Rickets
| Rickets | |
|---|---|
 | |
| X-ray of a two-year-old with rickets, with a marked bowing of the femurs and decreased bone density | |
| Pronunciation |
|
| Specialty | Pediatrics, rheumatology |
| Symptoms | Bowed legs, stunted growth, bone pain, large forehead, trouble sleeping[1][2] |
| Complications | Bone fractures, muscle spasms, abnormally curved spine, intellectual disability[2] |
| Usual onset | Childhood[2] |
| Types | Phosphopenic, calcipenic[3] |
| Causes | Diet without enough vitamin D or calcium, too little sun exposure, dark skin, exclusive breastfeeding without supplementation, celiac disease, certain genetic conditions[1][2][4] |
| Diagnostic method | Blood tests, X-rays[1] |
| Differential diagnosis | Fanconi syndrome, scurvy, Lowe syndrome, osteomalacia[2] |
| Prevention | Vitamin D supplements for exclusively-breastfed babies[5] |
| Treatment | Vitamin D and calcium[1] |
| Frequency | Relatively common (Middle East, Africa, Asia)[4] |
Rickets is a condition that results in weak or soft bones in children.[1] Symptoms include bowed legs, stunted growth, bone pain, large forehead, and trouble sleeping.[1][2] Complications may include bone fractures, muscle spasms, an abnormally curved spine, or intellectual disability.[1][2]
The most common cause of rickets is a vitamin D deficiency.[1] This can result from eating a diet without enough vitamin D, dark skin, too little sun exposure, exclusive breastfeeding without vitamin D supplementation, celiac disease, and certain genetic conditions.[1][2] Other factors may include not enough calcium or phosphorus.[4][5] The underlying mechanism involves defective mineralization at the growth plate.[6] Diagnosis is generally based on blood tests finding a low calcium, low phosphorus, and a high alkaline phosphatase together with X-rays.[1]
Prevention for exclusively breastfed babies is vitamin D supplements.[5] Otherwise, treatment depends on the underlying cause.[1] If due to a lack of vitamin D, treatment is usually with vitamin D and calcium.[1] This generally results in improvements within a few weeks.[1] Bone deformities may also improve over time.[5] Occasionally surgery may be done to correct bone deformities.[2][7] Genetic forms of the disease typically require specialized treatment.[5]
Rickets occurs relatively commonly in the Middle East, Africa, and Asia.[4] It is generally uncommon in the United States and Europe, except among certain minority groups.[2][4] It begins in childhood, typically between the ages of 3 and 18 months old.[2][4] Rates of disease are equal in males and females.[2] Cases of what is believed to have been rickets have been described since the 1st century,[8] and the condition was widespread in the Roman Empire.[9] The disease was common into the 20th century.[8] Early treatments included the use of cod liver oil.[8]
Signs and symptoms

Signs and symptoms of rickets can include bone tenderness, and a susceptibility for bone fractures particularly greenstick fractures.[10] Early skeletal deformities can arise in infants such as soft, thinned skull bones – a condition known as craniotabes,[11][12] which is the first sign of rickets; skull bossing may be present and a delayed closure of the fontanelles.
Young children may have bowed legs and thickened ankles and wrists;[13] older children may have knock knees.[10] Spinal curvatures of kyphoscoliosis or lumbar lordosis may be present. The pelvic bones may be deformed. A condition known as rachitic rosary can result as the thickening caused by nodules forming on the costochondral joints. This appears as a visible bump in the middle of each rib in a line on each side of the body. This somewhat resembles a rosary, giving rise to its name. The deformity of a pigeon chest[10] may result in the presence of Harrison's groove.
