Eclampsia
Eclampsia is the onset of seizures (convulsions) in a woman with pre-eclampsia.[1] Pre-eclampsia is one of the hypertensive disorders of pregnancy that presents with three main features: new onset of high blood pressure, large amounts of protein in the urine or other organ dysfunction, and edema.[7][8][9] The diagnostic criteria for pre-eclampsia is high blood pressure occurring after 20 weeks gestation or during the second half of pregnancy.[1] Most often it occurs during the 3rd trimester of pregnancy and may occur before, during, or after delivery.[1] The seizures are of the tonic–clonic type and typically last about a minute.[1] Following the seizure, there is either a period of confusion or coma.[1] Other complications include aspiration pneumonia, cerebral hemorrhage, kidney failure, pulmonary edema, HELLP syndrome, coagulopathy, placental abruption and cardiac arrest.[1]
| Eclampsia | |
|---|---|
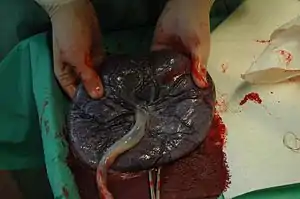 | |
| A gross anatomy image of a placenta that has been cut after delivery | |
| Specialty | Obstetrics |
| Symptoms | Seizures, high blood pressure[1] |
| Complications | Aspiration pneumonia, cerebral hemorrhage, kidney failure, cardiac arrest[1] |
| Usual onset | After 20 weeks of pregnancy[1] |
| Risk factors | Pre-eclampsia[1] |
| Prevention | Aspirin, calcium supplementation, treatment of prior hypertension[2][3] |
| Treatment | Magnesium sulfate, hydralazine, emergency delivery[1][4] |
| Prognosis | 1% risk of death[1] |
| Frequency | 1.4% of deliveries[5] |
| Deaths | 46,900 hypertensive diseases of pregnancy (2015)[6] |
Low dose aspirin is recommended to prevent pre-eclampsia and eclampsia in those at high risk. Other preventative recommendation include calcium supplementation in areas with low calcium intake and treatment of prior hypertension with anti-hypertensive medications.[2][3] Exercise during pregnancy may also be useful.[1] The use of intravenous or intramuscular magnesium sulfate improves outcomes in those with severe pre-eclampsia and eclampsia and is generally safe.[4][10] Treatment options include blood pressure medications such as hydralazine and emergency delivery of the baby either vaginally or by cesarean section.[1]
Pre-eclampsia is estimated to globally affect about 5% of deliveries while eclampsia affects about 1.4% of deliveries.[5] In the developed world eclampsia rates are about 1 in 2,000 deliveries due to improved medical care whereas in developing countries it can impact 10-30 times as many women.[1][11] Hypertensive disorders of pregnancy are one of the most common causes of death in pregnancy.[11] They resulted in 46,900 deaths in 2015.[6] Around one percent of women with eclampsia die.[1] The word eclampsia is from the Greek term for lightning.[12] The first known description of the condition was by Hippocrates in the 5th century BC.[12]
Signs and symptoms

Eclampsia is a disorder of pregnancy characterized by seizures in the setting of pre-eclampsia.[13] Most women have premonitory signs/symptoms in the hours before the initial seizure. Typically the woman develops hypertension before the onset of a convulsion (seizure).[14] Other signs and symptoms to looks out for include:[15]
- Long-lasting (persistent) frontal or occipital headaches or thunderclap headaches) [16]
- Visual disturbance (blurred vision, photophobia, diplopopia)
- Photophobia (i.e. bright light causes discomfort)
- Abdominal pain
- Either in the epigastric region (the center of the abdomen above the navel, or belly-button)
- And/or in the right upper quadrant of the abdomen (below the right side of the rib cage)
- Altered mental status (confusion)
Any of these symptoms may be present before or after the seizure.[17] It is also possible for the woman to be asymptomatic prior to the onset of the seizure.
Other cerebral signs that may precede the convulsion include nausea, vomiting, headaches, and cortical blindness. If the complication of multi-organ failure ensues, signs and symptoms of those failing organs will appear, such as abdominal pain, jaundice, shortness of breath, and diminished urine output.
