Iodine in biology
Iodine is an essential trace element in biological systems. It has the distinction of being the heaviest element commonly needed by living organisms as well as the second-heaviest known to be used by any form of life (only tungsten, a component of a few bacterial enzymes, has a higher atomic number and atomic weight). It is a component of biochemical pathways in organisms from all biological kingdoms, suggesting its fundamental significance throughout the evolutionary history of life.[1]
Iodine is critical to the proper functioning of the vertebrate endocrine system, and plays smaller roles in numerous other organs, including those of the digestive and reproductive systems. An adequate intake of iodine-containing compounds is important at all stages of development, especially during the fetal and neonatal periods, and diets deficient in iodine can present serious consequences for growth and metabolism.
Functions
Thyroid
In vertebrate biology, iodine's primary function is as a constituent of the thyroid hormones, thyroxine (T4) and triiodothyronine (T3). These molecules are made from addition-condensation products of the amino acid tyrosine, and are stored prior to release in an iodine-containing protein called thyroglobulin. T4 and T3 contain four and three atoms of iodine per molecule, respectively; iodine accounts for 65% of the molecular weight of T4 and 59% of T3. The thyroid gland actively absorbs iodine from the blood to produce and release these hormones into the blood, actions which are regulated by a second hormone, called thyroid-stimulating hormone (TSH), which is produced by the pituitary gland. Thyroid hormones are phylogenetically very old molecules which are synthesized by most multicellular organisms, and which even have some effect on unicellular organisms. Thyroid hormones play a fundamental role in biology, acting upon gene transcription mechanisms to regulate the basal metabolic rate. T3 acts on small intestine cells and adipocytes to increase carbohydrate absorption and fatty acid release, respectively.[2] A deficiency of thyroid hormones can reduce basal metabolic rate up to 50%, while an excessive production of thyroid hormones can increase the basal metabolic rate by 100%.[3] T4 acts largely as a precursor to T3, which is (with minor exceptions) the biologically active hormone. Via the thyroid hormones, iodine has a nutritional relationship with selenium. A family of selenium-dependent enzymes called deiodinases converts T4 to T3 (the active hormone) by removing an iodine atom from the outer tyrosine ring. These enzymes also convert T4 to reverse T3 (rT3) by removing an inner ring iodine atom, and also convert T3 to 3,3'-Diiodothyronine (T2) by removing an inner ring atom. Both of the latter products are inactivated hormones which have essentially no biological effects and are quickly prepared for disposal. A family of non-selenium-dependent enzymes then further deiodinates the products of these reactions.
In truth, the total amount of iodine in the human body is still controversial, and in 2001, M.T. Hays published in Thyroid that “it is surprising that the total iodine content of the human body remains uncertain after many years of interest in iodine metabolism. Only the iodine content of the thyroid gland has been measured accurately by fluorescent scanning, and it is now well estimate of 5–15 mg in the normal human thyroid. But similar methods are not available for other tissues and for the extrathyroidal organs. Many researchers reported different numbers of 10-50 mg of the total iodine content in human body.[4][5] Selenium also plays a very important role in the production of glutathione, the body's most powerful antioxidant. During the production of the thyroid hormones, hydrogen peroxide is produced in large quantities, and therefore high iodine in the absence of selenium can destroy the thyroid gland (often described as a sore throat feeling); the peroxides are neutralized through the production of glutathione from selenium. In turn, an excess of selenium increases demand for iodine, and deficiency will result when a diet is high in selenium and low in iodine.