Hypocalcemia, a low level of calcium in the blood can result in tetany – uncontrolled muscle spasms. Dental problems can also arise.[10]
An X-ray or radiograph of an advanced sufferer from rickets tends to present in a classic way: the bowed legs (outward curve of long bone of the legs) and a deformed chest. Changes in the skull also occur causing a distinctive "square headed" appearance known as "caput quadratum".[14] These deformities persist into adult life if not treated. Long-term consequences include permanent curvatures or disfiguration of the long bones, and a curved back.[15]
Cause
Maternal deficiencies may be the cause of overt bone disease from before birth and impairment of bone quality after birth.[16][17] The primary cause of congenital rickets is vitamin D deficiency in the mother's blood, which the baby shares.[17] Vitamin D ensures that serum phosphate and calcium levels are sufficient to facilitate the mineralization of bone.[18] Congenital rickets may also be caused by other maternal diseases, including severe osteomalacia, untreated celiac disease, malabsorption, pre-eclampsia, and premature birth.[16] Rickets in children is similar to osteoporosis in the elderly, with brittle bones. Pre-natal care includes checking vitamin levels and ensuring that any deficiencies are supplemented.[19]
Also exclusively breast-fed infants may require rickets prevention by vitamin D supplementation or an increased exposure to sunlight.[20]
In sunny countries such as Nigeria, South Africa, and Bangladesh, there is sufficient endogenous vitamin D due to exposure to the sun. However, the disease occurs among older toddlers and children in these countries, which in these circumstances is attributed to low dietary calcium intakes due to a mainly cereal-based diet.[21]
Those at higher risk for developing rickets include:
- Breast-fed infants whose mothers are not exposed to sunlight
- Breast-fed infants who are not exposed to sunlight
- Breast-fed babies who are exposed to little sunlight
- Adolescents, in particular when undergoing the pubertal growth spurt[22]
- Any child whose diet does not contain enough vitamin D or calcium
Diseases causing soft bones in infants, like hypophosphatasia or hypophosphatemia can also lead to rickets.[23]
Strontium is allied with calcium uptake into bones; at excessive dietary levels strontium has a rachitogenic (rickets-producing) action.[24]
Sunlight
Sunlight, especially ultraviolet light, lets human skin cells convert vitamin D from an inactive to active state. In the absence of vitamin D, dietary calcium is not properly absorbed, resulting in hypocalcaemia, leading to skeletal and dental deformities and neuromuscular symptoms, e.g. hyperexcitability. Foods that contain vitamin D include butter, eggs, fish liver oils, margarine, fortified milk and juice, portabella and shiitake mushrooms, and oily fishes such as tuna, herring, and salmon. A rare X-linked dominant form exists called vitamin D-resistant rickets or X-linked hypophosphatemia.
Cases have been reported in Britain in recent years[25] of rickets in children of many social backgrounds caused by insufficient production in the body of vitamin D because the sun's ultraviolet light was not reaching the skin due to use of strong sunblock, too much "covering up" in sunlight, or not getting out into the sun. Other cases have been reported among the children of some ethnic groups in which mothers avoid exposure to the sun for religious or cultural reasons, leading to a maternal shortage of vitamin D;[26][27] and people with darker skins need more sunlight to maintain vitamin D levels.
Rickets had historically been a problem in London, especially during the Industrial Revolution. Persistent thick fog and heavy industrial smog permeating the city blocked out significant amounts of sunlight to such an extent that up to 80 percent of children at one time had varying degrees of rickets in one form or the other. It is sometimes known "the English Disease" in some foreign languages (e.g. German: 'Die englische Krankheit', Dutch: 'Engelse ziekte', Hungarian: "angolkor").
Evolutionary considerations
Vitamin D natural selection hypotheses: Rickets is often a result of vitamin D3 deficiency. The correlation between human skin color and latitude is thought to be the result of positive selection to varying levels of solar ultraviolet radiation. Northern latitudes have selection for lighter skin that allows UV rays to produce vitamin D from 7-dehydrocholesterol. Conversely, latitudes near the equator have selection for darker skin that can block the majority of UV radiation to protect from toxic levels of vitamin D, as well as skin cancer.[28]
An anecdote often cited to support this hypothesis is that Arctic populations whose skin is relatively darker for their latitude, such as the Inuit, have a diet that is historically rich in vitamin D. Since these people acquire vitamin D through their diet, there is not a positive selective force to synthesize vitamin D from sunlight.[29]
Environment mismatch: Ultimately, vitamin D deficiency arises from a mismatch between a population's previous evolutionary environment and the individual's current environment. This risk of mismatch increases with advances in transportation methods and increases in urban population size at high latitudes.