Onset
The seizures of eclampsia typically present during pregnancy and prior to delivery (the antepartum period),[18] but may also occur during labor and delivery (the intrapartum period) or after the baby has been delivered (the postpartum period).[13][17][19] If postpartum seizures develop, it is most likely to occur within the first 48 hours after delivery. However, late postpartum seizures of eclampsia may occur as late as 4 weeks after delivery.[13][17]
Characteristics
Eclamptic seizure is typically described as a tonic–clonic seizure which may cause an abrupt loss of consciousness at onset.[20] This is often associated with a shriek or scream followed by stiffness of the muscles of the arms, legs, back and chest. During the tonic phase, the mother may begin to appear cyanotic. This presentation lasts for about a minute, after which the muscles begin in jerk and twitch for an additional one to two minutes.[21] Other signs include tongue biting, frothy and bloody sputum coming out of the mouth.[22]
Complications
There are risks to both the mother and the fetus when eclampsia occurs. The fetus may grow more slowly than normal within the womb (uterus) of a woman with eclampsia, which is termed intrauterine growth restriction and may result in the child appearing small for gestational age or being born with low birth weight.[23] Eclampsia may also cause problems with the placenta. The placenta may bleed (hemorrhage) or begin to separate early from the wall of the uterus.[24] It is normal for the placenta to separate from the uterine wall during delivery, but it is abnormal for it to separate prior to delivery; this condition is called placental abruption and can be dangerous for the fetus.[25] Placental insufficiency may also occur, a state in which the placenta fails to support appropriate fetal development because it cannot deliver the necessary amount of oxygen or nutrients to the fetus.[24] During an eclamptic seizure, the beating of the fetal heart may become slower than normal (bradycardia).[23][26] If any of these complications occurs, fetal distress may develop. Treatment of the mother's seizures may also manage fetal bradycardia.[18][27] If the risk to the health of the fetus or the mother is high, the definitive treatment for eclampsia is delivery of the baby. Delivery by cesarean section may be necessary, especially if the instance of fetal bradycardia does not resolve after 10 to 15 minutes of resuscitative interventions.[18][28] It may be safer to deliver the infant preterm than to wait for the full 40 weeks of fetal development to finish, and as a result prematurity is also a potential complication of eclampsia.[24][29]
In the mother, changes in vision may occur as a result of eclampsia, and these changes may include blurry vision, one-sided blindness (either temporary due to amaurosis fugax or potentially permanent due to retinal detachment), or cortical blindness, which affects the vision from both eyes.[30][31] There are also potential complications in the lungs. The woman may have fluid slowly collecting in the lungs in a process known as pulmonary edema.[24] During an eclamptic seizure, it is possible for a person to vomit the contents of the stomach and to inhale some of this material in a process known as aspiration.[23] If aspiration occurs, the woman may experience difficulty breathing immediately or could develop an infection in the lungs later, called aspiration pneumonia.[17][32] It is also possible that during a seizure breathing will stop temporarily or become inefficient, and the amount of oxygen reaching the woman's body and brain will be decreased (in a state known as hypoxia).[17][33] If it becomes difficult for the woman to breathe, she may need to have her breathing temporarily supported by an assistive device in a process called mechanical ventilation. In some severe eclampsia cases, the mother may become weak and sluggish (lethargy) or even comatose.[31] These may be signs that the brain is swelling (cerebral edema) or bleeding (intracerebral hemorrhage).[24][31]
Risk factors
Eclampsia, like pre-eclampsia, tends to occur more commonly in first pregnancies than subsequent pregnancies.[34][35][36] Women who have long term high blood pressure before becoming pregnant have a greater risk of pre-eclampsia.[34][35] Patients who have gestational hypertension and pre-eclampsia have an increased risk of eclampsia.[37] Furthermore, women with other pre-existing vascular diseases (diabetes or nephropathy) or thrombophilia disease such as the antiphospholipid syndrome are at higher risk to develop pre-eclampsia and eclampsia.[34][35] Having a placenta that is enlarged by multiple gestation or hydatidiform mole also increases risk of eclampsia.[34][35][38] In addition, there is a genetic component: a woman whose mother or sister had the condition is at higher risk than otherwise.[39] Patients who have experienced eclampsia are at increased risk for pre-eclampsia/eclampsia in a later pregnancy.[35] The occurrence of pre-eclampsia was 5% in white, 9% in Hispanic, and 11% in African American patients and this may reflect disproportionate risk of developing pre-eclampsia among ethnic groups.[40] Additionally, black patients were also shown to have a disproportionately higher risk of dying from eclampsia.[40]
Mechanism
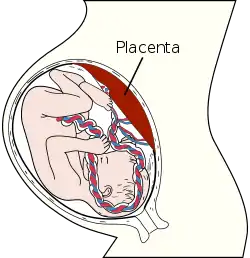