Extrathyroidal iodine
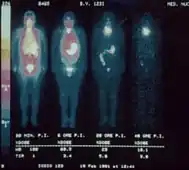
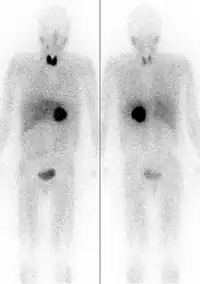
Extra-thyroidal iodine exists in several other organs, including the mammary glands, eyes, gastric mucosa, cervix, cerebrospinal fluid, arterial walls, ovary and salivary glands.[7] In the cells of these tissues the iodide ion (I−) enters directly by the sodium-iodide symporter (NIS). Different tissue responses for iodine and iodide occur in the mammary glands and the thyroid gland of rats.[8] The role of iodine in mammary tissue is related to fetal and neonatal development, but its role in the other tissues is not well known.[9] It has been shown to act as an antioxidant[9] and antiproliferant[10] in various tissues that can uptake iodine. Molecular iodine (I2) has been shown to have a suppressive effect on benign and cancerous neoplasias.[10]
The U.S. Food and Nutrition Board and Institute of Medicine recommended daily allowance of iodine ranges from 150 micrograms per day for adult humans to 290 micrograms per day for lactating mothers. However, the thyroid gland needs no more than 70 micrograms per day to synthesize the requisite daily amounts of T4 and T3. The higher recommended daily allowance levels of iodine seem necessary for optimal function of a number of other body systems, including lactating breasts, gastric mucosa, salivary glands, oral mucosa, arterial walls, thymus, epidermis, choroid plexus and cerebrospinal fluid, among others.[11][12][13]
Other functions
Iodine and thyroxine have also been shown to stimulate the spectacular apoptosis of the cells of the larval gills, tail and fins during metamorphosis in amphibians, as well as the transformation of their nervous system from that of the aquatic, herbivorous tadpole into that of the terrestrial, carnivorous adult. The frog species Xenopus laevis has proven to be an ideal model organism for experimental study of the mechanisms of apoptosis and the role of iodine in developmental biology.[14][1][15][16]
Agents containing iodine can exert a differential effect upon different species in an agricultural system. The growth of all strains of Fusarium verticillioides is significantly inhibited by an iodine-containing fungistatic (AJ1629-34EC) at concentrations that do not harm the crop. This might be a less toxic anti-fungal agricultural treatment due to its relatively natural chemistry.[17][18]
Dietary recommendations
The U.S. Institute of Medicine (IOM) updated Estimated Average Requirements (EARs) and Recommended Dietary Allowances (RDAs) for iodine in 2000. For people age 14 and up, the iodine RDA is 150 μg/day; the RDA for pregnant women is 220 μg/day and the RDA during lactation is 290 μg/day. For children 1–8 years, the RDA is 90 μg/day; for children 8–13 years, 130 μg/day.[19] As a safety consideration, the IOM sets tolerable upper intake levels (ULs) for vitamins and minerals when evidence is sufficient. The UL for iodine for adults is 1,100 μg/day. This UL was assessed by analyzing the effect of supplementation on thyroid-stimulating hormone.[9] Collectively, the EARs, RDAs, AIs and ULs are referred to as Dietary Reference Intakes (DRIs).[19]
The European Food Safety Authority (EFSA) refers to the collective set of information as Dietary Reference Values, with Population Reference Intake (PRI) instead of RDA, and Average Requirement instead of EAR; AI and UL are defined the same as in the United States. For women and men ages 18 and older, the PRI for iodine is set at 150 μg/day; the PRI during pregnancy or lactation is 200 μg/day. For children ages 1–17 years, the PRI increases with age from 90 to 130 μg/day. These PRIs are comparable to the U.S. RDAs with the exception of that for lactation.[20] The EFSA reviewed the same safety question and set its adult UL at 600 μg/day, which is a bit more than half the U.S. value.[21] Notably, Japan reduced its adult iodine UL from 3,000 to 2,200 µg/day in 2010, but then increased it back to 3,000 µg/day in 2015.[22]
As of 2000, the median observed intake of iodine from food in the United States was 240 to 300 μg/day for men and 190 to 210 μg/day for women.[19] In Japan, consumption is much higher due to the frequent consumption of seaweed or kombu kelp.[9] The average daily intake in Japan ranges from 1,000 to 3,000 μg/day; previous estimates suggested an average intake as high as 13,000 μg/day.[23]
Labeling
For U.S. food and dietary supplement labeling purposes, the amount in a serving is expressed as a percent of Daily Value (%DV). For iodine specifically, 100% of the Daily Value is considered 150 μg, and this figure remained at 150 μg in the May 27, 2016 revision.[24][25] A table of the old and new adult daily values is provided at Reference Daily Intake.
Food sources
Natural sources of iodine include many marine organisms, such as kelp and certain seafood products, as well as plants grown on iodine-rich soil.[26][27] Iodized salt is fortified with iodine.[27] According to a Food Fortification Initiative 2016 report, 130 countries have mandatory iodine fortification of salt and an additional 10 have voluntary fortification.
Deficiency
Worldwide, iodine deficiency affects two billion people and is the leading preventable cause of mental retardation.[28] Mental disability is a result which occurs primarily when babies or small children are rendered hypothyroidic by a lack of dietary iodine (new hypothyroidism in adults may cause temporary mental slowing, but not permanent damage).