Similar to the environmental mismatch when dark-skinned people live at high latitudes, Rickets can also occur in religious communities that require long garments with hoods and veils.[30] These hoods and veils act as sunlight barriers that prevent individuals from synthesizing vitamin D naturally from the sun.
In a study by Mithal et al.,[31] Vitamin D insufficiency of various countries was measured by lower 25-hydroxyvitamin D. 25(OH)D is an indicator of vitamin D insufficiency that can be easily measured. These percentages should be regarded as relative vitamin D levels, and not as predicting evidence for development of rickets.
Asian immigrants living in Europe have an increased risk for vitamin D deficiency. Vitamin D insufficiency was found in 40% of non-Western immigrants in the Netherlands, and in more than 80% of Turkish and Moroccan immigrants.
The Middle East, despite high rates of sun-exposure, has the highest rates of rickets worldwide.[32] This can be explained by limited sun exposure due to cultural practices and lack of vitamin D supplementation for breast-feeding women. Up to 70% and 80% of adolescent girls in Iran and Saudi Arabia, respectively, have vitamin D insufficiency. Socioeconomic factors that limit a vitamin D rich diet also plays a role. In the United States, vitamin D insufficiency varies dramatically by ethnicity. Among males aged 70 years and older, the prevalence of low serum 25(OH) D levels was 23% for non-Hispanic whites, 45% for Mexican Americans, and 58% for non-Hispanic blacks. Among women, the prevalence was 28.5%, 55%, and 68%, respectively.
A systematic review published in the Cochrane Library looked at children up to three years old in Turkey and China and found there was a beneficial association between vitamin D and rickets. In Turkey children getting vitamin D had only a 4% chance of developing rickets compared to children who received no medical intervention. In China, a combination of vitamin D, calcium and nutritional counseling was linked to a decreased risk of rickets.[33]
With this evolutionary perspective in mind, parents can supplement their nutritional intake with vitamin D enhanced beverages if they feel their child is at risk for vitamin D deficiency.[34]
Diagnosis
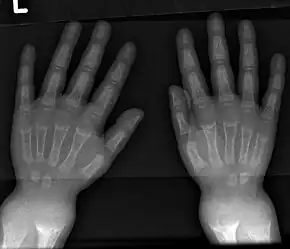

Rickets may be diagnosed with the help of:
- Blood tests:[35]
- Serum calcium may show low levels of calcium, serum phosphorus may be low, and serum alkaline phosphatase may be high from bones or changes in the shape or structure of the bones. This can show enlarged limbs and joints.