The mechanisms of eclampsia and preeclampsia are not definitively understood, but following provides some insight. The presence of a placenta is required, and eclampsia resolves if it is removed.[41] Reduced blood flow to the placenta (placental hypoperfusion) may be a key feature of the process. It is typically accompanied by increased sensitivity of the maternal vasculature to agents which cause constriction of the small arteries, leading to reduced blood flow to multiple organs. Vascular dysfunction-associated maternal conditions such as Lupus, hypertension, and renal disease, or obstetric conditions that increase placental volume without an increase in placental blood flow (such as multifetal gestation) may increase risk for pre-eclampsia.[42] Also, activation of the coagulation cascade can lead to microthrombi formation, which may further impair blood flow. Thirdly, increased vascular permeability results in the shift of extracellular fluid from the blood to the interstitial space which reduces blood flow and causes edema. These events can lead to hypertension, renal dysfunction, pulmonary dysfunction, hepatic dysfunction, and cerebral edema with cerebral dysfunction and convulsions.[41] In clinical context, increased platelet and endothelial activation may be detected before symptoms appear.[41]
Hypoperfusion of the placenta is associated with abnormal modelling of the fetal–maternal placental interface that may be immunologically mediated.[41] The pathogenesis of pre-eclampsia is poorly understood and may be attributed to factors related to the woman and placenta since pre-eclampsia is seen in molar pregnancies absent of a fetus or fetal tissue.[42] The placenta normally produces the potent vasodilator adrenomedullin but it is reduced in pre-eclampsia and eclampsia.[43] Other vasodilators, including prostacyclin, thromboxane A2, nitric oxide, and endothelins, are reduced in eclampsia and may lead to vasoconstriction.[26]
Eclampsia is associated with hypertensive encephalopathy in which cerebral vascular resistance is reduced, leading to increased blood flow to the brain, cerebral edema and resultant convulsions.[44] An eclamptic convulsion usually does not cause chronic brain damage unless intracranial haemorrhage occurs.[45]
Diagnosis
If a pregnant woman has already been diagnosed with pre-eclampsia during the current pregnancy and then develops a seizure, she may be assigned a 'clinical diagnosis' of eclampsia without further workup. While seizures are most common in the third trimester, they may occur any time from 20 weeks of pregnancy until 6 weeks after birth.[46] Because pre-eclampsia and eclampsia are common conditions in women, eclampsia can be assumed to be the correct diagnosis until proven otherwise in pregnant or postpartum women who experience seizures.[47] However, if a woman has a seizure and it is unknown whether or not they have pre-eclampsia, testing can help make the diagnosis clear.
Pre-eclampsia is diagnosed when repeated blood pressure measurements are greater or equal to 140/90mmHg, in addition to any signs of organ dysfunction, including: proteinuria, thrombocytopenia, renal insufficiency, impaired liver function, pulmonary edema, cerebral symptoms, or abdominal pain.[48]
Vital signs
One of the core features of pre-eclampsia is the new onset of high blood pressure. Blood pressure is a measurement of two numbers: systolic blood pressure and diastolic blood pressure. A systolic blood pressure (the top number) of greater than 140 mmHg and/or a diastolic blood pressure (the bottom number) of greater than 90 mmHg is higher than the normal range. If the blood pressure is high on at least two separate occasions after the first 20 weeks of pregnancy and the woman has signs of organ dysfunction (e.g. proteinuria), then they meet the criteria for a diagnosis of pre-eclampsia.[29] If the systolic blood pressure is greater than 160 or the diastolic pressure is greater than 110, the hypertension is considered to be severe.[13]
Laboratory testing
Another common feature of pre-eclampsia is proteinuria, which is the presence of excess protein in the urine. To determine if proteinuria is present, the urine can be collected and tested for protein; if there is 0.3 grams of protein or more in the urine of a pregnant woman collected over 24 hours, this is one of the diagnostic criteria for pre-eclampsia and raises the suspicion that a seizure is due to eclampsia.[13]
In cases of severe eclampsia or pre-eclampsia, the woman can have low levels of platelets in the blood, a condition termed thrombocytopenia.[49][26] A complete blood count, or CBC, is a test of the blood that can be performed to check platelet levels.
Other investigations include: kidney function test, liver function tests (LFT), coagulation screen, 24-hour urine creatinine, and fetal/placental ultrasound.
Differential diagnosis
Convulsions during pregnancy that are unrelated to pre-eclampsia need to be distinguished from eclampsia. Such disorders include seizure disorders as well as brain tumor, aneurysm of the brain, and medication- or drug-related seizures. Usually, the presence of the signs of severe pre-eclampsia precede and accompany eclampsia, facilitating the diagnosis.[32]
Prevention
Detection and management of pre-eclampsia is critical to reduce the risk of eclampsia. The USPSTF recommends regular checking of blood pressure through pregnancy in order to detect preeclampsia.[50] Appropriate management of a woman with pre-eclampsia generally involves the use of magnesium sulfate to prevent eclamptic seizures.[51] In some cases, low-dose aspirin has been shown to decrease the risk of pre-eclampsia in women, especially when taken in the late first trimester.[48]
Treatment
The four goals of the treatment of eclampsia are to stop and prevent further convulsions, to control the elevated blood pressure, to deliver the baby as promptly as possible, and to monitor closely for the onset of multi-organ failure.