In areas where there is little iodine in the diet, typically remote inland areas and semi-arid equatorial climates where no marine foods are eaten, iodine deficiency also gives rise to hypothyroidism, the most serious symptoms of which are epidemic goitre (swelling of the thyroid gland), extreme fatigue, mental slowing, depression, weight gain, and low basal body temperatures.[29]
The addition of iodine to table salt (so-called iodized salt) has largely eliminated the most severe consequences of iodine deficiency in wealthier nations, but deficiency remains a serious public health problem in the developing world.[30] Iodine deficiency is also a problem in certain areas of Europe; in Germany, an estimated one billion dollars in healthcare costs is spent each year in combating and treating iodine deficiency.[9]
Iodine and cancer risk
Source:[31]
- Breast cancer. The mammary gland actively concentrates iodine into milk for the benefit of the developing infant, and may develop a goiter-like hyperplasia, sometimes manifesting as fibrocystic breast disease, when iodine level is low. Studies indicate that iodine deficiency, either dietary or pharmacologic, can lead to breast atypia and increased incidence of malignancy in animal models, while iodine treatment can reverse dysplasia,[8][32][33] with elemental iodine (I2) having been found to be more effective in reducing ductal hyperplasias and perilobular fibrosis in iodine-deficient rats than iodide (I−).[8] On the observation that Japanese women who consume iodine-rich seaweed have a relatively low rate of breast cancer, iodine is suggested as a protection against breast cancer.[34][35] Iodine is known to induce apoptosis in breast cancer cells.[36] Laboratory evidence has demonstrated an effect of iodine on breast cancer that is in part independent of thyroid function, with iodine inhibiting cancer through modulation of the estrogen pathway. Gene array profiling of the estrogen responsive breast cancer cell line shows that the combination of iodine and iodide alters gene expression and inhibits the estrogen response through up-regulating proteins involved in estrogen metabolism. Whether iodine/iodide will be useful as an adjuvant therapy in the pharmacologic manipulation of the estrogen pathway in women with breast cancer has not been determined clinically.[32]
- Gastric cancer. Some researchers have found an epidemiologic correlation between iodine deficiency, iodine-deficient goitre, and gastric cancer;[37][38][39] a decrease in the death incidence from stomach cancer after iodine-prophylaxis.[40] In the proposed mechanism, the iodide ion functions in gastric mucosa as an antioxidant reducing species that detoxifies poisonous reactive oxygen species, such as hydrogen peroxide.
Precautions and toxicity
Elemental Iodine
Elemental iodine is an oxidizing irritant, and direct contact with skin can cause lesions, so iodine crystals should be handled with care. Solutions with high elemental iodine concentration such as tincture of iodine are capable of causing tissue damage if use for cleaning and antisepsis is prolonged. Although elemental iodine is used in the formulation of Lugol's solution, a common medical disinfectant, it becomes triiodide upon reacting with the potassium iodide used in the solution and is therefore non-toxic. Only a small amount of elemental iodine will dissolve in water, and adding potassium iodide allows a much larger amount of elemental iodine to dissolve through the reaction of I2-I3. This allows Lugol's iodine to be produced in strengths varying from 2% to 15% iodine.
Elemental iodine (I2) is poisonous if taken orally in large amounts; 2–3 grams is a lethal dose for an adult human.[41][42] Potassium iodide, on the other hand, has a median lethal dose (LD50) that is relatively high in several other animals: in rabbits, it is 10 g/kg; in rats, 14 g/kg, and in mice, 22 g/kg.[43] The tolerable upper intake level for iodine as established by the Food and Nutrition Board is 1,100 µg/day for adults. The safe upper limit of consumption set by the Ministry of Health, Labor and Welfare in Japan is 3,000 µg/day.[44]
The biological half-life of iodine differs between the various organs of the body, from 100 days in the thyroid, to 14 days in the kidneys and spleen, to 7 days in the reproductive organs. Typically the daily urinary elimination rate ranges from 100 to 200 µg/L in humans.[45] However, the Japanese diet, high in iodine-rich kelp, contains 1,000 to 3,000 µg of iodine per day, and research indicates the body can readily eliminate excess iodine that is not needed for thyroid hormone production.[46] The literature reports as much as 30,000 µg/L (30 mg/L) of iodine being safely excreted in the urine in a single day, with levels returning to the standard range in a couple of days, depending on seaweed intake.[47] One study concluded the range of total body iodine content in males was 12.1 mg to 25.3 mg, with a mean of 14.6 mg.[48] It is presumed that once thyroid-stimulating hormone is suppressed, the body simply eliminates excess iodine, and as a result, long-term supplementation with high doses of iodine has no additional effect once the body is replete with enough iodine. It is unknown if the thyroid gland is the rate-limiting factor in generating thyroid hormone from iodine and tyrosine, but assuming it is not, a short-term loading dose of one or two weeks at the tolerable upper intake level may quickly restore thyroid function in iodine-deficient patients.