- A bone density scan may be undertaken.[35]
- Radiography typically show widening of the zones of provisional calcification of the metaphyses secondary to unmineralized osteoid. Cupping, fraying, and splaying of metaphyses typically appears with growth and continued weight bearing.[36] These changes are seen predominantly at sites of rapid growth, including the proximal humerus, distal radius, distal femur and both the proximal and the distal tibia. Therefore, a skeletal survey for rickets can be accomplished with anteroposterior radiographs of the knees, wrists, and ankles.[36]
Types
- Vitamin D-related rickets[37]
- Vitamin D deficiency
- Vitamin D-dependent rickets[37]
- Type 1 (25-Hydroxyvitamin D3 1-alpha-hydroxylase deficiency)
- Type 2 (calcitriol receptor mutation)
- Hypocalcemia-related rickets
- Hypocalcemia
- Chronic kidney failure (CKD-BMD)
- Hypophosphatemia-related rickets
- Congenital
- Vitamin D-resistant rickets[37]
- Autosomal dominant hypophosphatemic rickets (ADHR)
- Autosomal recessive hypophosphatemic rickets (ARHR)[38]
- Hypophosphatemia (typically secondary to malabsorption)
- Fanconi's syndrome
- Congenital
- Secondary to other diseases
- Tumor-induced osteomalacia
- McCune-Albright syndrome
- Epidermal nevus syndrome
- Dent's disease
Differential diagnosis
Osteochondrodysplasias also known as genetic bone diseases may mimic the clinical picture of rickets in regard to the features of bone deformities.[39] The radiologic picture and the laboratory findings of serum calcium, phosphate and alkaline phosphatase, are important differentiating factors. Blount's disease is an important differential diagnosis because it causes knee defomities in a similar fashion to rickets namely bow legs or genu varum. Infants with rickets can have bone fractures. This sometimes leads to child abuse allegations. This issue appears to be more common for solely nursing infants of black mothers, in winter in temperate climates, suffering poor nutrition and no vitamin D supplementation.[40] People with darker skin produce less vitamin D than those with lighter skin, for the same amount of sunlight.[41]
Treatment

The most common treatment of rickets is the use of vitamin D.[42] However, orthopedic surgery is occasionally needed.[7]
Diet and sunlight
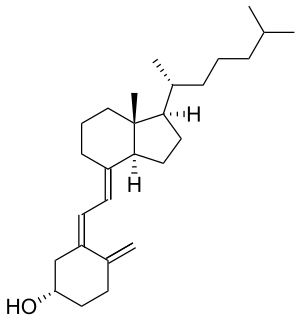
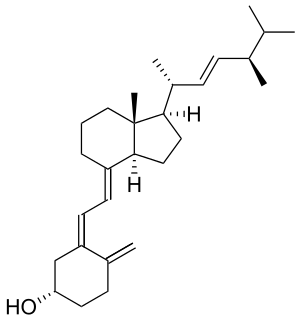
Treatment involves increasing dietary intake of calcium, phosphates and vitamin D. Exposure to ultraviolet B light (most easily obtained when the sun is highest in the sky), cod liver oil, halibut-liver oil, and viosterol are all sources of vitamin D.
A sufficient amount of ultraviolet B light in sunlight each day and adequate supplies of calcium and phosphorus in the diet can prevent rickets. Darker-skinned people need to be exposed longer to the ultraviolet rays. The replacement of vitamin D has been proven to correct rickets using these methods of ultraviolet light therapy and medicine.[43]
Recommendations are for 400 international units (IU) of vitamin D a day for infants and children. Children who do not get adequate amounts of vitamin D are at increased risk of rickets. Vitamin D is essential for allowing the body to uptake calcium for use in proper bone calcification and maintenance.
Supplementation
Sufficient vitamin D levels can also be achieved through dietary supplementation and/or exposure to sunlight. Vitamin D3 (cholecalciferol) is the preferred form since it is more readily absorbed than vitamin D2. Most dermatologists recommend vitamin D supplementation as an alternative to unprotected ultraviolet exposure due to the increased risk of skin cancer associated with sun exposure. Endogenous production with full body exposure to sunlight is approximately 250 µg (10,000 IU) per day.[44]
According to the American Academy of Pediatrics (AAP), all infants, including those who are exclusively breast-fed, may need vitamin D supplementation until they start drinking at least 17 US fluid ounces (500 ml) of vitamin D-fortified milk or formula a day.[45]
Surgery