Convulsions
Convulsions are prevented and treated using magnesium sulfate.[52] The study demonstrating the effectiveness of magnesium sulfate for the management of eclampsia was first published in 1955.[53] Effective anticonvulsant serum levels range from 2.5 to 7.5 mEq/L.[54]
With intravenous administration, the onset of anticonvulsant action is fast and lasts about 30 minutes. Following intramuscular administration the onset of action is about one hour and lasts for three to four hours. Magnesium is excreted solely by the kidneys at a rate proportional to the plasma concentration (concentration in the blood) and glomerular filtration (rate at which the blood is filtered through the kidneys).[54] Magnesium sulfate is associated with several minor side effects; serious side effects are uncommon, occurring at elevated magnesium serum concentrations greater than 7.0 mEq/L. Serious toxicity can be counteracted with calcium gluconate.[55]
Even with therapeutic serum magnesium concentrations, recurrent convulsions may occur, and additional magnesium may be needed, but with close monitoring for respiratory, cardiac, and neurological depression. If magnesium administration with resultant high serum concentrations fails to control convulsions, the addition of other intravenous anticonvulsants may be used and intubation and mechanical ventilation may be initiated. It is important to avoid magnesium toxicity, including thoracic muscle paralysis, which could cause respiratory failure and death.
Magnesium sulfate results in better outcomes than diazepam, phenytoin or a combination of chlorpromazine, promethazine, and pethidine.[56][57][58]
Blood pressure management
Blood pressure control is used to prevent stroke, which accounts for 15 to 20 percent of deaths in women with eclampsia.[59] The agents of choice for blood pressure control during eclampsia are hydralazine or labetalol.[26] This is because of their effectiveness, lack of negative effects on the fetus, and mechanism of action. Blood pressure management is indicated with a diastolic blood pressure above 105–110 mm Hg.[28]
Delivery
If the baby has not yet been delivered, steps need to be taken to stabilize the woman and deliver her speedily. This needs to be done even if the baby is immature, as the eclamptic condition is unsafe for both baby and mother. As eclampsia is a manifestation of a type of non-infectious multiorgan dysfunction or failure, other organs (liver, kidney, lungs, cardiovascular system, and coagulation system) need to be assessed in preparation for a delivery (often a caesarean section), unless the woman is already in advanced labor. Regional anesthesia for caesarean section is contraindicated when a coagulopathy has developed.
There is limited to no evidence in favor of a particular delivery method for women with eclampsia. Therefore, the delivery method of choice is an individualized decision.[27]
Monitoring
Invasive hemodynamic monitoring may be elected in an eclamptic woman at risk for or with heart disease, kidney disease, refractory hypertension, pulmonary edema, or poor urine output.[26]
Etymology
The Greek noun ἐκλαμψία, 'eklampsía', denotes a "light burst"; metaphorically, in this context, "sudden occurrence." The New Latin term first appeared in Johannes Varandaeus’ 1620 treatise on gynaecology Tractatus de affectibus Renum et Vesicae.[60] The term 'toxemia of pregnancy' is no longer recommended: placental toxins are not the cause of eclampsia occurrences, as previously believed.[61]
Popular culture
- In Downton Abbey, a historical drama television series, the character Lady Sybil dies (in series 3, episode 5) of eclampsia shortly after child birth.[62]
- In Call the Midwife, a medical drama television series set in London in the 1950s and 1960s, the character (in series 1, episode 4) named Margaret Jones is struck with pre-eclampsia, ultimately proceeding from a comatose condition to death. The term "toxemia" was also used for the condition, in the dialogue.[63]
- In House M.D., a medical drama television series set in the U.S., Dr. Cuddy, the hospital director, adopts a baby whose teenage mother dies from eclampsia and had no other parental figures available.[64]
- In The Lemon Drop Kid, the main character's wife dies of eclampsia shortly after giving birth to a boy.
References
- "Chapter 40: Hypertensive Disorders". Williams Obstetrics (24th ed.). McGraw-Hill Professional. 2014. ISBN 9780071798938.
- WHO recommendations for prevention and treatment of pre-eclampsia and eclampsia (PDF). 2011. ISBN 978-92-4-154833-5. Archived (PDF) from the original on 2015-05-13.
- Henderson, JT; Whitlock, EP; O'Connor, E; Senger, CA; Thompson, JH; Rowland, MG (20 May 2014). "Low-dose aspirin for prevention of morbidity and mortality from preeclampsia: a systematic evidence review for the U.S. Preventive Services Task Force". Annals of Internal Medicine. 160 (10): 695–703. doi:10.7326/M13-2844. PMID 24711050. S2CID 33835367.
- Smith, JM; Lowe, RF; Fullerton, J; Currie, SM; Harris, L; Felker-Kantor, E (5 February 2013). "An integrative review of the side effects related to the use of magnesium sulfate for pre-eclampsia and eclampsia management". BMC Pregnancy and Childbirth. 13: 34. doi:10.1186/1471-2393-13-34. PMC 3570392. PMID 23383864.
- Abalos, E; Cuesta, C; Grosso, AL; Chou, D; Say, L (September 2013). "Global and regional estimates of preeclampsia and eclampsia: a systematic review". European Journal of Obstetrics, Gynecology, and Reproductive Biology. 170 (1): 1–7. doi:10.1016/j.ejogrb.2013.05.005. PMID 23746796.