Iodine vapor is very irritating to the eye, to mucous membranes, and in the respiratory tract. Concentration of iodine in the air should not exceed 1 mg/m3 (eight-hour time-weighted average).
When mixed with ammonia and water, elemental iodine forms nitrogen triiodide, which is extremely shock-sensitive and can explode unexpectedly.
Iodide ion
Excessive iodine intake presents symptoms similar to those of iodine deficiency. Commonly encountered symptoms are abnormal growth of the thyroid gland and disorders in functioning,[49] as well as in growth of the organism as a whole. Iodide toxicity is similar to (but not the same as) toxicity to ions of the other halogens, such as bromides or fluorides. Excess bromine and fluorine can prevent successful iodine uptake, storage and use in organisms, as both elements can selectively replace iodine biochemically.
Excess iodine may also be more cytotoxic in combination with selenium deficiency.[50] Iodine supplementation in selenium-deficient populations is theoretically problematic, partly for this reason.[9] Selenocysteine (abbreviated as Sec or U, in older publications also as Se-Cys)[51] is the 21st proteinogenic amino acid, and is the root of iodide ion toxicity when there is a simultaneous insufficiency of biologically available selenium. Selenocysteine exists naturally in all kingdoms of life as a building block of selenoproteins.[52]
Hypersensitivity reactions
Some people develop a hypersensitivity to compounds of iodine but there are no known cases of people being directly allergic to elemental iodine itself.[53] Notable sensitivity reactions that have been observed in humans include:
- The application of tincture of iodine may cause a rash.
- Some cases of reaction to povidone-iodine (Betadine) have been documented to be a chemical burn.[54]
Medical use of iodine compounds (i.e. as a contrast agent) can cause anaphylactic shock in highly sensitive patients, presumably due to sensitivity to the chemical carrier. Cases of sensitivity to iodine compounds should not be formally classified as iodine allergies, as this perpetuates the erroneous belief that it is the iodine to which patients react, rather than to the specific allergen. Sensitivity to iodine-containing compounds is rare but has a considerable effect given the extremely widespread use of iodine-based contrast media; however, the only adverse effect of contrast material that can convincingly be ascribed to free iodide is iodide mumps and other manifestations of iodism.[55]
See also
- Biology and pharmacology of chemical elements
- Calcium in biology – Overview of the topic
- Magnesium in biology
- Potassium in biology – Description of the element's function as an essential mineral micronutrient
- Selenium in biology – Essential micro-nutrient for animals
- Sodium in biology
References
- 1 2 Venturi, Sebastiano (2011). "Evolutionary Significance of Iodine". Current Chemical Biology. 5 (3): 155–162. doi:10.2174/187231311796765012. ISSN 1872-3136.
- ↑ Widmaier, Eric; Strang, Kevin; Raff, Hershel (2016). Human Physiology: The Mechanisms of Body Function (Fourteenth ed.). New York: McGraw Hill. p. 340. ISBN 9781259294099.
- ↑ Nussey; Whitehead (2001). "Endocrinology: An Integrated Approach". NCBI. Oxford: BIOS Scientific Publishers. Retrieved 9 February 2017.
- ↑ Hays, M.T. (2001). "Estimation of Total Body Iodine Content in Normal Young Men". Thyroid. 11 (7): 671–675. doi:10.1089/105072501750362745. PMID 11484896.
- ↑ Venturi, Sebastiano (2020). "Controversy in the content and action of human extrathyroidal iodine". Human Evolution. 35 (1–2): 1–16. doi:10.14673/HE2020121064.
- ↑ Venturi, S.; Donati, F.M.; Venturi, A.; Venturi, M. (2000). "Environmental Iodine Deficiency: A Challenge to the Evolution of Terrestrial Life?". Thyroid. 10 (8): 727–9. doi:10.1089/10507250050137851. PMID 11014322.