Occasionally surgery is need to correct severe and persistent deformities of the lower limbs, especially around the knees namely genu varum and genu valgum. Surgical correction of rachitic deformities can be achieved through osteotomies or guided growth surgery. Guided growth surgery has almost replaced the use of corrective osteotomies. The functional results of guided growth surgery in children with rickets are satisfactory. While bone osteotomies work through acute/immediate correction of the limb deformity, guided growth works through gradual correction.[7]
Epidemiology
In developed countries, rickets is a rare disease[46] (incidence of less than 1 in 200,000). Recently, cases of rickets have been reported among children who are not fed enough vitamin D.[47]
In 2013/2014 there were fewer than 700 cases in England.[48] In 2019 the number of cases hospitalised was said to be the highest in 50 years.[49]
Rickets occurs relatively commonly in the Middle East, Africa, and Asia.[4]
History

Greek physician Soranus of Ephesus, one of the chief representatives of the Methodic school of medicine who practiced in Alexandria and subsequently in Rome, reported deformation of the bones in infants as early as the first and second centuries AD. Rickets was not defined as a specific medical condition until 1645, when an English physician Daniel Whistler gave the earliest known description of the disease. In 1650 a treatise on rickets was published by Francis Glisson, a physician at Caius College, Cambridge,[50] who said it had first appeared about 30 years previously in the counties of Dorset and Somerset.[51] In 1857, John Snow suggested rickets, then widespread in Britain, was being caused by the adulteration of bakers' bread with alum.[52] German pediatrician Kurt Huldschinsky successfully demonstrated in the winter of 1918–1919 how rickets could be treated with ultraviolet lamps. The role of diet in the development of rickets[53][54] was determined by Edward Mellanby between 1918–1920.[55] In 1923, American physician Harry Steenbock demonstrated that irradiation by ultraviolet light increased the vitamin D content of foods and other organic materials. Steenbock's irradiation technique was used for foodstuffs, but most memorably for milk. By 1945, rickets had all but been eliminated in the United States.
Etymology
The word rickets may be from the Old English word wrickken ('to twist'), although because this is conjectured, several major dictionaries simply say "origin unknown". The name rickets is plural in form but usually singular in construction. The Greek word "rachitis" (ῥαχίτης,[56] meaning "in or of the spine") was later adopted as the scientific term for rickets, due chiefly to the words' similarity in sound.
See also
References
- 1 2 3 4 5 6 7 8 9 10 11 12 13 "Rickets". Genetic and Rare Diseases Information Center (GARD) – an NCATS Program. 2013. Archived from the original on 22 December 2017. Retrieved 19 December 2017.
- 1 2 3 4 5 6 7 8 9 10 11 12 "Rickets, Vitamin D Deficiency". NORD (National Organization for Rare Disorders). 2005. Archived from the original on 4 October 2017. Retrieved 19 December 2017.
- ↑ Chanchlani, Rahul; Nemer, Paul; Sinha, Rajiv; Nemer, Lena; Krishnappa, Vinod; Sochett, Etienne; Safadi, Fayez; Raina, Rupesh (11 April 2020). "An Overview of Rickets in Children". Kidney International Reports. 5 (7): 980–990. doi:10.1016/j.ekir.2020.03.025. ISSN 2468-0249. PMID 32647755. Archived from the original on 15 December 2021. Retrieved 12 December 2021.
- 1 2 3 4 5 6 7 Creo, AL; Thacher, TD; Pettifor, JM; Strand, MA; Fischer, PR (May 2017). "Nutritional rickets around the world: an update". Paediatrics and International Child Health. 37 (2): 84–98. doi:10.1080/20469047.2016.1248170. PMID 27922335.
- 1 2 3 4 5 "Rickets - OrthoInfo - AAOS". September 2010. Archived from the original on 22 December 2017. Retrieved 19 December 2017.
- ↑ Conway, Richard (2020). "19. Bone disease". In Feather, Adam; Randall, David; Waterhouse, Mona (eds.). Kumar and Clark's Clinical Medicine (10th ed.). Elsevier. pp. 483–484. ISBN 978-0-7020-7870-5. Archived from the original on 12 December 2021. Retrieved 12 December 2021.
- 1 2 3 EL-Sobky, TA; Samir, S; Baraka, MM; Fayyad, TA; Mahran, MA; Aly, AS; Amen, J; Mahmoud, S (1 January 2020). "Growth modulation for knee coronal plane deformities in children with nutritional rickets: A prospective series with treatment algorithm". JAAOS: Global Research and Reviews. 4 (1). doi:10.5435/JAAOSGlobal-D-19-00009.