- GBD 2015 Mortality and Causes of Death, Collaborators. (8 October 2016). "Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980-2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet. 388 (10053): 1459–1544. doi:10.1016/s0140-6736(16)31012-1. PMC 5388903. PMID 27733281.
{{cite journal}}:|first1=has generic name (help) - Lambert, G; Brichant, JF; Hartstein, G; Bonhomme, V; Dewandre, PY (2014). "Preeclampsia: an update". Acta Anaesthesiologica Belgica. 65 (4): 137–49. PMID 25622379.
- Brown, Mark A.; Magee, Laura A.; Kenny, Louise C.; Karumanchi, S. Ananth; McCarthy, Fergus P.; Saito, Shigeru; Hall, David R.; Warren, Charlotte E.; Adoyi, Gloria; Ishaku, Salisu (July 2018). "Hypertensive Disorders of Pregnancy: ISSHP Classification, Diagnosis, and Management Recommendations for International Practice". Hypertension. 72 (1): 24–43. doi:10.1161/HYPERTENSIONAHA.117.10803. ISSN 0194-911X. PMID 29899139. S2CID 49184061.
- American College of Obstetricians Gynecologists; Task Force on Hypertension in Pregnancy (November 2013). "Hypertension in pregnancy. Report of the American College of Obstetricians and Gynecologists' Task Force on Hypertension in Pregnancy" (PDF). Obstet. Gynecol. 122 (5): 1122–31. doi:10.1097/01.AOG.0000437382.03963.88. PMC 1126958. PMID 24150027. Archived from the original (PDF) on 2016-01-06. Retrieved 2015-02-22.
- McDonald, SD; Lutsiv, O; Dzaja, N; Duley, L (August 2012). "A systematic review of maternal and infant outcomes following magnesium sulfate for pre-eclampsia/eclampsia in real-world use". International Journal of Gynaecology and Obstetrics. 118 (2): 90–6. doi:10.1016/j.ijgo.2012.01.028. PMID 22703834. S2CID 20361780.
- Arulkumaran, N.; Lightstone, L. (December 2013). "Severe pre-eclampsia and hypertensive crises". Best Practice & Research Clinical Obstetrics & Gynaecology. 27 (6): 877–884. doi:10.1016/j.bpobgyn.2013.07.003. PMID 23962474.
- Emile R. Mohler (2006). Advanced Therapy in Hypertension and Vascular Disease. PMPH-USA. pp. 407–408. ISBN 9781550093186. Archived from the original on 2017-09-10.
- Stone, C. Keith; Humphries, Roger L. (2017). "Chapter 19: Seizures". Current diagnosis & treatment. Emergency medicine (8th ed.). New York: McGraw-Hill. ISBN 9780071840613. OCLC 959876721.
- Kane SC, Dennis A, da Silva Costa F, Kornman L, Brennecke S (2013). "Contemporary Clinical Management of the Cerebral Complications of Preeclampsia". Obstetrics and Gynecology International. 2013: 1–10. doi:10.1155/2013/985606. PMC 3893864. PMID 24489551.
- Berhan, Yifru; Berhan, Asres (June 2015). "Should magnesium sulfate be administered to women with mild pre-eclampsia? A systematic review of published reports on eclampsia: Systematic review of reports on eclampsia". Journal of Obstetrics and Gynaecology Research. 41 (6): 831–842. doi:10.1111/jog.12697. PMID 25833188. S2CID 41573228.
- Zeeman, Gerda G. (June 2009). "Neurologic Complications of Pre-eclampsia". Seminars in Perinatology. 33 (3): 166–172. doi:10.1053/j.semperi.2009.02.003. ISSN 0146-0005. PMID 19464507.
- Gabbe MD, Steven G. (2017). "Chapter 31: Preeclampsia and Hypertensive Disorders". Obstetrics : Normal and Problem Pregnancies. Jennifer R. Niebyl MD, Joe Leigh Simpson MD, Mark B. Landon MD, Henry L. Galan MD, Eric R.M. Jauniaux MD, PhD, Deborah A. Driscoll MD, Vincenzo Berghella MD and William A. Grobman MD, MBA (Seventh ed.). Philadelphia, PA: Elsevier, Inc. pp. 661–705. ISBN 9780323321082. OCLC 951627252.
- Gill, Prabhcharan; Tamirisa, Anita P.; Van Hook MD, James W. (2020), "Acute Eclampsia", StatPearls, StatPearls Publishing, PMID 29083632, retrieved 2019-08-04
- Cunningham, F. Gary (2014). "Chapter 40: Hypertensive Disorders". Williams Obstetrics. Leveno KJ, Bloom SL, Spong CY, Dashe JS, Hoffman BL, Casey BM, Sheffield JS. (24th ed.). New York: McGraw-Hill Education. ISBN 9780071798938. OCLC 871619675.