- ↑ Venturi, S.; Donati, F.M.; Venturi, A.; Venturi, M. (2000). "Environmental Iodine Deficiency: A Challenge to the Evolution of Terrestrial Life?". Thyroid. 10 (8): 727–9. doi:10.1089/10507250050137851. PMID 11014322.
- 1 2 3 Eskin, Bernard A.; Grotkowski, Carolyn E.; Connolly, Christopher P.; Ghent, William R. (1995). "Different tissue responses for iodine and iodide in rat thyroid and mammary glands". Biological Trace Element Research. 49 (1): 9–19. doi:10.1007/BF02788999. PMID 7577324. S2CID 24230708.
- 1 2 3 4 5 6 Patrick L (2008). "Iodine: deficiency and therapeutic considerations" (PDF). Altern Med Rev. 13 (2): 116–27. PMID 18590348. Archived from the original (PDF) on 2013-05-31.
- 1 2 Aceves C, Anguiano B, Delgado G (August 2013). "The extrathyronine actions of iodine as antioxidant, apoptotic, and differentiation factor in various tissues". Thyroid. 23 (8): 938–46. doi:10.1089/thy.2012.0579. PMC 3752513. PMID 23607319.
- ↑ Brown-Grant, K. (1961). "Extrathyroidal iodide concentrating mechanisms". Physiol. Rev. 41 (1): 189–213. doi:10.1152/physrev.1961.41.1.189.
- ↑ Spitzweg, C., Joba, W., Eisenmenger, W. and Heufelder, A.E. (1998). "Analysis of human sodium iodide symporter gene expression in extrathyroidal tissues and cloning of its complementary deoxyribonucleic acid from salivary gland, mammary gland, gastric mucosa". J Clin Endocrinol Metab. 83 (5): 1746–51. doi:10.1210/jc.83.5.1746. PMID 9589686.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Banerjee, R.K., Bose, A.K., Chakraborty, t.K., de, S.K. and datta, A.G. (1985). "Peroxidase catalysed iodotyrosine formation in dispersed cells of mouse extrathyroidal tissues". J. Endocrinol. 106 (2): 159–65. doi:10.1677/joe.0.1060159. PMID 2991413.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Jewhurst K, Levin M, McLaughlin KA (2014). "Optogenetic Control of Apoptosis in Targeted Tissues of Xenopus laevis Embryos". J Cell Death. 7: 25–31. doi:10.4137/JCD.S18368. PMC 4213186. PMID 25374461.
- ↑ Venturi, S.; Venturi, M. (2014). "Iodine, PUFAs and Iodolipids in Health and Disease: An Evolutionary Perspective". Human Evolution. 29 (1–3): 185–205. ISSN 0393-9375.
- ↑ Tamura K, Takayama S, Ishii T, Mawaribuchi S, Takamatsu N, Ito M (2015). "Apoptosis and differentiation of Xenopus tail-derived myoblasts by thyroid hormone". J Mol Endocrinol. 54 (3): 185–192. doi:10.1530/JME-14-0327. PMID 25791374.
- ↑ Yates, IE; Arnold, JW; Bacon, CW; Hinton, DM (2004). "In vitro assessments of diverse plant pathogenic fungi treated with a novel growth control agent". Crop Protection. Elsevier. 23 (12): 1169–1176. doi:10.1016/j.cropro.2004.03.019. ISSN 0261-2194. S2CID 84907161.
- ↑ Durham, Sharon (January 2003). "Seed Saver: Iodine-based Fungicide Foils Fusarium". AgResearch. USDA ARS (United States Department of Agriculture Agricultural Research Service). 51 (1).
- 1 2 3 United States National Research Council (2000). Dietary Reference Intakes for Vitamin A, Vitamin K, Arsenic, Boron, Chromium, Copper, Iodine, Iron, Manganese, Molybdenum, Nickel, Silicon, Vanadium, and Zinc. National Academies Press. pp. 258–259. doi:10.17226/10026. ISBN 978-0-309-07279-3. PMID 25057538.
- ↑ "Overview on Dietary Reference Values for the EU population as derived by the EFSA Panel on Dietetic Products, Nutrition and Allergies" (PDF). 2017.