- 1 2 3 Rajakumar, K (August 2003). "Vitamin D, cod-liver oil, sunlight, and rickets: a historical perspective". Pediatrics. 112 (2): e132–5. doi:10.1542/peds.112.2.e132. PMID 12897318.
- ↑ Brown, Mark (19 August 2018). "Evidence in the bones reveals rickets in Roman times". the Guardian. Archived from the original on 1 January 2019. Retrieved 20 August 2018.
- 1 2 3 4 "Medical News – Symptoms of Rickets". Archived from the original on 14 August 2012. Retrieved 4 June 2012.
- ↑ Harvey, Nicholas C.; Holroyd, Christopher; Ntani, Georgia; Javaid, Kassim; Cooper, Philip; Moon, Rebecca; Cole, Zoe; Tinati, Tannaze; Godfrey, Keith; Dennison, Elaine; Bishop, Nicholas J.; Baird, Janis; Cooper, Cyrus (2014). "Vitamin D supplementation in pregnancy: a systematic review". Health Technology Assessment (Winchester, England). 18 (45): 1–190. doi:10.3310/hta18450. ISSN 2046-4924. PMC 4124722. PMID 25025896. Archived from the original on 24 January 2020. Retrieved 29 June 2017.
- ↑ Prentice, Ann (July 2013). "Nutritional rickets around the world". The Journal of Steroid Biochemistry and Molecular Biology. 136: 201–206. doi:10.1016/j.jsbmb.2012.11.018. PMID 23220549.
- ↑ "Mayo Clinic – Signs and Symptoms of Rickets". Archived from the original on 23 June 2012. Retrieved 4 June 2012.
- ↑ "caput quadratum". TheFreeDictionary.com. Archived from the original on 21 August 2017. Retrieved 21 August 2017.
- ↑ Pharmacologyonline. "Rickets and its Management: A Review" (PDF). Archived (PDF) from the original on 29 May 2015. Retrieved 2 June 2012.
- 1 2 Elidrissy AT (2016). "The Return of Congenital Rickets, Are We Missing Occult Cases?". Calcif Tissue Int (Review). 99 (3): 227–36. doi:10.1007/s00223-016-0146-2. PMID 27245342.
- 1 2 Paterson CR, Ayoub D (2015). "Congenital rickets due to vitamin D deficiency in the mothers". Clin Nutr (Review). 34 (5): 793–8. doi:10.1016/j.clnu.2014.12.006. PMID 25552383.
- ↑ "Office of Dietary Supplements - Vitamin D". Archived from the original on 31 December 2016. Retrieved 8 April 2016.
- ↑ "Pregnancy and prenatal vitamins". Archived from the original on 9 April 2016. Retrieved 8 April 2016.
- ↑ Balasubramanian S, Ganesh R (2008). "Vitamin D deficiency in exclusively breast-fed infants". The Indian Journal of Medical Research (Review). 127 (3): 250–5. PMID 18497439.
- ↑ Pettifor JM (2004). "Nutritional rickets: deficiency of vitamin D, calcium, or both?". The American Journal of Clinical Nutrition (Review). 80 (6 Suppl): 1725S–9S. doi:10.1093/ajcn/80.6.1725S. PMID 15585795.
- ↑ Glorieux FH, Pettifor JM (2014). "Vitamin D/dietary calcium deficiency rickets and pseudo-vitamin D deficiency rickets". BoneKEy Reports (Review). 3: 524. doi:10.1038/bonekey.2014.19. PMC 4015456. PMID 24818008.
- ↑ "Hypophosphatasia: Signs and Symptoms". Hypophosphatasia.com. Archived from the original on 15 October 2014. Retrieved 10 September 2014.
- ↑ Pors Nielsen, S. (2004). "The biological role of strontium". Bone. 35 (3): 583–588. doi:10.1016/j.bone.2004.04.026. PMID 15336592.
