The correlation with schwannoma predisposition disorders like NF2 and schwannomatosis, however, is minimal (approximately 5 percent of cases)[9].These tumors might lack a capsule or be less encapsulated than a typical schwannoma.More challenging to identify from MPNST are the infrequent plexiform schwannomas that develop in deep anatomical sites, such as soft tissue[10] or major peripheral nerves.[11] These tumors may exhibit enhanced cellularity and mitotic activity. Although the likelihood of these tumors developing into cancer is extremely low, local recurrence is possible in around half of cases. On MRI, it usually shows hyper or iso-intensity on T1-weighted images and heterogenous hyperintensities on T2 weighted images. Pleural schwannoma typically shows fatty degeneration, hemorrhage, perivascular hyalinization, and cystic formation thus giving heterogenous hyperintensities on T2 weighted images. Complete surgical removal of pleural schwannoma is the usual treatment.[12]
- Cellular schwannoma is a relatively rare variation. Cellular schwannoma is nearly exclusively made up of a fascicular proliferation of well-differentiated Schwann cells that are cytologically bland, missing Verocay bodies, and just slightly exhibiting Antoni B pattern growth (10% of the tumor area).[13][14][15] Local recurrence is Variable (5-40%) and perhaps greater than in normal schwannomas.[16][17]
- Melanotic schwannoma is an uncommon, unique, and possibly cancerous neoplasm defined by epithelioid cells with variable-sized nuclei, substantial melanin deposition in neoplastic cells, and associated melanophages.[18]
Diagnosis
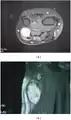 MRI showing schwannoma of ulna nerve
MRI showing schwannoma of ulna nerve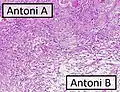 Micrograph of a schwannoma showing both a cellular Antoni A area (top) and a loose paucicellular Antoni B area (bottom). HE stain.
Micrograph of a schwannoma showing both a cellular Antoni A area (top) and a loose paucicellular Antoni B area (bottom). HE stain.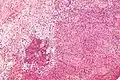
.JPG.webp)
_Antoni_B.jpg.webp) Subcutaneous schwannoma
Subcutaneous schwannoma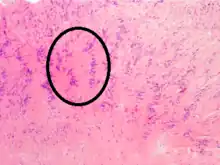 Antoni A area of schwannoma with Verocay bodies (one annotated by circle)
Antoni A area of schwannoma with Verocay bodies (one annotated by circle)_Antoni_B.jpg.webp)
_Antoni_B.jpg.webp)
_S-100_immunostain.jpg.webp)
Treatment
References
- 1 2 3 4 WHO Classification of Tumours Editorial Board, ed. (2020). "1. Soft tissue tumours: Schwannoma". Soft Tissue and Bone Tumours: WHO Classification of Tumours. Vol. 3 (5th ed.). Lyon (France): International Agency for Research on Cancer. pp. 226–227. ISBN 978-92-832-4503-2.
- ↑ "Schwannoma". www.cancer.gov. 30 July 2020. Archived from the original on 31 December 2022. Retrieved 13 March 2023.
- 1 2 3 James, William D.; Elston, Dirk; Treat, James R.; Rosenbach, Misha A.; Neuhaus, Isaac (2020). "28. Dermal and subcutaneous tumors". Andrews' Diseases of the Skin: Clinical Dermatology (13th ed.). Edinburgh: Elsevier. pp. 626–627. ISBN 978-0-323-54753-6. Archived from the original on 2023-10-26. Retrieved 2023-10-23.
- ↑ Biswas D, Marnane CN, Mal R, Baldwin D (September 2007). "Extracranial head and neck schwannomas--a 10-year review". Auris, Nasus, Larynx. 34 (3): 353–359. doi:10.1016/j.anl.2007.01.006. PMID 17376620.
- 1 2 Hanemann CO, Evans DG (December 2006). "News on the genetics, epidemiology, medical care and translational research of Schwannomas". Journal of Neurology. 253 (12): 1533–1541. doi:10.1007/s00415-006-0347-0. PMID 17219030. S2CID 11854280.
- ↑ Nguyen AH, Smith ML, Maranda EL, Punnen S (June 2016). "Clinical Features and Treatment of Penile Schwannoma: A Systematic Review". Clinical Genitourinary Cancer. 14 (3): 198–202. doi:10.1016/j.clgc.2015.12.018. PMID 26797586.
- ↑ Fletcher CD, Davies SE. Benign plexiform (multinodular) schwannoma: a rare tumour unassociated with neurofibromatosis. Histopathology. 1986; 10:971–980. [PubMed: 3096870]
- ↑ Woodruff JM, Marshall ML, Godwin TA, Funkhouser JW, Thompson NJ, Erlandson RA. Plexiform (multinodular) schwannoma. A tumor simulating the plexiform neurofibroma. Am J Surg Pathol. 1983; 7:691–697. [PubMed: 6638259]
- ↑ Berg JC, Scheithauer BW, Spinner RJ, Allen CM, Koutlas IG. Plexiform schwannoma: a clinicopathologic overview with emphasis on the head and neck region. Hum Pathol. 2008; 39:633–640. [PubMed: 18439936]
- ↑ Agaram NP, Prakash S, Antonescu CR. Deep-seated plexiform schwannoma: a pathologic study of 16 cases and comparative analysis with the superficial variety. Am J Surg Pathol. 2005; 29:1042–1048. [PubMed: 16006798]
- ↑ Hebert-Blouin MN, Amrami KK, Scheithauer BW, Spinner RJ. Multinodular/plexiform (multifascicular) schwannomas of major peripheral nerves: an underrecognized part of the spectrum of schwannomas. J Neurosurg. 2010; 112:372–382. [PubMed: 19499977]
- ↑ Iwasaki T (2016). "Giant ancient schwannoma of the pleura: Commentary". Lung India. 33 (4): 449–50. doi:10.4103/0970-2113.184928. PMC 4948239. PMID 27578944.
- ↑ Casadei GP, Scheithauer BW, Hirose T, Manfrini M, Van Houton C, Wood MB. Cellular schwannoma. A clinicopathologic, DNA flow cytometric, and proliferation marker study of 70 patients. Cancer. 1995; 75:1109–1119. [PubMed: 7850709]
- ↑ Fletcher CD, Davies SE, McKee PH. Cellular schwannoma: a distinct pseudosarcomatous entity. Histopathology. 1987; 11:21–35. [PubMed: 3557324]
- ↑ Wick MR, Swanson PE, Scheithauer BW, Manivel JC. Malignant peripheral nerve sheath tumor. An immunohistochemical study of 62 cases. Am J Clin Pathol. 1987; 87:425–433. [PubMed:2435144]
- ↑ White W, Shiu MH, Rosenblum MK, Erlandson RA, Woodruff JM. Cellular schwannoma. A clinicopathologic study of 57 patients and 58 tumors. Cancer. 1990; 66:1266–1275. [PubMed:2400975]
- ↑ Casadei GP, Scheithauer BW, Hirose T, Manfrini M, Van Houton C, Wood MB. Cellular schwannoma. A clinicopathologic, DNA flow cytometric, and proliferation marker study of 70 patients. Cancer. 1995; 75:1109–1119. [PubMed: 7850709]
- ↑ Mennemeyer RP, Hallman KO, Hammar SP, Raisis JE, Tytus JS, Bockus D. Melanotic schwannoma. Clinical and ultrastructural studies of three cases with evidence of intracellular melanin synthesis. Am J Surg Pathol. 1979; 3:3–10. [PubMed: 534381]
External links
| Classification |
|---|