- ↑ Tolerable Upper Intake Levels For Vitamins And Minerals (PDF), European Food Safety Authority, 2006
- ↑ Overview of Dietary Reference Intakes for Japanese (2015) Minister of Health, Labour and Welfare, Japan| url = http://www.mhlw.go.jp/file/06-Seisakujouhou-10900000-Kenkoukyoku/Overview.pdf
- ↑ Zava, Theodore T.; Zava, David T. (2011). "Assessment of Japanese iodine intake based on seaweed consumption in Japan: A literature-based analysis". Thyroid Research. 4: 14. doi:10.1186/1756-6614-4-14. PMC 3204293. PMID 21975053.
- ↑ "Federal Register May 27, 2016 Food Labeling: Revision of the Nutrition and Supplement Facts Labels. FR page 33982" (PDF).
- ↑ "Daily Value Reference of the Dietary Supplement Label Database (DSLD)". Dietary Supplement Label Database (DSLD). Retrieved 16 May 2020.
- ↑ "Sources of iodine". International Council for the Control of Iodine Deficiency Disorders.
- 1 2 "MedlinePlus Medical Encyclopedia: Iodine in diet".
- ↑ McNeil, Donald G. Jr (2006-12-16). "In Raising the World's I.Q., the Secret's in the Salt". New York Times. Retrieved 2008-12-04.
- ↑ Felig, Philip; Frohman, Lawrence A. (2001). "Endemic Goiter". Endocrinology & metabolism. McGraw-Hill Professional. ISBN 978-0-07-022001-0.
- ↑ "Micronutrients - Iodine, Iron and Vitamin A". UNICEF.
- ↑ De la Vieja, A.; Santisteban, P (2008). "Role of iodide metabolism in physiology and cancer". Endocr. Relat. Cancer. 25 (4): R225–R245. doi:10.1530/ERC-17-0515. PMID 29437784.
- 1 2 Stoddard II, F. R.; Brooks, A. D.; Eskin, B. A.; Johannes, G. J. (2008). "Iodine Alters Gene Expression in the MCF7 Breast Cancer Cell Line: Evidence for an Anti-Estrogen Effect of Iodine". International Journal of Medical Sciences. 5 (4): 189–96. doi:10.7150/ijms.5.189. PMC 2452979. PMID 18645607.
- ↑ Venturi, S.; Grotkowski, CE; Connolly, CP; Ghent, WR (2001). "Is there a role for iodine in breast diseases?". The Breast. 10 (1): 379–82. doi:10.1054/brst.2000.0267. PMID 14965610. S2CID 41558438.
- ↑ Smyth PP (July 2003). "The thyroid, iodine and breast cancer". Breast Cancer Research (review). 5 (5): 235–8. doi:10.1186/bcr638. PMC 314438. PMID 12927031.
- ↑ Smyth PP (2003). "Role of iodine in antioxidant defence in thyroid and breast disease". BioFactors (review). 19 (3–4): 121–30. doi:10.1002/biof.5520190304. PMID 14757962. S2CID 7803619.
- ↑ Shrivastava, A. (2006). "Molecular Iodine Induces Caspase-independent Apoptosis in Human Breast Carcinoma Cells Involving the Mitochondria-mediated Pathway". Journal of Biological Chemistry. 281 (28): 19762–19771. doi:10.1074/jbc.M600746200. ISSN 0021-9258. PMID 16679319.
- ↑ Josefssson, M.; Ekblad, E. (2009). "Sodium Iodide Symporter (NIS) in Gastric Mucosa: Gastric Iodide Secretion". In Preedy, Victor R.; Burrow, Gerard N.; Watson, Ronald (eds.). Comprehensive Handbook of Iodine: Nutritional, Biochemical, Pathological and Therapeutic Aspects.
- ↑ Abnet CC, Fan JH, Kamangar F, Sun XD, Taylor PR, Ren JS, Mark SD, Zhao P, Fraumeni JF Jr, Qiao YL, Dawsey SM (2006). "Self-reported goiter is associated with a significantly increased risk of gastric noncardia adenocarcinoma in a large population-based Chinese cohort". International Journal of Cancer. 119 (6): 1508–1510. doi:10.1002/ijc.21993. PMID 16642482. S2CID 45732451.
- ↑ Behrouzian, R.; Aghdami, N. (2004). "Urinary iodine/creatinine ratio in patients with stomach cancer in Urmia, Islamic Republic of Iran". East Mediterr Health J. 10 (6): 921–924. PMID 16335780..