- Sanders, T G; Clayman, D A; Sanchez-Ramos, L; Vines, F S; Russo, L (August 1991). "Brain in eclampsia: MR imaging with clinical correlation". Radiology. 180 (2): 475–478. doi:10.1148/radiology.180.2.2068315. ISSN 0033-8419. PMID 2068315.
- Spurr, Frederick (June 1900). "Three Cases of Puerperal Eclampsia". The Lancet. 155 (4007): 1717–1719. doi:10.1016/s0140-6736(01)78186-x. ISSN 0140-6736.
- Wichert-Ana, Lauro; Ferruzzi, Emerson Henklain; Alexandre Jr, Veriano; Velasco, Tonicarlo Rodrigues; Bianchin, Marino Muxfeldt; Terra-Bustamante, Vera Cristina; Kato, Mery; Santos, Antonio Carlos; Azevedo-Marques, Paulo Mazzoncini de; Oliveira, Lucas Ferrari de; Sakamoto, Américo Ceiki (December 2006). "Epistaxis during a generalized seizure leading to an atypical ictal SPECT finding at the skull base". Journal of Epilepsy and Clinical Neurophysiology. 12 (4): 225–227. doi:10.1590/s1676-26492006000700007. ISSN 1676-2649.
- Fleisher MD, Lee A. (2018). "Chapter: Eclampsia". Essence of Anesthesia Practice. Roizen, Michael F.,, Roizen, Jeffrey D. (4th ed.). Philadelphia, Pa.: Elsevier Inc. pp. 153–154. ISBN 9780323394970. OCLC 989062320.
- Bersten, Andrew D. (2014). "Chapter 63: Preeclampsia and eclampsia". Oh's Intensive Care Manual. Soni, Neil (Seventh ed.). [Oxford]: Elsevier Ltd. pp. 677–683. ISBN 9780702047626. OCLC 868019515.
- Robert Resnik, MD; Robert k. Creasy, MD; Jay d. Iams, MD; Charles j. Lockwood, MD; Thomas Moore, MD; Michael f Greene, MD (2014). "Chapter 46: Placenta Previa, Placenta Accreta, Abruptio Placentae, and Vasa Previa". Creasy and Resnik's maternal-fetal medicine : principles and practice. Creasy, Robert K.,, Resnik, Robert,, Greene, Michael F.,, Iams, Jay D.,, Lockwood, Charles J. (Seventh ed.). Philadelphia, PA. pp. 732–742. ISBN 9781455711376. OCLC 859526325.
- Acog Committee On Obstetric Practice (January 2002). "ACOG practice bulletin. Diagnosis and management of preeclampsia and eclampsia. Number 33, January 2002". Obstet Gynecol. 99 (1): 159–67. doi:10.1016/s0029-7844(01)01747-1. PMID 16175681.
- ACOG Committee on Obstetric Practice (April 2002). "ACOG practice bulletin. Diagnosis and management of preeclampsia and eclampsia. Number 33, January 2002. American College of Obstetricians and Gynecologists". International Journal of Gynaecology and Obstetrics. 77 (1): 67–75. ISSN 0020-7292. PMID 12094777.
- Sibai, Baha M. (February 2005). "Diagnosis, prevention, and management of eclampsia". Obstetrics and Gynecology. 105 (2): 402–410. doi:10.1097/01.AOG.0000152351.13671.99. ISSN 0029-7844. PMID 15684172.
- "Chapter 35: Hypertension". High risk pregnancy : management options. James, D. K. (David K.), Steer, Philip J. (4th ed.). St. Louis, MO: Saunders/Elsevier. 2011. pp. 599–626. ISBN 9781416059080. OCLC 727346377.
{{cite book}}: CS1 maint: others (link) - Cunningham FG, Fernandez CO, Hernandez C (April 1995). "Blindness associated with preeclampsia and eclampsia". American Journal of Obstetrics and Gynecology. 172 (4 Pt 1): 1291–8. doi:10.1016/0002-9378(95)91495-1. PMID 7726272.
- James, David K. (2011). "Chapter 48: Neurologic Complications of Preeclampsia/Eclampsia". High Risk Pregnancy. Steer, Philip J. (4th ed.). St. Louis, MO: Saunders/Elsevier. pp. 861–891. ISBN 9781416059080. OCLC 727346377.
- Cronenwett, Jack L. (2014). "Chapter 40: Systemic Complications: Respiratory". Rutherford's vascular surgery. Johnston, K. Wayne (Eighth ed.). Philadelphia, PA: Saunders, Elsevier. pp. 626–637. ISBN 9781455753048. OCLC 877732063.
- Adams, James (2013). "Chapter 99: Seizures". Emergency medicine : clinical essentials (2nd ed.). Philadelphia, PA: Elsevier/ Saunders. pp. 857–869. ISBN 9781437735482. OCLC 820203833.