- ↑ Daily Telegraph, page 4, Wednesday 19 January 2011
- ↑ Rise in rickets linked to ethnic groups that shun the sun Archived 11 September 2017 at the Wayback Machine The Independent, published 2011-07-25, accessed 2011-07-251
- ↑ Doctors fear rickets resurgence Archived 10 February 2009 at the Wayback Machine BBC, published 2007-12-28, accessed 2011-07-25
- ↑ Loomis, W.G. (August 1967). "Skin-pigment regulation of vitamin-D biosynthesis in man". Science. 157 (3788): 501–6. doi:10.1126/science.157.3788.501. PMID 6028915.
- ↑ Barr, Sharma; Macdonald H.M., Sheehy T., Novotny R., Corriveau A. (August 2011). "Vitamin D deficiency and disease risk among aboriginal Arctic populations". Nutritional Review. 69 (8): 468–478. doi:10.1111/j.1753-4887.2011.00406.x. PMID 21790613.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Bachrach, S.; Fisher J., Parks J.S. (1979). "An outbreak of vitamin D deficiency rickets in a susceptible population". Pediatrics Volume. 64 (6): 871–877.
- ↑ Mithal, A.; Wahl D.A., Bonjour J.P., Burckhardt T., Dawson-Hughes B., Eisman J.A., El-Hajj Fuleihan G., Josse R.G., Lips P., Morales-Torres J. (19 June 2009). "Global vitamin D status and determinants of hypovitaminosis D" (PDF). Osteoporosis International. 20 (11): 1807–1820. doi:10.1007/s00198-009-0954-6. PMID 19543765.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ THE MIDDLE EAST & AFRICA REGIONAL AUDIT, Executive Summary, Epidemiology, costs & burden of osteoporosis in 2011 Archived 25 August 2017 at the Wayback Machine, The International Osteoporosis Foundation, www.iofbonehealth.org, retrieved 6 April 2017
- ↑ Lerch, C; Meissner, T (17 October 2007). "Interventions for the prevention of nutritional rickets in term born children". The Cochrane Database of Systematic Reviews (4): CD006164. doi:10.1002/14651858.CD006164.pub2. PMID 17943890.
- ↑ Weisberg, P.; Scanlon K.S., Ruowei L., Cogswell M.E. (2004). "Nutritional rickets among children in the United States: review of cases reported between 1986 and 2003". The American Journal of Clinical Nutrition. 80 (6): 1697S–1705S. doi:10.1093/ajcn/80.6.1697S. PMID 15585790.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - 1 2 "NHS Choice - Rickets Diagnoses". Archived from the original on 19 June 2012. Retrieved 4 June 2012.
- 1 2 Cheema, Jugesh I.; Grissom, Leslie E.; Harcke, H. Theodore (2003). "Radiographic Characteristics of Lower-Extremity Bowing in Children". RadioGraphics. 23 (4): 871–880. doi:10.1148/rg.234025149. ISSN 0271-5333. PMID 12853662.
- 1 2 3 "Rickets: Not a Disease of the Past". Archived from the original on 9 April 2012. Retrieved 4 June 2012.
- ↑ Levy-Litan V, Hershkovitz E, Avizov L, Leventhal N, Bercovich D, Chalifa-Caspi V, Manor E, Buriakovsky S, Hadad Y, Goding J, Parvari R (2010). "Autosomal-recessive hypophosphatemic rickets is associated with an inactivation mutation in the ENPP1 gene". Am J Hum Genet. 86 (2): 273–8. doi:10.1016/j.ajhg.2010.01.010. PMC 2820183. PMID 20137772.
- ↑ EL-Sobky, TA; Shawky, RM; Sakr, HM; Elsayed, SM; Elsayed, NS; Ragheb, SG; Gamal, R (15 November 2017). "A systematized approach to radiographic assessment of commonly seen genetic bone diseases in children: A pictorial review". J Musculoskelet Surg Res. 1 (2): 25. doi:10.4103/jmsr.jmsr_28_17.