- ↑ Golkowski F, Szybinski Z, Rachtan J, Sokolowski A, Buziak-Bereza M, Trofimiuk M, Hubalewska-Dydejczyk A, Przybylik-Mazurek E, Huszno B (2007). "Iodine prophylaxis--the protective factor against stomach cancer in iodine deficient areas". Eur J Nutr. 46 (5): 251–6. doi:10.1007/s00394-007-0657-8. PMID 17497074. S2CID 24494246.
- ↑ "Iodine". CDC NIOSH. 1994.
- ↑ Moore, Merrill (1938). "The Ingestion of Iodine as a Method of Attempted Suicide". New England Journal of Medicine. 219 (11): 383–388. doi:10.1056/NEJM193809152191104. ISSN 0028-4793.
- ↑ Lewis, Richard (1996). Sax's Dangerous Properties of Industrial Materials. 9th Ed. Volumes 1-3. New York, NY: Van Nostrand Reinhold. ISBN 9780442022570.
- ↑ Zava, TT; Zava, DT (2011). "Assessment of Japanese iodine intake based on seaweed consumption in Japan: A literature-based analysis". Thyroid Res. 4: 14. doi:10.1186/1756-6614-4-14. PMC 3204293. PMID 21975053.
- ↑ World Health Organization (2007). United Nations Children's Fund & International Council for the Control of Iodine Deficiency Disorders. Assessment of iodine deficiency disorders and monitoring their elimination . 3rd ed.
- ↑ Zava, T. T.; Zava, D. T. (2011). "Assessment of Japanese iodine intake based on seaweed consumption in Japan: A literature-based analysis". Thyroid Research. 4: 14. doi:10.1186/1756-6614-4-14. PMC 3204293. PMID 21975053.
- ↑ Nagataki, S.; Shizume, K.; Nakao, K. (1967). "Thyroid Function in Chronic Excess Iodide Ingestion: Comparison of Thyroidal Absolute Iodine Uptake and Degradation of Thyroxine in Euthyroid Japanese Subjects". Journal of Clinical Endocrinology & Metabolism. 27 (5): 638–647. doi:10.1210/jcem-27-5-638. PMID 4164900.
- ↑ Hays, M. T. (2001). "Estimation of Total Body Iodine Content in Normal Young Men". Thyroid. 11 (7): 671–675. doi:10.1089/105072501750362745. PMID 11484896.
- ↑ Pearce, EN.; Gerber, AR.; Gootnick, DB.; Kettel Khan, L.; Li, R.; Pino, S.; Braverman, LE. (2002). "Effects of Chronic Iodine Excess in a Cohort of LongTerm American Workers in West Africa". Journal of Clinical Endocrinology & Metabolism. 87 (12): 5499–5502. doi:10.1210/jc.2002-020692. PMID 12466344.
- ↑ Smyth, PP (2003). "Role of iodine in antioxidant defence in thyroid and breast disease". BioFactors. 19 (3–4): 121–30. doi:10.1002/biof.5520190304. PMID 14757962. S2CID 7803619.
- ↑ "IUPAC-IUBMB Joint Commission on Biochemical Nomenclature (JCBN) and Nomenclature Committee of IUBMB (NC-IUBMB)". European Journal of Biochemistry. 264 (2): 607–609. 1999. doi:10.1046/j.1432-1327.1999.news99.x.
- ↑ Johansson, L.; Gafvelin, G.; Amér, E. S. J. (2005). "Selenocysteine in Proteins — Properties and Biotechnological Use". Biochimica et Biophysica Acta (BBA) - General Subjects. 1726 (1): 1–13. doi:10.1016/j.bbagen.2005.05.010. hdl:10616/39311. PMID 15967579.
- ↑ Böhm I, Silva Hasembank Keller P, Heverhagen JT (2016). ""Iodine Allergy" – The Neverending Story" (PDF). RöFo. 188 (8): 733–4. doi:10.1055/s-0042-110102. PMID 27459005.
- ↑ D. O. Lowe; S. R. Knowles; E. A. Weber; C. J. Railton; N. H. Shear (2006). "Povidone-iodine-induced burn: case report and review of the literature". Pharmacotherapy. 26 (11): 1641–5. doi:10.1592/phco.26.11.1641. PMID 17064209. S2CID 25708713.
- ↑ Katelaris, Constance (2009). "'Iodine Allergy' label is misleading". Australian Prescriber. 32 (5): 125–128. doi:10.18773/austprescr.2009.061..