- "Chapter 48: Pregnancy-Related Hypertension". Creasy and Resnik's Maternal-Fetal Medicine : Principles and Practice. Creasy, Robert K.,, Resnik, Robert,, Greene, Michael F.,, Iams, Jay D.,, Lockwood, Charles J. (Seventh ed.). Philadelphia, PA: Saunders, an imprint of Elsevier Inc. 2014. pp. 756–781. ISBN 9781455711376. OCLC 859526325.
{{cite book}}: CS1 maint: others (link) - Gabbe MD, Steven G. (2017). "Chapter 31: Preeclampsia and Hypertensive Disorders". Obstetrics : Normal and Problem Pregnancies. Jennifer R. Niebyl MD, Joe Leigh Simpson MD, Mark B. Landon MD, Henry L. Galan MD, Eric R.M. Jauniaux MD, PhD, Deborah A. Driscoll MD, Vincenzo Berghella MD and William A. Grobman MD, MBA (Seventh ed.). Philadelphia, PA: Elsevier, Inc. pp. 661–705.e3. ISBN 9780323321082. OCLC 951627252.
- Gardner, David G. (2018). "Chapter 16: The Endocrinology of Pregnancy". Greenspan's basic & clinical endocrinology. Shoback, Dolores M.,, Greenspan, Francis S. (Francis Sorrel), 1920-2016. (Tenth ed.). [New York]: McGraw-Hill Education. ISBN 9781259589287. OCLC 995848612.
- American College of Obstetricians and Gynecologists (June 2020). "Gestational Hypertension and Preeclampsia". Obstetrics & Gynecology. 135 (6): e237–e260. doi:10.1097/AOG.0000000000003891. PMID 32443079. S2CID 218856298. Retrieved September 12, 2022.
- Kasper, Dennis L. (2015). "Chapter 117: Gynecologic Malignancies". Harrison's principles of internal medicine. Fauci, Anthony S., 1940-, Hauser, Stephen L.,, Longo, Dan L. (Dan Louis), 1949-, Jameson, J. Larry,, Loscalzo, Joseph (19th ed.). New York: McGraw-Hill Education. ISBN 9780071802154. OCLC 893557976.
- Murray, Michael F. (2014). "Chapter 102: Pre-eclampsia". Clinical genomics : practical applications in adult patient care. Babyatsky, Mark W.,, Giovanni, Monica A.,, Alkuraya, Fowzan S.,, Stewart, Douglas R. (First ed.). New York: McGraw-Hill Education. ISBN 9780071622448. OCLC 899740989.
- Williams obstetrics. Williams, J. Whitridge (John Whitridge), 1866-1931., Cunningham, F. Gary,, Leveno, Kenneth J.,, Bloom, Steven L.,, Spong, Catherine Y.,, Dashe, Jodi S. (25th ed.). New York. 12 April 2018. ISBN 978-1-259-64432-0. OCLC 958829269.
{{cite book}}: CS1 maint: others (link) - Roberts JM, Cooper DW (January 2001). "Pathogenesis and genetics of pre-eclampsia". Lancet. 357 (9249): 53–6. doi:10.1016/S0140-6736(00)03577-7. PMID 11197372. S2CID 25280817.
- Greenspan's basic & clinical endocrinology. Gardner, David G.,, Shoback, Dolores M.,, Greenspan, Francis S., 1920- (Francis Sorrel) (10th ed.). New York, N.Y. 10 October 2017. ISBN 9781259589287. OCLC 1075522289.
{{cite book}}: CS1 maint: others (link) - Li H, Dakour J, Kaufman S, Guilbert LJ, Winkler-Lowen B, Morrish DW (November 2003). "Adrenomedullin is decreased in preeclampsia because of failed response to epidermal growth factor and impaired syncytialization". Hypertension. 42 (5): 895–900. doi:10.1161/01.HYP.0000095613.41961.6E. PMID 14517225.
- Cipolla MJ (July 2007). "Cerebrovascular function in pregnancy and eclampsia". Hypertension. 50 (1): 14–24. doi:10.1161/HYPERTENSIONAHA.106.079442. PMID 17548723.
- Richards A, Graham D, Bullock R (March 1988). "Clinicopathological study of neurological complications due to hypertensive disorders of pregnancy". J. Neurol. Neurosurg. Psychiatry. 51 (3): 416–21. doi:10.1136/jnnp.51.3.416. PMC 1032870. PMID 3361333.
- Current medical diagnosis & treatment 2021. Papadakis, Maxine A.,, McPhee, Stephen J.,, Rabow, Michael W. (Sixtieth ed.). New York. 10 September 2020. ISBN 978-1-260-46986-8. OCLC 1191849672.
{{cite book}}: CS1 maint: others (link) - Edlow, Jonathan A.; Caplan, Louis R.; O'Brien, Karen; Tibbles, Carrie D. (February 2013). "Diagnosis of acute neurological emergencies in pregnant and post-partum women". The Lancet. Neurology. 12 (2): 175–185. doi:10.1016/S1474-4422(12)70306-X. ISSN 1474-4465. PMID 23332362. S2CID 17711531.