- ↑ Keller, Kathy A.; Barnes, Patrick D. (22 September 2008). "Rickets vs. abuse: a national and international epidemic" (PDF). Pediatric Radiology. 38 (11): 1210–1216. doi:10.1007/s00247-008-1001-z. PMID 18810424. Archived from the original (PDF) on 5 July 2015. Retrieved 31 January 2012.
- ↑ Live Strong. "CDark Skin Color & Vitamin D". Archived from the original on 30 May 2012. Retrieved 2 June 2012.
- ↑ Meschino Health. "Complete Guide to Vitamin D". Archived from the original on 26 February 2014. Retrieved 2 June 2012.
- ↑ Rajakumar, Kumaravel (1 August 2003). "Vitamin D, Cod-Liver Oil, Sunlight, and Rickets: A Historical Perspective". Pediatrics. 112 (2): e132–e135. doi:10.1542/peds.112.2.e132. PMID 12897318. Archived from the original on 19 December 2011. Retrieved 14 July 2011.
- ↑ Vieth R (May 1999). "Vitamin D supplementation, 25-hydroxyvitamin D concentrations, and safety". The American Journal of Clinical Nutrition. 69 (5): 842–56. doi:10.1093/ajcn/69.5.842. PMID 10232622.
- ↑ Gartner LM, Greer FR (April 2003). "Prevention of rickets and vitamin D deficiency: new guidelines for vitamin D intake". Pediatrics. 111 (4 Pt 1): 908–10. doi:10.1542/peds.111.4.908. PMID 12671133. Archived from the original on 3 August 2009. Retrieved 13 December 2007.
- ↑ National Health Service of England > Rickets Archived 11 October 2017 at the Wayback Machine Last reviewed: 28 January 2010
- ↑ "Children who drink non-cow's milk are twice as likely to have low vitamin D". Archived from the original on 27 April 2021. Retrieved 14 March 2022.
- ↑ "Rickets and osteomalacia". nhs.uk. Archived from the original on 11 October 2017. Retrieved 24 December 2017.
- ↑ "How going hungry affects children for their whole lives". Independent. 17 May 2019. Archived from the original on 4 June 2019. Retrieved 4 June 2019.
- ↑ Claerr, Jennifer (6 February 2008). "The History of Rickets, Scurvy and Other Nutritional Deficiencies". An Interesting Treatise on Human Stupidity. Yahoo! Voices. Archived from the original on 2 July 2014.
URL references
- ↑ Gibbs D (1994). "Rickets and the crippled child: an historical perspective". Journal of the Royal Society of Medicine. 87 (12): 729–32. PMC 1294978. PMID 7503834.
- ↑ Dunnigan M (2003). "Commentary: John Snow and alum-induced rickets from adulterated London bread: an overlooked contribution to metabolic bone disease". International Journal of Epidemiology. 32 (3): 340–1. doi:10.1093/ije/dyg160. PMID 12777415.
- ↑ Pileggi VJ, De Luca HF, Steenbock H (September 1955). "The role of vitamin D and intestinal phytase in the prevention of rickets in rats on cereal diets". Archives of Biochemistry and Biophysics. 58 (1): 194–204. doi:10.1016/0003-9861(55)90106-5. PMID 13259690.
- ↑ Ford JA, Colhoun EM, McIntosh WB, Dunnigan MG (1972). "Biochemical Response of Late Rickets and Osteomalacia to a Chupatty-free Diet". British Medical Journal. 3 (5824): 446–7. doi:10.1136/bmj.3.5824.446. PMC 1786011. PMID 5069221.
- ↑ Rajakumar K (2003). "Vitamin D, cod-liver oil, sunlight, and rickets: a historical perspective" (PDF). Pediatrics. 112 (2): e132–5. doi:10.1542/peds.112.2.e132. PMID 12897318. Archived from the original (PDF) on 8 August 2017. Retrieved 25 October 2017.
- ↑ "Greek Word Study Tool". Archived from the original on 7 November 2013. Retrieved 29 April 2012.
External links
| Classification | |
|---|---|
| External resources |