- Current diagnosis & treatment : obstetrics & gynecology. DeCherney, Alan H.,, McGraw-Hill Companies. (12th ed.). [New York]. 12 February 2019. ISBN 978-0071833905. OCLC 1080940730.
{{cite book}}: CS1 maint: others (link) - Tintinalli, Judith E. (2016). "Chapter 100: Maternal Emergencies After 20 Weeks of Pregnancy and in the Postpartum Period". Tintinalli's Emergency Medicine : A Comprehensive Study Guide. Stapczynski, J. Stephan,, Ma, O. John,, Yealy, Donald M.,, Meckler, Garth D.,, Cline, David, 1956- (Eighth ed.). New York: McGraw-Hill Education. ISBN 9780071794763. OCLC 915775025.
- Sperling, Jeffrey D.; Gossett, Dana R. (25 April 2017). "Screening for Preeclampsia and the USPSTF Recommendations". JAMA. 317 (16): 1629–1630. doi:10.1001/jama.2017.2018. PMID 28444259.
- Harrison's principles of internal medicine. Jameson, J. Larry,, Kasper, Dennis L.,, Longo, Dan L. (Dan Louis), 1949-, Fauci, Anthony S., 1940-, Hauser, Stephen L.,, Loscalzo, Joseph (20th ed.). New York. 13 August 2018. ISBN 978-1-259-64403-0. OCLC 1029074059.
{{cite book}}: CS1 maint: others (link) - Patel, Minal K.; Goodson, James L.; Alexander, James P.; Kretsinger, Katrina; Sodha, Samir V.; Steulet, Claudia; Gacic-Dobo, Marta; Rota, Paul A.; McFarland, Jeffrey; Menning, Lisa; Mulders, Mick N. (2020-11-13). "Progress Toward Regional Measles Elimination — Worldwide, 2000–2019". MMWR. Morbidity and Mortality Weekly Report. 69 (45): 1700–1705. doi:10.15585/mmwr.mm6945a6. ISSN 0149-2195. PMC 7660667. PMID 33180759.
- Pritchard JA (February 1955). "The use of the magnesium ion in the management of eclamptogenic toxemias". Surg Gynecol Obstet. 100 (2): 131–40. PMID 13238166.
- "Magnesium Sulfate - FDA prescribing information, side effects and uses". Drugs.com. Retrieved 2020-12-07.
- Smith, Jeffrey Michael; Lowe, Richard F.; Fullerton, Judith; Currie, Sheena M.; Harris, Laura; Felker-Kantor, Erica (2013-02-05). "An integrative review of the side effects related to the use of magnesium sulfate for pre-eclampsia and eclampsia management". BMC Pregnancy and Childbirth. 13 (1): 34. doi:10.1186/1471-2393-13-34. ISSN 1471-2393. PMC 3570392. PMID 23383864.
- Duley, L; Henderson-Smart, DJ; Walker, GJ; Chou, D (Dec 8, 2010). "Magnesium sulphate versus diazepam for eclampsia". The Cochrane Database of Systematic Reviews (12): CD000127. doi:10.1002/14651858.CD000127.pub2. PMC 7045443. PMID 21154341.
- Duley, L; Henderson-Smart, DJ; Chou, D (Oct 6, 2010). "Magnesium sulphate versus phenytoin for eclampsia". The Cochrane Database of Systematic Reviews (10): CD000128. doi:10.1002/14651858.CD000128.pub2. PMID 20927719.
- Duley, L; Gülmezoglu, AM; Chou, D (Sep 8, 2010). "Magnesium sulphate versus lytic cocktail for eclampsia". The Cochrane Database of Systematic Reviews (9): CD002960. doi:10.1002/14651858.CD002960.pub2. PMC 7138041. PMID 20824833.
- Townsend, Rosemary; O’Brien, Patrick; Khalil, Asma (2016-07-27). "Current best practice in the management of hypertensive disorders in pregnancy". Integrated Blood Pressure Control. 9: 79–94. doi:10.2147/IBPC.S77344. ISSN 1178-7104. PMC 4968992. PMID 27555797.
- Ong, S. (2003). "Pre-eclampsia: A historical perspective". In Baker, P.N.; Kingdom, J.C.P. (eds.). Pr-eclampsia: Current perspectives on management. Taylor & Francis. pp. 15–24. ISBN 978-1842141809.
- FAQ: Toxemia Archived 2015-09-25 at the Wayback Machine at the Pre-Eclampsia Foundation website
- Stone, Rachel Marie (January 30, 2013). "Stop With All the Dangerous Childbirth Stories Already". Christianity Today. Archived from the original on March 11, 2016. Retrieved March 11, 2016.
- "Episode #1.4". 5 February 2012. Archived from the original on 10 September 2017. Retrieved 4 September 2016 – via IMDb.
- "House" Joy to the World (TV Episode 2008) - IMDb, retrieved 2021-10-02
External links
- Eclampsia at Curlie